Does My Parent Need Assisted Living
Still not sure if your parent needs assisted living? Lets go over a few example scenarios to help clear things up:
SCENARIO #1
Is Mary a good fit?
Yes. Most important, in an assisted living community, Mary could receive help with medication management. Meals would also be provided, and the housekeeping would be taken care of for her.
SCENARIO #2
Richard
Richard suffered a fall and hospitalization about three months ago. He has since recovered, but his children are worried. Hes a bit unsteady on his feet, and although he insists hes fine, theyve noticed that he has issues getting around the house and dressing himself. He used to love being out and about, but now hes always at home.
Is Richard a good fit?
Yes. When mobility becomes a concern, assisted living can be a good fit. The suites are designed with senior needs in mind, and theres a trained, professional staff available around the clock in the event of a fall, or if Richard needs help getting dressed in the mornings. Additionally, there will be plenty of activities and programs to get him back to his social self.
SCENARIO #3
Dottie
Dotties daughter has noticed recently that Dottie isnt cooking anymore. She usually goes out to eat or heats up frozen meals. Also, the house is getting messy. When her daughter asks her if everythings okay, Dottie is dismissive and says she just doesnt bother with it anymore.
Is Dottie a good fit?
Researching assisted living? We have resources that can help.
Does New Jersey Help With My Medicare Premiums
Many Medicare beneficiaries who struggle to afford the cost of Medicare coverage are eligible for help through a Medicare Savings Program . In New Jersey, these programs pay for Medicare Part B premiums, Medicare Part A and B cost-sharing, and in some cases Part A premiums.
- Qualified Medicare Beneficiary : The income limit is $1,063 a month if single and $1,437 a month if married. QMB pays for Part A and B cost sharing, Part B premiums, and if a beneficiary owes them it also pays their Part A premiums.
- Specified Low Income Medicare Beneficiary : The income limit is from QMB levels up to $1,276 a month if single and $1,724 a month if married. SLMB pays for Part B premiums.
- Qualified Individuals : The income limit is from SLMB levels up to $1,436 a month if single and $1,940 a month if married. QI pays for Part B premiums.
MSP asset limits: The asset limits for QMB, SLMB and QI are $7,860 if single and $11,800 if married.
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
Also Check: Dentist That Take Medicaid In Ri
Medicaids Rules For Immigrants:
- Undocumented immigrants do not qualify for full Medicaid coverage, but they may qualify for Medicaid coverage for emergency services.
- Most immigrants who have been lawfully present for less than five years do not qualify for full Medicaid coverage. However, they may qualify for private coverage subsidized by the government.
- Immigrants who have been lawfully present for five years or longer and some other noncitizens who meet specific noncitizen requirements qualify for the same programs that U.S. citizens can get.
Unitedhealthcare Dual Complete Plans

Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the planâs contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
Recommended Reading: Income Guidelines For Medicaid Missouri
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comunÃquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
This is not a complete list. The benefit information is a brief summary, not a complete description of benefits. For more information contact the plan or read the Member Handbook. Limitations, copays, and restrictions may apply. For more information, call UnitedHealthcare Connected Member Services or read the UnitedHealthcare Connected Member Handbook. Benefits, List of Covered Drugs, pharmacy and provider networks and/or copayments may change from time to time throughout the year and on January 1 of each year.
How Does New Jersey Regulate Long
Medicare beneficiaries increasingly rely on long-term services and supports or long-term care which is mostly not covered by Medicare. In fact, 20 percent of Medicare beneficiaries who lived at home received some assistance with LTSS in 2015. Medicaid fills this gap in Medicare coverage for long-term care, but its complex eligibility rules can make qualifying for benefits difficult. Whats more eligibility rules vary significantly from state to state.
Medicaid nursing home coverage
Income limits: The income limit is $2,349 a month if single and $4,698 a month if married . When only one spouse needs nursing home care, many states only count that spouses income toward the eligibility limit.
This income limit doesnt mean nursing home enrollees can keep all of their income up to the limit. Instead, enrollees must pay nearly all their income toward their care, other than a small personal needs allowance and money to pay for health insurance premiums .
Assets limits: The asset limit is $2,000 if single and $3,000 if married . If one spouse doesnt need Medicaid, the other spouse can keep up to $128,640.
Certain assets are never counted, including many household effects, family heirlooms, certain prepaid burial arrangements, and one car.
Applicants are not allowed to have more than $893,000 in home equity.
