Although The Verification Process Varies Somewhat Cancer Treatment Centers Of America Generally Accepts Medicare
Cancer Treatment Centers of America does accept Medicare, but there are exceptions. There is some variety in which insurance plans each treatment center accepts. Most Cancer Treatment Centers of America facilities accept both Medicare and Medicare Advantage plans. Some also accept Medicaid.
Due to the variation involved, Cancer Treatment Centers of America advises potential patients to contact them for more information.
Medicare Advantage And Cancer
If you have Medicare Advantage , this means that youve purchased your Medicare plan from a private insurance company as opposed to getting it directly from the federal government. These types of plans are required to give you the same basic coverages as Original Medicare, but the CMS warns that they can have different rules and costs. Therefore, its important to go through your individual plan so you understand what it says regarding cancer coverage specifically. And if any portion of that policy is unclear, follow up with your policys administrator so you know what is covered and what isnt.
If any portion of that policy is unclear, follow up with your policys administrator so you know what is covered and what isnt.
Does Medicare Cover Wigs
Although Medicare has traditionally provided a number of medical treatment benefits related to cancer, it has consistently fallen short is with regard to the hair loss many cancer treatment patients experience. More specifically, it has never helped with the cost of purchasing a wig. However, some U.S. legislators are hoping to change that. On June 15, 2017, Rep. James P. McGovern introduced a bill that would amend title XVIII of the Social Security Act to include wigswhat the bill refers to as medically necessary cranial prosthesesas durable medical equipment under the Medicare program. If this bill passes, cancer patients with Medicare could get some or all of their wig-related expenses covered or reimbursed.
Read Also: Eye Doctors In Fort Worth That Accept Medicaid
If You Want Medicare To Cover Any Treatment The First Step Is Getting Approval From A Qualified Healthcare Provider
Understanding cancer care can be complicated for a few reasons. Cancer care tends to involve a wide variety of treatment forms, from surgery to medications, and these are all covered in different ways by Medicare. Here well focus on immunotherapy treatment, which can also vary according to several parameters. First, well discuss what immunotherapy is and who it can be used for, and then get into the details of how it is covered by Medicare.
Where Can You Find Cancer Treatment Centers Of America
Cancer Treatment Centers of America operate two types of centers: hospitals and outpatient care centers. These are located throughout the country. As mentioned above, CTCA can help you with transportation if necessary, to ensure that you can get to a location that serves your needs.
CTCA hospitals are in:
Outpatient care centers are in:
- Chicago, Illinois
- Scottsdale, Arizona
You May Like: How To Hide Money From Medicaid
Does Medicare Cover Cancer Treatment
Medicare covers a variety of cancer treatments. This includes chemotherapy and radiation therapy, which are both covered whether you are a hospital inpatient, or an outpatient receiving care at a clinic or doctors office. Medicare will usually pay for any other medically necessary service related to your cancer treatment.
There may be instances where your doctor suggests a treatment that isnt covered by Medicare. In this case, you should check with your doctor to see if Medicare will cover the treatment in question.
How Does The Insurance Verification Process Work
If you are interested in learning more about becoming a patient at CTCA, contact us to begin the insurance verification process. After we obtain your insurance policy information, we will conduct a preliminary check to determine how your insurance plan benefits might work and, if possible, schedule an appointmentall during the same phone call. If we need to investigate further, we will get back to you within 24 hours. Once your benefits have been confirmed, an Oncology Information Specialist will review the details of your insurance plans coverage and answer questions you may have.
