Q: How Long Does It Take For Applications To Be Processed
HHSC FPP contracted providers must screen all family planning applicants for eligibility in the following programs that provide family planning services, in this order:
- Healthy Texas Women
Once a client is deemed ineligible for Medicaid and HTW, the clinic will determine whether a client is eligible for FPP.
It can take up to 45 days for Medicaid/HTW applications to be processed. If questions arise, clients should contact 866-993-9972 to discuss the status of their application.
An individual is eligible for services beginning the date the contractor determines the individual eligible for the program and signs the completed application. Services delivered while a client’s application was pending may be billed to FPP for up to 95 days prior to determining eligibility.
Medicaid Family Planning Services And Supplies
Guidance for : The purpose of this letter is to clarify previous guidance on the delivery of family planning services and supplies to all Medicaid beneficiaries, as well as to highlight approaches states may take to ensure timely access to this benefit. Specifically, this letter provides guidance on family planning services provided under both fee-for-service and managed care delivery systems clarifies the purpose of the family planning visit offers strategies to reduce barriers to receiving family planning services and supplies and suggests ways to increase access to contraceptive methods.
Issued by: Centers for Medicare & Medicaid Services
Issue Date: June 14, 2016
HHS is committed to making its websites and documents accessible to the widest possible audience, including individuals with disabilities. We are in the process of retroactively making some documents accessible. If you need assistance accessing an accessible version of this document, please reach out to the .
DISCLAIMER: The contents of this database lack the force and effect of law, except as authorized by law or as specifically incorporated into a contract. The Department may not cite, use, or rely on any guidance that is not posted on the guidance repository, except to establish historical facts.
Topic
Q: How Do I Make Referrals To Other Providers And Programs
If a client covered by FPP does not want to pay out-of-pocket for services not covered by the program, providers must refer them to another physician or clinic. Providers should make referrals when health issues are identified, and necessary services related to those health issues are not covered under the program.
Individuals in need of treatment for postpartum depression must be referred to a provider of behavioral health services. Providers must have arrangements in place for appropriate referral of individuals to behavioral health providers in their area.
The Texas Health and Human Services Commission prefers referrals to local indigent care services, but 2-1-1 Texas can assist with locating other primary care providers, if needed.
The HHSC Breast and Cervical Cancer Services program offers free breast and cervical cancer screening and diagnostic services throughout Texas to eligible women. Additionally, the program provides Medicaid coverage to eligible women diagnosed with breast or cervical cancer and cervical dysplasia management and treatment for BCCS-enrolled women.
Read Also: Does Medicaid Cover Glasses In Texas
Who Is Eligible For Family Planning
Beneficiaries must meet the following eligibility criteria:
- Family income no more than 194 percent of the federal poverty level conversion)
- Must be capable of reproducing ages 13-44 years of age.
- Must not have had a procedure that prevents them from reproducing.
- Must not have Medicare, CHIP, or any other health insurance or third party medical coverage.
Q: Who Is Eligible For Fpp
- Females and males aged 64 years and younger
- Have a countable household income at or below 250% of the federal poverty level
- Ineligible for Medicaid and Healthy Texas Women
Note: Services may be provided to individuals with third-party insurance if the confidentiality of the person is a concern or if the person’s insurance deductible is 5% or more of their monthly income.
