Where States Stand On Medicaid Expansion
The map tracks implementation of the Affordable Care Acts Medicaid expansion in all states. The map indicates whether states are using alternative approaches through demonstration waivers, and also features information about state legislation or citizen referendums, governors stances, and other analyses. Expanding Medicaid increases coverage for people earning up to 138 percent of the federal poverty level.
*This map provides a record of legislation introduced, but does not track the exact status of bills moving through state legislatures. The map is updated when bills advance and/or become law.For information about state proposals to implement Medicaid work requirements, explore this chart.Know something NASHP should add to this map? Please email .
What Would Happen If All States Expanded Medicaid
If states that are currently not expanding their programs adopt the Medicaid expansion, all of the nearly 2.2 million adults in the coverage gap would gain Medicaid eligibility. In addition, 1.8 million uninsured adults with incomes between 100 and 138% of poverty6 would also gain Medicaid eligibility . Though most of these adults are eligible for substantial tax credits to purchase Marketplace coverage,7 Medicaid coverage would likely provide more comprehensive benefits and lower premiums or cost-sharing than they would face under Marketplace coverage. For example, research from early implementation of the ACA showed that coverage of behavioral health services, prescription drugs, rehabilitative and habilitative services, and long-term services and supports may be more limited in the Marketplace compared to Medicaid.8,9 In addition, research examining the population with incomes between 100-138% FPL in expansion and non-expansion states finds that Medicaid expansion coverage produced far greater reductions than subsidized Marketplace coverage in average total out-of-pocket spending, average out-of-pocket premium spending, and average cost-sharing spending.
Figure 3: Nonelderly Uninsured Adults in Non-Expansion States Who Would Be Eligible for Medicaid if Their States Expanded, 2019
If Your Income Is Low And Your State Hasnt Expanded Medicaid
If your state hasnt expanded Medicaid, your income is below the federal poverty level, and you don’t qualify for Medicaid under your state’s current rules, you wont qualify for either health insurance savings program: Medicaid coverage or savings on a private health plan bought through the Marketplace.
- Find out why
-
- When the health care law was passed, it required states to provide Medicaid coverage for all adults 18 to 65 with incomes up to 133% of the federal poverty level, regardless of their age, family status, or health.
- The law also provides premium tax credits for people with incomes between 100% and 400% of the federal poverty level to buy private insurance plans in the Health Insurance Marketplace®.
- The U.S. Supreme Court later ruled that the Medicaid expansion is voluntary with states. As a result, some states havent expanded their Medicaid programs.
- Adults in those states with incomes below 100% of the federal poverty level, and who dont qualify for Medicaid based on disability, age, or other factors, fall into a gap.
- Their incomes are too high to qualify for Medicaid in their states.
- Their incomes are below the range the law set for savings on a Marketplace insurance plan.
-
States are continuing to make coverage decisions. They could expand Medicaid in the future.
Don’t Miss: Does Medicaid Pay For Oxygen
Option : Get Around Stubborn States By Letting Cities Expand Medicaid
Instead of centralizing the approach, this next idea goes even more local. The COVER Now Act, introduced by Rep. Lloyd Doggett, D-Texas, would empower local jurisdictions to expand Medicaid. So, if you live in Austin, Texas, maybe you could get Medicaid, even if someone in Lubbock still couldn’t.
The political and logistical challenges would be tough, policy analysts say. Logistically, such a plan would require counties and cities to create new infrastructure to run a Medicaid program, Rudowitz notes, and the federal government would have to oversee how well these new local programs complied with all of Medicaid’s rules.
“It does not seem feasible politically,” Michener says. “The legislators who would have to vote to make this possible would be ceding quite a bit of power to localities.” It also might amplify geographic equity concerns, she says. People’s access to health insurance would not just “be arbitrarily based on what state you live in which is the current state of affairs It’s also going to be arbitrary based on what county you live in, based on what city you live in.”
What’s next: Doggett introduced the bill earlier this month. There’s no guarantee it would get a vote on the House floor and even if it did it wouldn’t survive a likely filibuster in the evenly divided Senate.
