What Is A Medical Assistance Program
State and federal programs that provide assistance to individuals who need help with health care coverage are commonly referred to as medical assistance programs. Millions of people rely on these programs each and every day to cover costly medical expenses. The two most common medical assistance programs are Medicaid and Medicare.
Implications Of Involvement In Clinical Medicine
We have outlined selected examples of how Medicare and Medicaid have influenced clinical medicine. Medicare and Medicaid emerged from a fierce political process in 1965 with the charge to stay away from clinical medicine. Early on, however, Federal administrators recognized that Medicare and Medicaid could not control costs or ensure quality without regulation. As regulation developed, it took several years for the Federal Government to adopt the strategy of prospective quality improvement through partnership with the medical community. This strategy has much promise for improving medical care.
Donât Miss: What To Do Before You Turn 65 Medicare
Medicare Vs Medicaid: Eligibility
Medicare: Youre eligible once you turn 65, as long as youre a U.S. citizen or legal permanent resident. Medicare also covers younger people with disabilities and certain diseases, including end stage renal disease and Lou Gehrigs disease or amyotrophic lateral sclerosis . People with higher incomes pay larger premiums for certain parts of Medicare, but eligibility isnt limited by income.
Medicaid: Medicaid coverage is based on income. Medicaid is available in every state to those with incomes below the poverty line. Under the Affordable Care Act, most states have expanded Medicare eligibility to people with incomes up to 133% of the federal poverty line.
Also Check: What Is The Number To Apply For Medicaid
What Is The Medicaid Waiver Program
Federal guidelines have provided an avenue for states to develop community-based services waivers to better meet the long-term care goals of individuals who prefer to seek care in their own community or home as opposed to a hospital or institutional setting. The waivers must target a specific group and states are able to operate as many waivers as they wish.
The Medicaid website outlines the four criteria for the waivers under federal guidelines. The waiver programs must:
- Demonstrate that providing waiver services wont cost more than providing these services in an institution.