You May Like: Where To Get Braces With Medicaid
Health Education Cancer Screenings Sti Testing And Treatment Pregnancy And Preconception Screening
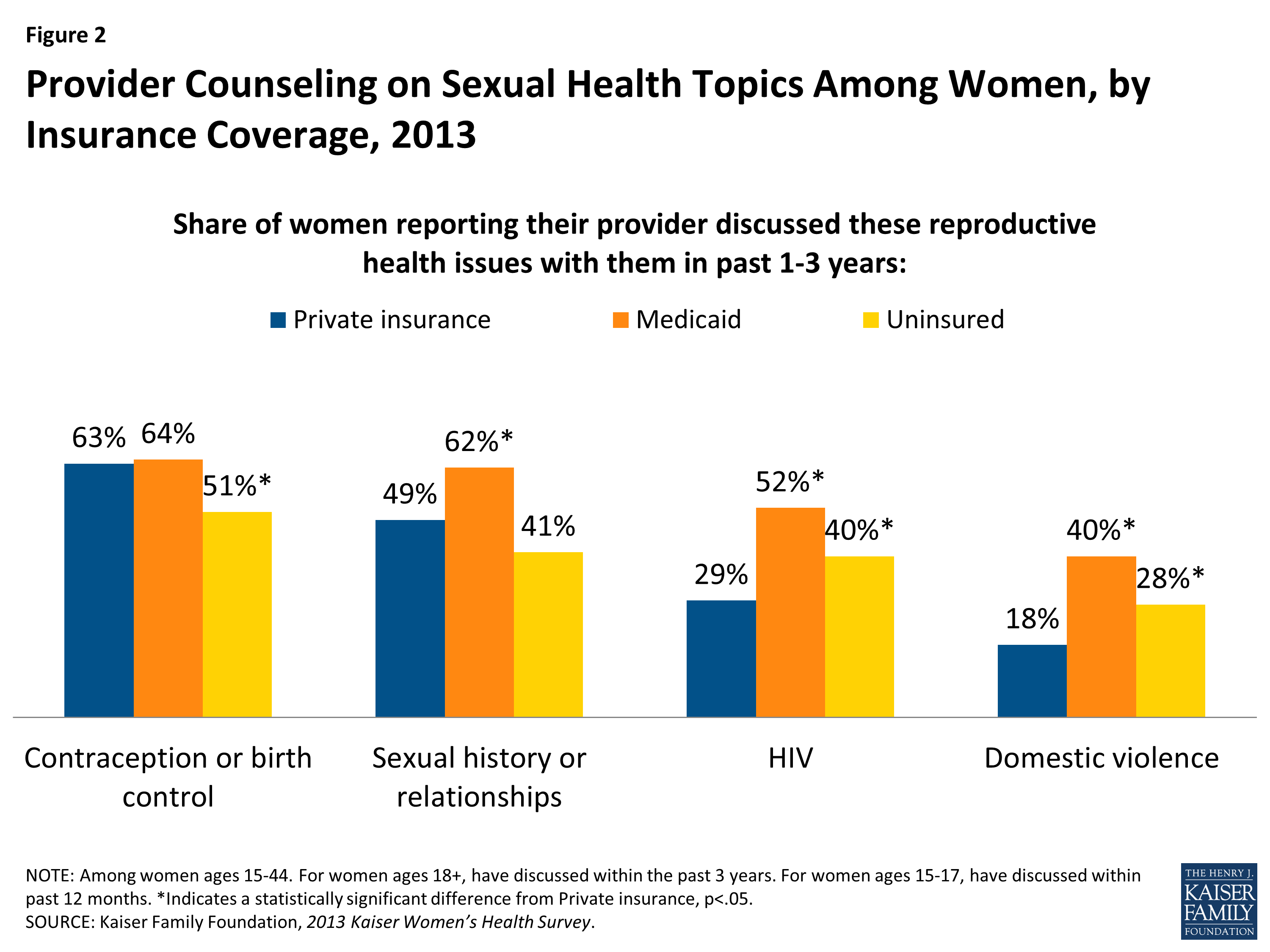
Oftentimes, states also include sexual and reproductive health education programs and testing and treatment for sexually transmitted infections in their family planning coverage, too. In addition to contraception to prevent pregnancy and space out births, many family planning programs include pregnancy testing and counseling, basic infertility services, STI and HIV services, and preconception services such as screening for obesity, smoking, and mental health. Screening for intimate partner violence is also often covered by Medicaid family planning benefits. However, there is no requirement that all states must provide all these benefits in their own Medicaid programs for family planning care.
Breast cancer and cervical cancer screenings are also typically covered by state Medicaid programs. The HPV vaccine for young adults is also covered in all but one state Medicaid program. This vaccine is the only vaccine proven to prevent cancer, in this case cervical cancer.
