New Chip Contracts Take Effect Nov 1 2019
CHIP is currently administered by two coordinated care organizations . New CHIP contracts with Molina Healthcare and UnitedHealthcare Community Plan will take effect Nov. 1, 2019. CHIP beneficiaries currently enrolled with the outgoing CHIP CCO, Magnolia Health Plan, will receive a letter giving them the opportunity to choose between Molina Healthcare and UnitedHealthcare Community Plan. If a CHIP beneficiary does not respond, they will be assigned to Molina Healthcare.
All CHIP beneficiaries can select which plan they want during annual open enrollment which will be held in October through December.
As always, DOM encourages providers to enroll in all Mississippi Medicaid programs and wants providers to be aware that Molina Healthcare will be providing CHIP services come Nov. 1, 2019.
Opting For Part A Only
Some people choose only to have Medicare Part A coverage so that they dont have to pay the monthly premiums for Medicare Parts B and D. If you still have insurance through a current employer , you can add the other parts later with no penalty.
However, if you decline Parts B and D and don’t have another insurance plan in place, you’ll face a late enrollment penalty when you add the other parts later.
In the past, Medicaid programs typically didn’t offer a lot of choice in terms of plan design. Today, most states utilize Medicaid managed care organizations . If there’s more than one MCO option in your area of the state, you will likely be given the option to select the one you prefer.
Medicaid Eligibility For Children
Children raised in families earning 138 percent or less of the federal poverty level per year are eligible for Medicaid. The FPL is calculated by the U.S. Department of Health and Human Services every year and is based on the number of people in a family with consideration also given to location. After all, some states are much more expensive to live in than others, like Hawaii.
Before the Affordable Care Act , i.e., Obamacare, was passed in 2010, children became eligible for Medicaid based on both their age and family income. Generally speaking, the older a child got, the less likely he was to get Medicaid coverage for the same family income. Oddly enough, this meant that only some children within the same family might be covered in any given year. The new legislation made the income eligibility standard the same for children 0 to 19 years of age.
Some states still have different eligibility requirements for different ages groups, but the standard value is now set for at least 138 percent of the FPL for all children. Before the ACA, the eligibility threshold was set at only 100 percent for children between 6 and 19 years old.
You May Like: How Does Medicaid Work In Maryland
Basic Definition Of Medicaid
Medicaid is another health coverage program that is funded by both the states and the federal government.
Unlike Medicare, which is limited to mainly the elderly population, Medicaid offers health insurance to:
- Low-income adults
- Preventative Care
- Child Dental Care
The purpose of this program is to allow those with low annual income access to quality medical care.
Do I Qualify For Medicaid
Medicaid provides free or low-cost health coverage to some low-income people, families and children, pregnant women, the elderly, and people with disabilities. Many states have expanded their Medicaid programs to cover all people below certain income levels. Medicaid qualifications depend partly on whether your state has expanded its program.
Don’t Miss: Plan First Medicaid Doctors List
Learn About The Benefits Of Chip Vs Medicaid
Together, Medicaid and CHIP Insurance provide health care benefits for millions of Americans across the country, especially children and youth with special health care needs. Similarly to most aspects of CHIP and Medicaid, states have control over the type, amount, duration and scope of covered services that will be provided to residents. However, the federal government has established a list of mandatory coverage that must be provided to beneficiaries. Some of this coverage includes:
- Inpatient and outpatient services.
Medicaid Vs Chip: An Overview
Medicaid and Childrens Health Insurance Program both play a critical role in ensuring that children in lower-income families have sufficient health care coverage. Although they are both federal programs largely implemented through the states with joint financing, the two programs differ in many respects.
Read Also: Aetna Better Health Of Ohio Mycare Ohio Medicare Medicaid Plan
D: Prescription Drug Coverage
Medicare Part D provides prescription drug coverage. The beneficiaries are required to pay the cost of Part D plans out-of-pocket and are required to pay monthly premiums, an annual deductible, and copays for specific prescriptions.
Participants enrolled in Medicare Part C may only be interested in Part D if their plan does not cover prescription drugs.
