I Am Covered Under Someone Elses Health Insurance Plan Will The Health Department Bill That Persons Insurance
Yes. Please note: Many health insurance providers send an Explanation of Benefits to the policy holder with details of the visit. The EOB will also show if a copayment is owed.
If you are concerned about the EOB being sent to the policy holder, you can contact your health insurance provider and ask for it to be sent to another address, or you can choose to pay for the visit yourself using the sliding scale.
Faqs: Health Insurance Billing And Fees At Sexual Health Clinics
The New York City Health Department asks for a fee for Sexual Health Clinic services given to adults . The Health Department must ask for insurance or payment for services to meet Medicaid standards and other legal requirements.
- If you want to use your health insurance to pay for the visit, your insurance plan will be billed. A copayment may be required.
- If you do not have health insurance or do not want your insurance billed for the visit, you will be asked to pay a sliding scale fee based on your family size and yearly income. You will not be asked for proof of family size or yearly income. No payments will be collected at the clinic.
If you do not have insurance or cannot pay the fee, you can still get services.
What Medicare Plans Cover Std Testing
Original Medicare consists of Medicare Part A and Part B. Medicare Part A is generally used to cover the costs of treatment in a hospital or a skilled nursing facility. Medicare Part B is most commonly used to cover STD testing and all other types of tests. If you do not have Original Medicare, Medicare Part C plans are also required to cover the same types of testing as Original Medicare. Also known as Medicare Advantage, these plans will cover STD testing at no cost for you. Medigap coverage is intended to provide assistance in paying copayments or deductibles for Medicare beneficiaries. Because STD testing is available at no cost through these plans, Medigap coverage is not applicable to these services.
In short, Medicare Part A, Medicare Part D and Medigap do not cover STD testing. Medicare Part A and Medicare Advantage plans, however, cover these services at 100% of your costs.
Read Also: Louisiana Medicaid Dental Coverage For Adults
How Much Does An Std Test Cost Without Insurance
The cost of an STD test without insurance will vary depending on the type of test and whether you choose to take the test in a clinic or at home. If you visit a clinic or doctors office to take an STD test, it may cost several hundred dollars without insurance.
Taking an at home STD test may be a better option if you dont have insurance. myLAB Box individual test kits for chlamydia+gonorrhea, trichomoniasis, HPV, syphilis, genital herpes, HIV, mycoplasma genitalium and hepatitis C are $79 each. We also offer combination test kits that test for multiple infections and are more cost-effective than purchasing individual test kits. Combination test kits are best for routine asymptomatic testing and testing when symptoms could indicate one of several different infections.
Std Treatment And Medicare Prescription Drug Coverage

Are you are enrolled in a stand-alone Medicare Part D Prescription Drug Plan or a Medicare Advantage Prescription Drug plan? Your plan might provide coverage for medications to treat STIs . As noted above, STD treatments often involve prescription medications.
While Medicare Prescription Drug Plans have formularies, or lists of covered drugs, medications used in the treatment of HIV are in a protected class. This means that Medicare plans offering prescription drug coverage must include all or substantially all drugs from this class in their formularies.
A plans formulary may change at any time. You will receive notice from your plan when necessary.
If youd like more information about your Medicare coverage and plan options for prescription drugs that might be prescribed to treat STDs, Im here to help answer your questions. To speak by phone or email, use the links below to set up a phone appointment or have me email information to you. To find plans right now, just click on the Compare Plans buttons on this page.
New To Medicare?
Becoming eligible for Medicare can be daunting. But don’t worry, we’re here to help you understand Medicare in 15 minutes or less.
Read Also: How Much Does Medicaid Pay For Hearing Aids
What Tests Are Covered By Medicare
Examples of STD screenings that are typically covered by Medicare Part B include:
- Chlamydia
- Syphilis
- Hepatitis B
Medicare Part B also covers up to two 20-30 minute face-to-face behavioral counseling sessions if you are sexually active and at increased risk for an STD.
STD stands for sexually transmitted disease. STI stands for sexually transmitted infection.
How Much Will My Std Testing Appointment Cost
The cost of STD testing will vary depending on where you choose to go, your income level, what kind of testing you require and your insurance coverage. Tests can cost as much as $300 from a private provider. You will pay nothing, however, if you choose to use Medicare to cover these treatments when they are ordered by your physician.
Don’t Miss: Medicaid Long Term Care Virginia
Medicare Coverage Of Std Screenings
Medicare covers a variety of preventive care services, including screenings for sexually transmitted diseases. STDs are also known as sexually transmitted infections, or STIs.
Medicare will cover STI screenings once a year if youre pregnant or at increased risk for an STI.
STD Screenings Covered by Medicare
- Chlamydia
Medicare also covers a free HIV screening each year for those who qualify.
