How Much Is The Federal Poverty Level
The federal poverty level in 2021 is equal to an income of $12,880 per year for an individual adult, plus $4,540 for each additional household member. Alaska and Hawaii have different benchmarks because of their differing costs of living.
2021 Federal Poverty Level by State|
Number of people in home |
48 states and Washington D.C. |
Alaska |
|---|
What Makes Me Eligible For Medicaid
Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, such as lawful permanent residents. In addition, some eligibility groups are limited by age, or by pregnancy or parenting status.
Read Also: Michigan Medicaid Nursing Home Application
What Is The Monthly Income Limit For Medicaid In Arkansas
As of January 2020, the income limit for medically needy qualifying for a single applicant is $108.33/month, while the income limit for a is $216.66. This is also when we start requiring applicants to submit their most recent tax return to determine their eligibility. If an applicant does not meet the income requirement after this date, they will not be eligible until their income rises again.
Medicaid is funded by federal and state governments. The federal government provides 100% of the funds for Medicaid through the Social Security Administration . States must follow certain guidelines when implementing their own Medicaid programs including determining eligibility requirements, covering certain services, and providing assistance to low-income individuals.
In Arkansas, there are three groups that are covered by Medicaid: children, adults without dependents, and adults with disabilities. To be eligible for Medicaid, you must meet certain income requirements based on your filing status and number of dependents. In addition, states have the option of applying work requirements to Medicaid. These requirements can include working at a job or seeking employment if you are able to work but not working enough hours or making too much money. If you fail to comply, you could lose your coverage.
You May Like: Dentist In Farmington Nm That Take Medicaid
Arkansas Medicaid Income Limit
The Arkansas Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the Arkansas Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 142 percent of FPL
- Any child age 1-5 with a family income up to 142 percent of FPL
- Children ages 6- 18 with family income up to 142 percent of FPL
- CHIP for children with family income up to 211 percent of FPL
- Pregnant women with family income up to 209 percent of FPL
- Parents of minor children with family income up to 17 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 80% of the FPL
- Adults without dependents under Medicaid expansion with income up to 133% of the FPL
Arkansas Medicaid Phone Number
Heres how to contact the Arkansas Medicaid Agency:
Arkansas Medicaid Claims Questions Information Line
Arkansas Medicaid Complaint Hotline
Arkansas Medicaid Complaint Hotline, Telecommunication Device for the Deaf
Arkansas Medicaid Fraud and Abuse Hotline: 1-800-422-6641
For all other phone numbers for the Arkansas Medicaid Agency, .
Also Check: Texas Medicaid Find A Provider
Similar Program New Name
After 2016, Medicaid expansion in Arkansas was called Arkansas Works instead of the Private Option. But it was widely noted that the fundamental mechanics of the new program were very similar to the Arkansas Health Care Independence Program, which was the name of the Arkansas waiver program from 2014 through 2016. Arkansas still uses Medicaid funds to purchase private coverage for eligible enrollees in the exchange, which was the basic premise of the Private Option in the first place.
But lawmakers who were opposed to the Private Option were able to end it and replace it with Arkansas Works in many cases, fulfilling campaign promises but without the ramifications that would ensue if the state were to kick 300,000+ people off their health insurance .
Medicaid And Medicare Dual Eligibility
If you qualify for both Medicare and Medicaid, you are considered dual eligible. In this case, you may qualify for a certain type of Medicare Advantage plan called a Dual Eligible Special Needs Plan . D-SNPs are designed to meet the specific needs of people who have Medicaid and Medicare.
You can compare plans online to find out if D-SNPs are available where you live, or you can call to speak with a licensed insurance agent for information about eligibility and enrollment.
Recommended Reading: Does Medicaid Pay For Part B Medicare
Find A $0 Premium Medicare Advantage Plan Today
Copyright 2022 TZ Insurance Solutions LLC. All rights reserved.
For California residents, CA-Do Not Sell My Personal Info, .
MedicareAdvantage.com is a website owned and operated by TZ Insurance Solutions LLC. TZ Insurance Solutions LLC and TruBridge, Inc. represent Medicare Advantage Organizations and Prescription Drug Plans having Medicare contracts enrollment in any plan depends upon contract renewal.
