Can You Have Both
People who qualify for both Medicare and Medicaid are considered dual eligible. In this case, you may have original Medicare or a Medicare Advantage plan , and Medicare will cover your prescription drugs under Part D.
Medicaid may also cover other care and drugs that Medicare doesnt, so having both will probably cover most of your healthcare costs.
Q How Long Will My Medicaid Benefits Remain Active
A. Medicaid is based on month to month eligibility. However, your benefits are redetermined on a yearly basis by DMMA to confirm whether you still remain eligible for the program you are receiving. Certain Medicaid programs require you to report changes in your situation within 10 days of the change. One example of a change that must be reported is new employment.
Medicaid And Assisted Living
Medicaid waiver usually covers some approved assisted living services. As a result, seniors can expect assistance with medical treatment and personal care costs, which will lower their overall bills. On the other hand, the waiver program does not pay for the cost of room and board in an assisted living facility.
In most states, Medicaid can be used to pay for the following:
- Help with ADLs like toileting, mobility, and dressing
- Home health services, which may be provided in an assisted living community
- Physical, occupational, or speech therapy
- Medication management
Don’t Miss: Qualify For Medicaid Washington State
Spousal Impoverishment Prevention Coverage
This coverage applies to couples where one needs Nursing Care Services in a facility or at home.
The spouse receiving the nursing care services is allowed $3,000. The spouse who remains in the community is entitled to keep half of the couple’s countable assets, but not less than $26,076 and not more than $130,380 for calendar year 2021.
The spouse receiving the nursing care services may keep up to $65 of their monthly income and may deem income to bring the income of the spouse in community up to $2,550 per month and any dependent household members up to $718.
Effective Date Of Coverage
Once an individual is determined eligible for Medicaid, coverage is effective either on the date of application or the first day of the month of application. Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
Recommended Reading: Sign Up For Medicaid Health Insurance
How Do I Know If I Should Be Dual Eligible
Beneficiaries can find out if theyre eligible for Medicaid by contacting their Medicaid office. An Internet search for Medicaid offices in a beneficiarys state should provide the number to call but beneficiaries should make sure they are contacting a government office before sharing any personal information.
The Centers for Medicare and Medicaid Services also maintains a list of state agencies that oversee Medicaid. Beneficiaries can see if they already have Medicaid by contacting 1-800-MEDICARE and asking whether they receive Extra Help with their prescription drug costs .
Medicare Part D And Medicare Advantage Plans
Medicare beneficiaries can get prescription drug coverage in one of two ways:
- They can purchase a standalone Medicare Part D prescription drug plan
- They can enroll in a Medicare Advantage plan that includes prescription drug coverage
Beneficiaries who are enrolled in Medicare Part A and Part B can consider enrolling in a Medicare Part D drug plan.
Medicare Advantage plans are issued by private insurance companies that agree to provide all of the same covered services as Parts A and B. Many Part C plans also add in extra benefits, such as routine vision and dental care, which Original Medicare doesnt cover. Most Medicare Advantage plans include prescription drug coverage.
Don’t Miss: How To Renew Medicaid Nc
Medicaid Application Processing Timeline
In most cases, Medicaid applications are handled within 45 days of receipt or 90 days if a disability assessment is required. However, in order to collect the necessary paperwork for the application process, a family needs to add several weeks to that estimate. It can be challenging to reapply for Medicaid in a different state, whether for oneself or a family member.
Assignment: Describe The Qualifications To Receive Medicare And/or Medicaid How Can This Be Modified To Serve More People Who Are Considered A Vulnerable Population This Week You Will Reflect Upon T
Assignment:
Describe the qualifications to receive Medicare and/or Medicaid. How can this be modified to serve more people who are considered a vulnerable population?
This week you will reflect upon the Medicare and Medicaid programs to answer the following questions:
- How does Medicare affect medical billing?
- Briefly define the qualifications for Medicare and Medicaid benefits.
- Describe the impact that the ACA has had on Medicare and Medicaid recipients.
Length:
1000-1250 words answers must thoroughly address the questions in a clear, concise manner
References:
Two scholarly references are required you should include the appropriate APA style in-text citations and references for all resources utilized to answer the questions
Nickitas, D. M., Middaugh, D. J., & Aries, N. . Policy and politics for nurses and other health professions : Advocacy and action. Sudbury, MA: Jones and Bartlett Publishers. Chapters 12 & 13
Katz, M. . As needed for research.
Don’t Miss: New York State Medicaid Customer Service Number
Unitedhealthcare Senior Care Options Plan
UnitedHealthcare SCO is a Coordinated Care plan with a Medicare contract and a contract with the Commonwealth of Massachusetts Medicaid program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is a voluntary program that is available to anyone 65 and older who qualifies for MassHealth Standard and Original Medicare. If you have MassHealth Standard, but you do not qualify for Original Medicare, you may still be eligible to enroll in our MassHealth Senior Care Option plan and receive all of your MassHealth benefits through our SCO program.