You qualify for a free HIV screening if:
- Youre age 15 to 65
- Youre younger than 15 or older than 65 and at an increased risk for HIV
- Youre pregnant
Pregnant women can receive STI and HIV testing more frequently than other Medicare beneficiaries because the presence of an STI during pregnancy can result in significant health complications for the mother and child.
For example, Medicare coverage includes up to three HIV screenings for pregnant beneficiaries. This includes when the woman first learns she is pregnant during the third trimester and again during labor if ordered by the womans doctor.
Requirement For Documentation Of Reproductive Health Services
Revision 19-0 Effective July 1, 2019
All individuals should receive services related to reproductive health and/or contraception at least annually Individuals using long-acting reversible contraception and patients who have undergone permanent sterilization may continue to receive services under the program if they meet eligibility requirements. The guiding principle of the FPP is to improve the reproductive health of women and men to ensure that every pregnancy and every baby are healthy. At each patient encounter, including encounters for treatment of other conditions , the provider must educate the patient on how the service being provided relates to reproductive health or contraception, and this must be documented in the patient record.
For individuals who have undergone sterilization, and women who are post-menopausal or have had a hysterectomy, this counseling and documentation are not required when receiving covered services. This must be documented in the medical record at least annually.
Recommended Reading: Till What Age Does Medicaid Cover
How Long Does It Take To Get Std Test Results
Here at Rapid STD Testing, we offersame-day STD testing because we know getting your results as fast as possible is a top priority. After you give us a specimen, youll have the results in three days or less. All you have to do is log onto our secure server, and you can view them immediately.
Other testing methods arent as quick. While you wait anxiously for your results, your symptoms will most likely get worse. Thats why so many of our patients choose our testing servicesbecause they know theyll be able to get effective treatment as quickly as possible.
Prices And Payment Information
Please contact this health center for STD services pricing information.
Price ranges for our STD testing and treatment services and safer sex products are:
- condoms – FREE CONDOMS
Some services may have additional charges for lab and blood work.
Payment is expected at time of service unless other arrangements have previously been made.
Some STD testing and treatment services may be covered by your insurance. If you want to use your insurance, please be sure to bring in your insurance information at the time of your visit.
Medicaid, Medicaid Family Planning Benefits Program, and Medicaid for Pregnant Women accepted.
Medicaid managed care plans, however there may be limitations by county. The plans accepted at this Health Center Location are listed below:Humana Medical Plan CompMagellan Simply Healthcare SunshineStaywell/Wellcare/Healthease accepted.
If you are uninsured, you may be eligible to receive financial assistance for your procedure. You can confidentially find out if you qualify by calling us at.
If you are eligible for financial assistance you may be asked to bring documentation with you to the health center.
You May Like: What Do I Need To Qualify For Medicaid In Texas
Icd10 Code For Std Testing
ICD10 Coding for STD Testing
adudms said:my doctor sends in specimens to be tested for chlamydia and gonorrhea. we send in the requisitions with an ICD10 code of Z113. Quest has been sending letters stating: ” Need Additional ICD10 -limited covered test”. This in ONLY coming from tests covered by Molina Medicaid. Quest tells me they have nothing to do with it, it is from Molina. Molina doesn’t seem to know what to tell me. Is there some other ICD10 code I should be using on these requisitions?
How Much Do Std Tests Cost Without Health Insurance
The price of STD testing depends on the panel of tests you receive and whether theyre preventative or diagnostic. Generally, you can expect to pay anywhere from $50 to $500 for STD testing.
Another factor that affects cost is where you go for your STD testing. A popular place for low-income individuals and families is Planned Parenthood. While its a great option for many people, its not the best choice for everyone. Some people go to their doctors office, and some women choose to go to their gynecologist. Other people choose private STD clinics.
When you choose Rapid STD Testing, you can take advantage of our comprehensive testing panels and affordable pricing. The cost of our testing varies from around $100 to about $500 for thefull 10-panel STD test.
Recommended Reading: Does Medicaid Pay For Hospice Room And Board
Medicare Advantage And Sexually Transmitted Diseases Or Infections
If youre in a Medicare Advantage plan, you can still get an annual STI screening at no cost. Medicare Advantage plans must offer the same benefits as Medicare, but they can require you to use a healthcare provider in the plans network.
Prescription coverage is a feature of many Medicare Advantage plans. As with a standalone Part D prescription plan, you can expect your plan to cover many antibiotics and antivirals. Your prescription plan must cover antiretrovirals because theyre in a protected class.
Paying For Sti Prevention And Treatment Services
Access to prevention, screening, testing and treatment services for STIs is facilitated by private insurance, public coverage such as Medicaid and Medicare, as well as publicly-supported health programs. The CDC estimates that in 2008 , the annual direct medical costs in the US associated with STIs were nearly $16 billion.
