How Does Ohio Regulate Long
Medicare beneficiaries increasingly rely on long-term services and supports or long-term care which is mostly not covered by Medicare. In fact, 20 percent of Medicare beneficiaries who lived at home received some assistance with LTSS in 2015. Medicaid fills this gap in Medicare coverage for long-term care, but its complex eligibility rules can make qualifying for benefits difficult. Whats more eligibility rules vary significantly from state to state.
Medicaid nursing home coverage
In past decades, most Americans received long-term care services in nursing homes. Medicaid covers these services for an unlimited number of enrollees in each state who meet income and resource limits.
Income limits: The income limit is $2,349 a month if single and $4,698 a month if married .
When only one spouse needs nursing home care, the income limit for single applicants is used and usually only the applying spouses income is counted. Non-applying spouses are allowed to keep a portion of their Medicaid spouses income.
This income limit doesnt mean nursing home enrollees can keep all of their income up to the limit. Nursing home enrollees have to pay nearly all their income toward their care, other than a small personal needs allowance and money to pay for health insurance premiums .
Assets limits: The asset limit is $2,000 if single and $3,000 if married . If only one spouse has Medicaid, federal rules allow the other spouse to keep up to $128,640.
Estate recovery in Ohio
Is It Hard To Qualify For Medicaid
As long as you meet the eligibility rules in your state, it is not hard to qualify for Medicaid. After all, almost 74 million Americans are covered by the program.
Contact your state Medicaid program in order to apply for Medicaid. Applications are generally reviewed and approved within 90 days and typically are reviewed sooner.
Also Check: Doctors That Take Medicaid For Adults
How To Choose Caresource
Medicaid health care coverage is available for eligible Ohioans with low income, pregnant women, infants and children, older adults and individuals with disabilities.
| Choose CareSource |
|---|
| When you apply for Ohio Medicaid, you can choose CareSource as your managed care plan. Whether you apply online, by mail, over the phone or at your local Department of Job and Family Services , tell them you want to choose CareSource. |
| Switch to CareSource |
|---|
| If you were assigned to another managed care plan and want to switch to CareSource, call the Ohio Medicaid hotline, complete a change request within 90 days and tell them you want to switch to CareSource. If you have been on your plan more than 90 days, you can switch to CareSource during your next open enrollment period. |
Also Check: Group Homes That Take Medicaid
B Gift And Medicaid Compliant Annuity
Individuals often require long-term care without having engaged in any prior planning. They desire to apply for Medicaid, but have assets greatly in excess of the $2,000 limit, which they would like to preserve for their family. In such situations, it may be possible to save a significant portion of a persons assets, while still allowing them to qualify for Medicaid. This requires dividing the individuals assets into two shares: the Gifted Share and the Medicaid-Compliant Annuity Share. The Gifted Share is generally given to the individuals children or to an irrevocable trust for their benefit. The Medicaid-Compliant Annuity Share is used to purchase a special annuity that is not counted as an asset for Medicaid purposes. The annuity produces a monthly stream of payments. The objective is to preserve the assets gifted to the children by using the Medicaid-Compliant Annuity to pay through the penalty period created by the improper transfer.
Dividing Assets into Gifted Share and Medicaid-Compliant Annuity Share:
Also Check: Medicaid Breast And Cervical Cancer Program Texas
Where Can Medicare Beneficiaries Get Help In Ohio

Ohio Senior Health Insurance Information Program
You can access free counseling about Medicare benefits through the Ohio Senior Health Insurance Information Program at 800-686-1578.
The OSHIIP can help you enroll in Medicare, compare and change Medicare Advantage and Part D plans, and answer questions about state Medigap protections. OSHIIP counselors may also be able to provide referrals for local home care or long-term care services. This website has more information about the services OSHIIP offers.
Elder law attorneys
Elder law attorneys can help individuals plan for Medicaid long-term care benefits. You can use this National Academy of Elder Law Attorneys search feature to find an elder attorney locally.
Also Check: Can I Get Medicaid If I Own A House
Medicaid Income Limits By State
In order to qualify for Medicaid, you must be in need of health care/insurance assistance, and your financial situation must fall under low income or very low income.
The Medicaid income limit is based on a percentage of the Federal Poverty Levels.
States generally divide Medicaid recipients into four groups.
