Medicaid Offers Additional Mental Health Support
Medicaid is the single largest payer for mental health services in the United States. While they didnt always include therapy as a benefit and limitations do still exist, Medicaid now covers this and a myriad of other substance use, mental health, and behavioral health services.
If youre enrolled in a Medicaid plan, some of your covered services may include:
- Psychological testing and evaluation
- Social work services
- Case management for chronic mental illness
Other services like tobacco use cessation, mental health skill-building, and peer support should also be covered. If youre experiencing mental health concerns or battling a substance use disorder, its important to seek professional care and get the diagnosis and treatment you need.
If you or a loved one are struggling with substance use or addiction, contact the Substance Abuse and Mental Health Services Administration National Helpline at 1-800-662-4357 for information on support and treatment facilities in your area.
For more mental health resources, see our National Helpline Database.
Medicare Part B And Partial Hospitalization
Partial hospitalization allows patients to avoid inpatient care while still receiving the more intensive psychiatric services their condition requires. Care is provided during the day, with the patient returning home at night.
Medicare Part B covers partial hospitalization when it is provided in either a community mental health center or hospital outpatient department setting. In addition, your doctor must certify that, without partial hospitalization, inpatient care would be required.
What Is Medicaid And Who Is Eligible
The United States government established Medicaid in 1965 as a financial support program for needy families and individuals, covering part or all medical expenditures. Each state has the authority to change its rules and regulations, although most fundamental medical therapies are covered in general.
Among people who are considered eligible usually, these groups are especially well-treated:
- Pregnant women
- Low-income adults aged 65 or older
- Low-income parents of Medicaid-eligible children
- Disabled adults receiving Social Security Disability
But does this mean that everyones mental health is covered? Keep reading until the end to find out all the specifics.
Recommended Reading: Dcbs Ky Medicaid Phone Number
Inpatient Mental Health Care Coverage
Medicare Part A covers mental health care services you receive when youre admitted as a hospital patient. For each benefit period, your costs in Medicare are as follows:
- $1,556 deductible
- $0 coinsurance per day for Days 1-60 and then $389 coinsurance per day for Days 61-90
- $778 coinsurance per each lifetime reserve day after Day 90 for each benefit period
- All costs each day after the lifetime reserve days
- 20% of the Medicare-Approved Amount
How Do I Check If My Medicaid Plan Covers Therapy
To check if your Medicaid plan covers therapy, find your Summary and Benefits document, which is usually mailed to you with your Medicaid card or is posted online. On this document, youll find your copayment or coinsurance rates per service type. Look for outpatient mental health services in the list to determine how much your plan covers and how much youll have to pay out-of-pocket, if anything.
If you cant find this information using your Summary and Benefits document, locate the customer service phone number on the back of your Medicaid card. The representatives on the hotline will be able to look up your health insurance plan and share with you information about your mental health benefits.
Also Check: How To Find A Therapist That Takes Medicaid
Latinx Older Adults Expressed More Need
When Gunja and colleagues looked closely at the data, they found that Latinx Medicare beneficiaries stood out.
A much greater share of Hispanic/Latinx adults 65 and over said they were diagnosed with a mental health condition, compared to White or Black beneficiaries in the U.S. Also, 42%, compared to the U.S. total of 28%, reported needing mental health care.
Hispanic/Latinx older adults were also more likely to report emotional distress, defined as anxiety or great sadness which the respondents found difficult to cope with by themselves in the past 12 months. Thirty-one percent of Hispanic/Latinx adults reported this, compared to 18% of all U.S. older adults combined.
Entrenched healthcare bias and stigma might be influencing differences between racial groups, the authors wrote. For example, although Black older adults were the least likely to report mental health diagnoses, studies have found that providers are more likely to underdiagnose Black adults for mood disorders than they are for other adults.
At the same time, the authors wrote, job loss due to COVID-19, as well as fears around changes in immigration policies, disproportionately impact the mental health of older Latinx adults. To better address this groups mental health need, further investigation and policy reforms are needed.
Support Act Section 1003 Demonstration Project Post
CMS released a Notice of Funding Opportunity to solicit applications for participation in the 36-month post-planning period of the demonstration project to increase the treatment capacity of providers participating under the Medicaid state plan to provide substance use disorder treatment and recovery services, as originally described in NOFO CMS-2C2-19-001 . Only the 15 states that participated in the planning period were eligible to apply for this funding opportunity.
The following State Medicaid agencies were selected in September 2021 to participate in the 36-month post-planning period: Connecticut, Delaware, Illinois, Nevada, and West Virginia.
Recommended Reading: What Does My Medicaid Cover
Inpatient Mental Health Services Covered By Medicare
Medicare Part A helps pay for mental health care services received as a hospital inpatient. This means that you have been admitted and are not under observation status.