You May Like: What Are The Qualifications For Medicaid In Colorado
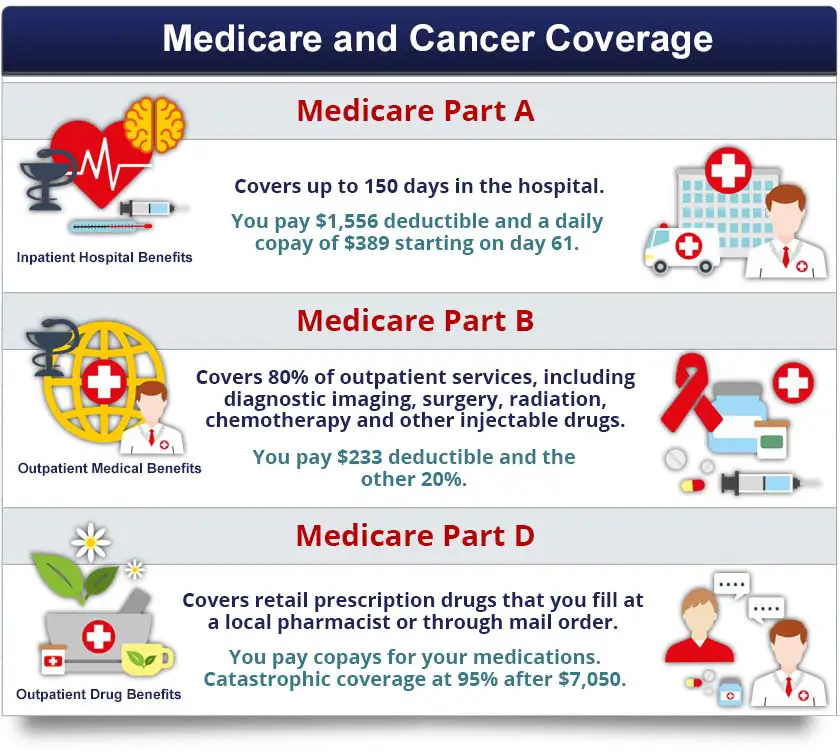
How Do The Parts Of Medicare Cover Cancer Treatment
The amount that Medicare will cover for cancer treatments can vary based on the type of cancer you have and the type of treatment plan prescribed by your doctor.
The type of policy you have can also play a role in your Medicare cancer coverage and how much youll have to pay out-of-pocket.
There are four parts of Medicare, referred to as Part A, Part B, Part C and Part D.
Does Medicare Cover Car T
The Trump administration has made the CAR T-Cell cancer therapy available to Medicare beneficiaries. This means access to innovative new cancer therapy. CMS is working closely to monitor patient outcomes from the treatment.
Trump and Secretary Azar finalized the decision to cover the FDA-approved Chimeric Antigen Receptor T-Cell or CAR T-Cell Therapy, which is a form of treatment for cancer that uses the patients own genetically-modified immune cells to fight cancer.
Get A Free Quote
Find the most affordable Medicare Plan in your area
This treatment is approved for people with certain types of non-Hodgkin lymphoma and B-cell precursor acute lymphoblastic leukemia.
Medicare covers CAR T-Cell therapy when its done in a healthcare facility enrolled in the FDA risk evaluation and mitigation strategies for FDA-approved indications.
Medicare also covers FDA-approved CAR T-cell therapy for off-label use when CMS-approves compendia.
The manufacture of the therapy will be conducting post-market observational studies. This is to monitor potential risks when considering whether to approve new CAR T-cell products.
Get A Free Quote
Find the most affordable Medicare Plan in your area
The FDA continues to work with CMS and the National Institute of Healths National Cancer Institute to help advance the availability of these new therapies to patients.
Get A Free Quote
Recommended Reading: Dentist In Tampa That Take Medicaid
Secondary Treatment Following Relapse
Hormone therapy may also be used as a secondary or salvage treatment when PSA levels rise following initial prostate cancer treatment, indicating the cancer has returned. This situation is known as biochemical recurrence. The salient points to keep in mind are that hormone therapy is most often used as a salvage treatment when PSA doubling time is less than six months, indicating that the cancer is aggressive or may have already metastasized.
Does Medicare Cover Car
The U.S. Centers for Medicare & Medicaid Services announced in 2019 that it would cover CAR-T cell immunotherapy in certain cases.
This type of immunotherapy is highly personalized, using your own T cells to find and kill cancer cells. Its also very expensive. As of 2019, a one-time treatment of CAR-T cell therapy was estimated to cost as much as $475,000, or up to $1.5 million if you include tests and hospitalization.
Medicare will only cover CAR-T cell therapy if you receive it in a hospital or other health care facility that is enrolled in the U.S. Food and Drug Administrations Risk Evaluation and Mitigation Strategies drug safety program.
The treatment also must meet other specific FDA requirements in order to be covered by Medicare Part B medical insurance.