Each of these groups has its income limit based on the Federal Poverty Level. The four groups are:
- Infants and Children
Medicaid Income Eligibility Chart State By State
The following is each of the states, listed alphabetically. Under your state of residence, you will find all of the relevant information regarding the Medicaid Income Eligibility Chart for each of three programs available: regular, in-home nursing care, and institutional nursing care.
Additionally, each of these programs will have additional information about the income limits for those who are single, married with both spouses applying, and married with only one spouse applying.
Read Also: Does Ms Medicaid Cover Dental
Who Can Get Medicaid In Ohio
You should apply for Medicaid if your income is low and you match one of the descriptions below:
- You think you are pregnant
- The parent or caretaker of a child and/or teenager under the age of 19.
- You are a child or teenager age 18 or under.
- An adult age 65 or older.
- You are legally blind.
- Living with a disability or disabled.
- You are in need of nursing home care.
Do You Qualify For Ssi Or 1619
If you have a disability, low income, and low resources, you may qualify for SSI. If you already get SSI benefits, you automatically get Medicaid coverage and do not need to apply separately.
If you dont get SSI benefits yet, you should learn whether you might qualify by reading DB101s SSI article. At the same time, you should apply for Medicaid separately, because it can take Social Security several months to review your SSI application and its important for you to have health coverage until then.
If you used to get SSI benefits, but stopped getting them after you started working, you may qualify automatically for Medicaid through a special rule called 1619 as long as your gross income is below $40,078 per year. Learn more about 1619 in DB101s SSI article.
If you do not get SSI benefits and do not qualify for 1619, income-based Medicaid might cover you.
Also Check: How To Get Contacts With Medicaid
How To Apply For Medicaid In In Ohio
Multiple methods exist for applying for Ohio Medicaid. Many people have taken to the online version which is fast to use and initiates a quick response. A pop-up window comes on the screen when attempting to start a new application. It allows users to either sign in with an existing account or create an account if it is their first time. Provide a first and last name, date of birth, and social security number to sign up and start the process.
Those who do not wish to use the online version may instead visit their local office to fill out a paper form. It can get submitted directly to a worker who can assess the information and approve or deny the claim. It is also possible to apply by telephone by calling the Ohio Medicaid Consumer Hotline at 324-8680.
If Your Income Is Low And Your State Hasnt Expanded Medicaid
If your state hasnt expanded Medicaid, your income is below the federal poverty level, and you don’t qualify for Medicaid under your state’s current rules, you wont qualify for either health insurance savings program: Medicaid coverage or savings on a private health plan bought through the Marketplace.
- Find out why
-
- When the health care law was passed, it required states to provide Medicaid coverage for all adults 18 to 65 with incomes up to 133% of the federal poverty level, regardless of their age, family status, or health.
- The law also provides premium tax credits for people with incomes between 100% and 400% of the federal poverty level to buy private insurance plans in the Health Insurance Marketplace®.
- The U.S. Supreme Court later ruled that the Medicaid expansion is voluntary with states. As a result, some states havent expanded their Medicaid programs.
- Adults in those states with incomes below 100% of the federal poverty level, and who dont qualify for Medicaid based on disability, age, or other factors, fall into a gap.
- Their incomes are too high to qualify for Medicaid in their states.
- Their incomes are below the range the law set for savings on a Marketplace insurance plan.
-
States are continuing to make coverage decisions. They could expand Medicaid in the future.
Also Check: Is Gender Reassignment Surgery Covered By Medicaid
Ohios Requirements For Medicaid Qualification
Ohio only approves applicants who meet the necessary requirements as set forth by the state. Certain income standards ensure only those who truly need the assistance receive it. With thousands of people on Medicaid in the state, it is not possible for everyone to get approved. Children and pregnant women are among the most common recipients, although adults who fall below the poverty level are now eligible as well. The Ohio Benefits website allows potential applicants to check if they may be eligible for services before even having to submit a full application.
A 2020 Medicaid Income Limits

In 2020, the maximum total monthly income from all sources that a person seeking Medicaid may have is $2,349 . If a Medicaid applicant has income greater than this amount, it is necessary to establish a Qualified Income Trust. A Qualified Income Trust is a special kind of legal instrument used for Medicaid eligibility purposes. Any income over the $2,349 limit that is placed into this Trust will be disregarded for Medicaid application purposes. Thus, a person who has income greater than the limit may still qualify for Medicaid.
