Can I Get Help With My Prescription Drugs
For many people, prescriptions are their number one health care cost. There are several ways that low-income people with both Medicare and Medicaid benefits can get extra help with their prescriptions. The first and most important way is to apply for the Social Security Administrations Extra Help program. This program provides low-income subsidies program helps Medicare beneficiaries pay for their Medicare Part D prescription drugs by paying some of the costs. Also known as “Extra Help”, beneficiaries who qualify for LIS receive premium…) to those who need them. These subsidies can help you pay all or part of the monthly premium for a Medicare Part D plan, and is worth about $5,000 per year. You will need to call Social Security directly at 1-800-772-1213 to check your eligibility.
If you are able to enroll in a Special Needs Plan, your SNP will include prescription drug coverage and pay many of the out-of-pocket costs with regular Medicare Advantage plans. Enrollees pay small copayments, but you dont have an annual deductible. You can use our SNP directory to discover enrollment opportunities in your area.
Understanding What The Two Programs Are
September 23, 2021
Category: Educational, Medicare Healthcare
Just when you think that Medicare itself cannot get any more confusing, it does. But, for some Americans, it becomes more confusing in a positive way. For many Americans who are close to retirement and qualify for Medicaid health assistance, the question about whether they will also qualify for Medicare health insurance is one theyre likely to consider, especially if they dont have the answer. And if its still a question you have, you can rest easy knowing that it will be answered by the end of this article.
This article is intended to answer your question about whether you qualify for both Medicare and Medicaid, what each is, how you can qualify for the two services and what their overall differences are.
Lets get into it by first understanding what the two programs are.
Extra Help Program For Medicare Part D
Medicaid is not the only government-sponsored resource that helps pay for medical costs. An individual can also apply for Extra Help, a program that helps beneficiaries with Medicare Part D, which covers prescription drug costs.
To qualify for Extra Help, a personâs combined investments, real estate, and savings must not exceed $29,160 if a person is married and living with their spouse or $14,610 if a person is single.
A person can visit Medicareâs website to find out more about getting and applying for Extra Help.
Don’t Miss: Dentist In Lafayette La That Accept Medicaid For Adults
Medicaid Vs Medicare: You Can Have Both
Posted: January 17, 2020
Medicaid and Medicare. Its hard to think of two words that cause as much confusion.
- Whats the difference between these two government health insurance programs?
- What exactly are Medicaid and Medicare?
- Whos eligible to get Medicaid or to get Medicare?
- And how can some people get both?
Read on to find out the answers to these questions and more.
How Do I Know If I Should Be Dual Eligible
Beneficiaries can find out if theyre eligible for Medicaid by contacting their Medicaid office. An Internet search for Medicaid offices in a beneficiarys state should provide the number to call but beneficiaries should make sure they are contacting a government office before sharing any personal information.
The Centers for Medicare and Medicaid Services also maintains a list of state agencies that oversee Medicaid. Beneficiaries can see if they already have Medicaid by contacting 1-800-MEDICARE and asking whether they receive Extra Help with their prescription drug costs .
Also Check: Dentist In Montgomery Al That Accept Medicaid
When To Enroll In Medigap
You may only purchase Medicare Supplement Insurance during your open enrollment period. This is a six-month period immediately following your 65th birthday and only after you have enrolled in Medicare Part B.
The enrollment period cannot be changed or repeated. Once the enrollment period ends, you may no longer be able to enroll in a Medigap policy. If you are able, it may cost you more.
Medigap insurers are not allowed to charge you more for a policy if you have pre-existing conditions and cannot ask you about your family medical history.
How Do I Know If I Qualify For Medicaid And Medicare
Twelve million individuals are currently enrolled in both Medicaid and Medicare.1 These individuals are known as dual eligible beneficiaries because they qualify for both programs. As long as you meet the federal qualifications for Medicare eligibility and the state-specific qualifications for Medicaid eligibility, you will qualify as a dual eligible. To qualify for Medicare, individuals generally need to be 65 or older or have a qualifying disability.
There are several levels of assistance an individual can receive as a dual eligible beneficiary. The term full dual eligible refers to individuals who are enrolled in Medicare and receive full Medicaid benefits. Individuals who receive assistance from Medicaid to pay for Medicare premiums or cost sharing* are known as partial dual eligible.
*Cost sharing is the amount of your health care that you pay out of your own pocket. Typically, this includes deductibles, coinsurance, and copayments.
Don’t Miss: Medicaid Requirements For Gastric Sleeve
What If I Need To Be In A Nursing Home
Medicare covers most of the costs associated with skilled nursing after an inpatient stays in the hospital. If you have both Medicare and Medicaid, a stay at a skilled nursing facility will cost very little.
