Who Is Eligible For Medicaid
You may qualify for free or low-cost care through Medicaid based on income and family size.
In all states, Medicaid provides health coverage for some low-income people, families and children, pregnant women, the elderly, and people with disabilities. In some states the program covers all low-income adults below a certain income level.
- First, find out if your state is expanding Medicaid and learn what that means for you.
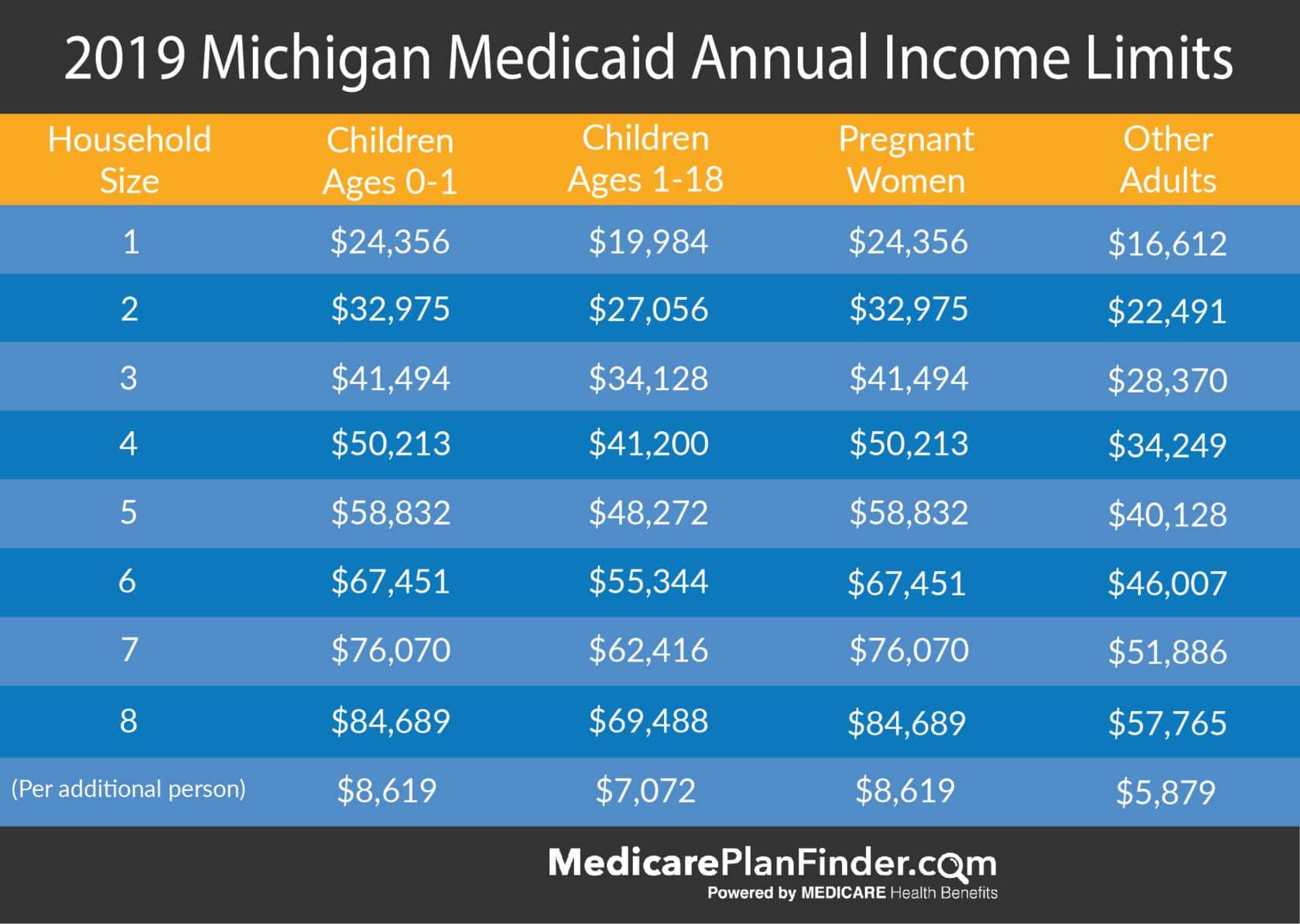
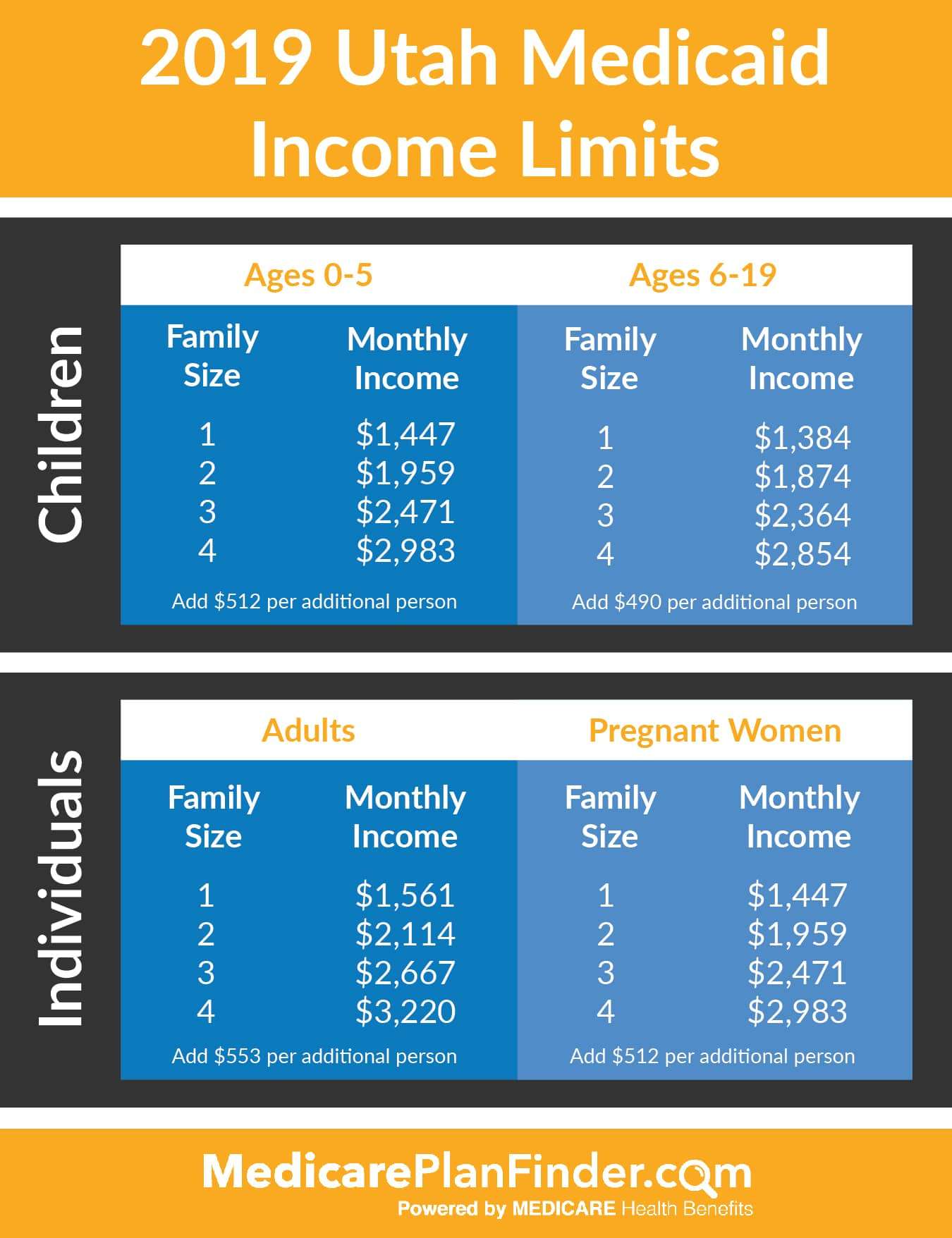
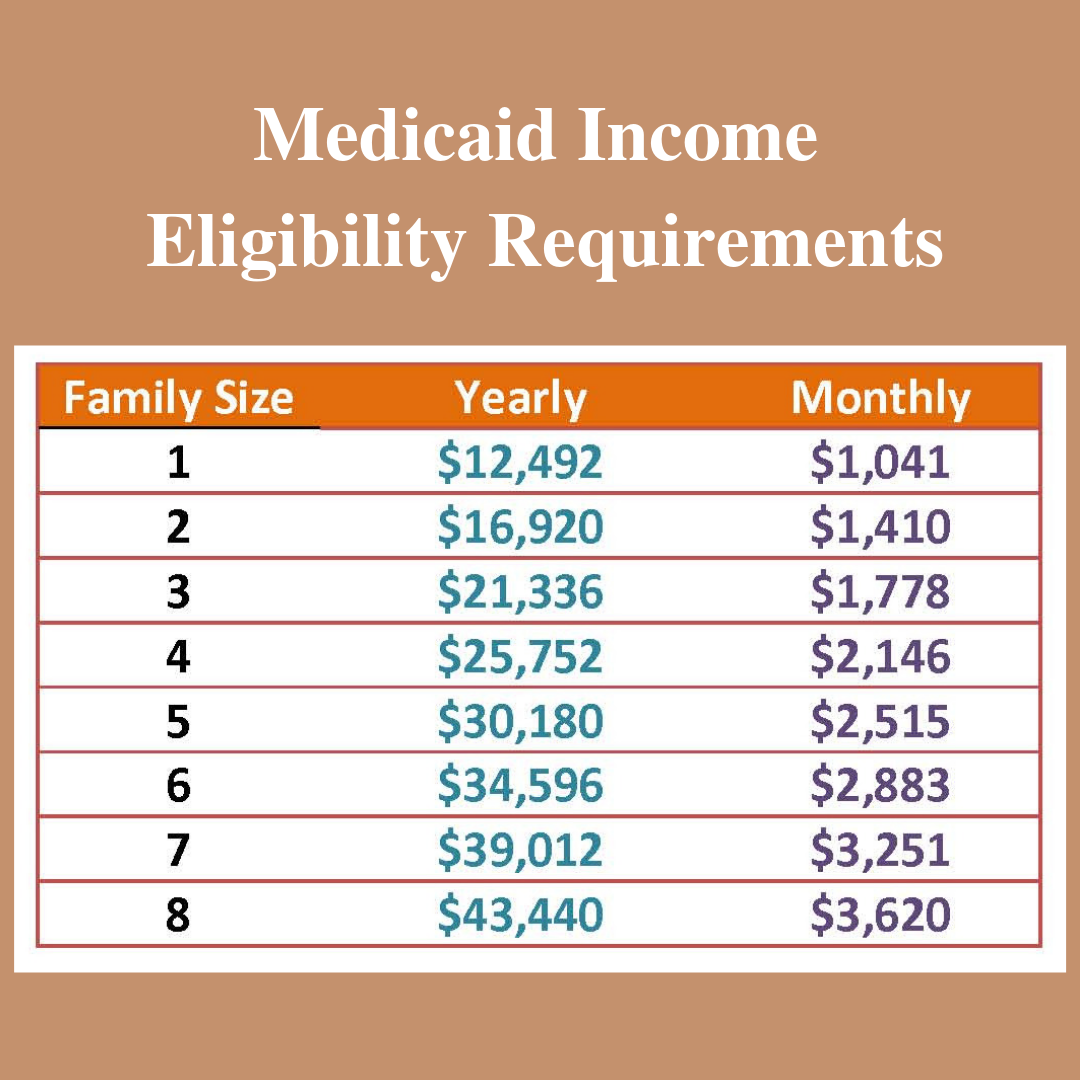
- If your state is expanding Medicaid, use this chart to see what you may qualify for based on your income and family size.
Even if you were told you didn’t qualify for Medicaid in the past, you may qualify under the new rules. You can see if you qualify for Medicaid 2 ways:
- Visit your state’s Medicaid website. Use the drop-down menu at the top of this page to pick your state. You can apply right now and find out if you qualify. If you qualify, coverage can begin immediately.
- Fill out an application in the Health Insurance Marketplace. When you finish the application, we’ll tell you which programs you and your family qualify for. If it looks like anyone is eligible for Medicaid and/or CHIP, we’ll let the state agency know so you can enroll.
Reduced Coverage / Medicare Cost Sharing Or Premium Payment
Qualified Medicare BeneficiariesCovered group: individuals covered by MedicareIncome limits: Income cannot exceed 100% of the federal poverty level. For more information, view the Guidelines for Medicare Cost-Sharing Programs brochure.Age: Medicare beneficiaries of any ageQualifications: Individuals must be eligible for Medicare Part A hospital insurance.