The purpose of this communication is the solicitation of insurance. Callers will be directed to a licensed insurance agent with TZ Insurance Solutions LLC, TruBridge, Inc. and/or a third-party partner who can provide more information about Medicare Advantage Plans offered by one or several Medicare-contracted carrier. TZ Insurance Solutions LLC, TruBridge, Inc., and the licensed sales agents that may call you are not connected with or endorsed by the U.S. Government or the federal Medicare program.
Plan availability varies by region and state. For a complete list of available plans, please contact 1-800-MEDICARE , 24 hours a day/7 days a week or consult www.medicare.gov.
Medicare has neither reviewed nor endorsed this information.
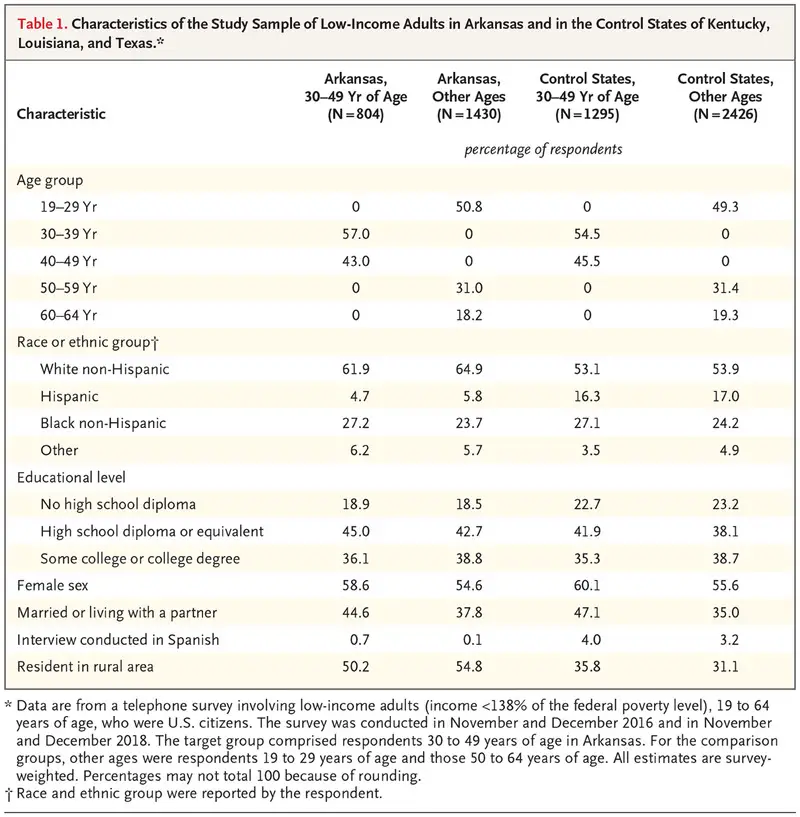
Data Dont Show Employment Gains Due To Work Requirements
The Harvard researchers studies cited above found no evidence that the work requirement policy increased employment, number of hours worked, or overall rates of community engagement activities . Employment rates for low-income Arkansas residents aged 30-49 did not meaningfully increase after the policy took effect, nor did they increase relative to employment rates for older low-income Arkansas residents or low-income younger people in neighboring states.
Whats more, nearly all of the beneficiaries who met Arkansas requirement by working were automatically deemed compliant because they were already working before the rules took effect or because they complied with work requirements already in place under SNAP . Only the group that had to report hours each month faced any new work incentive due to the policy. And of that group, only a few hundred each month met the requirement by reporting sufficient work hours, the state reports putting an upper bound on the number of people who could have found jobs because of the work requirement. Moreover, most of these people would likely have found jobs regardless: low-income people move in and out of jobs frequently under any circumstances.
Recommended Reading: Eye Doctors In Great Falls Mt That Accept Medicaid
Arkansas Medicaid Long Term Care Programs
In Arkansas in 2022, even if you are receiving Medicaid benefits you will have to reapply for long term care Medicaid. Listed below are the four main types of long term care available in Arkansas. Each one has different requirements and offers different services.
Arkansas is an income cap state, meaning that in order to be eligible for Medicaid long term care benefits there is a hard income limit. Non income cap states allow applicants to spend down money for their care, whereas income cap states require the amount to be no higher than their limit at time of application.
