Montana Health Department Plans More Frequent Audits For Medicaid Eligibility
Montanas health department is finalizing a proposal to increase how often it audits people enrolled in the states coverage program for low-income adults. Health care providers and advocacy groups say some will unnecessarily lose their health coverage.
State health officials told lawmakers Tuesday theyre aiming to comply with legislative intent by changing the eligibility policy within the states Medicaid expansion program, which provides health coverage to nearly 10% of Montanans.
Last spring, lawmakers passed a budget bill ending 12-month continuous eligibility for Medicaid recipients. Continuous eligibility aims to reduce the number of people churning through the health coverage program, allowing them to stay on for a full year, regardless of changes to their income.
Montana is one of only two states that allows Medicaid recipients to remain eligible for the program for an entire year.
Adam Meier is director of the Montana Department of Public Health and Human Services.
What were really doing here is changing back to the default of what Medicaid defines nationally as the standard for eligibility, Meier says.
If the states proposal is approved by the federal government, the health department will be able to audit recipients eligibility more frequently and end benefits for recipients more often.
Health officials are also applying to end continuous eligibility for a program that covers low-income residents with severe, disabling mental illness.
What You Need To Apply:
- The name, address, contact info, and birth date for everyone in your household
- Social security numbers and/or immigration documents
- Employer and income information for everyone in your household. Examples include pay stubs or W2 forms.
- Other income information including Social Security Administration or Supplemental Security Income payments and mentions
- Information about current health coverage for members of your household, including coverage through an employer, a spouse’s employer, or Medicare
What Is Montana Medicaid Number
Montana Medicaid number where you can call and speak to Montana state health care agent regarding Montana Medicaid Application is .
Montana Medicaid hours of operation regarding Montana Medicaid Application are Monday through Friday, from 9:00 am to 6:00pm, closed on State holidays, but the best calling hours for Montana Medicaid to call regarding Montana Medicaid Application are 9:00 am to 1:00 pm and 2:30pm to 4:00pm.
Recommended Reading: Moving To Another State Medicaid
Montana Homeowner/renter Credit Program
The Montana Elderly Homeowner/Renter Credit program is a property tax relief program that provides a refundable income tax credit of up to $1,000. Montana homeowners or renters age 62 or older may qualify for this program even if you do not have to file an income tax return if they meet the eligibility criteria.
Montana Department of Revenue1201 US Hwy 10 West, Unit D2Livingston, MT 59047
You May Like: Pediatric Dentist St Louis Medicaid
Learn About Requirements For Medicaid In Montana
Medicaid candidates who first learn how to qualify for Medicaid in Montana have a better chance of submitting a successful application. Medicaid benefits eligibility is extended to those who are part of a low-income household, as long as they meet all requirements. Currently, Montanas Medicaid provides some form of coverage for around 20 percent of residents in the state. Many of the Medicaid eligibility requirements are established by the federal government, but the state of Montana has some flexibility when it comes to determining eligibility for Medicaid applicants. The eligibility requirements for Medicaid can seem complex at first, but with some knowledge and understanding, a prospective petitioner can discover if he or she qualifies to receive Medicaid benefits. Anyone interested in qualifying for MT Medicaid should carefully review the information provided below.
Who qualifies for Medicaid in Montana?
What are the requirements for Medicaid in Montana?
Some basic requirements for Medicaid in Montana are established by the federal government. In order to be considered for Medicaid eligibility, a candidate must meet the following minimum requirements:
- Be a Montana state resident.
- Be a U.S. citizen or qualifying non-citizen .
- Meet income guidelines.
To qualify for Medicaid benefits in MT, candidates will need to show documentation that provides evidence of these qualifications. Examples of these documents include birth certificates, utility bills and tax returns.
You May Like: Spartanburg South Carolina Medicaid Office
Montana Living Life Well Program
The Montana Living Life Well Program provides healthy living incentives to Montana Medicaid members. Some of the benefits include:
- $200 yearly incentive for the Diabetes Prevention Program
- $200 yearly incentive for joining Weight Watchers
- $200 yearly incentive for joining the Healthy For Life Self-Study Program
- $250 for joining in the Allegiance Maternity Management Program in your first trimester
- Free breast pumps, supplies, and lactation consultation for eligible new mothers
Prizes for participants in the sprint Stay Active program, the Summer Challenge, and the Holiday Challenge.
Expansion Under The Affordable Care Act
The Affordable Care Act provided for the expansion of Medicaid to cover childless adults whose income is 138 percent of the federal poverty level or below. The provision for expanding Medicaid went into effect nationwide in 2014. As of November 2018, a total of 36 states and Washington, D.C., had expanded or voted to expand Medicaid.
