What Is The Ohio Income Limit For Food Stamps
In fact, Ohios food stamp income limit depends on the household size. For example, for one person, the annual income should not exceed $ 16,744. For a household of 3, the maximum annual income is $ 34,450. To find out the income limit for your household you should visit Ohio Office of Family Assistance or call 1-866-244-0071.
If you are unemployed you are also eligible for food stamps. However, this will only work if you do not specifically quit your job in order to meet the requirements.
How To Apply For Medicaid In In Ohio
Multiple methods exist for applying for Ohio Medicaid. Many people have taken to the online version which is fast to use and initiates a quick response. A pop-up window comes on the screen when attempting to start a new application. It allows users to either sign in with an existing account or create an account if it is their first time. Provide a first and last name, date of birth, and social security number to sign up and start the process.
Those who do not wish to use the online version may instead visit their local office to fill out a paper form. It can get submitted directly to a worker who can assess the information and approve or deny the claim. It is also possible to apply by telephone by calling the Ohio Medicaid Consumer Hotline at 324-8680.
Can Pregnant Or New Parent Get More Food Stamps
You cannot get more food stamps while you are pregnant, but you have another option that you can use. Apply for Woman, Infants, Children benefits . The WIC Program provides meals and supplies for pregnant women, young parents and children under 5 years old.
However, after the baby is born, you will be able to get more food stamps as the size of your household will be increased.
Recommended Reading: Medicaid For Pregnant Non Citizens
Medicaid Eligibility In Ohio
Funded by both the federal and state government, the health insurance program known as Medicaid was designed with low-income families in mind. Children, elderly, and disabled members of society are often first among the list of eligible applicants in the state of Ohio. Before applying, it is important to note the states specific criteria for getting approved and accepted into the program to receive coverage.
What Is The Medicaid Income Limit In My State
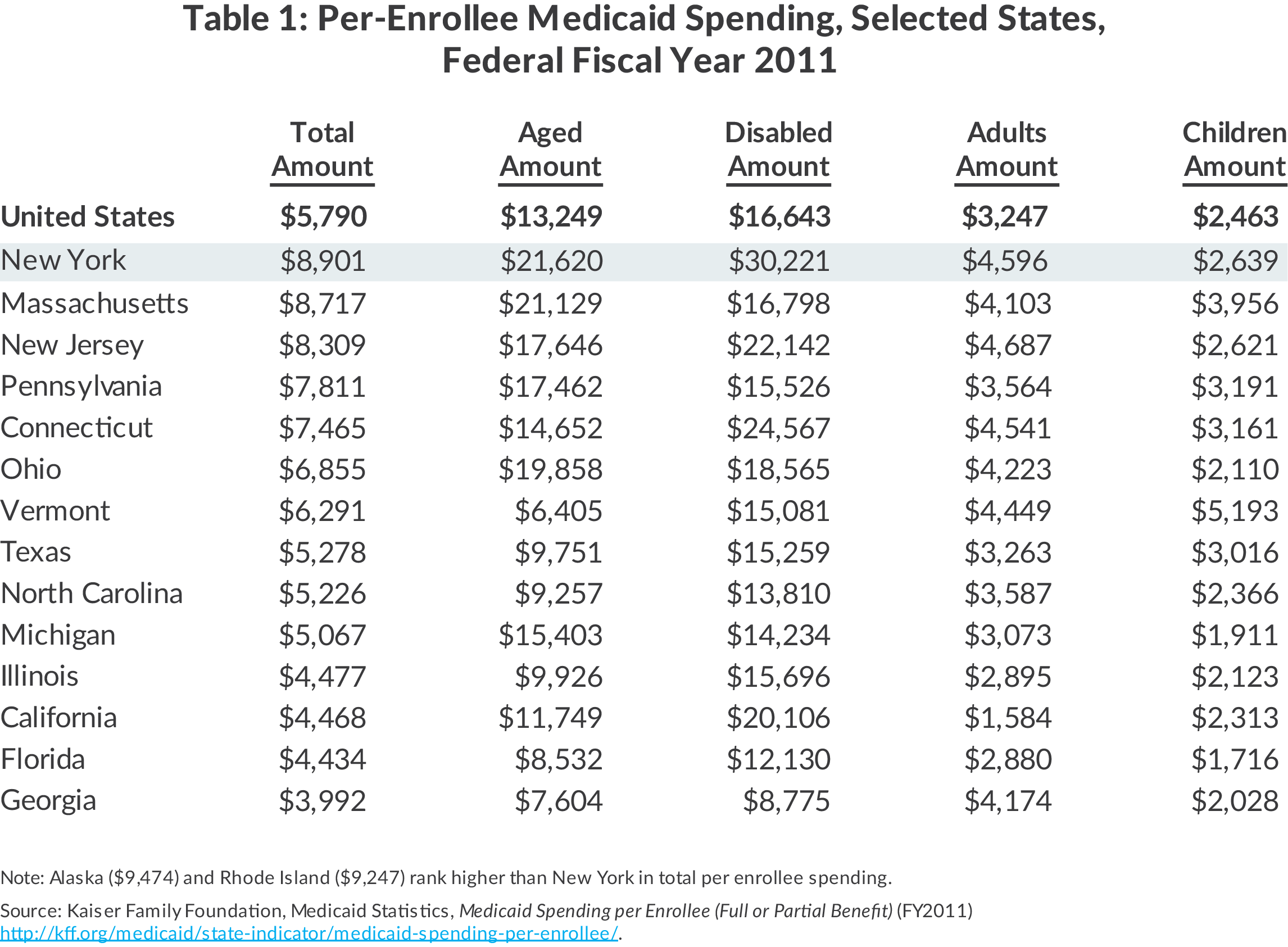
Most states use a standard of 138% of the federal poverty level as a basis for Medicaid eligibility. But each state is free to set its own limits.
