What To Do If You Don’t Qualify For Medicaid
If you don’t qualify for Medicaid, you can possibly get subsidized health care through the Obamacare marketplaces during a special enrollment or open enrollment period. Americans who making more than 100% of the FPL qualify for a premium tax credit that can significantly lower the cost of a plan.
Federal open enrollment for 2022 health care plans runs until Jan. 15, 2022, though some state exchanges are open longer. Learn 2022 open enrollments dates by state. Healthcare.gov, the federal exchange, usually opens from November 1 to December 15 each year.
If you can’t find affordable health care on your marketplace during open enrollment, you have a few back-up options.
These include:
Short-term health insurance: Originally designed to prevent short-term health insurance gaps, these plans are cheaper, but much less comprehensive than traditional coverage. They don’t have to cover Obamacare’s 10 essential benefits or pre-existing conditions. Following changes by the Trump administration, short-term health plans can last from three months to potentially three years, though som estates have stricter limits.
Limited benefit plans: These plans cover a very small portion of the costs associated with certain “medical events,” like a doctor’s visit or ambulance ride. Both the number of events and dollar amounts covered are capped.
Who Qualifies For Medicaid
In all but 13 states, adults who make below a certain income may qualify for Medicaid. In all states, Medicaid is available to people who make a low income and also meet other criteria such as being at least 65 years old, disabled, pregnant or other qualifications.
Each state runs its own Medicaid programs with its own set of qualifying criteria.
What Does Medicaid Cover For Adults
Mandatory benefits include services including inpatient and outpatient hospital services, physician services, laboratory and x-ray services, and home health services, among others. Optional benefits include services including prescription drugs, case management, physical therapy, and occupational therapy.
Recommended Reading: Does Medicaid Cover Swimming Lessons
Arkansas Medicaid Income Limits Summary
We hope this post on Arkansas Medicaid Income Limits was helpful to you.
If you have any questions about Medicaid in the state of Arkansas, you can ask us in the comments section below.
Help us spread the word! If you found this post on Arkansas Medicaid Income Limits helpful, help us spread the word by sharing it using the Share this button below.
Be sure to check out our other articles about Medicaid.
Medicaid Eligibility Program Overview
Medicaid pays for the cost of Nursing Home care in Arkansas that meet certain financial and health criteria. The average cost of Skilled Nursing Care in Arkansas is $58,860, so securing Medicaid coverage is essential. In Arkansas there are 242 Nursing Homes, of which 98% accept Medicaid insurance as a form of payment. The most expensive Nursing Home in Arkansas is Hudson Memorial Nursing Home which costs $300 per day and the least expensive Nursing Home is The Waters Of Stamps, Llc which costs $100 per day. Nursing Homes in Arkansas are currenlty 68.06% full with 17,618 patients currently using the 25,886 beds available.
To learn about the entire Medicaid eligibilty process, we have put together a comprehensive medicaid nursing home guide which you can read here.
Don’t Miss: Blue Cross Blue Shield Medicaid Indiana
What Is The Medicaid Income Limit In My State
Most states use a standard of 138% of the federal poverty level as a basis for Medicaid eligibility. But each state is free to set its own limits.
The table below shows the income limit as a percentage of the FPL required for Medicaid eligibility in each state for two-parent households and for individuals adults.
If 0% appears, that means individuals may not qualify for Medicaid in that state based on income alone and must meet other criteria, such as being pregnant or disabled.
Medicaid Income Limit by State|
State |
|
|---|---|
| 52% | 0% |
FPL is used to determine eligibility for Medicaid, certain welfare benefits and other assistance programs. The FPL is computed by the U.S. Census Bureau and can be adjusted every year based on inflation.
Medicaid uses a percentage of the FPL to determine its income limits for eligibility. For example, you may qualify for Medicaid if you earn less than 133% of the federal poverty level. Or you may qualify if you earn less than 150% of the federal poverty level and are disabled. Again, each state sets its own income limits to determine Medicaid eligibility.