- Ensure the protection of peoples health and welfare
- Provide adequate and reasonable provider standards to meet the needs of the target population
- Ensure that services follow an individualized and person-centered plan of care
Some of the services of care that are often covered under these waivers include case management, home health aides, adult day health services, personal care, and respite care. While these are the most common, states are able to propose other types of care that they believe will help individuals which is a unique feature of the waiver program. Essentially, these HCBS programs give states the ability to tailor resources to more specialized groups.
Can One Have Dual Eligibility For Both Medicare And Medicaid
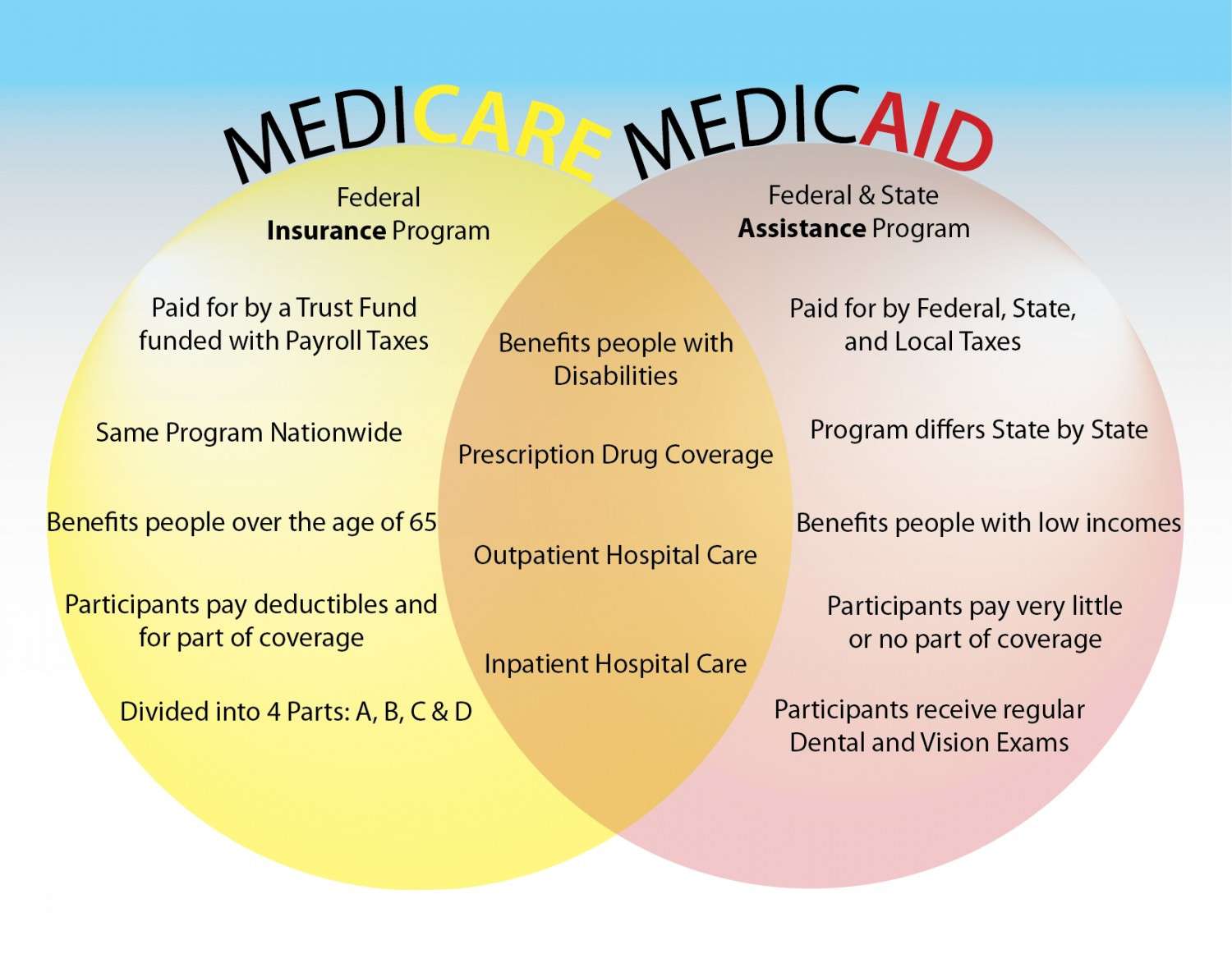
Yes, Medicare and Medicaid are not mutually exclusive programs. Persons who are eligible for both are referred to as having Dual Eligibility, Dual Eligibles, or often simply Duals. Medicare is the first payer of covered benefits, while Medicaid is the secondary payer.
Typically, Medicaid will pay for Medicare premiums and co-payments for dual eligibles. In fact, many states have special programs intended to make it easier for seniors to manage their dual eligibility status, as it can be confusing to know where to turn for what services. This is generally in the form of managed care.
There are also programs called Medicare Saving Programs for low-income seniors that dont quite qualify for Medicaid.
Also Check: What Is Family Planning Services Medicaid
Can You Have Both
People who qualify for both Medicare and Medicaid are considered dual eligible. In this case, you may have original Medicare or a Medicare Advantage plan , and Medicare will cover your prescription drugs under Part D.
Medicaid may also cover other care and drugs that Medicare doesnt, so having both will probably cover most of your healthcare costs.
Medicare Gives Many Options
Medicare offers a wealth of choices. Once you decide whether you want a Medicare Advantage or Original Medicare plus Part D, youre able to narrow your focus and select the best Medicare plan for you.
Premiums, deductibles and out-of-pocket costs can vary greatly, so make sure you compare each cost.
Medicaid, on the other hand, will likely give you one or very few choices. That plan could be through the state, or it could be a managed care plan offered by a private insurer.