Recommended Reading: Blue Choice Healthy Connections Medicaid
Medicaid Family Planning Services
- all types of birth control: pills, condoms, diaphragms, IUDs, Depo Provera, Norplant, and contraceptive foams
- emergency contraception
- testing and treatment for sexually transmitted diseases including colposcopy, cryotherapy and LEEP *
- HIV testing and pre test and post test counseling *
- Pap smears testing for cervical cancer, pelvic problems, breast disease, anemia, and high blood pressure *
*As part of a family planning visit
Read Also: Eye Doctors That Accept Medicaid In Farmington Nm
Billing For Codes And Services
SoonerPlan will pay for the following services:
- Birth control information and supplies
- Office visits and physical exams related to family planning
- Laboratory tests related to family planning services, including pregnancy tests, Pap smears and screening for some sexually transmitted infections
- Tubal ligations for women age 21 and older
- Vasectomies for men age 21 and older
- Gardasil 9 for males and females through age 45.
Tubal ligations and vasectomies are paid in accordance with current SoonerCare policy and require the Sterilization Consent form.
Medically necessary office visits related to family planning are unlimited for SoonerPlan members younger than 21.
For SoonerPlan members 21 and older, medically necessary office visits and physical exams related to family planning are limited to four per month except for the initial visit code. For 99202, the limit is two per month.
Copayments do not apply for any family planning service, device, prescription or over-the-counter product.
Q: Do All Applicants Have To Prove Income Eligibility
No. If an applicant or family member receives the following services, they are considered adjunctively eligible for the HHSC Family Planning Program at an initial or renewal eligibility screening:
Proof of participation is required.
However, if an applicant does not participate in the above services, they will be asked to prove income eligibility.
Note: If the methods used for income verification jeopardize the individual’s right to confidentiality or impose a barrier to receipt of services, the contractor must waive this requirement and approve full eligibility. Reasons for waiving verification of income must be noted in the individual’s record.
Read Also: Medicaid Blue Cross Blue Shield Nevada
Potential Federal Actions To Restore Medicaid Enrollees Access To Family Planning Services
The Biden administration has tools at its disposal to address these constraints on access, such as disapproving pending Section 1115 waiver requests, revoking the approved Texas waiver, reissuing guidance outlining federal free-choice requirements, and initiating compliance actions in states that restrict access to family planning providers in ways not permitted by federal law.
The recently proposed rescission of the Title X gag rule represents a substantial step to undo family planning restrictions imposed by the prior administration. Advocates for sexual and reproductive health care are closely watching for signs of how the Biden administration will restore womens rights and strengthen their access to health care.
NOTES
1 Section 1902 of the Social Security Act generally allows Medicaid enrollees to obtain medical services from any provider that is qualified to perform the service or services required and that undertakes to provide such services. States that opt for a managed care delivery system are permitted to restrict enrollees to providers that participate in the managed care plans network. But even then, federal law preserves enrollees right to free choice of family planning providers, including those that do not participate in the plans network.
Publication Details
You May Like: Vein Clinics That Take Medicaid
What Are The Negatives Of Medicaid
Disadvantages of Medicaid Lower reimbursements and reduced revenue. Every medical practice needs to make a profit to stay in business, but medical practices that have a large Medicaid patient base tend to be less profitable. Administrative overhead. Extensive patient base. Medicaid can help get new practices established.
Also Check: Mental Health Places That Accept Medicaid
Family Planning Waiver Resources
MedicationsEffective January 1, 2015, beneficiaries enrolled in the Family Planning waiver demonstration program may have a prescription for contraceptives and/or medications to treat a sexually transmitted infection /sexually transmitted disease written by any Medicaid participating provider filled at their local Medicaid participating pharmacy.
Read Also: Can I Change Medicaid Plan
Preconception Health Care And Counseling
A Family Planning Program priority is to emphasize the importance of counseling family planning clients on establishing a reproductive life plan, and providing preconception counseling, as appropriate.