Once an individual is approved for Medicaid, all of the individuals income, including any income that was placed in the Qualified Income Trust, must be used to pay for their care before Medicaid covers the balance. Medicaid allows a person to retain only $50 of income for their personal use. If the individual is married, a portion of the individuals income may be paid to the individuals spouse, if the spouses monthly income is below $2,113.75.
You May Like: How To Find Medicaid Number Without Card
How Do You Calculate Your Medicaid Income Eligibility
Follow these steps to calculate whether or not your income may qualify you for Medicaid:
- Find the FPL for your household using the chart above
- Multiply that number by your states Medicaid income limit found below, and then divide by 100
For example, if there are two people living in your household and you live in Arizona, you would multiply $17,420 by 138 and then divide by 100. That equals $24,039.60.
You may also multiply $17,420 by 1.38.
Dont Miss: Child Counselors That Accept Medicaid
What Is The Lowest Income To Qualify For Medicaid
There are 13 states that do not grant Medicaid access to individuals based on income alone.
Of those that do, only Wisconsin uses a limit lower than 138%. An individual in Wisconsin can make no more than the federal poverty level in order to qualify for Medicaid.
Texas has the lowest income limit to qualify on a family basis, at 17% of the FPL. A two-parent household with one child in Texas can make no more than $37,332 and qualify for Medicaid.
Also Check: How To Sign Up For Medicaid Ny
How Do I Become Eligible For Medicaid In My State
Most states have multiple pathways to Medicaid eligibility. Furthermore, many states allow the use of Miller Trusts or Qualified Income Trusts to help person who cannot afford their care costs to become Medicaid eligible. There are also Medicaid planning professionals that employ other complicated techniques to help person become eligible.
Dont Miss: What Is The Income Limit For Arkansas Medicaid
Find A $0 Premium Medicare Advantage Plan Today
For California residents, CA-Do Not Sell My Personal Info, .
MedicareAdvantage.com is a website owned and operated by TZ Insurance Solutions LLC. TZ Insurance Solutions LLC and TruBridge, Inc. represent Medicare Advantage Organizations and Prescription Drug Plans having Medicare contracts enrollment in any plan depends upon contract renewal.
The purpose of this communication is the solicitation of insurance. Callers will be directed to a licensed insurance agent with TZ Insurance Solutions LLC, TruBridge, Inc. and/or a third-party partner who can provide more information about Medicare Advantage Plans offered by one or several Medicare-contracted carrier. TZ Insurance Solutions LLC, TruBridge, Inc., and the licensed sales agents that may call you are not connected with or endorsed by the U.S. Government or the federal Medicare program.
Plan availability varies by region and state. For a complete list of available plans, please contact 1-800-MEDICARE , 24 hours a day/7 days a week or consult www.medicare.gov.
Medicare has neither reviewed nor endorsed this information.
Dont Miss: Does Medicaid Cover All Pregnancy Costs
You May Like: Are Adults Eligible For Medicaid
Is Your Income Low Enough For Income
These are the main income rules for income-based Medicaid:
- If your familys income is at or under 138% of the Federal Poverty Guidelines , you may qualify.
- If you are 18 or younger and your familys income is at or under 211% of FPG , you may qualify.
- If you are pregnant and your familys income is at or under 205% of FPG , you may qualify. The unborn baby is counted as a family member.
Income-based Medicaid counts most types of earned and unearned income you have. However, some income is not counted, including Supplemental Security Income benefits and some contributions to retirement accounts. Learn more about what types of income affect income-based Medicaid eligibility.
Note: There are no limits to how much money or other resources you can have for income-based Medicaid.
Your family size:If your income is low enough and you meet all other requirements, you should sign up for Medicaid.
You may see the income limit for income-based Medicaid listed as 133% of FPG in some places. However, when Medicaid counts your income, theyll knock 5% of FPG off your income if you make more than 133% of FPG. That’s why we say that you can make up to 138% of FPG, because it more accurately shows how much income you could have and still get Medicaid. For children, this means we show 211% of FPG as the limit, instead of 206%.
Submit Your Application Online
The quickest and easiest way to apply for health care benefits is to call 1-844-640-6446 and follow the prompts. You may also apply online at www.benefits.ohio.gov. There you will answer a series of questions and your answers will direct you to the correct application for health care.
- If your income is within the new legal limit implemented by Medicaid Expansion , you will be directed to the citizens self-service portal.