Differences arent just between Medicare and Medicaid. The different types of Medicare plans also vary. Heres how Medicare and Medicaid plans compare:
Also Check: How Do I Choose Medicare Part D Plan
You May Like: Knee Braces Covered By Medicaid
Who Qualifies For Medicaid
Medicaid provides health care coverage for roughly one in every five Americans 63.9 million people, according to the U.S. Centers for Medicare & Medicaid Services. Two-thirds of all Medicaid spending is directed for the care of the elderly and disabled.
Because Medicaid is jointly funded by the federal government and the various states, eligibility requirements vary from state to state.
Some states may also allow out-of-pocket fees for such things as copayments if you are on Medicaid. But children and people living in nursing homes or other institutions are usually exempt from these costs.
Examples of Who May Qualify for Medicaid
- 65 or Older, Blind or Have a Disability
- People in these groups are eligible for Medicare. They may apply for both if they have low incomes or opt for Medicaid only if they cant afford Medicares additional costs.
- Low Income
- Varies from state to state, but you qualify in most states if you make 100 to 200 percent of the federal poverty level and meet other criteria elderly, disabled or have a minor child.
- Assets
- In most states, youre limited to $2,000 in countable assets or $3,000 for a married couple. These include stocks, bonds, checking and saving accounts and additional vehicles.
Applying for Medicaid varies from state to state. It can take weeks or months after you apply before you find out if you qualify for benefits. States may also require you to take a medical exam or provide documentation of your past and current financial status.
Can You Own A Home And Be On Medicaid
It is possible to qualify for Medicaid if you own a home, but a lien can be placed on the home if it is in your direct personal possession at the time of your passing. To prevent this, you could give the home to loved ones, but you have to act well in advance so you don’t violate the five-year look back rule.
You May Like: How To Get Copy Of Medicaid Card Online
What Are The Disadvantages Of Medicaid
Disadvantages of Medicaid
- Lower reimbursements and lower income. Every doctors office must make a profit to stay in business, but doctors offices that have a large Medicaid patient base tend to be less profitable.
- Administrative overhead.
What Must Be Covered Under Medicaid
Federal government mandates that all states must provide Medicaid plans that cover the following:
- Inpatient hospital services
- Early and Periodic Screening, Diagnosis, and Treatment
- Federally Qualified Health Centers services
- Family planning services
- Emergency and non-emergency medical transportation
- Pregnancy-related services
Read Also: Medicaid Indiana Provider Phone Number