The table below shows the income limit as a percentage of the FPL required for Medicaid eligibility in each state for two-parent households and for individuals adults.
If 0% appears, that means individuals may not qualify for Medicaid in that state based on income alone and must meet other criteria, such as being pregnant or disabled.
Medicaid Income Limit by State|
State |
|
|---|---|
| 52% | 0% |
FPL is used to determine eligibility for Medicaid, certain welfare benefits and other assistance programs. The FPL is computed by the U.S. Census Bureau and can be adjusted every year based on inflation.
Medicaid uses a percentage of the FPL to determine its income limits for eligibility. For example, you may qualify for Medicaid if you earn less than 133% of the federal poverty level. Or you may qualify if you earn less than 150% of the federal poverty level and are disabled. Again, each state sets its own income limits to determine Medicaid eligibility.
Contact your state Medicaid program for more eligibility information, as most states offer different types of Medicaid programs that may each have their own income limits and other qualifying criteria. Even if you make more than the standard limit found below, there may be additional programs for which you still qualify.
Don’t Miss: How Can You Protect Your Assets From Medicaid
How Much A Spouse Can Keep In Ohio
If you have a spouse who is going to continue to live independently, then Ohio will allow you and your spouse to keep more income and assets to support that spouse.
Your spouse will be allowed to keep some income each month. The amount will depend on how many dependents and expenses he or she has. In 2019, the minimum monthly Community Spouse Income Allowance is $2,057.50, and the maximum is $3,160.50.
Ohio assumes that half of the assets that you had at the time of your first admission to a nursing home ) should belong to your spouse, subject to a limit that changes annually. For married couples, as of 2019 the CSRA is up to a maximum of $126,420. When you apply for Medicaid, ODJFS will tell you how much your community spouse is entitled to keep.
When you apply for Medicaid, your CSRA is subtracted from your countable assets at the time of your application. For example, say Mr. and Mrs. Johnson have $80,000 in countable assets when he moves into a nursing home on February 1st. Mrs. Johnson continues to live in the couple’s home. On that date, Mrs. Johnson’s CSRA is calculated to be $40,000. The Johnsons use their savings to pay for Mr. Johnson’s nursing home care until December 1st, when he applies for Medicaid. On December 1st, Mr. and Mrs. Johnson have $40,000 left in countable assets. Because Mrs. Johnson’s CSRA is $40,000, she is entitled to keep the $40,000. Mr. Johnson then has no countable assets, and he meets the resource eligibility criteria for Medicaid.
Asset Requirements & Limits
Ohio Medicaid for long-term care requires all applicants to demonstrate financial need in order to receive benefits. To determine a persons financial eligibility, Medicaid takes their resources into consideration. Medicaid expects applicants to liquidate their assets to pay for their care, and will not step in until their resources fall within the asset value requirements.
The asset limit in Ohio for a single Medicaid applicant is $2,000. Married applicants are subject to different limits, which are determined on a case-by-case basis. Assets are considered jointly, and if a Medicaid applicants spouse intends to continue living independently , they may keep a portion of the couples assets to protect them from spousal impoverishment. The amount of assets the spouse may keep is known as the Community Spouse Resource Allowance .
Medicaid divides assets into two categories: countable, and exempt. Countable assets are those which count toward a persons asset limit, including stocks, bonds, and annuities. Exempt assets are not available for Medicaids consideration, and will not count toward a persons asset limits. Medicaid does not expect a person to liquidate their exempt assets to pay for their long-term care, however they do expect all countable assets in excess of $2,000 to be put toward care costs.