How Is Chip Funded
CHIP is funded jointly at the federal and state levels of legislature through a formula based on the Medicaid Federal Medical Assistance Percentage . As additional incentive for states to expand their coverage programs for children, Congress enhanced the federal matching rate for CHIP, which is generally about 23 percent higher than the Medicaid rate averaging 93 percent nationally.
Because CHIP is a capped program, each state is provided an annual CHIP allotment. Every fiscal year, the Centers for Medicare and Medicaid Services determines their share of program funding for that year. States must provide matching funds to get their federal funding allotment.
Also Check: Does Medicaid Cover Cord Blood Banking
Medicaid Funding May Be Cut
The Trump administration sought to repeal the Affordable Care Act and replace it with the American Health Care Act, which was then dubbed the Better Care Reconciliation Act in 2017. The legislation didnt pass, but it would end the expansion of Medicaid, and it would also change the way Medicaid is funded. According to the Congressional Budget Office, the BRCA will cut $756 billion from Medicaid over 10 years, so 15 million people on Medicaid will lose coverage.
BCRA does provide tax credits for individuals and families. In this way, it can be said that people are trying to reduce the cost of health care for Americans. Specifically, the BCRA will replace the ACA income-based tax credit with an age-adjusted flat tax credit. In some cases, BCRA subsidies will be higher than ACA, but these subsidies are capped at $14,000 per year regardless of family size. Additionally, anyone who is eligible for an employer-sponsored health plan, Medicare, Medicaid, or CHIP or TriCare is not eligible for these tax credits.
Efforts to repeal the Affordable Care Act are still ongoing. Because individual mandates were deemed unconstitutional in 2017, a federal court judge in Texas ruled in 2018 that the Affordable Care Act as a whole was unconstitutional. The ruling is on appeal and may eventually go to the Supreme Court. Until then, the Affordable Care Act is still in effect.
How To Apply For Medicaid And Chip
Determining qualification for Medicaid or CHIP is a rather straightforward process. There is an income calculator on the healthcare.gov Medicaid page to determine qualification based on income. This is a useful tool but does not automatically determine eligibility.
One way to apply for Medicaid and CHIP is through the Health Insurance Marketplace. Once you submit an application, your state agency will contact you regarding enrollment. At the time of application, you will also learn if you qualify for an individual plan as well, possibly with some savings based on income.
Parents, grandparents, guardians or other legally authorized representative can apply for benefits on behalf of a child. Teenagers living on their own may also apply for themselves, or any adult may apply for them.
The second way to apply for Medicaid and CHIP is through your state’s Medicaid agency. Following this link will allow you to select your state. Once your state is selected, you will be able to follow a provided URL that directs you to the Medicaid homepage for your state’s Medicaid agency.
Read Also: Medicaid For The Aged Blind And Disabled
Is Chip A Good Insurance
CHIP has been an effective program, providing comprehensive coverage and financial protection to millions of American children and increasing their access to and use of recommended care. It has also helped to reduce disparities in health coverage and care that affect low-income children and children of color.
C: Medicare Advantage Plans

People eligible for Part A and Part B are also qualified for Part C, also called the Medicare Advantage program. Private firms approved by Medicare provide Medicare Part C programs.
In addition to the insurance coverage through Parts B and A, Part C also provides hearing, vision, and dental coverage. It could also offer prescription insurance for drugs.
In this way, it works similar to Health maintenance groups and preferred provider organizations , through which many individuals receive medical treatment during their work-related years.
Participating in Part C could lower the cost of buying services individually. Individuals should be aware of their medical needs since Part C enrollees typically have to pay for these services.
You might also like to read: How To Win A Medicare Appeal
You May Like: Arkansas Long Term Care Medicaid Application
Information About The Requirements For Each Program
Both Medicaid and CHIP insurance offer numerous benefits to participating individuals. The coverage offered by Medicaid and CHIP provides health insurance to millions of Americans. Financial eligibility is determined using a Modified Adjusted Gross Income . In fact, MAGI has been used to calculate financial eligibility since the passing of the Affordable Care Act . Using a universal measurement has made it easier for applicants to understand the requirements to participate in government-funded health care programs.