Contact your state Medicaid program for more eligibility information, as most states offer different types of Medicaid programs that may each have their own income limits and other qualifying criteria. Even if you make more than the standard limit found below, there may be additional programs for which you still qualify.
What Makes Me Eligible For Medicaid
Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, such as lawful permanent residents. In addition, some eligibility groups are limited by age, or by pregnancy or parenting status.
Read Also: Michigan Medicaid Nursing Home Application
Number Losing Coverage Exceeded Policys Supposed Target Population: Beneficiaries Not Working Or Eligible For Exemptions
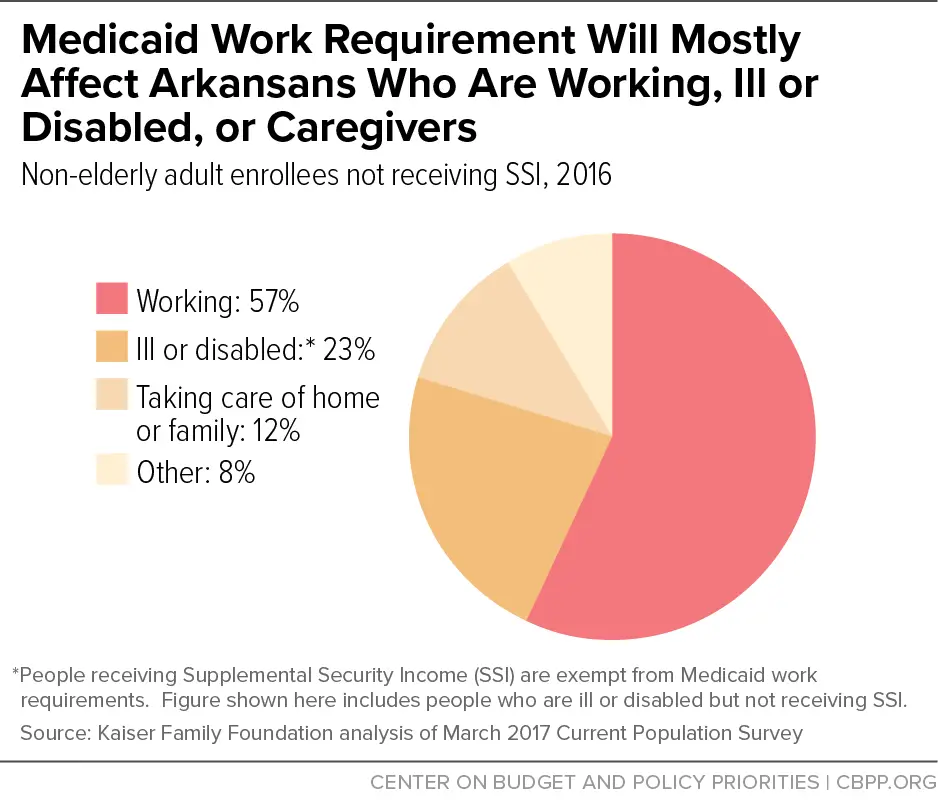
About 3 or 4 percent of those subject to the Arkansas work requirement were not working and did not qualify for exemptions, studies estimate. Yet each month, 8 to 29 percent of those subject to the requirement failed to report hours or reported insufficient work hours. In fact, over 75 percent of those required to report hours failed to do so each month. Likewise, a study estimates that all but a small minority of Medicaid expansion beneficiaries in New Hampshire were either working or ill or disabled , yet 40 percent of those subject to the work requirement were set to lose coverage had the state not put the policy on hold.
News accounts corroborate that eligible beneficiaries in Arkansas lost coverage and were at risk of losing coverage in New Hampshire. For example, one working Arkansas beneficiary with a chronic condition explained that he lost Medicaid and then could not afford medications, which in turn caused him to lose his job due to his deteriorating health. Another reported rationing her medication after failing to navigate the reporting requirement and losing coverage, despite working 25 to 35 hours each week which equates to well over the states monthly minimum requirement. And a New Hampshire woman described her struggle to obtain a medical frailty exemption, which failed because her primary care doctor and neurosurgeon each insisted that the other should fill out the necessary paperwork.