Is The Medicare Program Run By The Government
Medicare is a federal program. Its basically the same across the United States and is run by the Centers for Medicare & Medicaid Services, an agency of the federal government.
Can you get both Medicare and Medicaid?
It is possible for people to qualify and enroll in both Medicare and Medicaid. When a person qualifies for both programs, they become dually eligible and receive their care through certain Medicare savings programs.
Medicare And Medicaid For Ssi And Ssdi Recipients
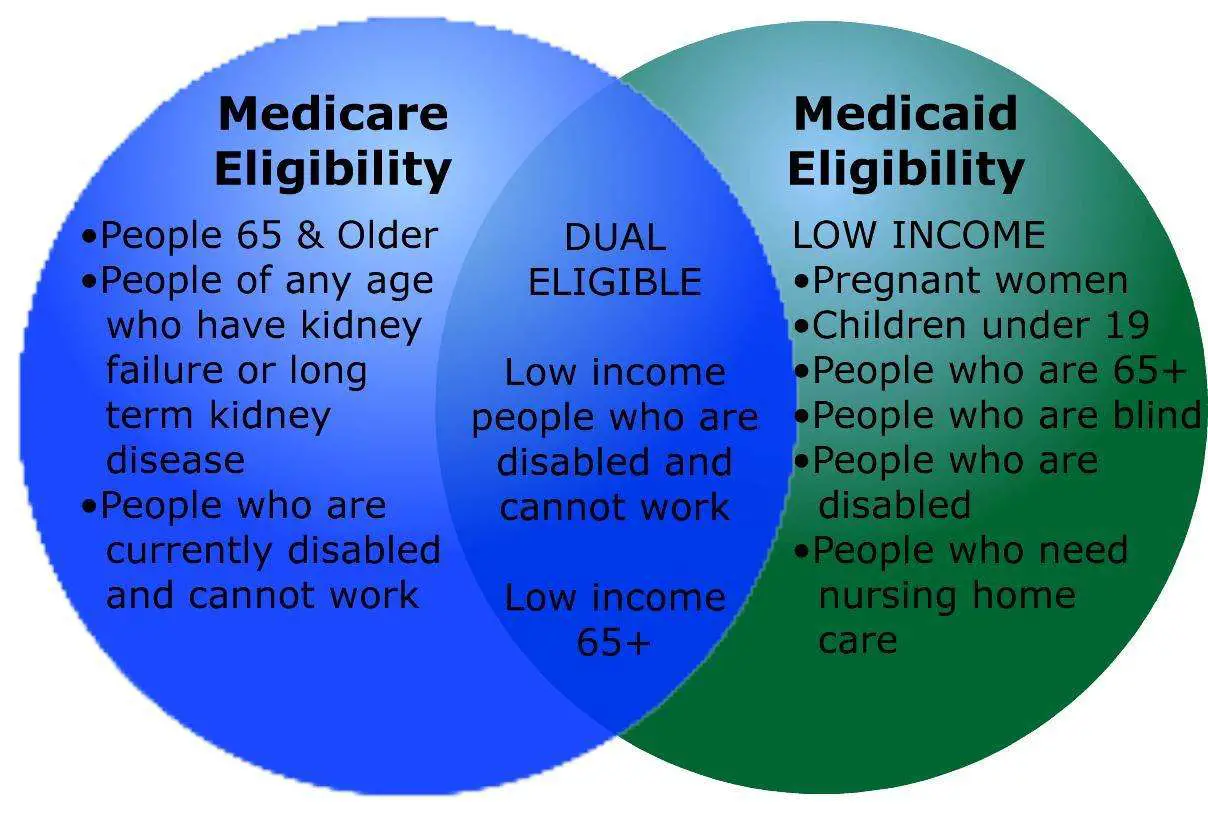
If you receive Social Security Disability Insurance benefits, you will automatically qualify for Medicare. If you receive Supplemental Security Income benefits, you will also receive Medicaid.
SSDI beneficiaries have to wait two years after they start receiving SSDI payments to receive Medicare benefits. They may also qualify for dual eligibility while on SSDI and may also be eligible for Medicaid coverage. In this case, they will typically receive Medicaid payments for the first two years and will have Medicare premiums paid through Medicare Savings Programs when those payments start.
SSI beneficiaries cant receive Medicare benefits only Medicaid coverage until they turn 65 or have end-stage renal disease. They will have to file an Uninsured Medicare Claim to start receiving Medicare when they qualify. They may also have to sign up for Medicaid separately if they receive SSI benefits. This varies by state.
You May Like: What Age Do You Get Medicaid
Medicare Vs Medicaid: How They Differ
Updated on Friday, September 13 2019 | 0 min. read| by Bryan Ochalla
What is the difference between Medicare and Medicaid? Heres what they cover, who can get them, how much they cost and more.
Medicare and Medicaid are very different programs the U.S. government created to cover the medical bills of two distinct groups of Americans.
Medicare is a health insurance program that mostly serves people over the age of 65. Medicaid is an assistance program that mostly serves low-income people of any age.
To qualify for Medicaid, you usually need to be below a certain income level. Your income level usually doesnt impact whether or not you qualify for Medicare.
The federal government runs Medicare. State and local governments run Medicaid within federal guidelines.
These are just the most basic differences between the Medicare and Medicaid programs. Keep reading to learn more about:
Signing Up For Medicare And Medicaid
You can sign up by going to Medicare.gov.
One option is to just get Part A, which covers hospitalizations and is free to nearly all Americans 65 and over. The only people who pay premiums for Part A are those who didnt pay 10 years worth of Medicare taxes.
So, if you decide to get Original Medicare or have other coverage and want to delay paying for Medicare, you could sign up for only Medicare Part A initially.