What Is Medicaid Understanding The Basics
Medicaid is a health-insurance program for low-income people of all ages that are jointly supported by the state and the federal government. Medicaid covers medical treatment, such as physician visits, as well as non-medical support services, such as in-home personal care, through the state plan. The state program also pays for nursing home care. As a result, Medicaid may cover virtually all of a seniors long-term care costs if he or she is financially and medically eligible.
Medicaid programs must adhere to federal regulations. The federal government contributes a share of the expenditures, but each state manages Medicaid independently. As a result, coverage and expenses may vary depending on your states demands and economic goals. One of the most perplexing aspects of this system is that most states offer several programs aimed at different groups of people. In California, for example, Medicaid is known as Medi-Cal. And the waiver program that pays for assisted living services is called ALW.
In addition to the regular Medicaid, there are also special and different poverty-level programs for the Aged, Blind or Disabled people. In this guide, well focus on institutional Medicaid, which is one of the more relevant programs for older persons.
Recommended Reading: Aged Blind Disabled Medicaid Nj
Extra Help Program For Medicare Part D
Medicaid is not the only government-sponsored resource that helps pay for medical costs. An individual can also apply for Extra Help, a program that helps beneficiaries with Medicare Part D, which covers prescription drug costs.
To qualify for Extra Help, a personâs combined investments, real estate, and savings must not exceed $29,160 if a person is married and living with their spouse or $14,610 if a person is single.
A person can visit Medicareâs website to find out more about getting and applying for Extra Help.
Explaining Medicaid Medicare & Dual Eligibility
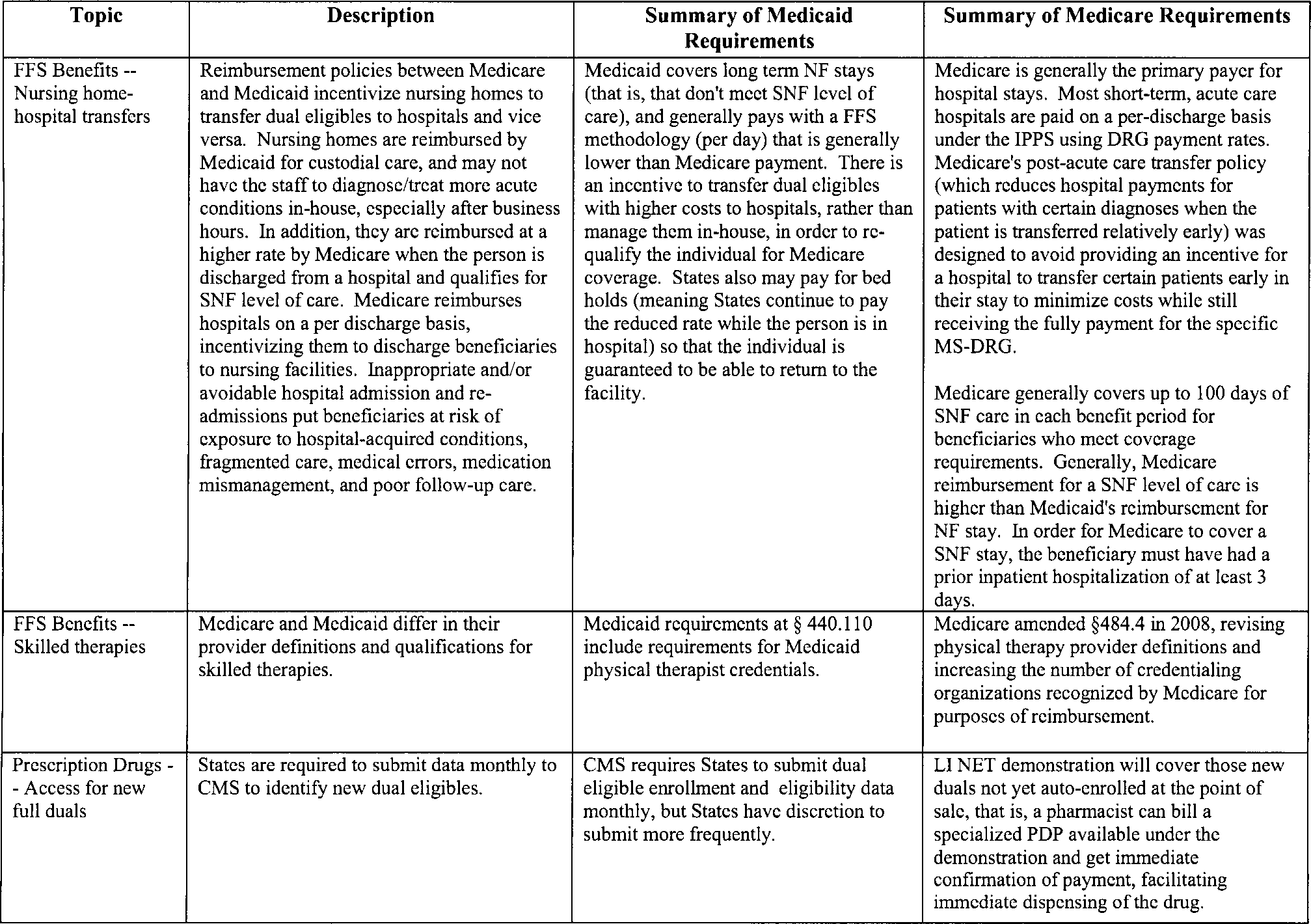
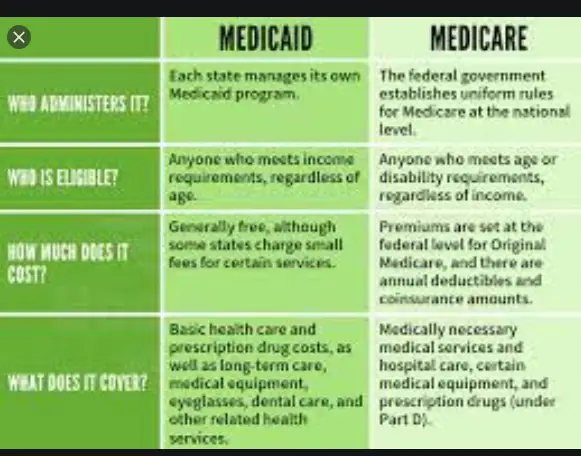
There are two key differences between the governmental health insurance programs Medicaid and Medicare:
Medicaid is run by ones state of residence, and Medicare is run by the federal government. Medicaid is for financially needy people who have monthly income and assets below a certain amount, while Medicare is for all Americans who are 65 or more years old and/or disabled.
Some benefits overlap, while others do not. Both programs pay for medical costs including doctor appointments and hospital care, but only Medicaid will cover all the costs of living in a nursing home for more than 100 days. Medicaid is also the program for receiving long-term care services at home or in assisted living, as Medicare does not pay for long-term care .
To be dual-eligible, one must meet the income requirements of their states Medicaid program, meaning having income and assets below a certain amount, and meet the age requirement for Medicare, meaning 65 and over. Put simply, dual eligibles will be low-income and above the age of 64.