Medicaid Expansion Improves Access To Care And Health Outcomes
Medicaid expansion significantly lowered uninsured rates across the country for adults with low incomes, providing coverage to over 12 Million people.Medicaid expansion significantly lowered uninsured rates across the country for adults with low incomes, providing coverage to over 12 million people with incomes below 138 percent of the poverty line . Overall, 7.3 percent of people in expansion states were uninsured in 2019, compared to 12 percent of people in non-expansion states, which helps illustrate expansions impact.
Medicaid expansion has improved access to care and made it more affordable for enrollees, and it has increased their financial security. Along with coverage gains, greater access to care, and more financial security, expansion is linked to improvements in some measures of health outcomes and health status as well as financial benefits for states and providers, according to a review of over 400 studies. Expansion is also associated with reductions in food insecurity, poverty, and evictions, research shows. Moreover, Medicaid expansion has saved the lives of at least 19,200 adults aged 55 to 64 from 2014 to 2017.
Also Check: Dentist That Accept Medicare Medicaid
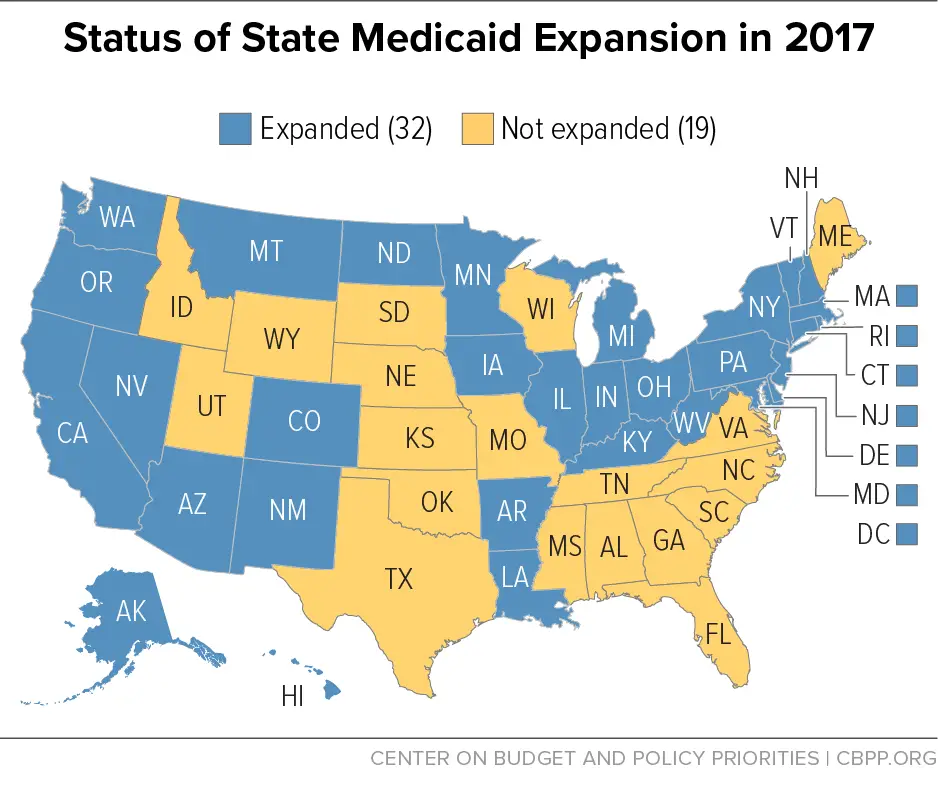
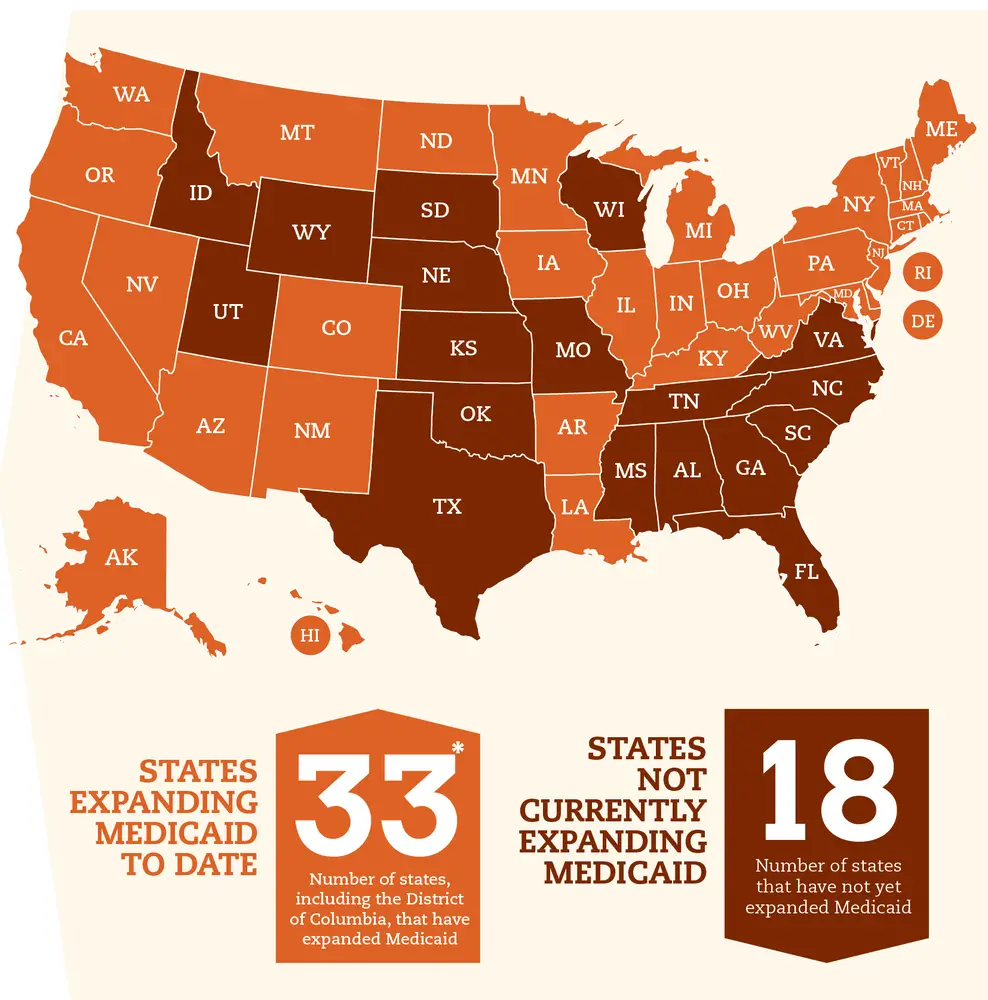
Status Of State Medicaid Expansion Decisions: Interactive Map
The Affordable Care Acts Medicaid expansion expanded Medicaid coverage to nearly all adults with incomes up to 138% of the Federal Poverty Level and provided states with an enhanced federal matching rate for their expansion populations.
To date, 39 states have adopted the Medicaid expansion and 12 states have not adopted the expansion. Current status for each state is based on KFF tracking and analysis of state expansion activity.
These data are available in a table format. The map may be downloaded as a PowerPoint slide.
Key States with Expansion Activity