- If your income is above 205 percent of the Federal Poverty Level, you will be directed to the Federally Facilitated Health Insurance Marketplace to shop for health care.
After you submit your application online, you may be asked to send verification documents to Hamilton County Job and Family Services. The best way to return documents is to fax them to 946-1076. You can fax documents for free from any Public Library of Cincinnati and Hamilton County branch.
Visit www.healthcare.gov or www.benefits.ohio.gov to learn more or call the Medicaid Consumer Hotline at 1-800-324-8680. Representatives are available to answer questions related to eligibility for Medicaid due to the Affordable Care Act and Medicaid Expansion and answer questions about where to apply.
Also Check: Eye Doctors In Beckley Wv That Take Medicaid
Whats The Highest Income To Qualify For Medicaid
Federal Poverty Level thresholds to qualify for Medicaid The Federal Poverty Level is determined by the size of a family for the lower 48 states and the District of Columbia. For example, in 2022 it is $13,590 for a single adult person, $27,750 for a family of four and $46,630 for a family of eight.
Ohio’s Medicaid Income Limit
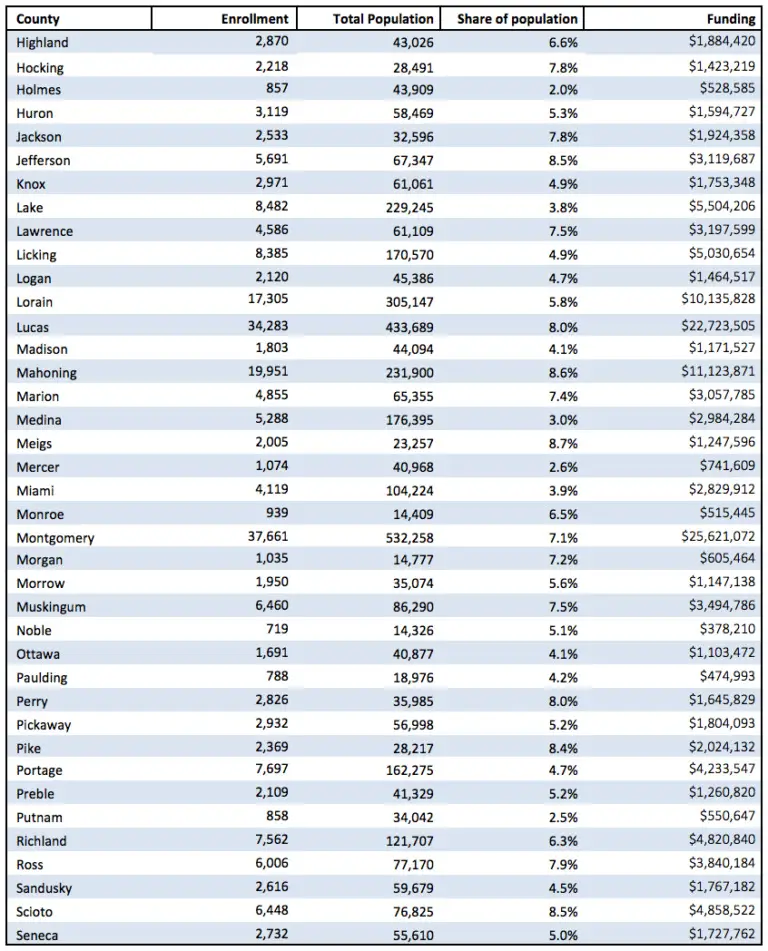
If you are 65 or older, blind, or disabled, and you need long-term care in a nursing home, then you must have income at or below $2,313 per month to qualify for Medicaid. The 2019 monthly income limit for a married couple with both spouses applying is $4,626.
If your income is above the limit, you still might be able to qualify for Medicaid if the income you have over the limit doesn’t cover your medical expenses. In Ohio, unlike some other states, people who are sixty-five and older, blind, or disabled can use unpaid medical bills, premiums, or nursing facility bills to “spend down” their income and qualify for Medicaid. A worker from ODJFS will determine how much your monthly spend-down amount is. You have to satisfy the spend-down to be eligible for Medicaid each month. You can satisfy your spend-down by showing proof that your medical expenses equal the spend-down amount or by paying the amount directly to ODJFS.
You May Like: Iowa Medicaid Customer Service Number