Specified Low-Income Medicare BeneficiariesCovered group: individuals covered by MedicareIncome limits: Income cannot exceed 135% of the federal poverty level. For more information, view the Guidelines for Medicare Cost-Sharing Programs brochure.Age: Medicare beneficiaries of any ageQualifications: Individuals must have Medicare Part A
Qualified IndividualsCovered group: individuals covered by MedicareIncome limits: Income cannot exceed 135% of the federal poverty level. For more information, view the Guidelines for Medicare Cost-Sharing Programs brochure.Age: Medicare beneficiaries of any ageQualifications: Individuals must have Medicare Part A
Managed Care And Third Party Liability
The contract language between the State Medicaid agency and the Managed Care Organization dictates the terms and conditions under which the MCO assumes TPL responsibility. Generally, TPL administration and performance activities that are the responsibility of the MCO will be set by the state and should be accompanied by state oversight.
There are four basic approaches to carrying out TPL functions in a managed care environment.
You May Like: Medicaid Estate Recovery Program Texas
What Do I Need To Apply
The necessary documentation needed to apply for Medicaid also depends on your category, specifically whether you fall under the Modified Adjusted Gross Income or non-MAGI guidelines. These guidelines are defined in the section below.
MAGI eligibility groups include:
- Pregnant women
- Infants and children under 19 years of age
- Childless adults who are not pregnant, 19-64 years of age, not on Medicare, and could be certified disabled but not on Medicare
- Parents/caretaker relatives
- Family Planning Benefit Program and/or
- Children in foster care
Non – MAGI Eligibility Groups include:
- Individuals 65 years of age or older, who are not a parent or caretaker relative,
- individuals who are blind or disabled who do not meet the criteria of any of the MAGI eligibility groups
- Residents of Adult Home run by LDSS, OMH Residential Care Centers/Community Residences
- Individuals eligible for the following programs:
- COBRA
- AIDS Health Insurance Program
- Medicaid Buy-in Program for Working People with Disabilities
- Medicaid Cancer Treatment Program
Application for Non-MAGI
The following paper application may only be printed and completed if you are applying at an LDSS for Medicaid because you are over 65 years of age or an individual in your household is deemed certified blind or disabled, or you are applying for Medicaid with a spenddown.
English, Spanish, Chinese, Haitian Creole, Italian, Korean, Russian
Helpful Ny Medicaid Resources
Applying for Medicaid can be a complex process depending on your medical conditions, resources, income, age, and more.
The good news is that there are plenty of helpful resources available to answer any questions you may have, and to provide you guidance.
Here are some helpful links.
NYC Human Resources Administration – They can help with the application process. You can call them at 557-1399.
You May Like: Medicaid And Medicare Differ In That
Option 2 Download Application
You can an application, complete it, and mail it to your county DHS office or submit it in person.
There are two ways to send in your paper application. You only need to choose one:
Mail it to:P.O. Box 305240Nashville, TN 37202-5240
Or Fax it to: 1-855-315-0669. Be sure to keep the page that says your fax went through.
Additionally, you call 855-259-0701 to apply over the phone.
What Does Medicaid Cover In Massachusetts
The Massachusetts Medicaid program covers various services. Children and adults alike can receive annual well-check exams. Emergency room or urgent care visits are also allowed, as well as emergency dental services, such as cracking a tooth or experiencing terrible pain. People can look into their specific plan details to see a full list of services covered by their insurance.
You May Like: Dentist Who Accept Medicaid Medicare
Eligibility Requirements For Medicaid In Ny
Since Medicaid is designed for low-income individuals and families, there are specific income and asset requirements that you must meet, depending on various factors, as we will discuss below.
To be eligible for Medicaid in NY, you must also meet the following eligibility criteria.
- You must be a U.S. national, citizen, permanent resident, or legal alien.
- You must be a resident of New York.
- You must need help with medical care/insurance coverage.
- Your financial situation must fall within the low-income category .
In addition to these requirements, you must also be one of the following:
- Pregnant
- 65 years of age or older
Can I Qualify Even If My State Does Not Have Expanded Medicaid
In states that have not expanded Medicaid, eligibility levels are lower than in states that have expanded. Even if your state hasn’t expanded Medicaid and it looks like your income is below the level to qualify for financial help with a Marketplace plan, you should fill out a Marketplace application.
Also Check: Can Medicaid Be Transferred To Another State
State Medicaid Programs And Use Of Contractors For Data Matching
State Medicaid programs may enter into data matching agreements directly with third parties or may obtain the services of a contractor to complete the required matches. When the state Medicaid program chooses to use a contractor to complete data matches, the program delegates its authority to obtain information from third parties to the contractor.