Montana expanded Medicaid under the Affordable Care Act in 2016 via an alternative method that required enrollees to pay premiums and copayments. Montana GovernorSteve Bullock supported Medicaid expansion, having submitted a proposal for expansion called Healthy Montana Plan to the state legislature in January 2015.
On November 6, 2018, voters rejected Montana I-185, the Extend Medicaid Expansion and Increase Tobacco Taxes Initiative. Voters defeated an initiative to extend Montana’s Medicaid expansion and raise taxes on tobacco products. Medicaid expansion in the state expired on June 30, 2019.
Support
Arguing in support of the expansion of Medicaid eligibility, the Center for American Progress states that the expansion helps increase the number of people with health insurance and benefits states economically. The organization argues that by providing health insurance to those who would otherwise be uninsured, Medicaid expansion allows low-income families to spend more money on food and housing:
Opposition
Also Check: Can I Change Medicaid Plan
Walk With Ease Program And Other Chronic Disease Management Programs
The Arthritis Foundation hosts the WWE program for individuals with arthritis. Participants meet three times per week for six weeks, beginning with a pre-walk discussion about arthritis recovery and ending with a 10-40 minute walk. Additionally,through the Arthritis Foundation Exercise Program in Montana, trained instructors can help people with arthritis recover their range-of-motion and rebuild endurance as well as practice relaxation techniques and learn more about their diagnosis. Classes typically meet two or three times per week for eight weeks.
Members with arthritis and other chronic diseases can also participate in a wellness workshop called the wCDSMP . wCDSMP participants meet twice per week for six weeks to learn how to increase and improve communication and physical activity while decreasing fatigue levels. Participants learn how to get back into the workforce while working through their chronic illnesses.
The Enhance Fitness program helps older adults at all fitness levels become more active and energized. Trained instructors will walk you through strength, balance, and flexibility training for a full 16 weeks.
How Much Does Medicaid Cost
Medicaid recipients in Montana may need to pay a monthly premium, which is a monthly fee for enrollment in the program. Premium amounts are based on the recipients annual income and will total two percent of your yearly income billed monthly.
Recipients may sometimes need to pay a small out-of-pocket cost for treatments, which are known as copayments. Copayment amounts depend on the recipients age, household income and what the state pays for the specific service.
Each Medicaid participant through the Montana Department of Public Health and Human Services has their own individual health care plan. Some participants may be required to pay fees, and some recipients may not be required to pay fees, i.e., are exempt.
To learn more about Medicaid premiums and copayments, click here.
You May Like: Medicaid Albany Ny Phone Number
Read Also: Does Wv Medicaid Cover Dentures
How To Qualify For Medicaid
Almost every state has multiple Medicaid programs. But, as a good rule of thumb, if you make less than 100% to 200% of the federal poverty level and are pregnant, elderly, disabled, a parent/caretaker or a child, thereâs likely a program for you. And if you make less than 133% of the FPL**, thereâs possibly a program for you, depending on whether your state expanded Medicaid under Obamacare. In 2021, the federal poverty levels range from $12,880 to $44,660 .
In 2021, the federal poverty level in Alaska ranges from $ $16,090 to $55,850 . The federal poverty level in Hawaii ranges from $14,820 to $51,360 .
Medicaid Spending In Montana
This page covering Medicaid spending by state last received a comprehensive update in 2017. If you would like to help our coverage grow, consider donating to Ballotpedia. Please contact us with any updates.
This article does not contain the most recently published data on this subject. If you would like to help our coverage grow, consider donating to Ballotpedia.
| Medicaid spending in Montana |
Montana’sMedicaid program provides medical insurance to groups of low-income people and individuals with disabilities. Medicaid is a nationwide program jointly funded by the federal government and the states. Medicaid eligibility, benefits, and administration are managed by the states within federal guidelines. A program related to Medicaid is the Children’s Health Insurance Program , which covers low-income children above the poverty line and is sometimes operated in conjunction with a state’s Medicaid program. Medicaid is a separate program from Medicare, which provides health coverage for the elderly.
This page provides information about Medicaid in Montana, including eligibility limits, total spending and spending details, and CHIP. Each section provides a general overview before detailing the state-specific data.
HIGHLIGHTS
Recommended Reading: What Is The Income Limit For Maryland Medicaid
Medicaid Certified Home Care Agency In Montana
Agencies that are looking for Medicaid reimbursement in Montana should consider getting a certification as HHA . There are certain regulations that must be fulfilled by the caregiver agency to claim Medicaid. These agencies must have an adequate license along with some certifications, which makes them eligible for claims.