Preconception health is defined as the state of a woman’s health before she becomes pregnant it focuses on conditions and risk factors that could affect a woman and/or her unborn baby. Preconception health care seeks to identify clients with risk factors that must be acted on before conception to prevent fertility problems and reduce health problems of the mother and baby. By acting on health issues and risks before pregnancy, a woman can prevent problems that might affect her or her baby.
Preconception health care is a critical component of health care for women of reproductive age. The main goal of preconception health care is to provide health promotion, counseling, screening and interventions for women of reproductive age to reduce risk factors that might affect future pregnancies.
Recommended Reading: Is Hypnotherapy Covered By Medicaid
Understanding Types Of Medicaid Insurance In New Mexico
There are various types of NM Medicaid insurance, and enrollees can review their options when completing the Medicaid application process. The medical insurance plans are offered by four managed care plans that have been contracted by the state of New Mexico to provide Medicaid services. The Medicaid coverage plans are through: Blue Cross Blue Shield, Molina Health Care, Presbyterian Health Plan and UnitedHealthcare Community Plan.
The types of Medicaid insurance in New Mexico in which members enroll determine the amount of coverage for which they qualify. The health plans offer the full array of Medicaid services, including community-based long-term services, institutional behavioral health, acute services and support services.
After signing up for NM Medicaid coverage, you will have to choose a health plan. If you do not, one will be automatically assigned to you. The Medicaid health policy you choose will determine the network of providers from which you can obtain services. NM Medicaid services are only covered if they are provided by health centers, facilities, clinics, providers or doctors that are in a plans network.
What Is Family Planning Medical Assistance
The purpose of the Family Planning Services Program is to assist in the. establishment and operation of voluntary family planning projects which consist of. the educational, comprehensive medical, and social services necessary to aid. individuals to determine freely the number and spacing of their children.
What does family planning include?
Family Planning Services include: Most FDA approved birth control methods, devices, and supplies Preconception counseling and preventive screening and family planning options before pregnancy. Transportation to family planning visits.
What is the purpose of family planning?
Family planning helps protect women from any health risks that may occur before, during or after childbirth. These include high blood pressure, gestational diabetes, infections, miscarriage and stillbirth.
Don’t Miss: What Is Family Planning Medicaid Nc
Who Is Eligible For The Fpp
- Men and women, ages 12 through 54, who are:
- Iowa residents or
- U.S. citizens or qualified immigrants
- Who meet income limits
Women whose pregnancies and deliveries were covered by Medicaid will have family planning services covered for an additional 12 months without having their eligibility re-determined.
In determining FPP eligibility, the households countable monthly income shall not exceed the amounts shown in the chart below for a household of the same size.
FAMILY PLANNING PROGRAM MONTHLY INCOME LIMITS: 300% OF POVERTY |
|---|
| HH SIZE |
What Do I Need To Provide With My Application When Applying For The Fpbp
You will need to bring or send in documentation for each of the items listed below:
- Full legal name as it appears on your birth certificate
- Social Security Number
- Proof of your citizenship or immigration status. If you are a U.S.citizen and provide a valid Social Security Number , a match with Social Security Administration will verify your SSN, date of birth/age and U.S. citizenship. If SSA verifies this information, no further proof is needed. The SSA match cannot verify birth information for a naturalized citizen. You will need proof of naturalization or a U.S. passport)
- Proof of your age , like a birth certificate, or a passport
- Proof of earned income, like recent paycheck stubs , a letter from your employer or a profit and loss statement if you are selfemployed
- Proof of your unearned income, from sources like Social Security Benefits, NYS Disability Benefits, or Unemployment Benefits
- Proof of where you live, like a rent receipt, letter from your landlord, mortgage statement, or postmarked nonwindow envelope from mail you received recently
- Health Insurance benefit card or policy statements
- You do not need to bring or send in proof of your resources, such as bank statements, vehicles you own or insurance policies. Resources are not counted in determining eligibility for the FPBP.