Dual eligibles receive a combination of benefits from both programs.
Medicare Benefits
Medicare is broken into types: Medicare Part A provides hospital insurance . Medicare Part B is medical insurance . Medicare Part C is also called Medicare Advantage, and it provides benefits through a private insurer . Medicare Part D covers prescription drugs.
Medicaid Benefits
Recommended Reading: Eye Doctor Accepts Medicaid Insurance
Medicaid And Dementia Care
Though not all communities accept Medicaid, it does pay for 24-hour dementia care in many memory care facilities and memory-related care in skilled nursing communities. This typically includes all lodging and board expenses as well. Medicaid laws require seniors to devote the majority of their available money to their care, with only a little monthly personal allowance remaining.
Medicare Vs Medicaid: Key Differences In Coverage And Benefits
- What are the differences between Medicare and Medicaid? How do they work together, and can the same person use both for full health insurance plancoverage?
Healthcare in the United States can be confusing for new beneficiaries. This is especially true for Americans who may qualify for Medicare and/or Medicaid health coverage.
People who are currently, or who soon will be, eligible for Medicare need to know about the differences between the Medicare and Medicaid programs, including the benefits that are offered by each type of coverage.
Read Also: Does Medicaid Cover Alternative Medicine
Learn About Medicaid Penalties
Medicaid has a look-back period of 60 months in general prior to the application date. It reviews applicants all types of asset transfers during this period of time. If any look-back rule is violated, a penalty period of Medicaid ineligibility will be established. It ensures that no assets were given away or sold for less than fair market value.
The penalty period usually begins when an applicant applies for Medicaid it does not begin when a disqualifying transfer is done. In some states, the penalty period may start on the first day of the month after the denial of a Medicaid application. One can reapply for long-term care Medicaid after the penalty period has passed.
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
Read Also: How Long Does It Take To Get Approved For Medicaid
Having Dual Eligibility For Medicaid & Medicare: Who Is Eligible And Benefits
SummaryMedicaid is a health insurance program run by each individual state for people who are low-income, and Medicare is a national health insurance program for all Americans over 65. People who are eligible for both Medicaid and Medicare are considered dual eligibles. While some benefits are available through both programs, there are also differences in coverage that make dual eligibility a good way for many seniors to pay for their care needs. Only Medicaid, for example, pays for long-term nursing home care.
