How To Apply For Medicaid And Chip
Medicaid is a federal and state-wide health insurance program available to people with low incomes.
The Childrens Health Insurance Policy provides health insurance for children. For eligibility, the family of the child must earn an income that is
- Too high to qualify for Medicaid
- Too little to be able to afford private insurance
How To Choose Your Medicaid Caregiver
Medicaid often allows beneficiaries to choose their own caregiver. Beneficiaries can designate a family member or friend as their paid primary caregiver who will be reimbursed by Medicaid for their service. Select states even allow a spouse to be hired as the primary caregiver.
You also do not have to be in your own home to receive home health care benefits from Medicaid. Home care coverage may be extended to the home of a friend or relative, adult foster care home or assisted living home.
Do I Qualify For Full Medicaid
- The eligibility requirements vary from state to state, but generally states consider your annual income and financial assets when determining whether you are eligible for full Medicaid.
- If you live in one of the 37 states that will have expanded Medicaid as of next January and you earn no more than 138 percent of the federal poverty level , you may qualify. In states that havent expanded the program, the income levels for Medicaid eligibility vary greatly. For all eligibility questions, you should check with your state Medicaid office.
- If you are a Medicare beneficiary, your enrollment in Medicaid may be subject to a financial asset test. The value of assets youre allowed to have and still be eligible varies from state to state. The federal guidelines allow you $2,000, but some states have higher thresholds while others dont have an asset test at all.
- Excluded from the $2,000 asset test are such things as your home, one car, some burial expenses, some life insurance and household and personal items. States generally look back at an applicants assets for five years to make sure they havent divested themselves of those resources just to qualify for Medicaid.
- The asset income limits for Medicare Savings Programs are higher and change every January. For 2018, the limits for those programs are $7,560 for a single person and $11,340 for a married person living with a spouse and no dependents. As with full Medicaid, some states have higher resource thresholds.
Also Check: How Do I Know If My Medicaid Is Active
Can You Have Both
People who qualify for both Medicare and Medicaid are considered dual eligible. In this case, you may have original Medicare or a Medicare Advantage plan , and Medicare will cover your prescription drugs under Part D.
Medicaid may also cover other care and drugs that Medicare doesnt, so having both will probably cover most of your healthcare costs.
Medicare Advantage And Medicaid Whats The Difference

The Medicare Advantage program is considered a âpartâ of Medicare â Medicare Part C. If you qualify for both Medicare and Medicaid, you can generally sign up for a Medicare Advantage plan. Or, you might want to look into the Medicare Savings Programs described above.
Many people prefer Medicare Advantage plans as a way to get their Medicare coverage. Medicare Advantage is a program that lets you get your Medicare Part A and Part B benefits through a private, Medicare-approved insurance company. Many plans have extra benefits, too, like prescription drug coverage and routine dental care.
Read Also: Pediatricians In Austin Tx That Accept Medicaid
What Is Pace For Medicare And Medicaid
Another Medicare and Medicaid program is PACE, or Programs of All-Inclusive Care for the Elderly.
PACE helps older Medicare beneficiaries to seek health care within their community, in their home and at PACE facilities.
Some of the things that can be covered by PACE include:
- Adult day primary care
- Caregiver training
- Transportation to a PACE facility when medically necessary
PACE is not strictly restricted to Medicare dual eligible beneficiaries. You may be eligible for PACE with only Medicare or only Medicaid .
However, you must meet all of the following conditions:
- Be at least 55 years old
- Live in the service area of a PACE organization
- Require a nursing home-level of care
- Be able to live safely in the community with help from PACE
Dont Miss: Does Medicare Cover Chronic Pain Management
What Steps Do I Need To Take To Move From Expanded Medicaid To Medicare
If youre enrolled in expanded Medicaid and youll soon be 65, youll want to familiarize yourself with the health coverage and assistance programs that might be available to you.
Understand that although your assets have not been taken into consideration to determine your eligibility for expanded Medicaid, that will likely change when you turn 65. Every state has an asset limit for full Medicaid eligibility if youre 65 or older, and most states also have asset limits for their MSPs.
But if you do qualify for an MSP particularly the Qualified Medicare Beneficiary program along with Extra Help for prescription drugs you may find that you still qualify for premium-free coverage and very limited out-of-pocket costs.