After inpatient treatment, many patients need more outpatient care in the home setting. To learn how to get financial assistance for home health care, read How to Qualify for Home Health Care & Get Financial Assistance.
If you require assisted living because you are no longer able to live independently, read Does Medicare Cover Assisted Living Costs? What About Independent Living?
If you need long-term care and have limited resources, Medicaid can help, however, strict asset limits do apply. We have a complete guide to long-term care if you need it.
What Does Medicare And Medicaid Pay For
Medicaid is known as the payer of last resort. As a result, any health care services that a dual eligible beneficiary receives are paid first by Medicare, and then by Medicaid. For full dual eligible beneficiaries, Medicaid will cover the cost of care of services that Medicare does not cover or only partially covers . Such services may include but are not limited to:
- Nursing home care
- Dental services
- Eye examinations for prescription glasses
The financial assistance provided to partial dual eligible beneficiaries is outlined in the table above.
Recommended Reading: How To Cancel Medicaid In Virginia
Health Services Not Covered By Medicare
Medicare is not an all-inclusive program. With rare exceptions, Original Medicare does not cover dental, hearing, and vision screening. That leaves beneficiaries to scramble for dentures, hearing aids, or corrective lenses . People who decide to enroll in Medicare Advantage may choose a plan that offers coverage for some of these services.
If your state Medicaid program offers these services, you may benefit from the added coverage. Not all states will offer coverage and if they do, it may not be available to everyone who qualifies for Medicaid.
Understanding Medicare And Medicaid
Medicare is health and hospitalization insurance for people age 65 and older and those under 65 with certain disabilities or end-stage renal disease. Some portions of Medicare are free and others cost money, with premiums typically deducted from your Social Security benefit checks.
Even if you have private insurance you should apply for Medicare. If you wait until after your 65th birthday to apply, you may end up paying a late penalty or higher premiums. For most people, the initial enrollment period is the seven-month period that begins three months before the month in which they turn 65. If you miss that window, you may enroll between January 1 and March 31 each year, although your coverage won’t begin until July 1.
There are four types of Medicare coverage available.
Don’t Miss: Florida Department Of Children And Families Medicaid
Can One Have Dual Eligibility For Both Medicare And Medicaid
Yes, Medicare and Medicaid are not mutually exclusive programs. Persons who are eligible for both are referred to as having Dual Eligibility, Dual Eligibles, or often simply Duals. Medicare is the first payer of covered benefits, while Medicaid is the secondary payer. Typically, Medicaid will pay for Medicare premiums and co-payments for dual eligibles. In fact, many states have special programs intended to make it easier for seniors to manage their dual eligibility status as it can be confusing to know where to turn for what services. This is generally in the form of managed care.
There are also programs called Medicare Saving Programs for low-income seniors that dont quite qualify for Medicaid.
Medicare Eligibility At 65 And Older

The year you turn 65, you can apply for Medicare starting three months before your birth month until three months after. You generally have to meet three eligibility requirements to qualify for full Medicare benefits when you turn 65.
The chief requirement is that you must be a U.S. citizen or permanent legal resident who has lived at least five years in the United States.
In addition, you have to meet one of the following other requirements:
- You or your spouse must have worked long enough to also be eligible for Social Security benefits or for railroad retirement benefits. This usually means youve worked for at least 10 years. You must also be eligible for Social Security benefits even if you are not yet receiving them.
- You or your spouse is either a government employee or retiree who did not pay into Social Security but did pay Medicare payroll taxes while working.
Paying Medicare payroll taxes for 10 full years means you wont have to pay premiums for Medicare Part A, which covers hospital care.
You dont need the work credits to qualify for Medicare Part B, which covers doctor visits or outpatient services, or Medicare Part D, which covers prescription drugs. But everyone has to pay premiums for both.
You can still get Medicare if you never worked but it may be more expensive depending on your spouse or total work history.
Prepare for the Medicare Advantage Open Enrollment Period
Recommended Reading: Does Medicaid Cover Gastric Bypass In Michigan
How To Qualify For Medicare And Medicaid
Beneficiaries can enroll in Medicaid through the state program office. If you think youre eligible, contact your state health department to apply. To be eligible for Medicaid your income will need to be below a predetermined amount.
If your income is above this amount but you struggle with high medical costs, you may want to check if a Medicaid spend-down program is available in your state.
Youre eligible for Medicare if youre over the age of 65 or on disability for at least 24 months. Although, you apply for Medicare online at the Social Security Administration website.