Third parties should treat a request from the contractor as a request from the state Medicaid agency. Third parties may request verification from the State Medicaid agency that the contractor is working on behalf of the agency and the scope of the delegated work.
How To Apply For Medicaid
- Medicaid can be applied for directly or through your state’s online exchange. Find out what the requirements are to apply and who to contact for help.
Medicaid is the joint federal and state health insurance program for people with qualifying income and assets. Seniors with limited or low income can apply for Medicaid on its own to help pay for basic medical care or as a supplement that helps cover the extra costs Medicare leaves uncovered.
Each state administers its own Medicaid program, so terms and requirements for participation vary somewhat depending on location. As always, it’s helpful to consult with a certified senior planner or benefits consultant before adding the Medicaid program to your comprehensive health coverage.
Also Check: Medicaid Assistance For Nursing Home Care
Gather The Information And Documents You Need To Apply
Before applying for Medicaid, you should have the following information ready for each person who is applying:
Even when your income qualifies for Medicaid, your state will still ask you to provide certain documents when you submit your application.
Due to COVID-19 precautions, an in-person application may not be possible, so please have these documents handy when you apply online.
- Social Security number
- Date of birth
- And how to download a paper application in pdf form.
Scroll down below to find your state and follow the instructions for submitting your application.
Your states Medicaid office has 45 days to process your application.
However, disability applications can take up to 90 days to be processed.
Additionally, if your Medicaid application isnt approved, you have the right to appeal the decision.
Scroll down below to find your state and pick the option that best suits you to apply for Medicaid.
Get Important News & Updates
Sign up for email and/or text notices of Medicaid and other FSSA news, reminders, and other important information. When registering your email, check the category on the drop-down list to receive notices of Medicaid updates check other areas of interest on the drop-down list to receive notices for other types of FSSA updates.
You May Like: Does Medicaid Pay For Partials
Complete And Submit Your Application For Nursing Home Medicaid
There are several types of Medicaid programs in every state, so find your local Medicaid office at this link, and be sure you get the correct information and application for the specific eligibility group you want to apply underin this case Nursing Home Medicaid or institutional Medicaid.
Most states allow you to submit your application for benefits in multiple ways: in person, by mail, or online. The online application is likely to result in a faster determination, approved or denied, than submitting physical documents in person or through the traditional mail.
Massachusettss Requirements For Medicaid Qualification
Enrollees must meet the requirements set forth by the state. Using the MassHealth website, applicants can discover if they would qualify or if they should skip the process. A summary of eligibility requirements is listed on the site, including being a resident of Massachusetts, having citizenship of the United States, and meeting income requirements. Children under age 19 and women who are pregnant may qualify more easily.
Also Check: Dentists In Logan Utah That Accept Medicaid
State Expanded Medicaid Eligibility
As of August 2021, 38 states had expanded Medicaid to cover all low-income adults whose household incomes are below a specified threshold. If your state has expanded Medicaid, you are eligible for coverage based on your income alone. Typically, your household income shouldnt exceed 138% of the federal poverty level.
In Idaho, for instance, the monthly income limits for expanded Medicaid range from $1,482 for one member to $5,136 for a household with eight members. The income limit is $523 for each additional member beyond eight. Check this page to understand your states Medicaid profile.
You should still fill out a marketplace application if your state hasnt expanded Medicaid and your income level doesnt qualify you for financial assistance with a . States have other coverage options if youre pregnant, have children, or live with a disability.
Awaiting Approval For Nursing Home Medicaid
How long does it take after applying to receive a Medicaid determination letter? The law requires an application for Medicaid to be approved or denied within 90 days. However, there is not really a mechanism to enforce this, and its possible your state Medicaid office will take longer than those 90 days to process your application and give you an answer. The time between applying for Medicaid and getting an answer is called Medicaid pending.
Don’t Miss: How Much Does Medicaid Cover For Nursing Home
Option 3 Download New Mexico Food Stamps Application
Call HSD at 1-800-283-4465 to have an application mailed to you. Complete it and mail it to your county HSD office or submit it in person.
Or mail your signed application. Send to:Central ASPEN Scanning Area PO Box 830
Or fax your signed application. Fax to:1-855-804-8960
Additionally, you can apply for Medicaid over the phone. Call: 1-855-637-6574.
New York State has separate Medicaid Applications: one for certain categories of New York City residents and the other for the rest of the state. See below and select appropriately based on your situation.