Dont Miss: Medicaid Eligibility Income Chart Florida
Also Check: Find Primary Care Doctor Medicaid
Income Requirements & Limits
Medicaid uses a persons monthly income in addition to their assets in order to determines their eligibility for benefits. A persons income is defined as the amount of money they receive on a monthly basis, including wages, Supplemental Security Income , child support, and other types of earned and unearned income. Like assets, some types of income are counted toward a persons income limits, and others are exempt from consideration.
When Medicaid calculates a persons income, they use their Modified Adjusted Gross Income as opposed to their gross or net income. By using the MAGI, Medicaid aims to create a more accurate depiction of a persons financial outlook to determine if they qualify for benefits. Unliked other income figures, the MAGI takes a persons gross income , their foreign income, and any deductions from their IRA to calculate how much income a person generates in total.
The income limit for Medicaid long-term care benefits in Ohio is equal to 300 percent or less of the SSI Federal Benefit Rate . In 2018, the FBR is $750, meaning an Ohio Medicaid applicant may retain up to $2,250 of exempt income without disqualifying themselves from Medicaid. However, Ohio Medicaid does not have an income cap, meaning applicants with income above the $2,250 limit may still qualify for benefits under certain circumstances.
The Following People Or Groups Will Not Use The New Magi Rules To Determine Eligibility:
- People not subject to an income decision by Medicaid including children in foster care and individuals found eligible under the Breast and Cervical Cancer Project
- Medicare-age adults seeking Medicaid due to medical needs caused by age
- Qualified Medicare Beneficiaries
- Individuals certified as blind or disabled by the Social Security Administration
- People seeking Long-Term Care
*This list is a general guideline there are some situations where an individual can be considered in more than one Medicaid program category. This includes an applicant being eligible for both a MAGI and Non-MAGI program category. If you think you or the applicant you are working with may fall into more than one category, please visit Morrow County Job and Family Services or by visiting www.benefits.ohio.gov, you can apply for Medicaid only, without applying for other programs that are offered.
Read Also: How Do I Qualify For Medicare And Medicaid
What To Do If You Dont Qualify For Medicaid
If you dont qualify for Medicaid, you can possibly get subsidized health care through the Obamacare marketplaces during a special enrollment or open enrollment period. Americans who making more than 100% of the FPL qualify for a premium tax credit that can significantly lower the cost of a plan.
Federal open enrollment for 2022 health care plans runs until Jan. 15, 2022, though some state exchanges are open longer. Learn 2022 open enrollments dates by state. Healthcare.gov, the federal exchange, usually opens from November 1 to December 15 each year.
If you cant find affordable health care on your marketplace during open enrollment, you have a few back-up options.
These include:
Short-term health insurance: Originally designed to prevent short-term health insurance gaps, these plans are cheaper, but much less comprehensive than traditional coverage. They dont have to cover Obamacares 10 essential benefits or pre-existing conditions. Following changes by the Trump administration, short-term health plans can last from three months to potentially three years, though som estates have stricter limits.
Limited benefit plans: These plans cover a very small portion of the costs associated with certain medical events, like a doctors visit or ambulance ride. Both the number of events and dollar amounts covered are capped.
Prescription discount cards: While these cards wont help you pay for inpatient or outpatient care, they do help you get medication at discounted rates.
Ohio’s Medicaid Income Limit
If you are 65 or older, blind, or disabled, and you need long-term care in a nursing home, then you must have income at or below $2,313 per month to qualify for Medicaid. The 2019 monthly income limit for a married couple with both spouses applying is $4,626.
If your income is above the limit, you still might be able to qualify for Medicaid if the income you have over the limit doesn’t cover your medical expenses. In Ohio, unlike some other states, people who are sixty-five and older, blind, or disabled can use unpaid medical bills, premiums, or nursing facility bills to “spend down” their income and qualify for Medicaid. A worker from ODJFS will determine how much your monthly spend-down amount is. You have to satisfy the spend-down to be eligible for Medicaid each month. You can satisfy your spend-down by showing proof that your medical expenses equal the spend-down amount or by paying the amount directly to ODJFS.
You May Like: Is Invisalign Covered By Medicaid
A 2020 Medicaid Income Limits
In 2020, the maximum total monthly income from all sources that a person seeking Medicaid may have is $2,349 . If a Medicaid applicant has income greater than this amount, it is necessary to establish a Qualified Income Trust. A Qualified Income Trust is a special kind of legal instrument used for Medicaid eligibility purposes. Any income over the $2,349 limit that is placed into this Trust will be disregarded for Medicaid application purposes. Thus, a person who has income greater than the limit may still qualify for Medicaid.