Arkansas Medicaid Eligibility Information
There are many paths to Medicaid eligibility. Medicaid eligibility can depend on factors such asyour household size, household income, household assets, you age, and whether you have a disability. If you’reunder 65 and don’t have a disability, you’re eligibility will likely be based on your income only .If you’re over65 or have a disability, you’re likely eligible for Medicare. If eligible for Medicare,there are alternate pathways to Medicaid eligibility which typically include asset tests. Additionally,the way that your income is calculated for these programs is more complicated, meaning that yourincome could be above the income limits and you’d still be eligible.For a more personalized estimate, you canuse our Medicaid eligibility calculator.Please note that there may be otherhealth insurance assistance programs offered by your state not listed here,and there may be other eligibilityrequirements for these programs that are not listed here. Additionally, the way that household incomeand household size are calculated can differ from a household’stotal pre-tax income and the number of people on the tax return.
This website is not affiliated with any government organization or Medicaid,CHIP, or health insurance program.
Recommended Reading: Medicaid Nursing Homes St Louis Mo
What Is Arkansas’ Medicaid Expansion ‘private Option’
Arkansas is among the states expanding Medicaid, but it is using a non-standard approach or waiver. Arkansas Medicaid expansion waiver allows the state to use Medicaid expansion funds to subsidize premiums for beneficiaries who purchase private health insurance through the health insurance marketplace.
Although a few other states have implemented similar programs, they had all abandoned that approach as of 2019. Enrolling Medicaid beneficiaries in private plans is significantly more expensive than using a traditional fee-for-service or Medicaid managed care approach.
What Is The Medicaid Income Limit In My State
Most states use a standard of 138% of the federal poverty level as a basis for Medicaid eligibility. But each state is free to set its own limits.
The table below shows the income limit as a percentage of the FPL required for Medicaid eligibility in each state for two-parent households and for individuals adults.
If 0% appears, that means individuals may not qualify for Medicaid in that state based on income alone and must meet other criteria, such as being pregnant or disabled.
Medicaid Income Limit by State|
State |
|
|---|---|
| 52% | 0% |
FPL is used to determine eligibility for Medicaid, certain welfare benefits and other assistance programs. The FPL is computed by the U.S. Census Bureau and can be adjusted every year based on inflation.
Medicaid uses a percentage of the FPL to determine its income limits for eligibility. For example, you may qualify for Medicaid if you earn less than 133% of the federal poverty level. Or you may qualify if you earn less than 150% of the federal poverty level and are disabled. Again, each state sets its own income limits to determine Medicaid eligibility.
Contact your state Medicaid program for more eligibility information, as most states offer different types of Medicaid programs that may each have their own income limits and other qualifying criteria. Even if you make more than the standard limit found below, there may be additional programs for which you still qualify.
You May Like: What Eye Clinic Takes Medicaid
Arkansas Medicaid Eligibility And Enrollment
- What does Arkansas Medicaid offer? How is it different from Medicaid in other states? Find out how Medicaid in Arkansas works and how you can get it.
Arkansas Medicaid is a health care managed program for low-income individuals who need medical services but can’t afford them. The Arkansas Department of Human Services manages and administers the program for state residents who qualify. The agency works to improve the quality of life for all state residents while protecting vulnerable populations, such as children, older adults and those with developmental disabilities.
A typical applicant is:
- Under age 19 or 65 and older
- Blind, disabled or pregnant
- A parent or relative who serves as the caretaker of a child with an absent, disabled or unemployed parent
- Living in a nursing home
- Under age 21 and in foster care
- In medical need of certain home and community-based services
- A breast or cervical cancer patient
- Aged 19 through 64 with a household income below 138% of the federal poverty level
Income Limits In Arkansas For Medicaid
In Arkansas the individual receiving Medicaid cannot have income over $2,250. If their income is over that amount, they will need to do some Medicaid Planning to create eligibility. One strategy that works well is a Miller Trust . If an individual is married, the spouses income does not typically count towards the income cap, but it is important to maximize income protection via the Monthly Needs Allowance rules. The maximum amount of income the Medicaid office allows a community spouse to keep in Arkansas is $3,090 and the minimum amount is $ 2,003. All of an individuals monthly income must go towards their cost of care, which can include medical bills, prescriptions and other health care costs, aside from $40 which is for a personal needs allowance. The income limits are based as a percentage of the Supplemental Security Income defined by the Social Security Administrations Federal Poverty Levels and change every year.