Home and Community Based Services waivers
Income limits: The income limit is $2,349 a month if single and $4,698 a month if married .
Estate recovery in New Jersey
Also Check: Qualifications For Medicare And Medicaid Benefits
What If I’m Pregnant
A. NJ FamilyCare covers low income pregnant women too! Apply online at www.NJFamilyCare.org or visit your County Welfare Agency. Pregnant women already enrolled in NJ FamilyCare should contact and advise them. NJ FamilyCare wants to be sure they are receiving all of the benefits that pregnancy entitles them to receive.
What Does Medicaid Cover In New Jersey
Coverage by Medicaid in New Jersey will include things like:
- Mental health services that are provided in a doctors office, an approved mental health clinic, or a hospital
- Medical services that are provided by a doctor in an office, clinic, or another medical facility
- Prescription drugs obtained from a pharmacy this also includes some types of over the counter medications
- Home health services, nursing home care, medical day care, or a personal care assistant
- Services from chiropractors, dentists, podiatrists, psychologists, and optometrists
- Eyeglasses, hearing aids, artificial limbs, braces, and orthopedic shoes
- Outpatient and inpatient hospital care, rehabilitation services and hospice care
- Clinic services like speech, occupational, and physical therapies
- Laboratory services, X-rays, and durable medical supplies and equipment
- Transportation to any services that Medicaid covers
Also Check: Ga Medicaid Income Limits 2020
What Does It Mean That I Have To Renew My Insurance Every 12 Months
Renewal is simply a way of checking to see if anything has changed in your family’s situation. You may be sent a preprinted form to confirm your income status and household size or you may be sent a blank application to fill out. It is very important that you immediately respond to any written request so that your insurance coverage will not be lost or interrupted.
Assisted Living Admission Requirements
New Jersey assisted living facilities have no restrictions or requirements that limit admission. However, if a resident does require long-term, specialized care, such as needing continued access to respirators or needing intensive behavioral management, mandatory discharge is required. Additional discharge requirements are left up to the discretion of the facility. These may include prolonged illnesses that require 24-hour nursing, or a resident becoming a danger to themselves or others.
An initial assessment must be conducted for all residents upon admission to determine the needs of the resident. A healthcare assessment should be completed within 14 days of admission if the initial assessment shows that the resident has specific health needs, and may only be conducted by a registered nurse or medical professional employed by either the facility or the DOH. Residents must also have continued reassessments in a time frame that is consistent with their health service plan.
Don’t Miss: What Is Medicaid Buy In Program
Thoughts On Learn Which Facilities In Nj Accept Medicare Or Medicaid
Hello. Im a unit manager in New Jersey looking for a assisted living willing to take a patient with medicaid. Can I please get a list of facilities that can help place our beloved resident.
please help me find assistant living in new jersey that accepts medicade
Im looking for an assisted living facility for my mother that accepts medicaid early on. Im finding that most of the places wont accept until two years in. She receives S.S. and a minimal amount of money in the bank.
Are there any assisted living facilities available for my mother shes on social security, if so when.?
iam seeking long term Medicaid assisted living facilitiy for myseif
I am seeking an assisted living facility for my mother that accepts Medicaid, in the Trenton area or Ocean County. She is 91 yrs. old, and only has her social security.
Donât Miss: Yearly Income To Qualify For Medicaid
Add Other Family Members
The second critical step involves counting all of your family members. You do not want to miss anyone, as each additional family member boosts the monthly income limit by $757.
You determine your household size based on how you intend to file income taxes for the current tax year.
