Does Medicare Pay For Home Care Nursing
If you meet the requirements for home health care, Medicare generally covers part-time, intermittent home care nursing and other medical therapies, such as physical and occupational therapy. If the home care nursing follows a qualifying hospital stay, Part A may cover 100% of allowable charges.
If there was no qualifying inpatient hospital stay, Part B may still cover some home care nursing services.
Medicare typically doesnt pay for more than eight hours a day of home care nursing, and it typically doesnt cover services seven days a week. Medicare only covers home care nursing for a short period of time.
If you qualify for hospice care and choose hospice benefits under Part A, Medicare pays for part-time home care nursing for as long as you receive hospice care.
How Else Can I Pay For Home Care
Besides Medicare and Medicaid, there are several programs and government aid options to help cover the costs of home care. Each has its own eligibility requirements and list of services it will cover. In addition, paying out of pocket is always an option, though many people will quickly find this cost-prohibitive without a plan to raise enough cash.
Quick Tip: To learn more about the costs of in-home care, visit our home care cost guide.
Reviewed By
Recommended Reading: Will Medicaid Cover Gastric Bypass Surgery
How And When Medicaid Can Pay For A Nursing Home
Thomas J Catalano is a CFP and Registered Investment Adviser with the state of South Carolina, where he launched his own financial advisory firm in 2018. Thomas’ experience gives him expertise in a variety of areas including investments, retirement, insurance, and financial planning.
Medicaid was created in 1965 as a social healthcare program to help people with low incomes receive medical attention. Many seniors rely on Medicaid to pay for long-term nursing home care.
Most people pay out of their own pockets for long-term care until they become eligible for Medicaid. Though Medicare is an entitlement program, Medicaid is a form of welfareor at least thats how it began. So to be eligible, you must become impoverished under the programs guidelines, says Laura M. Krohn, a Rhode Island-based elder law attorney.
Let’s look at how the economics work, and how Medicaid can be used to pay for a nursing home.
You May Like: Can I Apply For Medicaid As A College Student
Am I Eligible For Hospice Care
To be eligible for hospice care coverage, you must:
- Be certified as terminally ill. This typically means that you have an estimated lifespan of less than 6 months, although your doctor can extend this if necessary.
- Choose to accept palliative care instead of treatment to cure your condition. Palliative care is focused on providing comfort and support.
- Sign a statement indicating that youve chosen hospice care for your condition instead of other Medicare-covered treatments.
How Much Will Medicaid Pay For Nursing Home Care

For qualifying individuals, Medicaid picks up most of the tab for nursing home care, paying an average of 45 percent to 65 percent. However, coverage is largely dependent on a variety of factors such as financial status, the state you reside in, and the level of care needed.
Medicaid coverage amounts may vary from state to state, depending on the demand for nursing home care coverage. For example, the average cost of nursing home care in the state of California is on the higher end at $304 a day, compared to Texas at $165. This greatly impacts the coverage and benefits you can receive from Medicaid to offset the costs of nursing home care.
Recommended Reading: Day Care Covered By Medicaid
Medicaid Nursing Home Benefits
Medicaid pays 100% of nursing home costs in most cases if you meet eligibility requirements. In most states, the monthly income limit is $2,382 for individuals or $4,764 for spouses. Your countable resources must be less than $2,500. Income and resources that count toward the limit include:
- Life insuranceâ
âIn most states, Medicaid looks at your income over the last 5 years. Any assets you transferred out of your possession within that time may still count toward your income. Do not try to transfer financial assets in order to qualify for Medicaid.ââ
You may be penalized for violating Medicaid rules. This can result in having to pay for your nursing home care out-of-pocket until you meet eligibility requirements.ââ
Keep in mind that eligibility is on a rolling basis. It is possible to make as little as $1 over the monthly income limit and not qualify for the entire month. If this happens, you may have to pay for your nursing home care and related expenses yourself.ââ
Types of nursing home coverage. You have three nursing home options with Medicaid:
- Skilled nursing â care related to medical issues and related services
- Rehabilitation â staying in a facility short-term following an illness, injury, or surgery â
- Long-term care â around-the-clock care at a facility because of a mental or physical condition â
How Much Will Medicare Cover
Medicares coverage for skilled nursing facilities is broken down into benefit periods. A benefit period begins the day you are admitted as an inpatient to the hospital or skilled nursing facility.