Prepare for Medicare Open Enrollment
Recommended Reading: What Age Do You Get Medicaid
Neoadjuvant And Adjuvant Hormone Therapy For Early
Hormone therapy is sometimes given in conjunction with a definitive prostate cancer treatment, such as radiation therapy, in order to improve health outcomes. When hormone therapy is given in advance of a primary treatment, its known as neoadjuvant therapy when its given during or after a primary treatment, its known as adjuvant therapy.
Dont Miss: Does Medicare Cover The Cost Of A Shingles Shot
Cancer Screenings Covered By Medicare

Medicare covers several types of cancer screenings, as well as screenings for other diseases. This is part of the preventative coverage that Medicare provides. The following tests are covered by Medicare:
- Cervical and vaginal cancer
- Lung cancer
- Prostate cancer
Unless you are hospitalized, this coverage will be under Part B. You will have to pay for your prostate cancer exam depending on the type of exam, but you wont have to pay anything for the other tests if your doctor accepts Medicare assignment.
Don’t Miss: Does Medicaid Cover Gastric Bypass In Colorado
What Are Your Cancer Treatment Options
Cancer treatment is highly individualized. Several types of doctors work together to come up with a treatment plan that addresses your needs. A comprehensive cancer treatment plan will include one or more of the following types of treatments, all of which can be covered by Medicare.
- Surgery. Surgery may be recommended for removing cancerous tumors.
- Chemotherapy.Chemotherapy involves chemicals given orally or intravenously to kill cancer cells and stop cancer from spreading.
- Radiation.Radiation therapy uses intense beams of energy to kill cancer cells.
- Hormone therapy.Hormone therapy uses synthetic hormone and hormone blockers to target cancers that use hormones to grow.
- Immunotherapy.Immunotherapy drugs use your bodys immune system to attack cancer cells.
- Genetic therapy. These newer therapies typically deliver a virus to a cancer cell that will target and help destroy it.
One kind of cancer treatment that isnt covered by Medicare is alternative or holistic therapy. These treatments, which can include dietary changes, supplements, oils, and natural extracts, are not part of Medicares cancer coverage.
Appealing Medicares Decisions Regarding Cancer Coverage
You have the right to file an appeal in the event that Medicare does not reimburse a healthcare provider or service for something that you feel should be covered. That goes for whether youve already received the service or item, or if you believe that you should be eligible to receive it.
There are five levels to the appeals process that give you the opportunity to take your appeal all of the way to a judicial review by a federal district judge if you disagree with the decision made at any stage.
The exact process you will follow to go through this process depends on which type of Medicare plan you have. Also, if you need help with filing your appeal, you can either appoint a representative to help you or contact your State Health Insurance Assistance Program.
You May Like: Lift Chairs Covered By Medicaid
Medicare Covers A Variety Of Cancer Treatments As Well As Preventive Screenings Like Mammograms And Colonoscopies
The costs of receiving cancer treatment can add up fast, and the bills can be overwhelming. The good news is with Medicare, many of your expenses and needs are covered.
Original Medicare will cover many of the treatments you will need to help fight, and even cure, your cancer. Most treatments and surgery would be covered by either Part A or Part B . Prescription drugs or oral chemotherapy drugs you may need would be covered by Part D .
What Types Of Insurance Does Cancer Treatment Center Of America Accept
Cancer Treatment Center of America accepts a wide range of insurance policies including:
- Employer-sponsored group plans
Again, each Cancer Treatment Center of American location may have different policies regarding insurance acceptance, so its a good idea to ask prior to receiving any consultations or services.
The center will verify your insurance by obtaining your policy information and conducting a preliminary check to see how your benefits will work with their services. Once your coverage has been confirmed, you may schedule an appointment or ask any additional questions about how your insurance will work for your treatments.
If your insurance is not accepted at your preferred Cancer Treatment Center of America location, they will check to see if there are any other locations that will accept your coverage and will even assist with travel arrangements if necessary. Cancer Treatment Center of America hospitals are located in Atlanta, GA, Chicago, IL and Phoenix, AZ. Outpatient centers are located in Chicago along with the Arizona communities of North Phoenix, Scottsdale, Gilbert and Gurnee.
Your insurance company may also require an approval process on their end as well, and Cancer Treatment Center of America will attempt to complete that confirmation on your behalf.
Cancer Treatment Center of America will bill your insurance for you so there should be no need to file any claims yourself.