Youll want to reach out to your states Medicaid office prior to turning 65, to be sure you understand the specifics of 65+ Medicaid and MSP eligibility.
You can also reach out to the Medicare SHIP in your state, to see what resources and assistance are available to you.
You might also want to find a Medicare broker who can help you understand the available Medigap, Part D, and Medicare Advantage plans. Your limited income might make you a good candidate for a low-cost or zero-premium Medicare Advantage plan, leaving you with just the cost of Medicare Part B.
Heres more about choosing between Medigap and Medicare Advantage theres no single solution that works for everyone, so take your time and compare the options available to you.
Also Check: Infertility Clinic That Takes Medicaid
If I Have Medicaid Do I Need Medicare Part D
Those that have Medicare and Medicaid will automatically be enrolled in a Part D plan if they dont select one for themselves. Its in the enrollees best interest to select a policy to enroll in, instead of being dropped into a plan. But, either way, Medicaid will help cover the costs associated with premiums, copayments, or coinsurances.
Extra Help Program For Medicare Part D
Medicaid is not the only government-sponsored resource that helps pay for medical costs. An individual can also apply for Extra Help, a program that helps beneficiaries with Medicare Part D, which covers prescription drug costs.
To qualify for Extra Help, a personâs combined investments, real estate, and savings must not exceed $29,160 if a person is married and living with their spouse or $14,610 if a person is single.
A person can visit Medicareâs website to find out more about getting and applying for Extra Help.
Don’t Miss: Ohio Medicaid Customer Service Phone Number
What Might Medicaid Pay For That Medicare Doesnt
- The premium for Medicare Part B, which covers doctor visits and other outpatient services. That monthly premium will be $135.50 in 2019.
- The Medicare Part B deductible, which will be $185 for 2019.
- The Medicare PartA deductible, which for 2019 will be $1,364 for hospital stays.
- Both Medicare Part A and Part B copays and coinsurance.
- The Medicare Part D premium, deductibles and copays for prescription drugs. Coverage for those costs is available through the Extra Help program, which Medicaid and Medicare Savings Program enrollees automatically qualify for.
- Nursing home care and home- and community-based long-term services and supports.
- In some states, Medicaid will cover benefits that Medicare does not, such as dental care, transportation to and from doctor visits, eyeglasses, physical therapy and other services.
The Problem: Medicare Alone Will Cost You Money
Medicare is a great health insurance program, but it does have costs. You must pay your monthly Part B premium to stay enrolled in Medicare, plus premiums, out-of-pocket costs, etc. Copayments for medical services and prescriptions can add up beyond what many people can afford.
You could even wind up paying more than other folks for the same basic Medicare coverage, simply because extra coverage add-ons are out of reach.
Don’t Miss: Change My Ohio Medicaid Plan
What Is Fbde For Medicare And Medicaid
Full-Benefit Dual-Eligible individuals are eligible for Medicare and full Medicaid benefits through their state. FBDE beneficiaries qualify for coverage of the following through Medicare Savings Programs: Medicare Part A and Part B premiums, deductibles, coinsurance, and copays. FBDE beneficiaries often pay $0 out-of-pocket for any medically necessary healthcare services.
Do You Get Guaranteed Issue Rights For Loss Of Medicaid Coverage
If you are dual-eligible for Medicare and Medicaid and find yourself in a situation where your income increases and exceeds your state Medicaid requirements, you will receive guaranteed issue rights in certain states. However, not all states grant beneficiaries these rights when they lose Medicaid eligibility.
If your state grants guaranteed issue rights in this scenario, you would be eligible to enroll in the Medicare Advantage or Medicare Supplement plan of your choice.
Get A Free Quote
Find the most affordable Medicare Plan in your area
Recommended Reading: Can You Get Medicaid If You Have Insurance
Is There An Open Enrollment Period For Medicaid
- No. You can enroll in Medicaid at any time during the year. But in many states you have to update your enrollment information every year to make sure you still qualify. If you dont, you can lose your coverage. Jennifer Goldberg, directing attorney at Justice in Aging, says: We see people who dont know they dont have coverage until they get a bill or show up at the pharmacy and the prescription they used to pay $1 for is showing up as $100.
Also Check: How Do I Find Out My Medicare Number
Can I Be Enrolled In Medicare And Medicaid At The Same Time
Q: Can I be enrolled in Medicare and Medicaid at the same time?