This table tracks state actions related to adoption of the ACA Medicaid expansion. For non-expansion states, we include actions toward potential adoption. These include legislative actions , executive actions , and voter-led actions . We also mention some limited coverage expansions that would not qualify as full ACA Medicaid expansions and would not qualify for enhanced federal matching funds. For expansion states, we include summaries of when and how late-adopting states took up the expansion as well as notes on state attempts to place limits or requirements on the expansion population, especially through Section 1115 waivers.
What Is Medicaid Expansion
Medicaid expansion was designed to extend Medicaid benefits to groups who previously did not qualify for the program. Under the ACAs Medicaid expansion, individuals and families with incomes at or below 138 percent of the federal poverty line would be eligible. A 2012 Supreme Court decision ruled that the option to expand would be given to states rather than being implemented nationwide, as it was originally intended. This ruling has put Tennessee lawmakers in charge of Medicaid expansion for almost a decade, and they have not opted to expand yet.
Tennessee is winning the race to the bottom in terms of health. We are first in the nation for hospital closures per capita, in the bottom ten states for maternal and infant health, and we have some of the highest increases in uninsured residents, even before the pandemic. Medicaid expansion could help turn the tides on Tennessees poor health rankings by increasing healthcare coverage gains and improving long-term health outcomes.
Also Check: Therapists Rochester Ny Accept Medicaid
Democrats Treading Lightly On Bidens Next Big Health Care Promise
Health care advocates caution that Democrats have limited time to address stalled progress on Medicaid expansion seen as the biggest unfinished piece of the Affordable Care Act while the party controls Washington for the first time since the laws passage a decade ago.