B: Investigate Alternate Pathways To Eligibility For Nursing Home Medicaid
Medically Needy MedicaidMedically Needy Medicaid is available in 36 states, and Washington D.C., and is for getting Medicaid benefits to people who spend a significant amount of their income on care costs, even if their monthly income is above the Medicaid income limit. Another way of describing Medically Needy Medicaid is to say that an applicant becomes eligible if the difference between their monthly cost of care and their monthly income is less than a specific amount set by the state.
For example, if the Medically Needy Income Limit in your state is $600, someone who makes $3,000 per month would need to spend more than $2,400 on medical expenses to be eligible for Nursing Home Medicaid despite earning more than the monthly income limit for Medicaid.
Miller Trusts or Qualified Income TrustsAnother option is Miller Trusts or Qualified Income Trusts , which can get complicated but would be described basically as special accounts for someone to deposit income that put them over the Medicaid limit. Money in the trust would not count toward eligibility and would only be accessible by the applicant for specific purposes. The trust is managed by someone who is not the Medicaid applicant and can be used to pay for medical expenses not covered by Medicaid. Not every state allows for Miller Trusts or QITs.
Also Check: Medicaid Provider Enrollment Phone Number
Satisfying The Medicaid Work Requirement
Eight states had their waivers approved for Medicaid work requirements. They included Arizona, Georgia, Indiana, Nebraska, Ohio, South Carolina, Utah, and Wisconsin. Only Indiana and Utah implemented them. Seven other states were pending approval.
Altogether, Kentucky and 18 other states applied for waivers. Arizona, Arkansas, Georgia, Kentucky, Michigan, Montana, Nebraska, Ohio, Oklahoma, South Carolina, South Dakota and Wisconsin would require 80 hours of work per month Indiana up to 20 hours per week Alabama, Idaho and Mississippi 20 hours of work per week New Hampshire 100 hours per month and Utah three consecutive months of job search/training unless they are working 30 hours per week.
What constitutes “work” also varies by state. Activities include caregiving, drug treatment, education, employment and volunteerism.
How To Spend Down To Meet Medicaid Requirements
If your income or assets exceed your states Medicaid income threshold, your state may run a spend-down program that lets you qualify for coverage by spending the income above your program limits. You can spend down by incurring expenses for medical and remedial care for which you have no health insurance coverage.
Spend-down works like an insurance deductible. You cover medical care expenses up to a specific amount for a given base period, usually three or six consecutive months.
Once the incurred medical expenses exceed the difference between your income and your states Medicaid income limit, as part of the spend-down, Medicaid benefits will be authorized for all or part of the base period. States with a medically needy program must also allow spend-down for blind, aged, and disabled people who dont meet the Medicaid eligibility requirements.
You May Like: Find A Ob Gyn Who Takes Medicaid
How To Apply For Medicaid In Florida
Knowing where and how to apply for Medicaid in Florida is important for residents who need medical benefits assistance. Petitioners must complete the FL Medicaid application form properly as well as submit the required documents. The Medicaid application and associated paperwork helps officials determine who is eligible for Medicaid coverage. Prospective applicants wondering where to apply for Medicaid in FL may be surprised about the methods and locations available for signing up for government assistance. To find out more about applying to Medicaid in Florida, continue reading the outlined information below.
Where do you sign up for Medicaid in Florida?
To find out where to apply for Medicaid, you first must look at all the options available in Florida. Applicants can apply for Medicaid online, by mail, in person or via fax. For those who have questions about Medicaid eligibility requirements, applying for Medicaid in person may be the best option, as there are representatives to assist with the process. Please be aware that enrollment in Medicaid is not lifelong. Recipients will have to reapply for Medicaid every 12 months or another predetermined time period.
Information Required on the Medicaid Application Form in Florida
The Florida Medicaid application form requires you to give a lot of details about yourself and your family. Regardless of how and where you apply to Medicaid, you will need to provide the following information:
Check The Status Of An Application
The Division of Family Resources provides tools to strengthen families through services that focus on prevention, early intervention, self-sufficiency, family support, and preservation.
You can check the status of your application online by clicking on your county of residence or by calling 1-800-403-0864. You will need to have your case number to check the status of your application.
Please remember that your application must be completed and all required documentation submitted before DFR can begin processing your application.
Pursuant to HIPAA and other applicable federal regulations, DFR is committed to respecting the privacy of each client. For that reason, DFR will not share or disclose information about your case without a signed release. You may download the DFR online.
Recommended Reading: How Do I Apply For Medicaid In Massachusetts