A: In many cases, yes. Some Americans qualify for both Medicare and Medicaid, and when this happens, it usually means they dont have any out-of-pocket healthcare costs.
Beneficiaries with Medicare and Medicaid are known as dual eligibles and account for about 20 percent of Medicare beneficiaries . Dual eligibles are categorized based on whether they receive partial or full Medicaid benefits.
Full-benefit dual eligibles have comprehensive Medicaid coverage, while partial benefit dual eligibles receive help with Medicares premiums and cost sharing through a Medicare Savings Program .
The federal government oversees Medicare eligibility meaning it is the same in each state. But states set their own eligibility rules for Medicaid and the MSPs and income limits for these programs vary widely.
You May Like: Denture Places That Accept Medicaid
Medicaid Vs Medicare: You Can Have Both
Posted: January 17, 2020
Medicaid and Medicare. Its hard to think of two words that cause as much confusion.
- Whats the difference between these two government health insurance programs?
- What exactly are Medicaid and Medicare?
- Whos eligible to get Medicaid or to get Medicare?
- And how can some people get both?
Read on to find out the answers to these questions and more.
How Do You Qualify For Medicaid
You qualify for Medicaid based on your finances. Medicaid needs to see difficulties with one of two things:
What are the income requirements?
Medicaid is primarily a state-run program. Each state runs its own Medicaid program the way it sees fit. They also set local financial standards to receive Medicaid benefits.
Thats why you may qualify for Medicaid benefits when you apply, but your friend with similar income and assets who lives in a different state doesnt. It all depends on where you live.
Medicaid has two funding sources: the state and the federal government. Therefore, the money to operate Medicaid is split between the federal governments contribution and the taxes a state collects.
Keep in mind that annual income limits for Medicaid are indexed to the federal poverty level. In 2021, the limit in the continental U.S. was $12,880 for an individual and $17,420 for a couple.
Recommended Reading: Florida Medicaid In Home Care
D: Prescription Drug Coverage
Medicare Part D provides prescription drug coverage. The beneficiaries are required to pay the cost of Part D plans out-of-pocket and are required to pay monthly premiums, an annual deductible, and copays for specific prescriptions.
Participants enrolled in Medicare Part C may only be interested in Part D if their plan does not cover prescription drugs.
Can You Have Medicaid And Medicare At The Same Time
You could potentially be eligible for Medicare and Medicaid. If you are, you’re considered dual eligible. In this case, you may qualify for a certain type of Medicare Advantage plan called a Dual Eligible Special Needs Plan .
You can compare plans online to find out if D-SNPs are available where you live.
Also Check: Can You Have Savings And Get Medicaid
What Are The Benefits Of Medicare
While Medicare plans have varying benefits, they must all provide a baseline of coverage. Part A plans must include:
- Inpatient hospital stays
- A yearly check-up
Part B plans also cover ambulance rides, medical equipment, and more.
Medicare does not cover long-term care in the home. It also does not include dental care, eye exams, foot care, and hearing aids.
C How Will Those Default Enrolled In A Dual

Once default enrolled, the individual will be enrolled in the aligned Medicare D-SNP for primary coverage and prescription drug coverage, AND will remain enrolled in the Medicaid managed care or HARP plan for secondary coverage.
If the individual received Medicaid home care or other LTSS from the MMC plan, they are default enrolled into a MAP plan. These plans provide ALL Medicaid services, not just those covered by MLTC plans These members must make sure to use only providers in the plan’s network, whether the provider is providing a Medicare or Medicaid service.
Also Check: I Have Medicare How Do I Apply For Medicaid
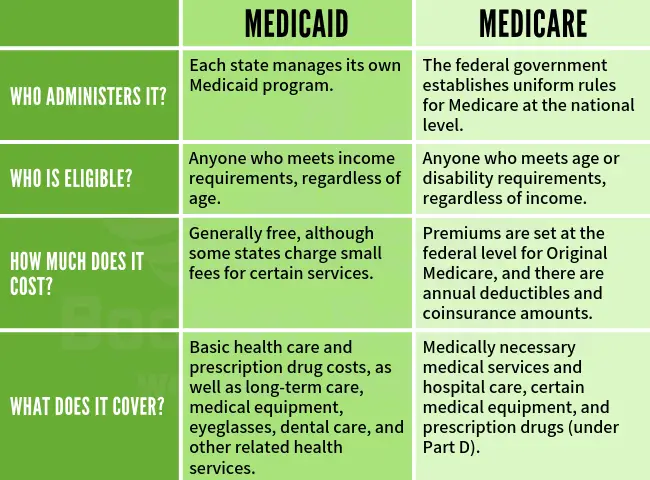
What Are The Main Differences Between Medicare And Medicaid
The key difference between Medicare and Medicaid is who is eligible for each program. There are different rules for eligibility, and there may be circumstances where you qualify for Medicaid but do not qualify for Medicare, and vice versa.