As an inpatient, your Medicare Part A coverage includes:
- Room
- Therapy and other treatments for your condition
Medicare Part A also covers related services and supplies required for your treatment.
Please note that Medicare Part A only covers 190 days throughout your lifetime for inpatient care in a psychiatric hospital. Your out-of-pocket includes the Part A deductible per benefit period and coinsurance starting on day 61.
A benefit period begins when you are admitted as an inpatient and ends once you go 60 days without receiving inpatient care.
Demonstration Project To Increase Substance Use Provider Capacity
On October 24, 2018, the Substance Use Disorder Prevention that Promotes Opioid Recovery and Treatment for Patients and Communities Act became law. Under section 1003 of the SUPPORT Act, the Centers for Medicare & Medicaid Services , in consultation with the Substance Abuse and Mental Health Services Administration and the Agency for Healthcare Research and Quality, is conducting a 54-month demonstration project to increase the treatment capacity of Medicaid providers to deliver substance use disorder treatment and recovery services. The demonstration project includes:
- Planning grants awarded to 15 states for 18 months and
- 36-month demonstrations with up to 5 states that received planning grants.
States participating in the 36-month demonstration will receive enhanced federal reimbursement for increases in Medicaid expenditures for substance use disorder treatment and recovery services.
Read Also: Does Medicaid Cover Dermatology In Nc
Outpatient Mental Health Services Covered By Medicare
Original Medicare includes two parts. Medicare Part A covers inpatient services that you’d receive in a hospital or skilled nursing facility . Medicare Part B provides outpatient care, meaning care you typically receive outside of a hospital setting. Mental health providers covered by Medicare Part B include:
- Psychiatrists
- Clinical psychologists, clinical social workers, and clinical nurse specialists
- Nurse practitioners
- Physician assistants
Part B also helps pay for lab tests and durable medical equipment deemed medically necessary by your healthcare provider. It may also cover partial hospitalization services in the event you need “intensive coordinated outpatient care.”
As with your physical health, mental health coverage depends on your provider accepting assignment. This means they have agreed to accept the rate Medicare approves for covered services. Your out-of-pocket costs may include the Part B deductible and 20 percent coinsurance.
If you have a Medicare Supplement Insurance plan , make sure your healthcare provider knows. This ensures proper payment of your medical bills.
Medicaid Expansion Under The Affordable Care Act
The Affordable Care Act made more individuals eligible for Medicaid by eliminating some of the barriers to qualify. Under the ACA, there were only financial requirements. Qualifying adults must have income below 138% of the federal poverty level .
Not only did the ACA get rid of some of the qualification barriers, it also expanded the health benefits. There are 10 essential health benefits that all plans offered in the must provide. Mental health and substance use disorder service is included as one of the 10 essential health benefits. Substance use disorder is often referred to as substance abuse. The covered treatment includes but is not limited to behavioral treatment.
Also Check: Assisted Living In New Jersey That Accepts Medicaid
To Improve Behavioral Health Start By Closing The Medicaid Coverage Gap
Jennifer Sullivan, Miriam Pearsall, and Anna Bailey
Closing the Medicaid coverage gap is a critical step toward addressing the nations behavioral health crisis. In 2019, 2.2 million uninsured adults with incomes below the poverty line, which is too low to qualify for subsidized health insurance coverage in the Affordable Care Act marketplaces, were left without a pathway to coverage, because their states didnt expand Medicaid. Most of these adults live in the South, 60 percent are people of color, and more than 1 in 4, about 600,000 people, are estimated to have a behavioral health condition.
Improved access to coverage has been shown to increase access to behavioral health services by reducing financial barriers to care and increasing the number of behavioral health providers that accept Medicaid. Having health coverage has also been shown to improve mental well-being and reduce stress and anxiety among low-income people. For those without a pathway to coverage, closing the coverage gap would expand access to critically needed behavioral health services which include services to treat mental health conditions and substance use disorders at a time when the need for these services is high and increasing.
Policymakers have an opportunity to address the coverage gap in recovery legislation, which would help millions of currently uninsured people, many with behavioral health needs that can have fatal consequences when neglected, access the care they need.
How Much Does Medicare Pay For Mental Health Care Services

An annual depression screening is free if the doctor accepts Medicare assignment. Otherwise, Medicare Part B pays 80 percent of the Medicare-approved amount for most covered mental health care services. You are responsible for the remaining 20 percent, and the Part B deductible applies.
Medicare Advantage plans also help pay for mental health care services and may cover additional mental health services or items. Check with your plan provider to get coverage and cost details.
Also Check: Drug Rehab Centers In Illinois That Take Medicaid
Individual Or Group Counseling
Who is Eligible? Any Medicaid beneficiary with a medical need
How often? 52 hours per year applies to individuals age 21 and older only.