You May Like: Can A Person Be Eligible For Both Medicare And Medicaid
What Is The Monthly Income Limit For Medicaid In Nc
The medically needy income restrictions are $242 for a single person and $317 for a married couple as of April 2021. In North Carolina, one has six months to fulfill their “Medicaid deductible,” or to “spend-down” their extra income to the Medicaid qualifying level. If they fail to do so, they will be dropped from the program.
Income limits for the general population start at $16,989 for an individual and $24,027 for a married couple filing jointly. These amounts increase annually with inflation. The income limit is sufficient to cover two percent of household income for any given year. For example, if your income is $60,000, you can expect to spend between $120 and $150 per month on health care.
There is also a maximum amount that an individual can earn before being required to file as part of the general population. This amount is currently $99,582. If an individual’s income exceeds this amount, they will be required to file as a high-income individual instead.
High-income individuals must file an annual tax return even if they don’t make enough to be eligible for other programs such as Medicare or Social Security. They also have more stringent eligibility requirements than those who qualify as low-income.
High-income status requires meeting a minimum threshold of income over two years in a row.
What Are The Different Types Of Care Available
The Medicaid programs available in each state are: regular Medicaid, Medicaid for long-term nursing home care, and Medicaid for home-based nursing care.
Regular Medicaid is the health care benefits program available to all of a states residents, providing they meet the eligibility requirements. Some of the eligibility requirements include:
- Legal status on the United States
- Resident of the state of application
Those who meet these criteria are able to use their regular Medicaid benefits for their doctors visits, hospital care, laboratory testing, and transportation for medical purposes.
The income limit for regular medicaid will be a set amount, depending on state and marital status. Some states allow one lump sum for a married couple and others have an income limit per spouse.
Medicaid for long-term nursing home care is for those who are elderly and can no longer live independently, those with chronic illness, and people with disabilities. At the facility, the residents receive 24/7 supervision and medical care, as well as lodgings and meals.
All state residents who meet the eligibility criteria and require long-term nursing home care are entitled to and will receive the care. There are no waitlists or lotteries for this benefit and you cant be denied if you meet the eligibility requirements.
Read Also: Can You Get Both Medicaid And Medicare
Medicaid Eligibility Program Overview
Medicaid pays for the cost of Nursing Home care in Arkansas that meet certain financial and health criteria. The average cost of Skilled Nursing Care in Arkansas is $58,860, so securing Medicaid coverage is essential. In Arkansas there are 242 Nursing Homes, of which 98% accept Medicaid insurance as a form of payment. The most expensive Nursing Home in Arkansas is Hudson Memorial Nursing Home which costs $300 per day and the least expensive Nursing Home is The Waters Of Stamps, Llc which costs $100 per day. Nursing Homes in Arkansas are currenlty 68.06% full with 17,618 patients currently using the 25,886 beds available.
To learn about the entire Medicaid eligibilty process, we have put together a comprehensive medicaid nursing home guide which you can read here.
Dont Miss: Blue Cross Blue Shield Medicaid Indiana
Lawsuit Over Arkansas Medicaid Work Requirement Was Slated For Scotus But Hearing Was Canceled And Work Requirement Waiver Was Then Rescinded By Hhs
The Trump administration appealed the case, as expected, and a panel of three judges on the U.S. Court of Appeals for DC heard oral arguments in the appeal in October 2019. During the arguments, all three judges expressed concerns about the coverage losses that stem from Medicaid work requirements, which was the crux of Boasbergs ruling earlier in the year that suspended the work requirement. And in February 2020, the three-judge panel unanimously ruled that it was arbitrary and capricious for HHS to approve the Arkansas Works waiver, and upheld Boasbergs ruling to overturn the states Medicaid work requirement. So the work requirement has remained suspended.
In July 2020, however, the Trump administration asked the Supreme Court to intervene and allow Arkansas to reinstate its work requirement once the COVID-19 situation is under control enough to allow the unemployment rate to return to normal levels. The Supreme Court justices agreed to hear the case, and oral arguments in the lawsuit, Arkansas v. Gresham, were scheduled for March 29, 2021 at the Supreme Court.
But the Biden administration does not support Medicaid work requirements, and asked the Supreme Court to cancel the hearing. That request was granted, and Arkansas v. Gresham was not heard by the Supreme Court.
You May Like: Does Medicaid Pay For Prescription Glasses