Private Insurance
The Affordable Care Act requires most private health insurance plans to cover recommended preventive services, including HIV and other STI screening, with no cost sharing. For adults, this includes US Preventive Services Taskforce recommendations receiving an A or B grade, which include vaccines recommended by the CDCs Advisory Committee for Immunization Practices, and services for women recommended by the Health Resources and Services Administration . STI-related services that must be covered without cost-sharing by most plans are presented in Table 2.
In June 2019, the USPSTF Task Force added an A grade recommendation for PrEP for the prevention of HIV in high-risk populations, which means that most insurance plans must begin covering the full cost of the drug in the plan year that starts after June 2020. CDC guidelines on PrEP advise that individuals on PrEP have follow up visits and lab work, including being re-tested for HIV four times a year, but it is unclear whether these follow-up visits and lab work must be covered without cost-sharing by most insurance plans.
Medicaid
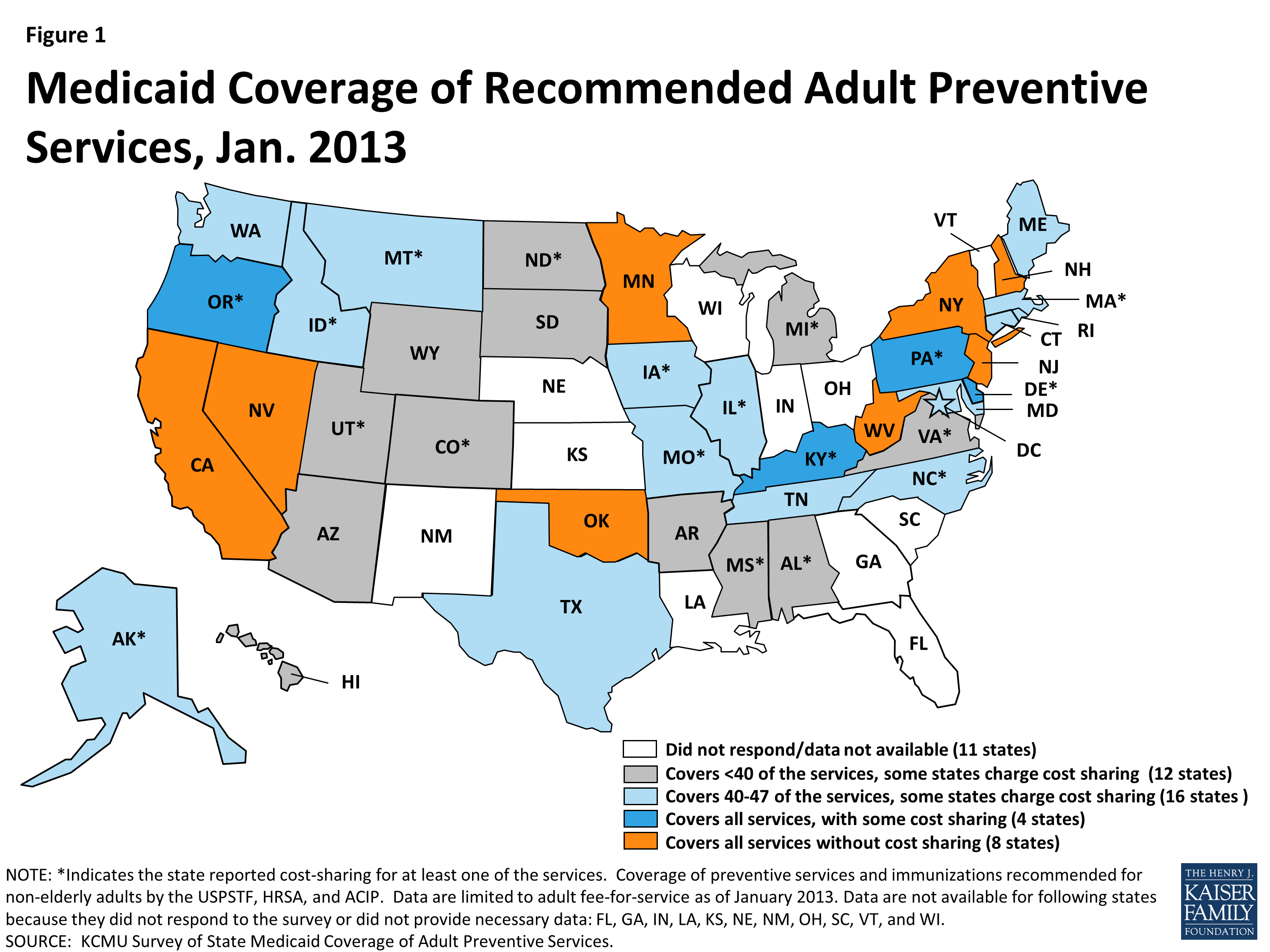
Medicare
Services and Programs for Uninsured Individuals
Recommended Reading: Apply For Montana Medicaid Online
Family Planning Program Policy Manual
Revision 19-0 Effective July 1, 2019
This section describes the requirements and recommendations for FPP contractors pertaining to the delivery of direct clinical services to patients. In addition to the requirements and recommendations found within this section, contractors should develop protocols consistent with national evidence-based guidelines appropriate to the target population.