How Medicaid Planners Can Help
Medicaid planning can entail a wide range of services pertaining to Medicaid eligibility and application. A Medicaid planner may do one or more of the following tasks, depending on the needs of the client:
- Explain Medicaid eligibility and the application process
- Gather necessary documents for the client
- Check a clients application file to ensure they have all the necessary information and documents before submission
- Provide asset structure advice
- Help clients meet financial eligibility requirements
Read Also: How Much Does Medicaid Cover For Nursing Home
Whos Eligible For Medicaid Coverage
Medicaid eligibility is typically based on income and family size. Here are two ways to find out if you qualify.
-
Review your states Medicaid website. If there is an option to apply online, you can submit your application.
-
Complete an application on healthcare.gov using the Health Insurance Marketplace. Youll find out what programs you qualify for after you submit your application.
Minimum Requirements For Drivers Section 209

Section 209 of the Consolidated Appropriations Act, 2021 also adds a NEMT provider and driver requirement. Specifically, Section 209 added Section 1902 of the Social Security Act requiring the Medicaid Plan to provide for a mechanism which may include an attestation that ensures any provider including transportation network companies and individual drivers meet specific minimum requirements. Those minimum requirements are:
Read Also: Does Medicaid Pay For Dentures In Nc
Program Financing Beneficiary Liabilities And Provider Payments
All financial operations for Medicare are handled through two trust funds, one for the HI program and one for the SMI program. These trust funds, which are special accounts in the U.S. Treasury, are credited with all receipts and charged with all expenditures for benefits and administrative costs. The trust funds cannot be used for any other purpose. Assets not needed for the payment of costs are invested in special Treasury securities. The following sections describe Medicare’s financing provisions, beneficiary cost-sharing requirements, and the basis for determining Medicare reimbursements to health care providers.
Who Is Eligible For Medicaid
You may qualify for free or low-cost care through Medicaid based on income and family size.
In all states, Medicaid provides health coverage for some low-income people, families and children, pregnant women, the elderly, and people with disabilities. In some states the program covers all low-income adults below a certain income level.
- First, find out if your state is expanding Medicaid and learn what that means for you.
- If your state is expanding Medicaid, use this chart to see what you may qualify for based on your income and family size.
Even if you were told you didn’t qualify for Medicaid in the past, you may qualify under the new rules. You can see if you qualify for Medicaid 2 ways:
- Visit your state’s Medicaid website. Use the drop-down menu at the top of this page to pick your state. You can apply right now and find out if you qualify. If you qualify, coverage can begin immediately.
- Fill out an application in the Health Insurance Marketplace. When you finish the application, we’ll tell you which programs you and your family qualify for. If it looks like anyone is eligible for Medicaid and/or CHIP, we’ll let the state agency know so you can enroll.
Also Check: Does Missouri Medicaid Cover Assisted Living
Who Qualifies For Medicaid
To be eligible for full Medicaid coverage, you must first be a United States citizen or lawful permanent resident. Ones income determines Medicaid eligibility. Your eligibility is also determined by whether you have a disability, the size of your family, and your age. Though the requirements differ by jurisdiction, both your assets and income are taken into account. Some seniors may be eligible for both Medicare and Medicaid.
Medicare And Medicaid Dual Eligibility In 2022
by Christian Worstell | Published February 03, 2022 | Reviewed by John Krahnert
As of 2018, 12.2 million Americans are dual eligible beneficiaries of Medicare and Medicaid. This equals over 19% of the total Medicare population in that year.1
Medicare is the federally-administered health insurance program for people age 65 and over and people with qualifying disabilities.
Medicaid is a health insurance program for people with limited financial resources that is administered both by federal and state governments.
People who qualify for both Medicare and Medicaid benefits are dual eligible beneficiaries.
Recommended Reading: North Carolina Managed Medicaid Plans
Which Medicaid Benefits And Services Are Mandatory In All States
The Centers for Medicare & Medicaid Services oversees the Medicaid program. The agency is part of the U.S. Department of Health and Human Services . CMS monitors state programs to ensure compliance with federal laws.
Each state is responsible for establishing and managing their own Medicaid program. States will determine the following based on federal guidelines:
-
Scope of services
-
Duration of services
-
Service limits
Although states establish their own program, federal law still requires certain mandatory benefits for Medicaid beneficiaries. Below are 18 mandatory services that are required no matter which state you live in:
-
Certified pediatric services
-
State Plan home & community-based services 1915
-
Tuberculosis services for the care of TB infection or disease
Additional services and benefits that may be provided depending on your state include:
-
Approved services in a religious nonmedical healthcare institution
-
Approved services in an emergency hospital services by a non-Medicare-certified hospital
-
Approved services in a critical access hospital
Medicaid programs also cover mental health and substance use disorder services. The type of services covered will depend on your state.