Don’t Miss: How To Get Breast Reduction Covered By Medicaid
Does Medicare Cover Arthritis
Different Medicare plan options Original Medicare, Medicare Advantage, Medicare Part D and Medigap can help cover different costs associated with different types of arthritis.
What each plan covers may be determined by the type of arthritis you have, the type of treatment you need and whether your treatment requires prescription medications.
How Medicare Plans Cover Arthritis
The Insurance Verification Process With Cancer Treatment Centers Of America
Cancer Treatment Centers of America provides detailed support during the health insurance verification process. The process begins with a consultation call during which they will check your insurance to determine whether it will cover their services. In some cases, they may need to contact you the next day with more information.
Once they have confirmed the details from your insurance company, CTCA will review your coverage with you. This will include answering questions about your out-of-pocket costs or anything else you may be wondering about.
Once your Medicare insurance is verified, you can schedule an appointment and begin discussing your treatment. If you have questions about your coverage and/or treatment options, this is a great time to ask.
If you want more information about which insurance plans a given CTCA location covers, call them toll-free at 866-954-0606.
Read Also: Psychiatrist In Richmond Va That Accept Medicaid
How Much Does Medicare Pay For Prostate Cancer Screenings
Medicare Part B generally pays 80 percent of the Medicare-approved amount for covered doctor services, such as a medically necessary prostate biopsy.
You typically pay the remaining 20 percent after you meet your Part B deductible. In 2022, the Part B deductible is $233 per year.
Medicare Part B also covers two other types of prostate cancer screenings:
- Digital rectal exams
- Prostate specific antigen blood tests
These preventive screenings are covered by Medicare Part B once every 12 months for men over the age of 50.
You typically pay 20 percent of the cost of your digital rectal exam after you meet your Part B deductible.
What To Do If You Have Medicare And Are Diagnosed With Cancer
If you have Medicare and are diagnosed with cancer, the ACS recommends thatprior to scheduling any type of doctors appointment or testyou first ensure that the healthcare providers youve chosen accept your Medicare insurance plan. If they dont, you may be required to pay some or all of their costs up front. Yes, Medicare may reimburse you for some of these expenses, but only the amounts dictated by your individual plan. So, if the provider charges more than Medicare is obligated by your policy to pay, you are responsible for the balance. The ACS also says that some doctors have completely opted out of Medicare, which means that if