What Is Arkansas Medicaid Expansion Private Option
Arkansas is among the states expanding Medicaid, but it is using a non-standard approach or waiver. Arkansas Medicaid expansion waiver allows the state to use Medicaid expansion funds to subsidize premiums for beneficiaries who purchase private health insurance through the health insurance marketplace.
Arkansas received federal approval in late 2014 to amend its Private Option waiver. The approved changes establish health savings accounts for beneficiaries, allow cost-sharing for Private Option Beneficiaries at 50% of FPL, and limit some transportation services.
The growth in Arkansas Medicaid enrollment has played a significant role in the reduction in the uninsured rate in the state. According to U.S. Census data, 16% of Arkansas residents were uninsured in 2013, and that had dropped to 7.9% by 2016 a decrease of more than 50%.
However, the future of Arkansas Private Option/Arkansas Works is not certain. The state legislature must reauthorize the program annually with a 75% majority in both the House and Senate. In 2014, it took five attempts to pass reauthorization. S.B.196 reauthorized Medicaid expansion in March 2017. In 2019, the Arkansas House Medicaid expansion funding just two days after the states Medicaid work requirement had been overturned by a federal judge. But the following week the measure was approved was signed into law in early April, reauthorizing Medicaid expansion funding in Arkansas until the end of June 2020.
Recommended Reading: I Lost My Medicaid Card
What Do I Need For Proof Of Income
In order to prove that you fall within the limit for income eligibility, you will need to provide documentation of all sources of income that you have.
Documents to include are things like pay stubs from wages, copies of social security deposits, copies of alimony checks, and award letters from any other monthly financial benefit that you may receive.
It would also be helpful to have all of your most recent income tax returns and any other tax forms that would be relevant to verifying your income.
Some states are able to electronically gather the resources to verify your income, which does simplify the process as well as eliminate fraud. To find out if your state has this technology for your application, click here to learn more about the application process in your state of residence.
Can I Qualify For Medicaid If I Have Savings
Medicaid is the government health insurance program for people with low income and the disabled. There used to be a limit on how much you could have in assets and still qualify for Medicaid. Medicaid does not look at an applicants savings and other financial resources unless the person is 65 or older or disabled.
Recommended Reading: Does Kelsey Seybold Accept Medicaid
Does Arkansas Have A Medicaid Work Requirement
Arkansas implemented a Medicaid work requirement in 2018, described below in detail. But Federal Judge James Boasberg overturned the Medicaid work requirements in Kentucky and Arkansas as of March 2019, noting that officials had not taken steps to prevent coverage losses stemming from the work requirement.
The Biden administration officially withdrew the states Medicaid work requirement waiver approval in March 2021, although it had not been in effect for two years prior to that.
So Arkansas is no longer removing people from the Medicaid program for failure to comply with the work requirement or reporting requirement, and the people who had already lost their coverage under the work requirement rules were able to re-apply for Medicaid although many may not be aware that their access to Medicaid has been reinstated .
As of March 2021, there were more than 905,000 people enrolled in Arkansas Medicaid and CHIP, which was higher than it had been in the months following implementation of the work requirement, but still lower than it had been in 2018, despite the fact that the COVID pandemic had been ongoing for a year.
Where To Apply For Medicaid In Arkansas In Person
If you need help filling out your Medicaid application form you can apply for Arkansas Medicaid in person. Many people who do not know how to apply for Medicaid choose this option to enlist the help of office employees. You can pick up, complete, and submit an application at the Department of Human Services office in the county where you live.
Furthermore, applicants can obtain more information about Medicaid regulations and program details. If you cannot make it in person, you can have a family member or friend apply for you. When you visit the Department of Human Services office, you should be ready with the information you need to apply for Medicaid.