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comuníquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
Recommended Reading: What Is Family Planning Medicaid Nc
Dual Eligible Special Needs Plans
In some states, dual eligible beneficiaries may have the option of enrolling in a D-SNP, which is different from a traditional SNP or Special Needs Plan. These plans are specially designed to coordinate the care of dual eligible enrollees. Some plans may also be designed to focus on a specific chronic condition, such as chronic heart failure, diabetes, dementia, or End-Stage Renal Disease. These plans often include access to a network of providers who specialize in treating the specified condition. They may also include a prescription drug benefit that is tailored to the condition.
Unitedhealthcare Senior Care Options Plan
UnitedHealthcare SCO is a Coordinated Care plan with a Medicare contract and a contract with the Commonwealth of Massachusetts Medicaid program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is a voluntary program that is available to anyone 65 and older who qualifies for MassHealth Standard and Original Medicare. If you have MassHealth Standard, but you do not qualify for Original Medicare, you may still be eligible to enroll in our MassHealth Senior Care Option plan and receive all of your MassHealth benefits through our SCO program.
Don’t Miss: Is Wisdom Teeth Removal Covered By Medicaid
What Is The Texas Health Information Counseling And Advocacy Program
If you are eligible for Medicare, the Texas’ Health Information, Counseling and Advocacy Program can help you enroll, find information and provide counseling about your options. This partnership between the Texas Health and Human Services system, Texas Legal Services Center and the Area Agencies on Aging trains and oversees certified benefits counselors across the state.
What Are Dual Special Needs Plans
Dual health plans are also known as dual special needs plans. Theyre offered by private insurance companies, so you can find a dual health plan that best meets your health insurance needs. Being on a dual health plan does not change your Medicaid eligibility or benefits.
See UnitedHealthcare plans in your area.
Please note that the specific benefits dual health plans include can change depending on where you live. Search by your ZIP code to find the right plan to meet your health care needs.
Resource Center
Were here to help.
Contact us at:
Were here to help.
Contact us at:8 a.m. to 8 p.m. local time, 7 days a week.
Looking for the federal governments Medicaid website? Look here at Medicaid.gov.
Read Also: If I Have Medicaid Do I Qualify For Food Stamps
What If Im Turned Down By Medicaid
- You may be able to buy a private health plan through the Marketplace instead for the 2018 plan year in the fall. You may qualify for savings based on your income through a premium tax credit and savings on out-of-pocket costs.
- If you don’t qualify for either Marketplace or Medicaid savings, you still have options. Learn more here.
Who Can Get Medicaid
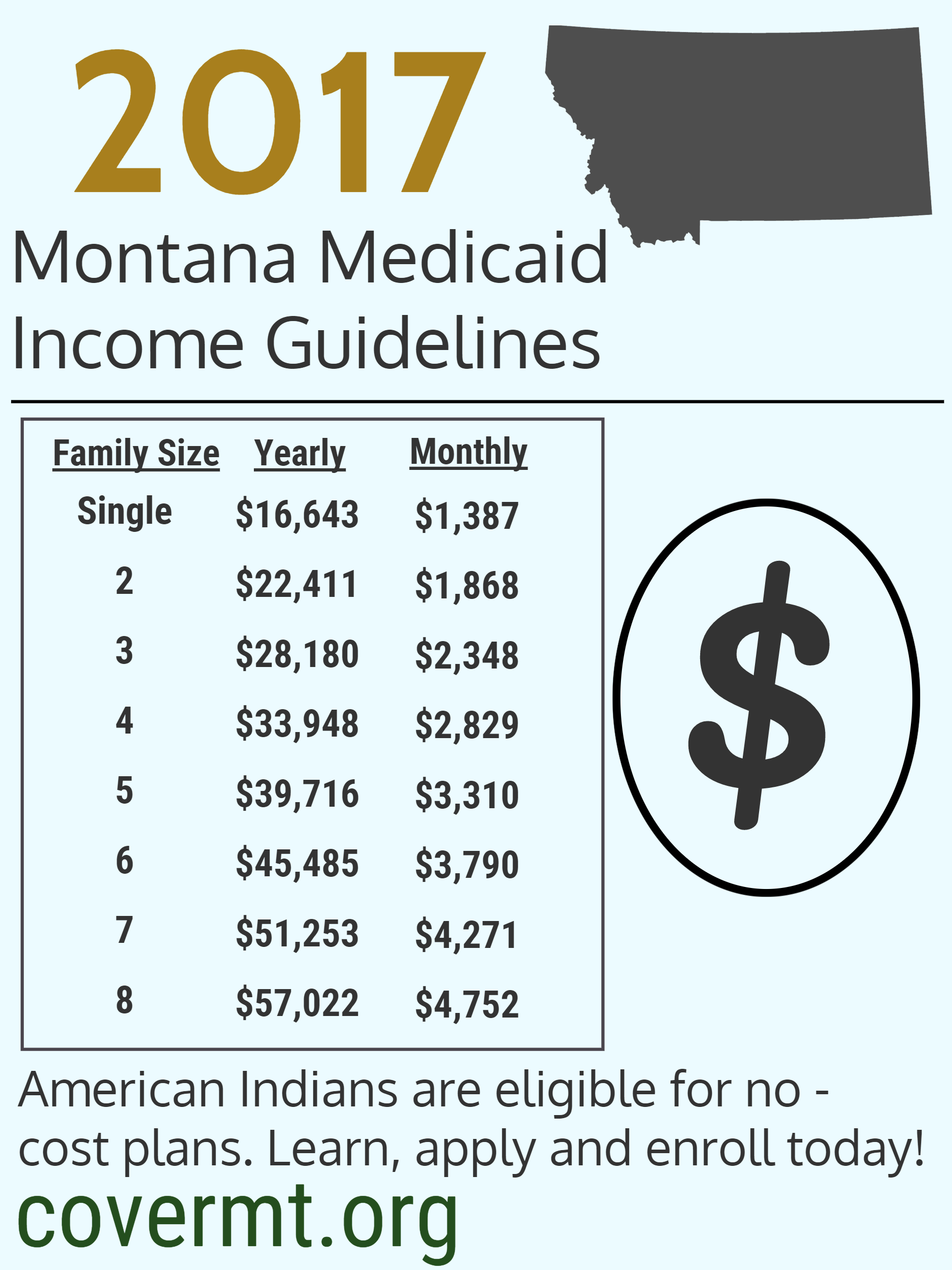

- No matter your state, you may qualify for Medicaid based on your income, household size, disability, family status, and other factors. But if your state has expanded Medicaid coverage, you can qualify based on your income alone.