Another difference is that Medicaid covers long-term care services and support, while Medicare will often limit this form of coverage.
What Is The Difference Between Medicare And Medicaid
If youve ever been confused about the differences between Medicare and Medicaid, you are not alone. Simply put, both Medicare and Medicaid are government-regulated health insurance programs that help to provide healthcare service and treatment to millions of Americans, but each program has slightly different rules of eligibility and provides different coverage to different groups of people.
Recommended Reading: Which Medicare Plans Cover Silver Sneakers
Read Also: Does Medicaid Cover Eye Exams And Glasses For Adults
Where Can I Find Out More
- Medicaid.gov has links to information explaining the program and to every states Medicaid office.
- Each state has a State Health Insurance Assistance Program that provides counseling and help for Medicare beneficiaries. SHIP counselors can answer some of your Medicaid questions and refer you to local Medicaid officials to help with others.
- The National Council on Aging has a benefits checkup website that has information on Medicare, Medicaid and other programs that help older Americans.
More on Medicare
D Which Plans Have Been Approved In Nys For Default Enrollment
As of June 2021, the following plans were approved for default enrollment. Some were added to those originally approved for the 1st batch of default enrollment in April 2021. updated with DOH info as of 3/3/21 and with CMS Medicare Dual-SNP plan info for 2022. See MRC Flier Default Enrollment in New York State.
See also list on NYS Dual Eligibles webpage under the IB-Dual dropdown:
- MMC plans approved for default enrollment into a D-SNP
Metroplus MMC and HARP – will be enrolled into Metroplus Advantage Plan iin NYC ONLY
Empire Health Plus D-SNP MMC and HARP
2021/2022 – D-SNP was Empire MediBlue HealthPlus Dual Plus
UnitedHealthcare MMC/HARP – Default enrolled in MANY counties – see LIST HERE – into:
2021 – UnitedHealthCare Dual Complete H3387
2022 – UnitedHealthcare Dual Complete 1 H3387
Fidelis MMC/HARP – In MANY COUNTIES -Default enrolled into:
2021- D-SNP was Fidelis Dual Advantage
2022 – D-SNP is Wellcare Fidelis Dual Access
- MAP -MMC plans approved for default enrollment into a MAP plan
-
Empire Health Plus MMC and HARP plans — enrolled into HealthPlus Medicaid Advantage Plus – Default enrolled into:
-
2021- Empire MediBlue HealthPlus Dual Advantage
-
2022 – Empire MediBlue HealthPlus Dual Connect H1732
Healthfirst MMC and HARP plans – default enrolled into “Healthfirst CompleteCare” MAP Plan
Fidelis MMC/HARP – In NYC, Albany, Montgomery, Rensselaer, Schenectady – See LIST HERE – Default enrolled into
2021- Fidelis Medicaid Advantage Plus
2022 – Wellcare Fidelis Dual Plus
You May Like: Who Qualifies For Medicaid In Mississippi
The Solution: Medicaid Could Make Up The Medicare Difference For You
Some people think that Medicaid is welfare, but that is not true. Medicaid covers medical expenses, long-term care services, case management, and much more. Medicaid is a different program than Medicare.
Medicaid is for people whose incomes are close to the federal poverty line. Today, Medicaid provides extra help paying doctor bills, hospital bills, and prescriptions for millions of Americans aged 65 and over. If you fall into this category, then youll want to take a close look at your Medicaid eligibility.
Not Limited to Seniors
Others besides seniors can receive Medicaid benefits In all states, Medicaid provides health coverage for some low-income people, families and children, pregnant women, the elderly, and people with disabilities. In some states the program covers all low-income adults below a certain income level. People with a disability or certain medical conditions may qualify for Medicaid at any age.