- Tax Filer: yourself, spouse, plus dependents
- Claimed as Dependents: same as tax filer with some exceptions
- Non-Filers: yourself, your spouse if living with you, children under 19
Read Also: Is Geisinger Ghp Family Medicaid
New Jersey Has Accepted Federal Medicaid Expansion
- 2,053,575 Number of New Jerseyans covered by Medicaid/CHIP as of October 2021
- 769,724 Increase in the number of New Jerseyans covered by Medicaid/CHIP fall 2013 to October 2021
- 40% Reduction in the uninsured rate from 2010 to 2019
- 54% Increase in total Medicaid/CHIP enrollment in New Jersey since Medicaid expansion took effect
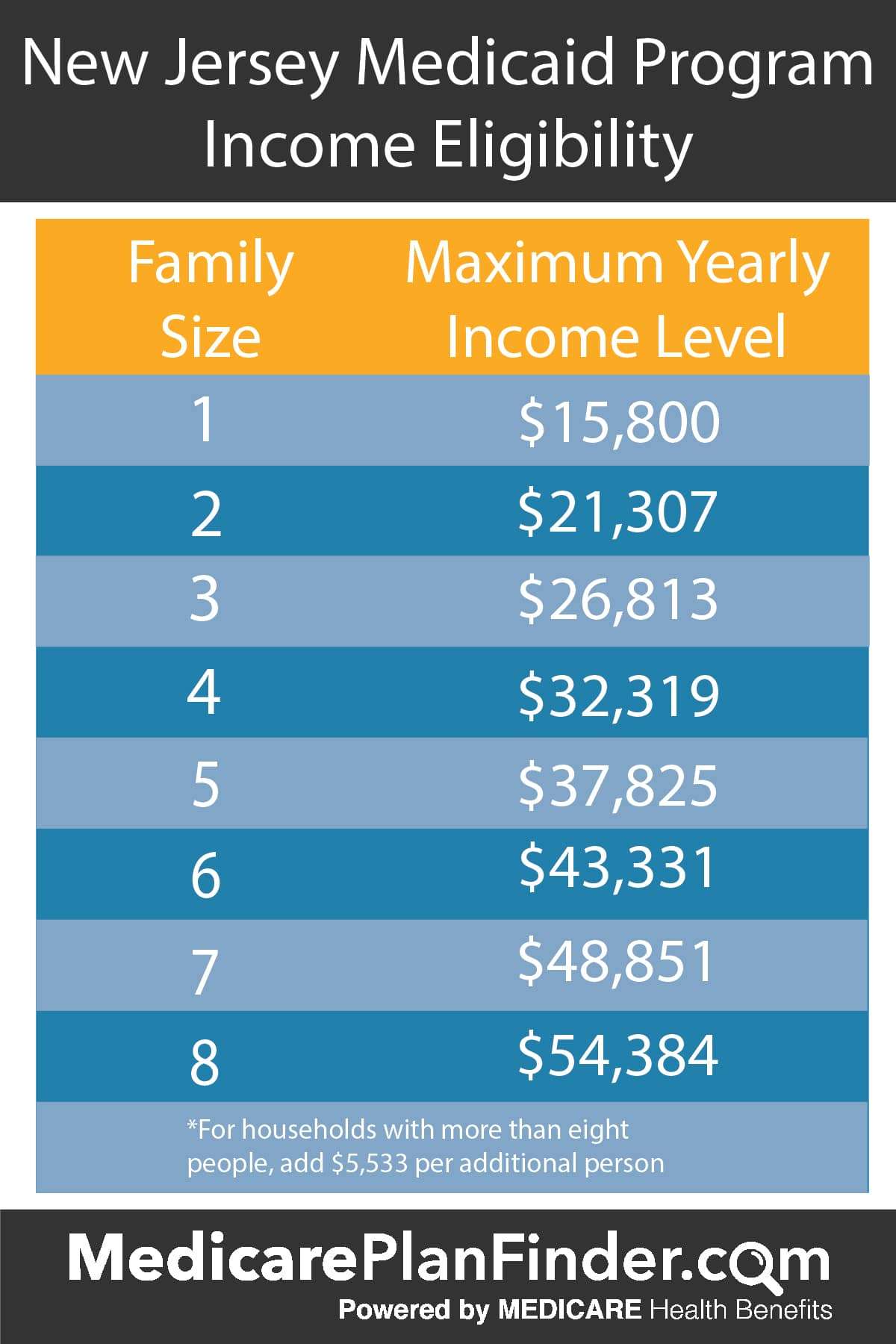
New Jersey Medicaid Income Limit
The New Jersey Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the New Jersey Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 194 percent of FPL
- Any child age 1-5 with a family income up to 142 percent of FPL
- Children ages 6- 18 with family income up to 142 percent of FPL
- CHIP for children with family income up to 350 percent of FPL
- Pregnant women with family income up to 194 percent of FPL
- Parents of minor children with family income up to 29 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 100% of the FPL
- Adults without dependents under Medicaid expansion with income up to 133% of the FPL
Don’t Miss: Does Walmart Vision Center Accept Medicaid For Contacts
Medicare Supplement Insurance Plans
Medicare beneficiaries must pay deductibles, copays, coinsurance and other out-of-pocket costs. Many beneficiaries in New Jersey purchase Medicare Supplement Insurance, also known as Medigap, to cover these extra expenses.