- Enter your household size and state. We’ll tell you who is eligible for Medicaid, if your state expanded and if you qualify for Medicaid based only on your income.
- If you think you have Medicaid eligibility, you can create an account and fill out a Marketplace application. If it looks like anyone in your household qualifies for Medicaid or CHIP, we’ll send your information to your state agency. They’ll contact you about enrollment. You can apply any time of year.
- If you don’t qualify for Medicaid, we’ll tell you if you qualify for financial help to buy a Marketplace health plan instead.
Don’t Miss: What Is The Website To Apply For Medicaid
Medicaid Eligibility And Costs
The federal and state partnership results in different Medicaid programs for each state. Through the Affordable Care Act , signed into law in 2010, President Barack Obama attempted to expand healthcare coverage to more Americans. As a result, all legal residents and citizens of the United States with incomes 138% below the poverty line qualify for coverage in Medicaid participating states.
While the ACA has worked to expand both federal funding and eligibility for Medicaid, the U.S. Supreme Court ruled that states are not required to participate in the expansion to continue receiving already established levels of Medicaid funding. As a result, many states have chosen not to expand funding levels and eligibility requirements.
Those covered by Medicaid pay nothing for covered services. Unlike Medicare, which is available to nearly every American of 65 years and over, Medicaid has strict eligibility requirements that vary by state.
However, because the program is designed to help the poor, many states have stringent requirements, including income restrictions. For a state-by-state breakdown of eligibility requirements, visit Medicaid.gov and BenefitsCheckUp.org.
The Difference Between Medicare And Medicaid
Although the two programs share the same prefix and offer health coverage, theyre different. Nearly every American will one day qualify for Medicare, but Medicaid is only for those with a low income.
With Medicare, think care for those 65+ or those with disabilities. Then, Medicaid is aid to those with a low income. Medicaid is free. Medicare is not free. Those with Medicaid wont be subject to the Part B premium or Part B late enrollment penalties. But, those with only Medicare will be responsible for applicable costs.
Just because Medicaid is free doesnt mean its for everyone. Approval time for Medicaid can take up to 60 days. Benefits are for US citizens but, children of illegal immigrants can qualify.
If you get Social Security supplemental benefits, youll qualify for Medicaid. Also, Medicaid has benefits Medicare doesnt this includes vision, dental, and long-term custodial care.
Recommended Reading: Is Nebraska Total Care Medicaid
Aged & Disabled Federal Poverty Level Program
If you are aged or disabled and are not eligible for the SSI program, you may be able to get Medi-Cal through the Aged & Disabled Federal Poverty Level program. To qualify, you must:
This Medi-Cal program uses SSI countable income rules as well as a few extra rules you should know. For more information, visit the Medi-Cal section of the Disability Benefits 101 website.