Once an individual is approved for Medicaid, all of the individuals income, including any income that was placed in the Qualified Income Trust, must be used to pay for their care before Medicaid covers the balance. Medicaid allows a person to retain only $50 of income for their personal use. If the individual is married, a portion of the individuals income may be paid to the individuals spouse, if the spouses monthly income is below $2,113.75.
Learn About Requirements For Medicaid In Ohio
Applicants often ask, What are the requirements for Medicaid in Ohio? as the state and federally funded program is known to have various qualifications that applicants must meet in order to receive Medicaid benefits eligibility. However, before learning how to qualify for Medicaid in OH, it is important to note that the program is intended for low-income families and individuals who do not receive health insurance through work and cannot afford to purchase private health insurance. As such, income is a major factor in determining who is eligible for Medicaid, but income requirements only make up one portion of the established qualifications. To find out more about the Medicaid eligibility requirements in Ohio, and to obtain answers to important questions like, What are the income requirements for Medicaid? review the sections provided below.
Who qualifies for Medicaid in Ohio?
Note: For applicants who do not meet Medicaid eligibility requirements due to their gross-income amount but still require health insurance for infants or expectant mothers, consider the Ohio CHIP program. Additionally, similar to the CHIP program, Ohio also offers other medical assistance benefits to the disabled and the elderly who make more than the income limit required by Medicaid.
How do I qualify for Medicaid in Ohio?
What are the Medicaid application guidelines in Ohio?
What are common Medicaid disqualifications in Ohio?
Read Also: Dentist That Take Medicaid In Idaho Falls
Medicaid And Medicare Dual Eligibility
If you qualify for both Medicare and Medicaid, you are considered dual eligible. In this case, you may qualify for a certain type of Medicare Advantage plan called a Dual Eligible Special Needs Plan . D-SNPs are designed to meet the specific needs of people who have Medicaid and Medicare.
You can compare plans online to find out if D-SNPs are available where you live, or you can call to speak with a licensed insurance agent for information about eligibility and enrollment.
I Introduction To Medicaid Guide
Do you know someone who has spent time in a nursing home? Have you ever thought it could be you?
Most people answer the first question yes, and the second question no. It is one of those situations where we believe it could never happen to me. However, studies show that approximately 70% of those age 65 or older will need some type of long-term care prior to death. By 2020, an estimated 12 million older Americans will need some form of long-term care.
Recommended Reading: Can I Have Medicare And Medicaid Together
You May Like: Can A Pregnant Woman Get Medicaid
Ohio Medicaid Eligibility Requirements
To qualify for long-term care benefits through Medicaid in Ohio, a person must meet the states financial and medical eligibility requirements. Many seniors choose to reside in a nursing home or receive other types of long-term care without a doctor ordering them to do so, and Medicaid will not cover any voluntary care services. An applicant must prove they require the care they want Medicaid to cover before they may receive benefits. Additionally, they must prove they cannot pay their medical bills alone and require financial assistance to receive care.
What Is The Highest Income To Qualify For Medicaid
Washington D.C. has the highest allowable income to qualify for Medicaid, at 215% of the FPL for individuals and 221% for a family of three.
That means an individual in Washington D.C. can make up to $27,692 per year and still be eligible for Medicaid. Washington D.C.s high cost of living factors into its higher income limit for Medicaid. No other state uses more than the standard 138% limit for individuals.
A family of three can make up to $48,531.60 and still qualify for Medicaid in Washington D.C. Connecticut is the only other state to use a limit higher than 138%.
Recommended Reading: How To Find Out If I Qualify For Medicaid
Medicaid If You Are 18 Or Younger
If you are 18 or younger, you may qualify for income-based Medicaid if your familys income is 211% of the Federal Poverty Guidelines or less . It doesn’t matter how much your family has in resources or whether you have a disability. Note: Income-based Medicaid for children 18 and younger is sometimes called “Healthy Start.”
Check whether your family’s income is low enough for you to get income-based Medicaid:
Your family size:| Income limits for your family: | |
| $13,590 | |
| Income-based Medicaid, adults | |
| Income-based Medicaid, children | |
| Subsidized private plans, reduced fees | |
| Subsidized private plans | — |
If your family’s income is at or below the limit for a program, you may qualify if you meet other program rules.Notes:
|
Note: Some young people with disabilities who don’t get SSI and don’t qualify for income-based Medicaid may still qualify for disability-based Medicaid. If you have any questions about this, talk to a benefits planner.
How Much Does Medicaid Cost In Ohio
More than $21 billion gets spent on Ohio Medicaid costs. The federal government shares these expenses with the state, with Ohio allocating over 37 percent of their budget to its funding. This amount will only grow over time, as there are plans to expand the program to ensure more people who need coverage can receive it.
Also Check: How To Find Case Number For Medicaid