you decide to use them, Medicare wont pay any of the costs incurred. In this instance, you would have to pay for everything. Medicare offers many benefits related to cancer, but there are also some it doesnt. Thats why its critical to familiarize yourself with your specific plan. And if you have questions, ask. In the meantime, Medicare.gov has provided the forms and resources necessary to help you understand what your Medicare policy can do for you.
AgingInPlace.org keeps our resources free by working as an affiliate partnerwith some companies mentioned on our site. We may earn a commission when you click on certain product links.
You May Like: What Doctors Take Florida Medicaid
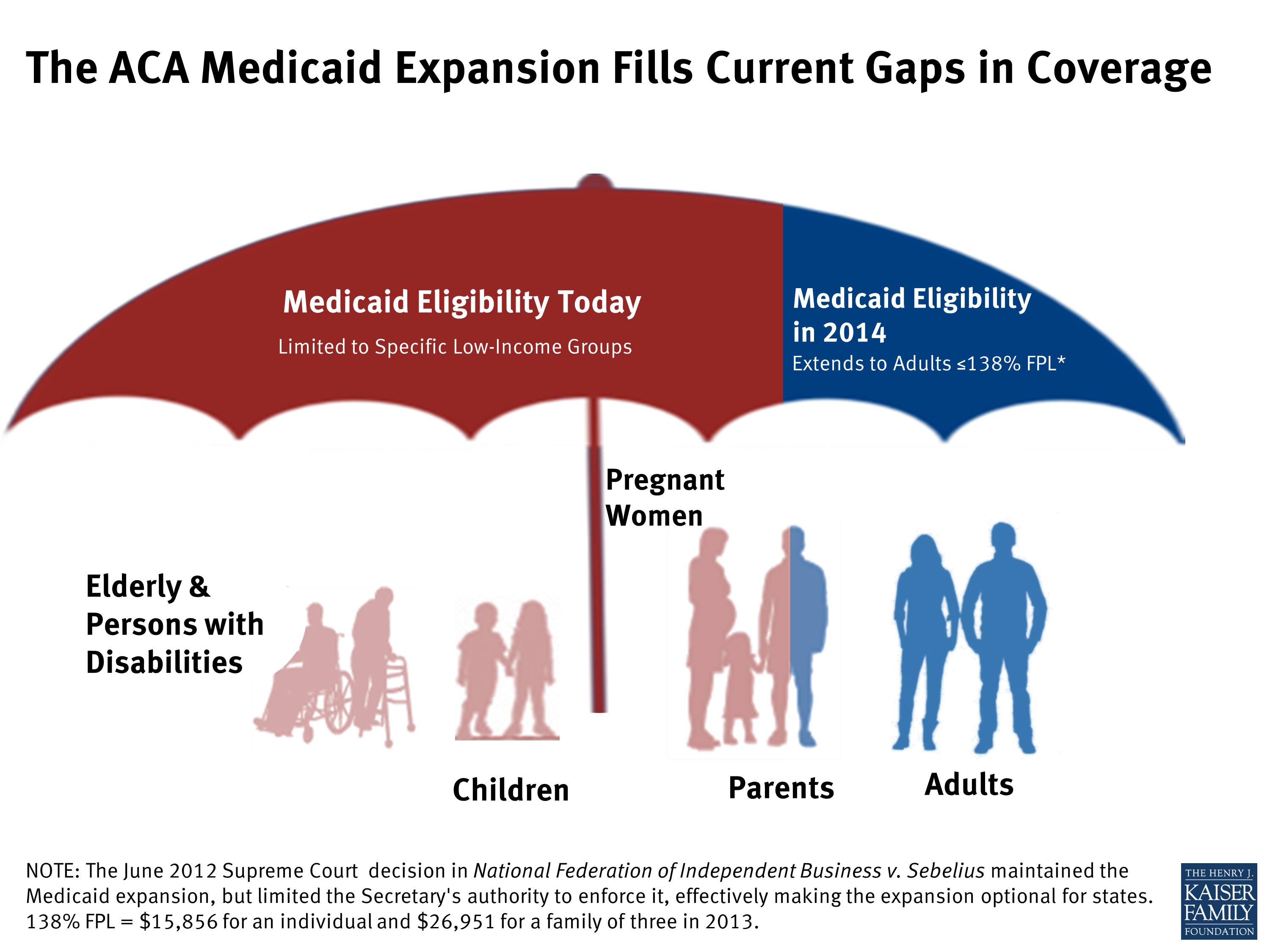
Policies That Impede Access To Medicaid
Certain Medicaid policies under discussion or being implemented in states under federal research and demonstration waivers potentially threaten access to Medicaid for all enrollees. But because of the ongoing need for uninterrupted access to medical care for people with cancer or survivors, such policies are particularly concerning.
Options In Hormone Therapy
Testosterone levels in the body can be reduced either surgically or with drugs. The surgical option is castration, achieved by removing the testicles during a bilateral orchiectomy. Once the only option, it has since been supplanted by drugs that lower testosterone levels to amounts achieved by surgery.
For men, normal testosterone levels range from 300 to 1,000 ng/dl. The FDA requires that any new drug used in hormone therapy for prostate cancer lower testosterone levels to 50 ng/dl or less. In my practice, I usually try to lower levels even further, to 20 ng/dl.
You May Like: Blue Cross Blue Shield Medicaid Indiana
Who Is Immunotherapy For
Immunotherapy can be used for a wide array of cancers, from lung cancer to lymphoma. The only thing that will determine whether or not some form of immunotherapy is right for you is whether or not your doctor thinks that it is appropriate. It is not limited to one type of cancer, but rather to specific scenarios in which it is deemed to be the most fruitful treatment option.
Medicare Part A And Cancer Coverage
Medicare Part A covers inpatient care. Although this usually refers to hospitals, you can also be an inpatient at other locations, such as skilled nursing facilities or hospices. Part A will cover 80 percent of all medically necessary inpatient treatments, once youve met your deductible.
Because virtually all cancer care is medically necessary, you can expect to have any cancer care that you need to be covered by Part A. This includes most surgeries, which will be performed while you are an inpatient. Part A has specific limitations on how many days are covered per benefit period, so lets take a look at these in more detail.
Also Check: Can You Receive Both Medicare And Medicaid