Info: This service can only be provided by agencies certified by the Ohio Department of Mental Health and Addiction Services. for a map to link you with eligible providers in your area and which services they provide.
Copay: $0
Does Medicare Pay For Inpatient Mental Health Care
Inpatient mental health care administered at a general hospital or psychiatric hospital is covered by Medicare Part A.
There is no lifetime limit to the number of days a Medicare beneficiary can receive covered mental health treatment during inpatient hospital stays at a general health hospital.
When treated at a psychiatric hospital, Medicare coverage of mental health care is limited to 190 days over the course of your lifetime.
If you receive inpatient care that is covered by Medicare, you will be responsible for the Medicare Part A deductible, which is $1,408 per benefit period in 2020. If your inpatient hospital stay lasts longer than 60 days, youll then be required to pay additional Part A coinsurance costs.
Also Check: Does Medicaid Cover Hearing Aids In Florida
Medicaid Coverage And Eligibility Requirements Vary Widely From State To State
Medicaid is a joint federal and state program that allows states to have some flexibility in what and who they cover. Some states have stricter income and categorical eligibility requirements than others, especially the 12 states that have elected not to accept Medicaid expansion as of April 2022.
While federal statutes require state Medicaid programs to cover essential benefits like nursing facility services and physician services, other services, like clinic services and psychosocial rehabilitation, are optional. So, some mental health services are covered by Medicaid in some states but not in others.
According to MACPAC, all 50 state Medicaid programs cover individual and group therapy, and most also cover family therapy. Specifically, every states Medicaid plan currently covers some form of outpatient mental health services, which generally includes individual and group counseling. Many states plans also cover family counseling.
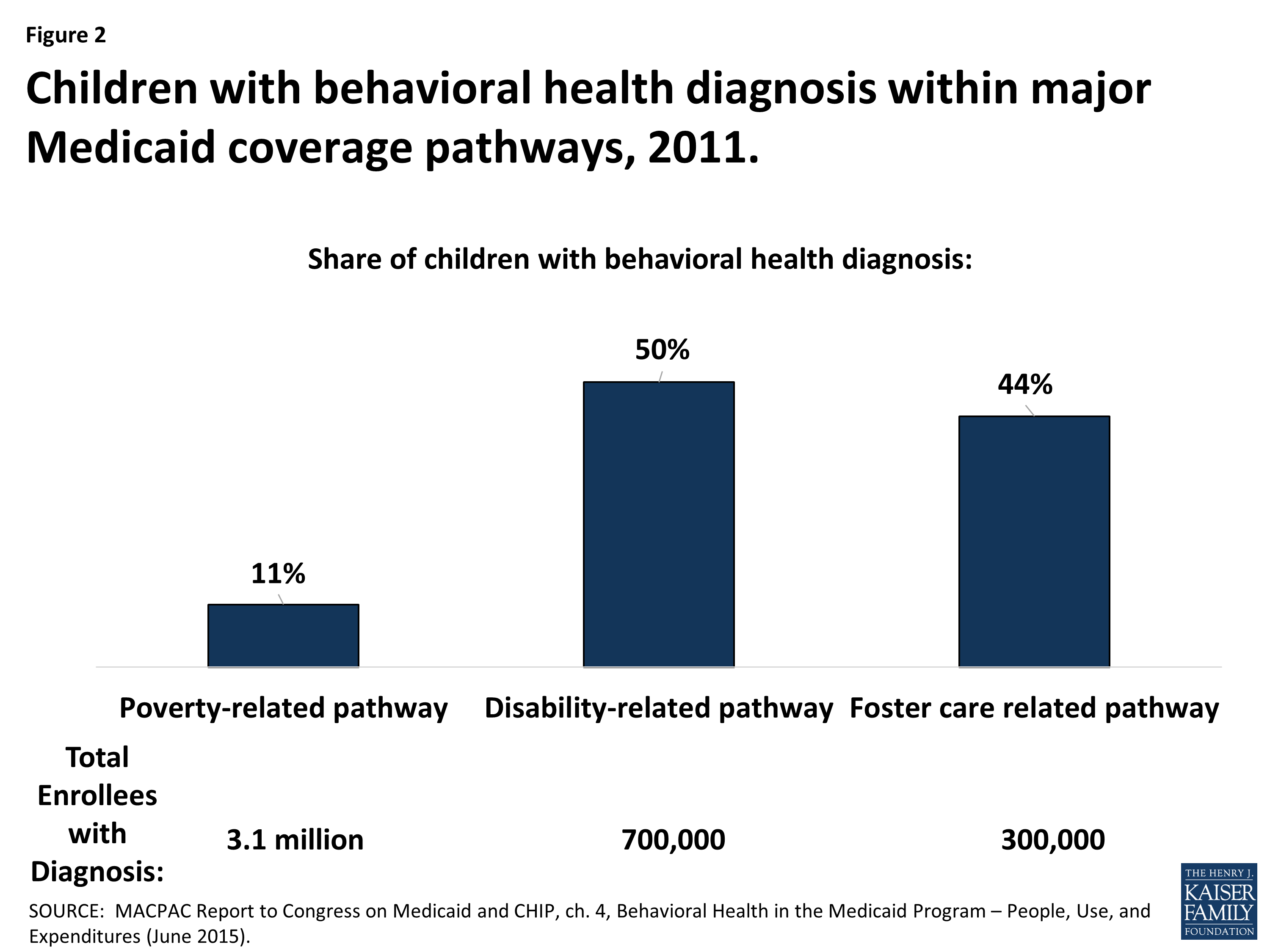
Does Medicaid Cover Mental Health For Children
Yes, children and young people under the age of 21 are always treated with greater care. This includes the mandated mental health coverage required in all states.