As with the other methods of applying for Medicaid, applicants need all current insurance forms, pay stubs, verifiable identification and other necessary documents. If you do not have all of this information available, the state can still process your Medicaid application, but it may take longer to get the health insurance for which you are entitled.
After submitting an application, applicants waiting to hear about the case status may wait for a status update via mail or phone call. There will be further instructions available, based on each applicants unique case.
You May Like: What States Does Medicaid Cover Abortions
What Are The Different Types Of Care Available
The Medicaid programs available in each state are: regular Medicaid, Medicaid for long-term nursing home care, and Medicaid for home-based nursing care.
Regular Medicaid is the health care benefits program available to all of a states residents, providing they meet the eligibility requirements. Some of the eligibility requirements include:
- Low-income
- Legal status on the United States
- Resident of the state of application
Those who meet these criteria are able to use their regular Medicaid benefits for their doctors visits, hospital care, laboratory testing, and transportation for medical purposes.
The income limit for regular medicaid will be a set amount, depending on state and marital status. Some states allow one lump sum for a married couple and others have an income limit per spouse.
Medicaid for long-term nursing home care is for those who are elderly and can no longer live independently, those with chronic illness, and people with disabilities. At the facility, the residents receive 24/7 supervision and medical care, as well as lodgings and meals.
All state residents who meet the eligibility criteria and require long-term nursing home care are entitled to and will receive the care. There are no waitlists or lotteries for this benefit and you cant be denied if you meet the eligibility requirements.
What Is The Eligibility Criteria For Medicaid
Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, such as lawful permanent residents. In addition, some eligibility groups are limited by age, or by pregnancy or parenting status.
Read Also: How To Add New Baby To Medicaid
What Are The 4 Types Of Medicaid
If you meet income, asset, and other guidelines in your state, you may qualify for one of the following Medicaid programs: Aged, blind, and disabled Medicaid: Beneficiaries with ABD Medicaid have coverage for a broad range of health services, including doctors visits, hospital care, and medical equipment.
Data Show Work Requirements Lead To Large Coverage Losses
In Arkansas, over 18,000 beneficiaries, or about a quarter of those subject to the work requirement, lost coverage over the first seven months of implementation. In New Hampshire, almost 17,000 beneficiaries, or about 40 percent of those subject to the work requirement, were set to lose Medicaid before the state suspended the requirement. In Michigan, some 80,000 beneficiaries, or about one-third of those subject to the work requirement, were set to lose coverage before the court vacated the states work requirement policy. These coverage losses are even higher than the 6 to 17 percent coverage loss that Kaiser Family Foundation researchers forecasted could result from implementing work requirements nationwide.
A study by Harvard researchers found that the uninsured rate among low-income Arkansans aged 30-49 the group potentially subject to work requirements rose from 10.5 percent in 2016 to 14.5 percent in 2018, after the work requirement took effect. There was no similar increase for low-income Arkansans of other ages or for low-income people aged 30-49 in other, similar states. This finding refutes claims, for example from HHS Secretary Alex Azar, that most people leaving Medicaid due to the policy did so because they found jobs with health insurance.
Also Check: Do Doctors Have To Accept Medicaid
Medicaid Income Eligibility Chart For 2022
If you are looking into applying to receive Medicaid, whether it is for the first or hundredth time, your eligibility is decided based on your income. However the income eligibility can change from year to year, depending on the economy and what sort of care you require.
The Medicaid Income Eligibility chart is a tool for determining if your income falls under the limit, depending on if you need regular medicaid or Medicaid for long-term nursing care. All you need to do is find the listings for your state, line that up with the care you need, and then you will see the income limit for both single and married applicants.
If you are looking for an overview of the Medicaid Income Eligibility Chart regarding your situation, this is the article you need to read. Here, I will be providing all of the information for each state, type of care, and marital status for those who are trying to learn the facts. Read on to get more information about the benefits that are available to you!