This is the moment, said Judy Solomon, a senior fellow at the left-leaning Center for Budget and Policy Priorities. This is probably the only moment that well have for years.
The White House has taken a largely hands-off approach in talks over a Medicaid expansion alternative, as it has with other major health care proposals Biden campaigned on. While Bidens budget proposal on Friday reiterated his support for those ideas, including closing the Medicaid coverage gap, it was short on specifics. The only major health promise Biden proposed including in major economic legislation is the one seen as the least politically divisive: making permanent the recent Covid relief packages temporary expansion of financial help for people buying Obamacare health plans.
The President has consistently supported providing coverage for this population, an administration official said when asked about the administrations plans in Medicaid expansion holdout states.
Of the holdout states, only Wyomings legislature seriously considered an expansion bill this year, but it died in the Senate after passing the House. And recent moves in other states showed expansion still faces tough hurdles across the country.
States Losing Billions In Refusing To Expand Medicaid Report Finds
Texas will lose $9.2 billion in 2022 Florida says goodbye to $5 billion Georgia is out $4.9 billion. A new report details just how much states are losing because they dont want to expand Medicaid under Obamacare, and its not chump change.
Red states may be sticking to their Republican beliefs in small government, but the Commonwealth Fund finds they are passing up billions in federal funding by saying no to the Medicaid expansion.
By choosing not to participate, Texas, for example, will forgo an estimated $9.58 billion in federal funding in 2022. Taking into account federal taxes paid by Texas residents, the net cost to taxpayers in the state in 2022 will be more than $9.2 billion, the report by Sherry Glied and Stephanie Ma of New York University says.
We find that the Medicaid expansion will be a relatively large source of federal revenue to state enterprises,” the report adds. States expanding Medicaid will get, on average, more than twice as much in federal funding than they get in federal highway funds, they said.
Its the latest report on what Medicaid expansion would mean on a fiscal level to states, and the timing couldnt be better for the administration of President Barack Obama. The White House has launched a three-week drive to highlight what it says are the benefits of the 2010 Affordable Care Act, and Obama has been urging states to expand Medicaid.
Many Republican-led states immediately said they would not be expanding Medicaid.
Read Also: Does Medicaid Cover A Breast Reduction
States Still Say No To Medicaid Expansion
Unfortunately for millions of uninsured Americans, in 2012 the Supreme Court ruled that states could not be penalized for opting out of Medicaid expansion. And a dozen states have not yet expanded their programs.
Until late 2015, there were still 22 states that had not expanded Medicaid, but Montana began enrolling people in their newly expanded Medicaid program in November 2015, for coverage effective January 2016, Alaskas Medicaid expansion took effect in September 2015, Louisianas Medicaid expansion took effect in July 2016, and Virginia began enrolling people in expanded Medicaid as of November 2018, for coverage effective January 2019. Maine expanded Medicaid as soon as Governor Mills took office in early 2019. Utah and Idaho both implemented full Medicaid expansion as of 2020, and Nebraskas Medicaid expansion took effect in October 2020. Medicaid expansion took effect in Oklahoma in July 2021, and in Missouri in October 2021.
As a result of those 12 states refusal to accept federal funding to expand Medicaid, the Kaiser Family Foundation estimates there are 2.2 million people in the coverage gap across 11 of those states .
Being in the coverage gap means you have no realistic access to health insurance. These are people with incomes below the poverty level, so they are not eligible for subsidies in the exchange. But they are also not eligible for their states Medicaid program.
How Many Uninsured People Who Could Have Been Eligible For Medicaid Are In The Coverage Gap
Nationally, more than two million3 poor uninsured adults fell into the coverage gap that results from state decisions not to expand Medicaid , meaning their income was above Medicaid eligibility but below the lower limit for Marketplace premium tax credits. These individuals would be eligible for Medicaid had their state chosen to expand coverage. Reflecting limits on Medicaid eligibility outside ACA pathways, most people in the coverage gap are adults without dependent children.4
Adults left in the coverage gap are spread across the states not expanding their Medicaid programs but are concentrated in states with the largest uninsured populations. More than a third of people in the coverage gap reside in Texas, which has both a large uninsured population and very limited Medicaid eligibility . Nineteen percent of people in the coverage gap live in Florida, twelve percent in Georgia, and ten percent in North Carolina. There are no uninsured adults in the coverage gap in Wisconsin because the state is providing Medicaid eligibility to adults up to the poverty level under a Medicaid waiver.