Governing Body: Department of Public Health and Human Services
Missed Or Canceled Appointments

When members do not show up for a scheduled appointment, it creates an unused appointment slot that could have been used for another member. It is very important to keep appointments and call the provider in advance if you cannot make it to a scheduled appointment. Medicaid providers cannot bill a member for no-show/missed appointments. However, a provider may discharge a member from their practice after so many no-show/missed appointments. The provider must have the same policy for Medicaid members as non-Medicaid members, and must notify Medicaid members that the policy exists.
For a full list of member rights and responsibilities, see the
Also Check: Anthem Medicaid Ky Dental Providers
View Or Download Our Free Guide
While we are not affiliated with the government in any way, our private company engaged writers to research the Medicaid program and compiled a guide and the following answers to frequently asked questions. Our goal is to help you get the benefits that you need by providing useful information on the process.
Our free Medicaid Guide is filled with helpful information about how to apply, program eligibility and how to get in touch with local offices. You can view or download our free guide here.
Instead Lawmakers Have Approved A 6
Since the ballot initiative failed, the issue of continued Medicaid expansion was in lawmakers hands during the 2019 legislative session, and a compromise had to be reached in order to extend Medicaid expansion past the end of June.
H.B.425 was introduced in February, and simply called for the existing Medicaid expansion program to be extended. That legislation didnt go anywhere, but H.B.658, which called for a six-year extension of Medicaid expansion along with a Medicaid work requirement, passed and was signed into law by Gov. Steve Bullock in May 2019. H.B.658 was introduced by Rep. Ed Buttrey, a Republican representing Great Falls who also sponsored the 2015 legislation that expanded Medicaid in Montana.
Recommended Reading: Does Medicaid Cover Cochlear Implants
Read Also: Give Me The Number To Medicaid
Children’s Health Insurance Program
The Children’s Health Insurance Program is a public healthcare program for low-income children who are ineligible for Medicaid. CHIP and Medicaid are related programs, and the former builds on Medicaid’s coverage of children. States may run CHIP as an extension of Medicaid, as a separate program, or as a combination of both. Like Medicaid, CHIP is financed by both the states and the federal government, and states retain general flexibility in the administration of its benefits.
CHIP is available specifically for children whose families make too much to qualify for Medicaid, meaning they must earn incomes above 138 percent of the federal poverty level, or $33,948 for a family of four in 2017. Upper income limits for eligibility for CHIP vary by state, from 175 percent of the federal poverty level in North Dakota to 405 percent of the FPL in New York. States have greater flexibility in designing their CHIP programs than with Medicaid. For instance, fewer benefits are required to be covered under CHIP. States can also charge a monthly premium and require cost sharing, such as copayments, for some services the total cost of premiums and cost sharing may be no more than 5 percent of a family’s annual income. As of January 2017, 14 states charged only premiums to CHIP enrollees, while nine states required only cost sharing. Sixteen states required both premiums and cost sharing. Eleven states did not require either premiums or cost sharing.
Dental And Vision Benefits Explained
Adults with Montana Medicaid will face a $1,125 cap each year for dental treatment but can have dental exams and cleanings every six months. Adults can get partial dentures every five years and full dentures every ten years. Members under the age of 20 can get dental exams and cleanings as often as medically necessary. Adult members will not have coverage for porcelain or ceramic crowns, noble metal crowns, brides, splints/mouth guards, implants, or orthodontics. Members will be responsible for no-show appointments.
Adults will have coverage for one eye exam and one pair of glasses every 24 months, and those under 20 will have coverage for one exam and one pair of glasses every 12 months. More coverage may be provided if it is absolutely medically necessary, like in the case of eye diseases. Eyeglasses are only covered when chosen through Classic Optical Laboratories, Inc.
Also Check: Vein Clinics That Take Medicaid
Montanas Medicaid Program Impacts That States Budget Economy And Health
Montanas Medicaid program provides Montanans with low-incomes access to health care benefits and services based on their medical needs and life circumstances. Its Healthy Montana Kids program is the largest provider of health care for children in the state. Medicaid more broadly serves as a safety net for Montanans who are blind and disabled, women who are pregnant or have breast or cervical cancer, families with dependent children, and other adults with low incomes.
- Medicaid provides coverage for one in four Montanans .
- Medicaid is jointly funded with the federal government, which reimbursed Montana for 75 cents of every dollar spent on member care in State Fiscal Year 2019.
- Medicaid expansion was central to reducing the rate of uninsured Montanans by half since 2008.
- Nearly two-thirds of Medicaid recipients live in rural Montana, and nearly 50,000 American Indians have coverage through Medicaid.
- Seniors and individuals with disabilities comprise only 15% of the Medicaid population but contribute to 40% of Medicaid expenditures.
- Medicaid-covered behavioral telehealth service visits increased by over 1,400% through August 2020, as Medicaid waived in-person service delivery requirements for many physical and behavioral health services during the pandemic.
Apply For Medicaid In Montana
Online at HealthCare.gov or at apply.mt.gov, or by phone at 1-800-318-2596.