Different amounts are paid throughout the benefit period. The benefit period ends when 60 days in a row have passed without a need for hospital or skilled nursing care. If you go back to the hospital after that 60-day window, a new benefit period begins.
Here are the costs that apply throughout the benefit period:
- Days 1 through 20: Medicare covers the entire cost of your care for the first 20 days. You will pay nothing.
- Days 21 through 100: Medicare covers the majority of the cost, but you will owe a daily copayment. In 2020, this copayment is $176 per day.
- Day 100 and on: Medicare does not cover skilled nursing facility costs beyond day 100. At this point, you are responsible for the entire cost of care.
While you are in a skilled nursing facility, there are some exceptions on what is covered, even within the first 20-day window.
There are some additional rules about Medicare coverage that you should know, including:
Also Check: Colorado Medicaid Home Health Care
Does Medicare Cover Nursing Homes
Medicare doesnt typically cover nursing homes, and for two reasons.
One is that Medicare seldom pays for room and board. Another is that Medicare doesnt cover custodial care if the individual doesnt specifically require attention from a medically trained specialist.
However, Medicare would cover any medical needs that might arise while a person is in a nursing home, such as needing hip surgery after a fall .
Additionally, if the care needed was above the level of a nursing home, Medicare might cover it. For example, if a Medicare-enrolled person needed rehabilitation after a surgery, Medicare Part A would pay for treatment in a skilled nursing facility . Treatment in an SNF could include a semi-private room, meals, physical therapy and more supposing the patient has enough days left on their benefit period. See everything Medicare Part A covers here.
What Happens When A Long
When a long-term care recipient dies, Estate Recovery provisions require that we take steps to recover the cost of certain Medicaid payments from his or her estate. These costs include the total amount of payments for facility or waiver services, hospital care, and prescription drugs the person received at age 55 or older.
Also Check: Whatâs The Income Level For Medicaid
Read Also: Caresource Medicaid Ohio Find A Doctor
What Home Care Services Are Covered In Choices
Here are some of the kinds of home care covered in CHOICES. Some of these services have limits. Your MCO will help you to determine what services below will meet your needs.
Some of these services can be provided through Consumer Direction.
Consumer Direction is a way of getting some of the home care you need that offers more choice and control over WHO gives your home care and HOW your care is given than receiving CHOICES services and not consumer directing. You actually employ the people who provide some of your home care services they work for you . This means you must be able to do the things that an employer would do like hire, train, and schedule workers.
You can hire a family member, friend, neighbor, or other person you know to provide care in Consumer Direction, but there are some limitations. We want to support, but not replace, care already provided by family and friends. Youll find out more if you sign up for CHOICES.
LTSS Help Desk: 1-877-224-0219
You May Like: Paramount Medicaid Ohio Phone Number
How Much Does Medicare Cover For Nursing Homes
Original Medicare nursing home coverage is intended for rehabilitation, not long-term care. It only covers a portion of nursing home expenses for a maximum of 100 days. Medicare calculates nursing home rates by time period, so your out-of-pocket cost changes over time. Below is a breakdown of what you’ll pay per benefit period during those 100 days:
- Days 21-100: $194.50 per day coinsurance
- Days 101 and beyond: All expenses
FYI: If you’re new to Medicare or just want to learn more about the program, head to our 2022 Medicare guide. It covers everything you need to know about coverage and enrolling, and it answers the most frequently asked Medicare questions.
Also Check: Psychiatrist In Richmond Va That Accept Medicaid
Paying For Nursing Home Care If You Run Out Of Money
It is possible to pay for nursing home care if you run out of money. However, you can avoid this from happening if you work with a certified financial advisor to plan as early as possible. By planning ahead, you will be able to protect assets, plan for future care needs, and give you and your family peace of mind.
