How Do I Qualify For Weight Loss Surgery
The general medical guidelines for weight-loss surgery are based on body mass index .The surgery may also be an option for an adult who meets these three conditions:
- BMI of 35 or higher.
- At least one obesity-related medical condition.
- At least six months of supervised weight-loss attempts.
16.12.2020
Lets Take A Closer Look At The Different Types Of Bariatric Surgery
Some of the common types of Medicare bariatric surgeries include gastric bypass, lap band surgery and gastric sleeve surgery.
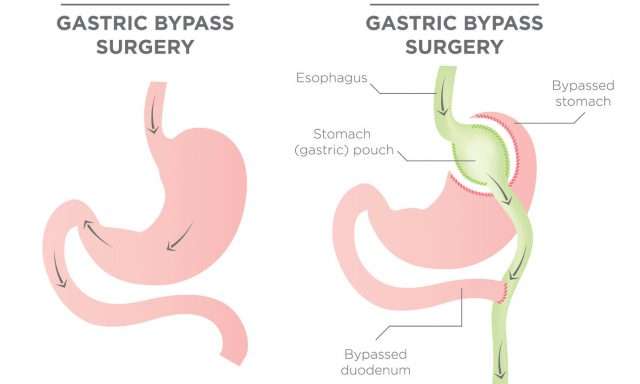
Gastric bypass surgery
This common malabsorptive weight loss surgery is also known as Roux-en-Y gastric bypass . In this procedure, a small stomach pouch is created to restrict food intake. The rest of the stomach is bypassed via a Y-shaped segment of the small intestine, which reduces the amount of calories and nutrients the body absorbs.
LAP-BAND® surgery
This surgery is defined as Laparoscopic adjustable gastric banding . This common weight loss procedure involves the placement of a hollow band around the upper end of the stomach, creating a small pouch and a narrow passage into the larger remainder of the stomach. The band is inflated with saline solution, which can be increased or decreased over time to alter the size of the passage.
Gastric sleeve surgery
This weight loss surgery is also commonly known as vertical sleeve gastrectomy or sleeve gastrectomy . This procedure involves the removal of the greater curvature of the stomach and approximately 80% of the stomach volume. While pyloric sphincter and stomach functions are preserved, the remaining stomach resembles a slender curved tube.
Weight Gain After Gastric Bypass
After getting a Roux-en-Y in Maryland, you should experience weight loss that will speed up, slow down, and plateau at various times until you reach your ideal weightassuming you are maintaining a proper diet and exercise routine. However, the occasional patient will only experience initial weight loss, then begin gaining again. An even smaller percentage never lose weight at all.
When a patient gains weight after gastric bypass surgery, it is important that their doctor ascertains the reason this is occurring. This will not only determine what the next steps are, but also might impact whether or not Medicare will pay for gastric bypass revision.
Also Check: Dentist In Louisiana That Accept Medicaid For Adults
Important Things To Know
For Medicaid to cover your weight loss surgery, you must have your procedure at a Center for Excellence . These facilities have a level of excellence that makes them successful at performing these procedures. If you have any specific questions about your Medicaid coverage and whether or not weight loss surgery is an option for you, contact them directly. Yes, your surgeon is an excellent source of information, but you are responsible for making sure there is no surprises post-op regarding out of pocket costs and overall coverage.
- Editor
Also Check: Can I Get A Breast Pump Through Medicaid
Experimental And Investigational Bariatric Surgical Procedures

Aetna considers each of the following procedures experimental and investigational because the peer-reviewed medical literature shows them to be either unsafe or inadequately studied:
You May Like: How To Pay For Medicare Without Social Security
You May Like: Who Qualifies For Qmb Medicaid
Is Obesity A Disease
Ding ding ding! Just like type 1 diabetes or multiple sclerosis, obesity is a diseaseand a difficult-to-control one, at that.
When the American Medical Association officially recognized this in 2013, it was an important step forward educating millions of people, including health care providers, that obesity is not a personal choice or a character flaw. Its a stubborn, difficult-to-treat condition with far-reaching health implications.