Medigap plans are sold by private insurance companies and have a premium that depends on factors such as the enrollee’s location and the amount of coverage provided. Any time a beneficiary incurs a medical expense, Medicare pays its share of the costs before the Medigap coverage kicks in.
Massachusetts, Minnesota and Wisconsin standardize their Medicare Supplement Insurance plans differently than New Jersey and the other 46 states.
How Many People Are On Medicaid
According to the Centers for Medicare & Medicaid Services, as of November 2020, here are the number of people enrolled in Medicaid and Chip in the entire United States:
- 78,521,263 individuals were enrolled in Medicaid and CHIP
- 72,204,587 individuals were enrolled in Medicaid
- 6,695,834 individuals were enrolled in CHIP
Also Check: Qualifying For Medicaid In Arizona
Comprehensive Personal Care Home
A Comprehensive Personal Care Home is a facility thats approved by the Department of Health to provide:
- Assisted Living Services
- Arrange for resident transportation to and from health care services
In a CPCH:
- The stove in the kitchen can be removed if it is a safety hazard
- There is a front door that can be locked from inside
- You can get to your own apartment kitchen at any time to get food and drinks
- You may share a unit with another person
You cannot receive this service at the same time as:
- Adult Day Health services
You May Like: Having A Baby On Medicaid
Cost And Coverage Of Medicaid In New Jersey
When your application for Medicaid has been approved, you will receive a letter in the mail that will give you the information regarding the premium for your coverage. This cost will be determined by a variety of factors that will include your family or household size, income, how many people will need coverage, and more.
Don’t Miss: Medicaid Fraud Statute Of Limitations
Get The Insights You Need To Find The Right City
Families looking for assisted living in New Jersey have a wide array of communities to choose from, since estimated that there are more than 30,000 assisted living communities serving seniors across the U.S., and over 262 statewide. The state is also home to a rapidly growing number of senior citizens, with adults over 65 making up an estimated 16 percent of the population. A resident in an assisted living community in New Jersey will pay $6,065 per month on average.
Also Check: Does Medicaid Cover Gastric Balloon
What Is The Income Limit For Medicaid In New Jersey

The income limit for New Jersey Medicaid depends on an applicant’s age, medical status and/or family situation. For adults without dependent children and parents/caretakers with dependent children, the income limit is set at 138% of the federal poverty level . New Jersey FamilyCare, like other Medicaid programs, uses Modified Adjusted Gross Income to determine if an applicant is under the income limit. MAGI is calculated by taking an individual’s adjusted gross income and adding back deductions taken for things like student loan interest, rental losses and tuition and fees.
The table below shows the income limit for New Jersey Medicaid based on household size. These limits apply to adults without dependent children and parents/caretakers with tax-dependent children.
|
Household Size |
The limits are higher for pregnant women, up to 205% of the FPL, and children under 18, up to 355% of the FPL.
Recommended Reading: Can A Single Person Get Medicaid
Why Seek Legal Advice Before You File A Medicaid Application In New Jersey
As life expectancies and long-term care costs continue to rise, the challenge quickly becomes how to pay for these services. Many people cannot afford to pay $8,500 to $13,000 per month or more for the cost of a nursing home, assisted living or home-based care. Those who can pay for a while may find their life savings wiped out in a matter of months, rather than years.
Fortunately, the NJ Medicaid Program can help. In fact, in our lifetime, Medicaid has become the long-term care insurance option for the middle class. But eligibility to receive Medicaid benefits requires that you pass certain eligibility tests involving your income and assets.
Resource Limit For Long
You must have few resources in order to qualify financially for Medicaid. In New Jersey, applicants for long-term care can have assets up to $2,000, or $3,000 for a married couple with both spouses applying. For applicants to regular Medicaid , the resource limits are higher, so that an individual can have up to $4,000 in resources and still qualify. A couple with both spouses applying can have up to $6,000 in assets.
People who qualify for the Medically Needy Program are also allowed up to $4,000 in resources, or $6,000 for a couple with both applying. Keep in mind that if you are entering a nursing home and your spouse is not, you will be allowed to keep extra income and resources to support your spouse, according to New Jersey’s “community spouse allowance” rules.
Not all property counts toward the resource limit. In New Jersey, your home is an exempt resource as long as it is your principal residence. But when you live away from your home for six months , it is presumed to not be your principal residence anymore — unless your spouse still lives there. Also, one car is exempt regardless of its value, as long as you or a family member uses it for transportation.
Also Check: United Healthcare Medicaid Dental Plan