If youre still working or on your spouses insurance, you may decide to stay on that plan for physician services and wait to sign up for Part B until later. You can do that, but beware that you may pay higher premiums once you sign up for Part B. CMS will charge you a 10% premium penalty for every 12 months that you dont enroll in Part B. That penalty will get added to your premiums once you get Part B.
Heres another reason to sign up for Medicare when you turn 65. You may have to wait until the open enrollment period if you dont sign up when you become eligible.
Meanwhile, if you need to sign up for Medicaid, you can check out our Medicaid page. Just choose your state on the tool on that page and well tell you the name of Medicaid in your state, where you can sign up and whether youre eligible for Medicaid in your state.
Recommended Reading: Blue Cross Blue Shield Nevada Medicaid
Medicare Vs Medicaid: The Simularities
- Theyre both health insurance programs that are designed to help specific people receive affordable health insurance coverage.
- Theyre both government-sponsored programs. The government collects taxes and fees where necessary and is responsible for the way the programs run.
- Theyre both run by the Centers for Medicare and Medicaid Services .
Medicare and Medicaid also sound similar, but theyre actually very different. Lets review the basics of both programs and explain how it works when you qualify for both Medicare and Medicaid.
Who Does Medicare Cover
Medicare is a federal government-sponsored healthcare program for those 65 and over, and for younger people who are disabled . Most people with Medicare paid FICA taxes during their working years, and realize the benefits of that tax through Medicare coverage. The federal government establishes the eligibility criteria for Medicare.
Recommended Reading: How To Fight Medicaid Denial
Can You Get Medicaid If You Have Medicare
Some low-income, elderly Americans are dual-eligible for Medicare and Medicaid. These individuals are enrolled in Original Medicare, but receive Medicaid benefits through a Medicare Savings Program. These programs include:
-
Qualified Medicare Beneficiary Program, which helps cover Original Medicare premiums, deductibles and coinsurance/copayments
-
Specified Low-Income Medicare Beneficiary Program or Qualifying Individual Program, which both helps cover Medicare Part B premiums
-
Qualified Disabled Working Individual Program, which pays Medicare Part A premiums for certain disabled Americans who still are working
Learn more about Medicare Savings Programs.
CMS releases the criteria for each dual-eligibility each year. Given these programs tap Medicaid resources, they are income-driven. You can find 2020 requirements here.
If you have both Medicare and Medicaid, Medicare serves as your primary form of coverage. Medicaid only pays for health care services or supplies after Medicare, employer group health plans, and/or Medicare Supplement Insurance have been exhausted.
Former Head of Content at Policygenius
Jeanine Skowronski is the former head of content at Policygenius in New York City. Her work has been featured in The Wall Street Journal, American Banker Magazine, Newsweek, Business Insider, Yahoo Finance, MSN, CNBC and more.
Questions about this page? Email us at .
32 Old Slip, 30th Fl New York, NY 10005
Medicare Vs Medicaid: The Important Differences To Know
In the United States, there are currently two government-provided health insurance policies that citizens can enroll in: Medicare and Medicaid.
While they both provide general health insurance benefits, there are differences in eligibility and coverage that are crucial to identify and be aware of the largest being that Medicare is available to adults who are over 65 years old whereas Medicaid is only available to low-income families.
Medicaid is usually cheaper than Medicare, providing those who are near or below the poverty line with free or low-cost coverage. In contrast, Medicare is open to all income levels and usually costs a few hundred dollars per month.
Find Cheap Medicare Plans in Your Area
Don’t Miss: Affordable Braces For Adults With Medicaid
What Is The Difference Between Medicaid And Medicare
Insurance Coverage, Older Adults /Sanitas Medical Center
The United States has been referenced as one the most important countries in the world. It has guided other countries towards global inclusion in terms of progress, human rights and justice.
To aid American people, the government created two separate social security programs to help vulnerable American citizens with their healthcare needs. You might be familiar with one of their names, if not both: Medicaid and Medicare. Today we will briefly talk about what they mean and point out some of the differences between them.