All providers must offer the following core family planning services:
- Contraceptive services
- Intrauterine devices , contraceptive implants, oral contraceptive pills, three-month injections, sterilizations, etc.
Is Std Testing Covered By Insurance
Insurance plans usually cover STD testing at your doctors office or at an STD testing clinic, but the specifics of this coverage will vary by insurance company.
The five largest insurance providers will cover:
- United Health Group gonorrhea, chlamydia, syphilis and HIV testing for women. HPV DNA testing is also provided to women over the age of 30. HIV testing is covered for men, but no other information for men is given.
- Anthem sexually transmitted disease screening as needed for sexually active persons. STD screenings for pregnant women are also covered.
- Aetna yearly STD testing coverage
- Humana STD testing is not featured in the preventive care section
- Cigna chlamydia and gonorrhea screening for women under 24 or older women if they are at high risk. HIV screening for pregnant women, teens and adults between 15 to 64 years old, at-risk older adults, and sexually active women.This insurance provider also covers HPV DNA testing for women who are 30 years of age or older.
Under the Affordable Care Act , chlamydia and gonorrhea preventive screenings are free for women under 24 (older women are also covered if they are high risk. ACA also covers HIV and syphilis screenings for sexually active men and women. No other STD screenings are mentioned.
Read Also: Does Medicaid Cover Incontinence Pads
Does Medicare Cover Hiv Testing
Medicare covers an annual HIV screening test for everyone aged 15-65 whos on Medicare. It also pays for a yearly screening for younger or older people at risk of contracting the virus. If youre pregnant, you can have up to three screenings during your pregnancy.
HIV testing is preventative service. You wont pay anything for the test as long as your provider accepts Medicare assignment.
What Are The Benefits Of Using Insurance For Std Testing
STD testing with insurance lowers the cost of being tested. If cost is a barrier, it is definitely better to test with insurance than not to test at all. Read more here.
But remember, insurance will not cover every type of STD testing. Its important to read through your policy to determine which types of STD testing are covered by your provider.
Read Also: United Health Care Managed Medicaid
Can Urgent Care Really Help Me With An Std Test
The short answer is, yes! Many people who are looking for routine or precautionary STD tests visit urgent care facilities instead of a private practice or their primary care physician. Urgent care facilities are a great option if you are concerned that you may have contracted an STD and need to see a physician.
If you are sexually active, it is best practice for you and your partner to receive regular STD tests, even if youre both taking precautionary steps to avoid receiving and transferring STDs. Many STDs spread through body fluids, such as blood, vaginal fluids, or semen. While condoms are 98% effective in preventing transferring STDs like chlamydia and gonorrhea that are spread through body fluids, they do not protect against STDs that spread from skin-to-skin contact, like genital warts, herpes, and syphilis. Some STDs hide in plain sight and do not show symptoms, so you may not know you have one. The best thing for you and your partner to do is to get tested once every three to twelve months, depending on your level of sexual activity to ensure that you are STD free.
Prevalence Of Sexually Transmitted Infections

While women still account for the highest reported cases of STIs , men, in particular gay and bisexual men, saw greater increases in rates of syphilis, chlamydia, and gonorrhea in recent years. Syphilis infection rates nearly doubled among men from 2014 to 2018 .
| Table 1: Sexually Transmitted Infection Rates of Reported Cases, by Selected Characteristics, 2018Rate per 100,00 population | |
| 48.5 | 9.3 |
| NOTES: NR is Not Reported. Primary and secondary syphilis stages are the earliest stages of infection, reflect symptomatic disease, and are indicators of incident infection.SOURCE: Centers for Disease Control and Prevention , Sexually Transmitted Disease Surveillance 2018 CDC, Diagnoses of HIV Infection in the United States and Dependent Areas, 2018. |
Figure 1: Rates of sexually transmitted infections by sex from 2014 to 2018
Congenital syphilis rates increased 173% between 2014 and 2018, with the number of cases the highest they have been since 1995. The highest rates of congenital syphilis were in the South, West, and Southwest .
Figure 2: The highest rates of reported congenital syphilis are in the western and southern U.S.
STIs also have a disproportionate impact on young people, ages 15-24, who acquire half of all new STIs, despite only representing 25% of the sexually active population . Young people, ages 15-24, account for 60% of all reported cases of gonorrhea and chlamydia.
Figure 3: Young people bear a disproportionate burden of gonorrhea and chlamydia infections
Recommended Reading: How To Qualify For Medicaid In Nevada