Figure 2: Distribution of Adults in the Coverage Gap, by State and Region, 2019
Read Also: How Do I Get Proof Of Medicaid
States Refuse To Expand Medicaid It Hurts Us All
In 2020, Missouri residents voted to expand Medicaid, the federal health insurance program for the poor. Under the terms of the 2010 Affordable Care Act, the federal government contributes more generous funding to states that offer expanded access to the program to their residents. In Missouri, expansion would have meant an estimated 275,000 more people would have become eligible.
But in the spring, Missouris legislature refused to include funds for the expansion in the state budget, and in May, Gov. Mike Parsons.
The Human Toll Of The Medicaid Coverage Gap
Of course, theres more to Medicaid expansion than just money. Harold Pollack very clearly explains the human toll of the Medicaid coverage gap: Based on the 3,846,000 people who were expected to be in the coverage gap in January 2015, we can expect 4,633 of them to die in any given year because they dont have health insurance.
Read Also: Is Wisdom Teeth Removal Covered By Medicaid
The Effects Of Earlier Medicaid Expansions: A Literature Review
The American Rescue Plan of 2021 temporarily increased the federal government contribution for Medicaid expansion to the 13 states that have not yet expanded Medicaid coverage to all low-income adults. Since the Affordable Care Act expansion of Medicaid in 2014, there have been numerous studies that looked at its impact. These studies find first order effects including increased insurance coverage and improvements in health with no negative impact on state budgets. They also find second order, or indirect, effects such as gains in food security, housing security, financial wellbeing, and child support. These important effects have all come with little impact on state budgets as federal funding and decreases in state spending on uncompensated care, among other things, tend to cover the increased costs associated with expansion.
The Marginal Cost Of Filling The Gap
The results presented above reflect the effects of joint policies of expanding subsidies and filling the Medicaid coverage gap. An alternative way to analyze this issue is to estimate the cost of filling the gap for those below 100 percent of FPL, building on an existing policy that has previously expanded subsidies. In option 1 above, federal spending for people in the Medicaid gap increases by $16.6 billion as they become eligible for subsidies. However, spending on health grows somewhat less $15.1 billion largely because the cost of premium tax credits falls for people already in the subsidized nongroup market. Premium tax credits are smaller, because the new enrollees have lower expected health costs than the currently insured population, and those lower costs are spread among all participants in the nongroup market, lowering premiums across the board. These lower premiums lead to a small increase in enrollment among those not eligible for premium tax credits.
As shown in Exhibit 5, the 10-year costs of just filling the gap, building on existing subsidies, are $199 billion, $207 billion, and $217 billion, respectively. The cost of increasing the federal match in expansion states increases these amounts to $344 billion, $352 billion, and $362 billion, respectively.
You May Like: Is Medicaid The Best Insurance
Changes In The Uninsured By Income
Exhibit 2 and Table 4 show the reduction in the uninsured by income level.
Option 1 opens the ACA marketplace to people below the poverty level and reduces the number of uninsured below 138 percent of FPL by 2.9 million. There are small reductions in the uninsured above 138 percent of FPL because of reductions in premiums as the risk pool improves. Overall, the number of uninsured falls by 3.0 million.
Option 2 is like option 1 but with enhanced premium subsidies. It reduces the number of uninsured by 3.2 million among people with incomes below 138 percent of FPL in nonexpansion states. There are also sizable reductions in the number of uninsured at higher income levels. Overall, the number of uninsured falls by 4.6 million.
Option 3 has both enhanced premium and cost-sharing subsidies and reduces the number of uninsured below 138 percent of FPL by 3.3 million in nonexpansion states. Overall, the number of uninsured falls by 5.0 million, more than in option 2 because the cost-sharing subsidies are more generous. Both options 2 and 3 have dual objectives: filling the gap and improving subsidies.
Medicaid expansion reduces the number of uninsured below 138 percent of FPL by 4.1 million. This option increases coverage the most for low-income adults. There is a slight reduction in the uninsured above 138 percent of FPL. Overall, the number of uninsured people falls by 4.1 million.