Since these programs each have specific goals, the requirements for each differ slightly. Individual states are in charge of implementing and managing these programs for their residents. However, there are federal guidelines that must be followed in order for states to receive funding. Applicants can visit a Medicaid office to inquire about the particular MAGI limits in their area.
How The Programs Differ
Medicare is an insurance program while Medicaid is a social welfare program.
Medicare recipients get Medicare because they paid for it through payroll taxes while they were working, and through monthly premiums once theyre enrolled.
Medicaid recipients need never have paid taxes and most dont pay premiums for their Medicaid coverage .
Taxpayer funding provides Medicaid to eligible needy people in a manner similar to other social welfare programs like Temporary Assistance for Needy Families Women, Infants and Children and the Supplemental Nutrition Assistance Program.
Also Check: What Is The 1 800 Number For Medicaid
Learn About Medicaid Requirements
States have the authority to set up and administer both Medicaid and CHIP however they see fit, as long as they meet all the established federal guidelines. Since Medicaid is generally meant to cover eligible low-income families who may be having trouble purchasing their own insurance coverage, the eligibility requirements are slightly different than those of CHIP. Eligibility for Medicaid is determined using both financial and non-financial requirements. The passing of the Affordable Care Act has recently expanded Medicaid coverage to even more Americans than ever before.
Financially, taxable incomes and tax filing relationships are used to determine eligibility for Medicaid. The finances for a household are measured using the Modified Adjusted Gross Income system. Now, nearly all low-income Americans who are 65 years or younger qualify for Medicaid coverage. The eligibility limits for children has also been extended to a higher percentage of the FPL in each state . Each state was also given the option to extend the eligibility levels for adults. Medicaid has also established mandatory eligibility for certain groups of people. These mandatory eligibility groups usually consist of:
- Some low-income families.
- Qualified pregnant women and children.
- Individual receiving Supplementary Security Income .
Note: Any children engaged in an adoption assistance agreement or young adults who are former foster care recipients can be eligible for CHIP and Medicaid at any income level.
Federal Funding For Chip
Federal funding for CHIP, on the other hand, has pre-set limits. Each state is given an allotment every year as a block grant. The dollar amount is fixed regardless of the number of people covered by the program.
The 50 states and the District of Columbia have a choice to use their block grants in one of three ways:
- As a combination Medicaid-CHIP program
- As part of the state’s Medicaid expansion
- As a separate CHIP program
To encourage states to participate in CHIP, the federal government offers a higher matching rate than it does for Medicaid. This is referred to as the enhanced Federal Matching Assistance Percentages . The minimum for Medicaid matching in 2020 is 50 percent but all states are 65% or higher. Again, states with higher economic needs get reimbursed at an even higher rate.
Those states using combination programs or Medicaid expansion have the same program requirements as traditional Medicaid. States with separate CHIP programs, however, have more wiggle room. If need be, they can put children on waiting lists or establish enrollment caps to rein in CHIP costs. Many of those states will also charge premiums and copayments to their beneficiaries.
Read Also: Does Walmart Pharmacy Take Medicaid
Who Are Dc Medicaid And Dc Healthy Families Intended To Help
In order to qualify for Medicaid and CHIP, individuals must meet certain financial and non-financial requirements. Because of the impact of historic and current racism, in DC people who meet the income requirements are disproportionately Black and Latinx. According to the most recent Census estimates, the median income for DCs white households is almost four times that of Black households and over twice that of Latinx households , with even bigger gaps for households with children. Given that disparity, Black residents are more than four times and Latinx residents are twice as likely as white residents to live in poverty .9
Non-financial requirements for Medicaid include being a resident of the District and being a US citizen or meeting a specifically eligible immigration status, such as a lawful permanent resident .10 Non-financial requirements used to also include being part of certain populations . In 2010, however, the District became one of the first jurisdictions to enact Medicaid expansion under the Affordable Care Act to all adults under age 65 meeting income requirements .11
Medicaid expansion also increased the income threshold for low-income adults to help them qualify for Medicaid.14 Financial eligibility for DC Medicaid and DC Healthy Families is calculated as a percentage of the Federal Poverty Level. Different age groups and populations are subject to different income limits, described in the addendum below.