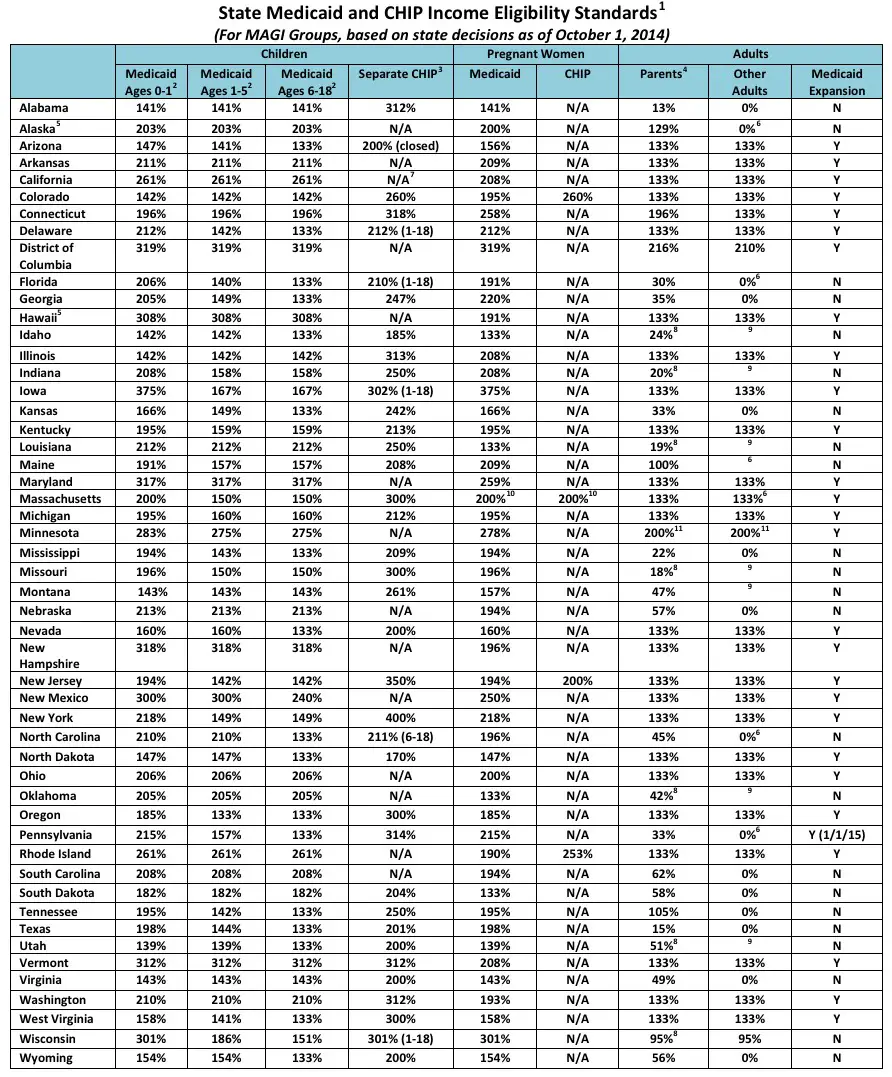
Eligibility: Children are eligible for Medicaid with household income up to 143% of the federal poverty level , and CHIP with household income up to 261% of FPL. Pregnant women are eligible for Medicaid with household income up to 157% of FPL. Other adults are eligible for Medicaid with household income up to 138% of FPL .
Don’t Miss: Michigan Pregnancy Medicaid Income Limits
State And Federal Spending
During fiscal year 2016, Medicaid spending nationwide amounted to nearly $553.5 billion. Spending per enrollee amounted to $7,067 in fiscal year 2013, the most recent year for which per-enrollee figures were available as of June 2017. Total Medicaid spending grew by 33 percent between fiscal years 2012 and 2016. The Medicaid program is jointly funded by the federal and state governments, and at least 50 percent of each state’s Medicaid funding is matched by the federal government, although the exact percentage varies by state. Medicaid is the largest source of federal funding that states receive. Changes in Medicaid enrollment and the cost of healthcare can impact state budgets. For instance, in Montana, the percentage of the state’s budget dedicated to Medicaid rose from 15.4 percent in 2010 to 17.4 percent in 2015. However, state cuts to Medicaid funding can also mean fewer federal dollars received by the state.
During fiscal year 2016, combined federal and state spending for Medicaid in Montana totaled about $1.4 billion. Spending on Montana’s Medicaid program increased by about 42.1 percent between fiscal years 2012 and 2016. Hover over the points on the line graph below to view Medicaid spending figures for Montana. Click on the red bar below the graph to view these figures as compared with three of Montana’s neighboring states.