The Obesity Medicine Association put this succinctly: For most people suffering with obesity, simply eating less and moving more will not result in sustainable long-term weight loss.
Also Check: How To Obtain A Medicaid Provider Number
Reasons To Be Denied Weight Loss Surgery
Although weight loss surgery is a highly safe procedure with exceptionally good success rates, a conscientious bariatric surgeon will only accept you as a candidate if they believe that the benefits significantly outweigh the risks. The surgeons foremost priority will be your safety, and you could be denied this procedure if the surgeon is convinced that you are not eligible for it. Heres why some patients may fail to qualify for this surgery:
- Your BMI is low enough to be corrected with diet and exercise.
- You are under 18 years of age and your physiology is still developing.
- You have been diagnosed with a certain health condition that could pose threat to your safety during or after the surgery.
- You have been a regular smoker and are unwilling or unable to quit the habit for at least a few weeks before and after the surgery.
- You are taking blood thinners, NSAIDs, or other medications that increase your risk of surgery, and your physician cannot take you off them temporarily.
- You are not willing to commit to a pre- and post-operative weight loss surgery diet plan as recommended by your surgeon.
Don’t Miss: Apply For Medicaid Insurance Online
Do Medicare Advantage Plans Cover Weight Loss Surgery
Medicare Advantage plans must cover at least as good as Medicare, but they can have more extensive pre-requisites for coverage. You can expect a Medicare Advantage plan to cover weight loss programs that are medically necessary, including surgery.
Advantage plans may require you to stay in the plan network, obtain referrals, and adhere to very specific guidelines. Before you enroll in this type of plan be sure its in your best interest long term.
Contraindications To Obesity Surgery
Surgery for severe obesity is a major surgical intervention with a risk of significant early and late morbidity and of perioperative mortality . Contraindications for these surgical procedures include peri-operative risk of cardiac complications, poor myocardial reserve, significant chronic obstructive airways disease or respiratory dysfunction, non-compliance of medical treatment, psychological disorders of a significant degree that a psychologist/psychiatrist would have thought would be exacerbated or interfere with the long-term management of the patient after the operation, significant eating disorders, or severe hiatal hernia/gastroesophageal reflux.
A Multidisciplinary Care Task Group identified contraindications to weight loss surgery, including unstable or severe coronary artery disease, severe pulmonary disease, portal hypertension with gastric or intestinal varices, and/or other conditions thought to seriously compromise anesthesia or wound healing. The Task Group also noted that weight loss surgery is contraindicated in those who are unable to comprehend basic principles of weight loss surgery or follow operative instructions. The Task Group stated that any combination of the following factors revisional surgery, male, greater than 50 years of age, BMI greater than 50 kg/m2, and obstructive sleep apnea, hypertension, and type 2 diabetes indicates high risk.
Don’t Miss: Dentist In Ashland Ky That Take Medicaid
Not All Policies Are The Same
The first thing to understand is that every insurance policy is different. You might have health insurance that covers weight loss surgery, at least in part, and you might not.
Since the passing of the Affordable Care Act, all medical insurance policies sold on the Marketplace must offer obesity coverage. However, the ACA does not outline what this means. Insurance policies can decide that obesity coverage is strictly nutritional guidance or therapy sessions. Others might include certain medications. And others still can extend this coverage to bariatric surgeries.
With that said, most companies offer at least partial coverage of gastric bypass, gastric sleeve, and lap band surgeries. If you are wondering, does Medicaid cover weight loss surgery? The answer is yes. However, there are limits for it and private policies.
Other Things To Consider
To be covered by Medicaid for your surgery, you must have your weight loss surgery procedure performed at a Center for Excellence . These facilities have a level of excellence established that make them successful at administering these life-changing procedures. Medicaid requires that you use one of these centers to guarantee the best treatment.