Don’t Miss: What States Does Medicaid Cover Abortions
Waiver Authority For The Program
On May 9, 2018 the Health Care Authority received approval for renewal of the Section 1115 Family Planning Only Demonstration Waiver for five years . The approval letter, Special Terms and Conditions, and Expenditure Authority can be found on CMSs website under Washington Family Planning Only Program and then clicking on Demonstration Approval.
The Health Care Authority intends to submit an application to extend the Section 1115 Family Planning Only Demonstration Waiver for five years . The current waiver expires on June 30, 2023, and covers limited family planning and family planning-related services for people who are in need of contraceptive care and are enrolled in the Family Planning Only programs. The purpose, client eligibility requirements, and benefit package will remain the same. The only potential change is the elimination of the Family Planning pregnancy-related program, due to the implementation of the After-Pregnancy Coverage program. This change will take effect when the end of the federal Public Health Emergency is declared. There is currently no established end date for the PHE.
-
Family Planning Program 1115 waiver renewal public hearing #2 | Presentation
- Family Planning Program 1115 waiver renewal public hearing #1 | Presentation
Public Notice Of Annual Public Forum For 1115 Family Planning Waiver
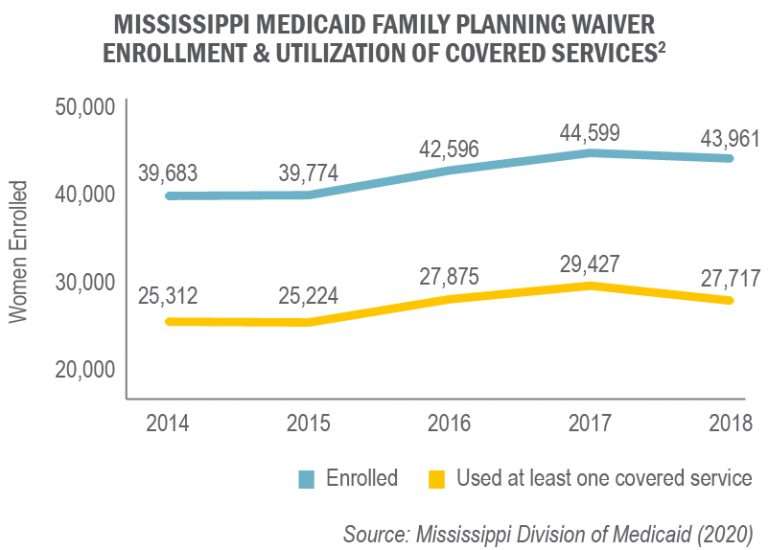
Pursuant to 42 C.F.R. Section 431.420, a Public Forum is required annually after the implementation of the Division of Medicaids Family Planning Waiver. This Public Forum provides stakeholders the opportunity to provide meaningful comments on the progress of the Family Planning Waiver. The Family Planning Waiver operates under the authority of an 1115 waiver approved by the Centers for Medicare and Medicaid Services effective January 1, 2018 through December 31, 2027. This Public Forum will be held at 10 a.m. on Wednesday, September 30, 2020. Due to the public health emergency, the Public Forum will be held via teleconference at 888-822-7517, access code: 4282244. There will be an opportunity for public comment during the forum.
Read Also: Doctors In San Antonio That Accept Medicaid
Don’t Miss: What Is Traditional Medicaid For Adults
Family Planning Medicaid Or Be Smart Medicaid
The NC Medicaid Family Planning Program or Be Smart program is designed to reduce unintended pregnancies and improve the well-being of children and families in North Carolina. Family planning, reproductive health and contraceptive services are provided to eligible men and women, whose income is at or below 195% of the federal poverty level, with no age restrictions.
What Is The Family Planning Program

This program allows men and women to get family planning services only. This program is a form of limited insurance coverage. If you are able to enroll in the FPP, most of your basic family planning services will be paid for. However, it does not meet the Affordable Care Act requirements for a minimum essential benefits plan.
Don’t Miss: Medicaid Change Plan Phone Number