Lets start with the basics.
These two programs were created by the federal government to assist people with the cost of healthcare. Both are funded by taxes and work all along American grounds. Both are designed primarily for citizens of the United States or very long term residents who have contributed to the countrys growth. However, although their names are very similar, they have two completely different purposes.
What is Medicaid and how can I get enrolled in it?
Medicaid is an assistance program designed to help people with low incomes. It does not have an age restriction and its copays or deductibles, if they exist, are usually very low. Eligibility for Medicaid varies from state to state, and depends on specific requirements.
So, if I am not eligible for Medicaid, can I get Medicare healthcare?
If you wish to know if you are eligible for Medicare, visit the Medicare eligibility tool.
How Much Does Medicaid Cost
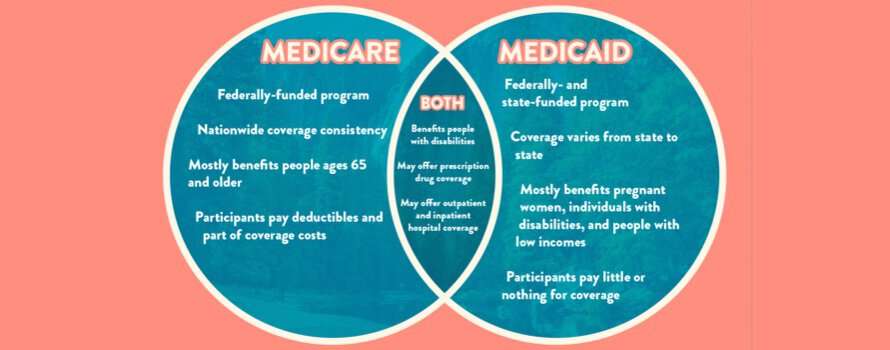
States can require Medicaid beneficiaries to pay nominal premiums, deductibles and copays/coinsurance for services and prescription drugs. These out-of-pocket costs are capped, but those caps are based on how much the states pay for services, so theyll vary by where you live, what your income is and what care youve received.
Certain Medicaid beneficiaries are exempt from most or all out-of-pocket costs. These beneficiaries typically include pregnant women, children, terminally ill individuals and patients living in a health care institutions.
Also Check: Dentist In Amarillo Tx That Accept Medicaid
Which Of The Following Is An Example Of A Means
Means-tested eligibility programs fall into two broad categories: health programs and income security programs . earned income tax credit and child tax
Is the Medicaid program the same as Medicare?
Its basically the same across the United States and is run by the Centers for Medicare & Medicaid Services, an agency of the federal government. For more information about Medicare and its components, go to http://www.medicare.gov. Medicaid is an assistance program. It serves low-income people of all ages.
Medicaid Eligibility And Costs
The federal and state partnership results in different Medicaid programs for each state. Through the Affordable Care Act , signed into law in 2010, President Barack Obama attempted to expand healthcare coverage to more Americans. As a result, all legal residents and citizens of the United States with incomes 138% below the poverty line qualify for coverage in Medicaid participating states.
While the ACA has worked to expand both federal funding and eligibility for Medicaid, the U.S. Supreme Court ruled that states are not required to participate in the expansion to continue receiving already established levels of Medicaid funding. As a result, many states have chosen not to expand funding levels and eligibility requirements.
Those covered by Medicaid pay nothing for covered services. Unlike Medicare, which is available to nearly every American of 65 years and over, Medicaid has strict eligibility requirements that vary by state.
However, because the program is designed to help the poor, many states have stringent requirements, including income restrictions. For a state-by-state breakdown of eligibility requirements, visit Medicaid.gov.
When Medicaid recipients reach age 65, they remain eligible for Medicaid and also become eligible for Medicare. At that time, Medicaid coverage may change based on the recipient’s income. Higher-income individuals may find that Medicaid pays their Medicare Part B premiums. Lower-income individuals may continue to receive full benefits.
You May Like: Mental Health Places That Accept Medicaid