If you have any questions regarding your Medicaid coverage and whether or not your coverage covers weight loss surgery, contact Medicaid directly. While your surgeon should be a source of information for you and who is responsible for the overall approval, its essential that you take the time necessary to ensure your surgery is covered so that there is no surprises post-op.
- Bariatric Journal Editor
Also Check: Medicaid Exclusion List By State
Does Medicare Cover Gastric Sleeve Surgery
Medicare does cover gastric sleeve surgery when available in your service area. The level of coverage also depends on whether youre getting care as an inpatient or outpatient. Gastric sleeve surgery removes and separates about 85% of the stomach, and then the remaining gets molded into a tubular shape that cant contain much food or liquid.
Patients lose an average of 65% of extra weight after gastric sleeve surgery, which may be why it was the fastest-growing bariatric surgery in 2019.
You May Like: What Income Is Used To Calculate Medicare Premiums
Medicaid And Epsdt Program Analysis
We reviewed current evidence-based guidelines for adult and pediatric obesity assessment and treatment. We selected the following interventions for analysis of Medicaid coverage and payment practices for adults with obesity: nutritional assessment/counseling, drug therapy, and bariatric surgery. For children, based on current guidelines, we focused our search on coverage and reimbursement of nutrition and behavioral therapies.
Based on current treatment recommendations, specific national medical service billing Current Procedural Terminology codes for obesity assessment and treatment were selected . These codes would most likely be used in billing for the nutritional, behavioral, and surgical therapies that comprise the bulk of treatment approaches for obesity.,
You May Like: How To Apply For Medicaid In Houston
Learning The Basics Of Bariatric Surgery
Bariatric surgery, commonly known as weight loss surgery, alters persons digestive process within the gastrointestinal tract to assist the person in losing weight. There are 2 types of bariatric surgical techniques: restrictive and malabsorptive. These 2 techniques can also be combined to form a third technique. Most procedures are performed using a laparoscopic or open approach.
- Restrictive procedures: Reduce the stomach size thus decreasing the amount of food the stomach can hold
- Malabsorptive procedures: Limit the amount of nutrients and calories that the body can absorb
Does Medicaid Cover Gastric Sleeve
Does Medicaid Cover Gastric Sleeve
Does Medicaid Cover Gastric Sleeve Lets take a look at does Medicaid cover gastric sleeve. First of all, we need to look at what this Medicaid is. Next, lets examine what it covers and what it doesnt. People dont want to be obese, but they do. These surgeries have very high costs. People need extra help.
Don’t Miss: Does Medicaid Give You A Free Breast Pump
Will Medicare Pay For Gastric Bypass Revision Surgery
I know that medicare will pay for gastric bypass but does it also cover the surgery to have it reversed.
|
Answer by Rubberchicken Medicare will likely not pay for gastric bypass surgery unless a second opinion from a doctor shows that the surgery is needed for assistance in other concurrent health issues, such as diabetes. In the vast majority of obesity cases, Medicare will look for other obesity management alternatives. |
|
Answer by Roland27 That is something that youre going to need to call Medicare and talk to them about. It varies state by state what they cover so its always best to ask BEFORE you get the procedure done to avoid finding out later that for some reason you wont be covered and you have to pay the bill yourself. |
S To Getting Approved For Gastric Sleeve
Steps to getting approved for gastric sleeve surgery are important to know as you learn about the process. Your surgeon will evaluate your medical history and current physical state to determine eligibility.
- Several factors will be used for your approval, including your commitment to following instructions.Confirm your BMI. Some patients may fear their BMI is not high enough for surgery. Those with a lower BMI can still be cleared on a case-by-case basis.
- Contact your insurance to ask about additional information. Many times they require a psychological evaluation. Even if you may have medical or financial barriers to surgery, a surgeon may work with you to determine the most effective, safest way for you to have a gastric sleeve using a more personalized approach.
- Experienced medical tourism representatives can arrange a free consultation for you with a weight loss surgeon. Youll experience a comprehensive program that can provide you with long-lasting results. However, if gastric sleeve was determined not right for you, other surgery options may still be available, such as a Gastric Bypass or a Gastric Lap Band surgery.