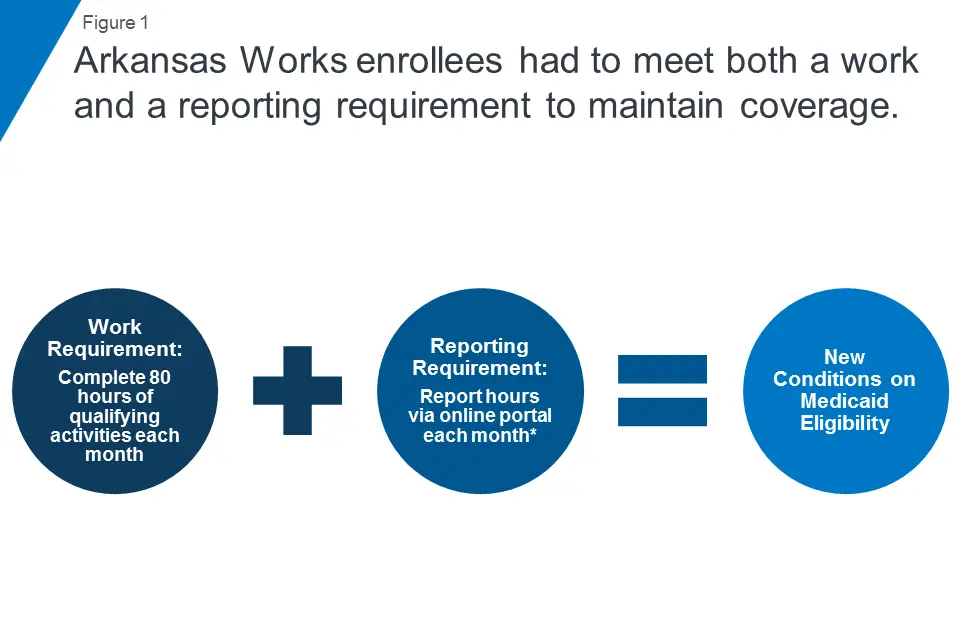
Transition To Arkansas Works In 2017
In April 2016, lawmakers in Arkansas voted to approve and fund an overhaul of Medicaid expansion in Arkansas, dubbed Arkansas Works. The state submitted the new waiver proposal to CMS in June 2016, and CMS reviewed it over the following months. In December 2016, CMS granted approval for most of the modifications the state had requested, with a five-year extension of the Arkansas Works Medicaid demonstration waiver, which took effect in 2017 .
Under Arkansas Works, enrollees with income above the poverty level now pay modest premiums for their coverage , unemployed enrollees are referred to job training/referral, and enrollees can obtain coverage from their employers with supplemental funding from Medicaid.
But only about 20% of the 63,000 enrollees subject to premiums actually paid those premiums in 2017. . The state reported that of the people referred to job training, less than 5% followed through and obtained work referrals. And only one person ever used the Medicaid premium assistance program for employer-sponsored insurance.
Additional changes to Arkansas Medicaid expansion were approved by state lawmakers in May 2017, and Governor Hutchinson submitted an amendment to the states waiver in June 2017, which was under HHS review for several months. The proposed changes, detailed below, were mostly approved by the Trump Administration, although the states proposal to cap Medicaid eligibility at the poverty level was rejected.
You May Like: Community Medicaid Look Back Period
Selecting Medicare Part D Or Medicare Advantage Plan
The Arkansas Insurance Departments Senior Health Insurance Information Program is a health insurance information program that provides free one-on-one counseling, education, and information to individuals with Medicare of all ages. SHIIP answers questions related to Medicare health coverage, Medicare supplemental insurance, long-term care insurance, Medicare Advantage Plans, and Medicaid.
Download a free copy of the Medicare Protection Toolkit from SHIIP. Contact SHIIP at 224-6330 or 371-2782.