It has long been established that the greatest therapy for any condition is prevention, and mental health and care are no exception. Children are especially vulnerable and require access to all treatments as well as Medicaid coverage with no co-payment.
So, if your child is suffering from a mental ailment, you can now rely on Medicaid for financial support.
Also Check: Michigan Medicaid Nursing Home Application
Medicare Inpatient Mental Health Services
If you do need inpatient care as part of your treatment, Medicare Part A covers services during an inpatient hospital or psychiatric hospital stay. Theres a limit to Medicare coverage if you stay at a psychiatric hospital thats dedicated to treating mental health patients, as opposed to a general hospital. Medicare Part A pays for up to 190 days of psychiatric hospital care in your lifetime.
Even during inpatient stays, Medicare Part B still covers certain mental health benefits, such as physician services.
Rural And Remote Support
If you live in a remote area, it might be hard to see a mental health professional. You may be able to have a telehealth video consultation instead. You can claim for video consultation sessions with a mental health professional.
Ask your GP or mental health professional if they offer this service. You can also search the find a health service tool on the healthdirect website for mental health telehealth services.
Find out more about Medicare services for rural and remote Australians.
You May Like: Does Medicaid Cover Prenatal Care
What Is Covered Under Mainecare
Generally, MaineCare covers the costs of going to the hospital, going to see your doctor, getting medical supplies, or receiving long term care in your own home, assisted living facility, or skilled nursing facility. The amount of your MaineCare benefit is based on your income, age, medical needs, and family situation.
Does Medicare Cover Mental Health Therapy
Yes, Medicare covers mental health care, which includes counseling or therapy. Depending on your needs, mental health care can be provided in a variety of settings. The goal is that you get the right kind of support when you need it.
Mental health pertains to our emotional, psychological, and social well-being. Our mental health can impact how we think, feel, and act. From a holistic, whole-person perspective, mental health plays a big part in our general overall health. Just as Medicare helps cover physical ailments, it also offers various benefits to support emotional, psychological, and social health.
Mental health concerns include anxiety and depression, substance abuse, eating and stress disorders, schizophrenia, and attention-deficit/hyperactivity disorders. These concerns can range from mild to severe and can be addressed on an outpatient or inpatient basis.
You can access mental health benefits through Original Medicare or Medicare Advantage plans, an alternative to Original Medicare. MA plans offer the same services, follow the same Medicare rules as Original Medicare, and generally require in-network providers, referrals, and prior authorization to receive benefits.
You May Like: What Does It Cost For Medicare Part B
Read Also: What Are The Qualifications For Medicaid In Colorado
Timeline Of Federal Health Insurance Parity Policies
1961
President Kennedy directs the Civil Service Commission to implement parity
1970s through present day
Parity laws enacted in many states – mostly for small group health plans some for individual policies many states establish minimum benefit level requirements for mental health and substance use disorders – employer-sponsored group health plans are generally exempt
1992
The first federal parity legislation is introduced in Congress by Senators Pete Domenici and John Danforth
1996
The Mental Health Parity Act enacted requiring comparable annual and lifetime dollar limits on mental health and medical coverage in large group health plans including employer-sponsored group health plans
1999
President Clinton directs the Office of Personnel Management to implement parity in the Federal Employee Health Benefit Plan
2003
President Bush’s New Freedom Commission on Mental Health includes a recommendation regarding parity in the Commission’s Final Report
2008
Paul Wellstone and Pete Domenici Mental Health Parity and Addiction Equity Act is signed into law – applying to large group health plans including employer-sponsored plans, effective for most plans starting in 2010
Medicare Improvements for Patients and Providers Act enacted including a provision to phase out statutory provision requiring a higher co-pay for outpatient mental health services
2009
Q What Can I Do If I Think I Need Mental Health Or Substance Use Disorder Services For Myself Or Family Members
Here are three steps you can take right now:
Recommended Reading: Dentist In Woodbridge Va That Accept Medicaid