When youre in need of surgery and others say No!, remember Jet Medical Tourism® for all your bariatric needs!
Also Check: Unitedhealthcare Louisiana Medicaid Phone Number
Prophylactic Mesh Placement For Prevention Of Incisional Hernia After Open Bariatric Surgery
In a systematic review and meta-analysis, Dasari and colleagues examined if mesh prevents post-operative incisional hernia in open and laparoscopic bariatric surgery patients. A total of 7 studies met inclusion criteria. These investigators abstracted data regarding post-operative IH development, surgical site infection, and seroma or wound leakage and performed a meta-analysis. The prophylactic mesh group had significantly decreased odds of developing IH than the standard closure group . No included studies evaluated outcomes after prophylactic mesh during laparoscopic bariatric surgery. The authors concluded that prophylactic mesh during open bariatric surgery appeared to be beneficial in reducing post-operative IH without significant increasing the odds of surgical site infection or seroma or wound leakage. Moreover, they stated that higher quality studies, including those in laparoscopic patients, and cost-utility analysis, are needed to support routine use of this intervention.
Recommended Reading: Who Is Not Eligible For Medicaid
Does Bariatric Surgery Shorten Your Life
The study found that while life expectancy improved in most diabetic obese patients who underwent bariatric surgery, it might actually reduce life expectancy in super super obese patients, which is a category of obesity that applies to people with a BMI over 60, for example a person who is 5 feet 8 inches tall and
Don’t Miss: What Is Medicaid In Wisconsin
Who Is Not Eligible For Bariatric Surgery
An extensive pre-surgery screening process is required in most cases, which would involve a consultation with a team of professionals, including a doctor, dietician, psychologist, and surgeon, according to Mayo Clinic.
These experts will look further into your weight history, diet attempts, eating habits, exercise, stress, and other factors. They will also evaluate your health history, such as blood clots, heart problems, kidney stones, or nutritional deficiencies. Any of these may deem a person ineligible for bariatric surgery
Other factors include your mental health conditions, or whether or not you have a history of a binge-eating disorder, substance abuse, anxiety, major depression, schizophrenia, severe bipolar disorder, or issues related to childhood sexual abuse.
Even if you are approved for bariatric surgery, it could potentially be delayed or canceled if your team of doctors finds:
- You are not psychologically or medically ready for surgery
- You have not made appropriate diet or exercise changes
- You have gained weight during the evaluation
Bariatric Surgical Management Of Morbid Obesity

L35022
Fee schedules, relative value units, conversion factors and/or related components are not assigned by the AMA, are not part of CPT, and the AMA is notrecommending their use. The AMA does not directly or indirectly practice medicine or dispense medical services.The AMA assumes no liability for data contained or not contained herein.
Recommended Reading: Dentists In Grand Island Ne That Accept Medicaid
How To Get Medicaid Approval For Weight Loss Surgery
If the Medicaid provided by your state covers bariatric surgery, you must consult your physician. Medicaid accepts coverage when there is a medical need for the surgery. It is vital to have a physician who can share relevant information for the medical necessity of bariatric surgery for the patient. Further, to assess the situation, a physician can recommend the patient to approved surgeons.
Approved surgeons help you understand the surgerys basics and different options you may have. After you make a decision, you need to go through some tests and then consult the Medicaid office for pre-approval of the surgery. The process is time-consuming and requires patience as well as perseverance.Before approval, you may have to attend classes to understand the surgery, nutritional requirements, lifestyle changes, and exercises, which are mandatory post the operation. This ensures that the patient understands all implications of the surgery and whats essential to make it successful.
With necessary provisions, you may get approval from Medicaid. These provisions can further include additional classes or further testing. After approval from Medicaid, your surgeon needs to determine your ability to undergo the procedure. This can include medical preparation, blood work, and X-rays. Finally, the surgery is booked. Hence, you get a step closer to a healthier lifestyle and your weight goals.