Health Coverage For Children Under The Aca
Under the ACA, eligibility for children through Medicaid and CHIP remains strong. The ACA requires states to use a uniform definition of income, called Modified Adjusted Gross Income , to better coordinate eligibility across health care programs. Using MAGI, more than half of the states cover children in families with incomes at or above 250% FPL and 19, including DC, cover children in families with incomes at or above 300% FPL . The ACA protects the gains already achieved in childrens coverage by requiring states to maintain eligibility thresholds for children that are at least equal to those they had in place at the time the law was enacted through September 30, 2019.
Figure 5: Childrens Eligibility for Medicaid/CHIP by Income, January 2014
While all states have already significantly expanded coverage to children through Medicaid and CHIP, not all eligible children are enrolled in the program due to lack of parent knowledge about their eligibility and historic enrollment barriers. Over 5.2 million of the 14 million currently uninsured individuals who are estimated to be eligible for Medicaid in 2014 are children.16 In states not implementing the Medicaid expansion, children account for 75% of the uninsured eligible for Medicaid or CHIP .
Figure 6: Uninsured Adults and Children Eligible for Medicaid / CHIP, 2014
Recommended Reading: How To Become A Medicaid Consultant
What Are The Benefits Of Medicare
While Medicare plans have varying benefits, they must all provide a baseline of coverage. Part A plans must include:
- Inpatient hospital stays
- A yearly check-up
Part B plans also cover ambulance rides, medical equipment, and more.
Medicare does not cover long-term care in the home. It also does not include dental care, eye exams, foot care, and hearing aids.
What Does Medicaid Cover
Despite the draconian measures still in place in some states, over 67 million people were enrolled in Medicaid in February of 2018. If you add the roughly 6.4 million children who qualify for CHIP, a Medicaid expansion for children, the total number is roughly 74 million. Since the ACA passed, Medicaid expansion has added 16.3 million people to Medicaid and CHIP rolls.