Categories:
How Much Does Medicaid Pay Towards A Nursing Home
Some Medicaid services are covered 100 percent, but others are not. Because individual states manage their own Medicaid programs, the extent of coverage depends on your facility’s location. For example, different states might cover routine dental services or have higher cost allowances. The federal government does require Medicaid-certified nursing homes to provide the same minimum services.
Medicaid Pays For*
- Specialized rehabilitation
*Level of service varies by state
Medicaid Does not Pay For
- Personal comfort items
- Cosmetics or extra grooming products
- Social activities beyond the facility’s activity program
- Special care outside Medicaid-contracted coverage
Read Also: Breast Pumps Covered By Illinois Medicaid
People Who Have Both Medicare & Medicaid
People who have both Medicare and full Medicaid coverage are dually eligible. Medicare pays first when youre a dual eligible and you get Medicare-covered services. Medicaid pays last, after Medicare and any other health insurance you have.
You can still pick how you want to get your Medicare coverage: Original Medicare or Medicare Advantage . Check your Medicare coverage options.
If you choose to join a Medicare Advantage Plan, there are special plans for dual eligibles that make it easier for you to get the services you need, include Medicare coverage , and may also cost less, like:
- Special Needs Plans
- Medicare-Medicaid Plans
- Program of All-Inclusive Care for the Elderly plans can help certain people get care outside of a nursing home
Do Medicare Supplement Insurance Plans Cover Nursing Home Costs
Some Medicare Supplement insurance plans include increased coverage in skilled nursing facilities . Medicare Supplement insurance plans may cover your out-of-pocket costs for doctor visits and other medical services covered under Part A and Part B while you are a nursing home resident.
You can start comparing Medicare Advantage plans right away just enter your zip code in the box on this page.
New To Medicare?
Becoming eligible for Medicare can be daunting. But don’t worry, we’re here to help you understand Medicare in 15 minutes or less.
Also Check: Pros And Cons Of Expanding Medicaid
Medicaid And The Minimum Monthly Maintenance Needs Allowance
newwww.elderneedslaw.com
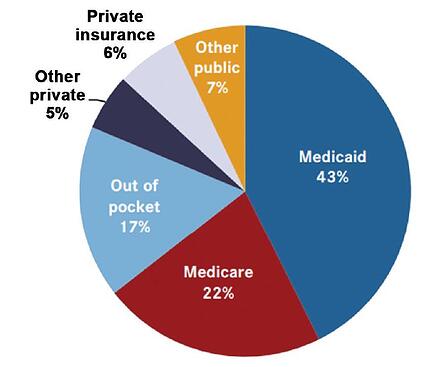
How much does Medicaid pay for home health care
Health First Colorado: Physical Benefits
Health First Colorado: Pregnancy Benefits
Health First Colorado â Keeping Your Information Up Toâ¦
Colorado Medicaid EVV | HCPF Ready EVV System
Medicare & You: Home Health Care
State officials speak to AIM Home Health terminationâ¦
Medicaid Eligibility for Nursing Home Care for theâ¦
How To Find Medicaid-Certified Assisted Living inâ¦
Health First Colorado â En Español
What is a Personal Needs Allowance in Florida Medicaid
Personal Needs Allowance ALF and Nursing Home inâ¦
Colorado Choice Transition Services â Haroldâs Story
Home Health Aide
Personal Needs Allowance â Florida Medicaid
NP Policy Update: Home Health Services for Medicareâ¦
What is Medicaid and Does It Pay For Long Term Care?
Medicare & You: Different Parts Of Medicare
Medicare & You: Ways to Save Money
Medicare & You: Nursing Home / Long-Term Care
How Do I Apply For Coverage?
Colorado Medicaid EVV | Electronic Visit Verificationâ¦
Medicare, Medicaid and Private Duty Accreditation & â¦
Apply for SNAP, Medicaid, and More from Home
Home Health and Senior Care: Barton Home Care -â¦
Nursing home staff react to President Bidenâs vaccineâ¦
Plan to Expand Medicaid In-Home Care Means Moreâ¦
Medicaid Transformation Demonstration Waiver 101
Which Health Policies Actually Work?