In total, children comprise roughly half of Medicaid recipients. 35.7 million children were enrolled in either Medicaid or CHIP at the beginning of 2018. This means that one-third of American children are on Medicaid, and half of all births in the country are paid for by the program.
Though states craft their own Medicaid programs, there is a list of mandatory benefits that must be provided by the state. These include health services like hospital care, x-rays, pediatric services, and transportation to medical care. Some optional benefits include items that most people view as essential like prescription drugs, respiratory care, physical therapy, and dental services.
Recommended Reading: Dentist That Accept Medicaid In Sterling Heights Mi
Health Coverage Of Children Pre
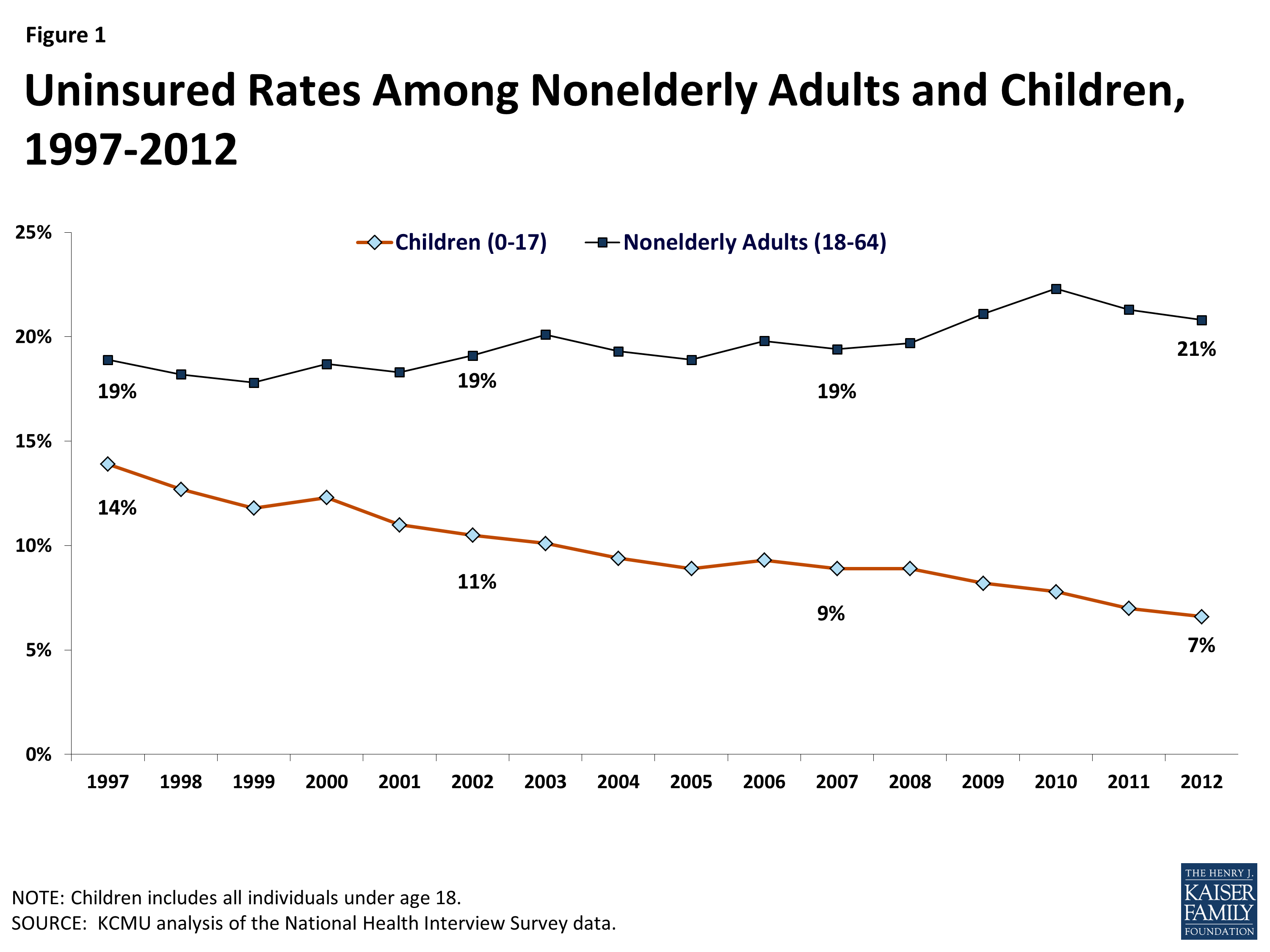
Experience with Medicaid and CHIP demonstrates that the combined effects of eligibility expansions, enrollment simplifications, and outreach efforts lead to increased coverage and reductions in the number of uninsured children over time. Medicaid provides the foundation of coverage for poor and near poor-children. CHIP was created in 1997 as a complement to Medicaid to provide coverage to uninsured children who were not eligible for Medicaid. CHIP, which provided states some flexibility on program design, as well as a higher federal match rate compared to Medicaid, helped spur efforts to expand eligibility to reach more low-income children, adopt strategies to simplify enrollment and renewal processes and conduct outreach and enrollment efforts. A year ahead of the implementation of the ACA, median eligibility levels for children were 235% FPL and states had adopted an array of enrollment simplification procedures to make it easier for children to obtain and maintain coverage. As a result of these combined efforts, Medicaid and CHIP have helped to reduce the uninsured rate for children to a record low of 7% in 2012. Coverage gains continued for children during the recent economic downturn when uninsured rates for adults climbed .
Figure 1: Uninsured Rates Among Nonelderly Adults and Children, 1997-2012
Figure 2: Uninsured Rates for Children by State, 2011-2012
Figure 3: Health Insurance Coverage of Children by Income and Race, 2012