Nursing home against proposed Medicaid changes
Fremont County Health Dept. confirms first outbreak atâ¦
Does Medicare Pay For A Skilled Nursing Facility
Medicare does not cover the full amount of time in a skilled nursing facility beyond what is required by its regulations. Medicare covers SNF care as follows:
- On days 1 through 20, Medicare will cover 100% of the approved cost.
- The beneficiary must pay a daily co-payment on days 21 through 100, while Medicare covers the rest.
- Medicare pays nothing beyond Day 101.
You May Like: Are You Automatically Enrolled In Medicare At 65
Read Also: Florida Medicaid Asset Protection Trust
Medicare Covers Some Short
Medicare Part A, which covers inpatient hospital services, will pay for short-term stays in a Medicare-certified skilled nursing facility in some situations. Your doctor may send you to there to receive specialized nursing care and rehabilitation after a hospital stay.
Care in a skilled nursing facility is covered only if you had a qualifying hospital stay, meaning that you were formally admitted as an inpatient to the hospital for at least three consecutive days. This is different from observation status, which doesnt count even if you stayed in the hospital overnight.
When you enter the hospital, ask if you are being officially admitted or if you are there only for observation. That will be important in determining the beginning of your benefit period, which begins the day you are admitted to a hospital as an inpatient or become a patient in a skilled nursing facility, and ends when youve been out of those places for 60 days in a row. These rules also mean you might have more than one benefit period in a year.
You must be admitted to a skilled nursing facility within 30 days of leaving the hospital for the same illness or a condition related to it. Your doctor also must certify that you need daily skilled care from, or under the supervision of, skilled nursing or therapy staff.
Medicaid Coverage Of Nursing Home Care
Medicaid is a federal government program administered jointly with state governments, and it pays long-term nursing home costs for people with low income and few assets . Each state administers its own Medicaid program, with slightly different eligibility rules. In some states, Medicaid pays some of the cost of assisted living for eligible residents in participating facilities.
Read Also: Can A Pregnant Woman Get Medicaid
Medicaid For Texans In Assisted Living Facilities
Assisted living facilities provide food, personal care services like help with bathing or dressing, and medication administration. Historically, Medicaid did not pay for ALFs. However, Texas has a program offering Medicaid payment for assisted living facilities, if you meet specific criteria.
If you are otherwise eligible for Medicaid and if you can show that a nursing home is medically necessary for you , then you may qualify for STAR+PLUS Waiver services. This program pays for home- and community-based services, including assisted living facilities, for people who would otherwise have to be institutionalized in a nursing home. The STAR+PLUS Waiver program has limited enrollment and there may be a waiting list for certain services. For more information, contact the ALF program staff of Texas Health and Human Services.
Texas also offers continuing care retirement communities , which combine independent living, assisted living, and nursing home care in one residential setting. CCRCs, which are regulated by the Texas Department of Insurance, typically charge entrance and monthly fees. Once in a CCRC, you can use long-term care insurance, private insurance, Medicare, or Medicaid to pay for some of your health care, depending on your coverage options and the types of services you require.
Types Of Nursing Home Costs Medicaid Covers

For eligible beneficiaries, Medicaid pays the full cost of room and board in a nursing facility, plus any therapies that are part of the nursing homes regular resident care. Medicaids payment also includes personal care items such as incontinence supplies and toiletries, as well as services such as bathing, grooming, and laundry.
Theres no time limit on Medicaid nursing home coverage, and the Medicaid beneficiary has no co-payments to make.
The income limits for Medicaid nursing home coverage eligibility are different for an unmarried, divorced or widowed person than for a married couple.
Also Check: Primary Care Doctors Who Take Medicaid
Does Medicaid Cover Nursing Homes
Yes, Medicaid covers the cost of nursing homes, though coverage varies from state to state. Also, Medicaid should cover the cost of a nursing home once a person receiving Medicare coverage falls below a specified resource level.
A nursing home that meets the federal standards set by Medicaid will provide the following free of charge to Medicaid-eligible residents:
- Semi-private room
- Basic grooming and hygiene services
Medicaid doesnt include any extras . Items or services such as these will be charged to the resident.
To check your eligibility for Medicaid or ask questions about your states Medicaid program, see this Medicaid.gov hub of state sites.
