What Does Part B Of Medicare Cover
Medicare Part B helps cover medically-necessary services like doctors services and tests, outpatient care, home health services, durable medical equipment, and other medical services. Part B also covers some preventive services. Look at your Medicare card to find out if you have Part B.
The basic medically-necessary services covered include:
- Abdominal Aortic Aneurysm Screening
- Tests
- Transplants and Immunosuppressive Drugs
To find out if Medicare covers a service not on this list, visit www.medicare.gov/coverage, or call 1-800-MEDICARE . TTY users should call 1-877-486-2048.
Medigap Helps Cover Medicare Copayments
There are 10 standardized Medigap plans available in most of the United States. These plans help you pay out-of-pocket costs associated with Original Medicare.
Most Medigap plans cover some or all of the costs of your Medicare Part A and Medicare Part B deductibles, copayments and coinsurance. Two of the 10 plans cover either 50 or 75 percent of copayment and coinsurance costs.
You cannot, however, buy a Medigap plan if you have a Medicare Advantage plan.
What Is The Federal Poverty Level
The Federal Poverty Level is a measure of income issued yearly by the Department of Health and Human Services .
The HHS uses FPL to decide whether you might qualify for medical programs and benefits, including Medicaid, based on your income.
For 2020, here are the numbers to determine Federal Poverty Level.
- For one individual – An annual income of $12,760.
- For a family of 2 people – An annual household income of $17,240.
- For a family of 3 people – An annual household income of $21,720.
- For a family of 4 people – An annual household income of $26,200.
- For a family of 5 people – An annual household income of $30,680.
- For a family of 6 people – An annual household income of $35,160.
- For a family of 7 people – An annual household income of $39,640.
- For a family of 8 people – An annual household income of $44,120.
A note about income, AGI, and MAGI
We listed the incomes based on the number of people in your household that determine whether you fall over or under the Federal Poverty Level .
But we have to go one step further and briefly describe how the Health and Human Services defines income, when it comes to your eligibility for benefits.
This is where AGI and MAGI come in .
AGI – AGI is your adjusted gross income. It is your income that is deemed taxable after you deduct any eligible expenses, etc.
- Untaxed foreign income
- Social Security benefits that are non-taxable, if any
- Any tax exempt interest youâve earned in the previous fiscal year
Also Check: Iowa Dhs Medicaid Income Guidelines
Will Medicare Pay For A Yearly Physical Examination
En español | Medicare does not pay for the type of comprehensive exam that most people think of as a physical. But it does cover a one-time Welcome to Medicare checkup during your first year after enrolling in Part B and, later on, an annual wellness visit that is intended to keep track of your health.
Initial visit: The Welcome to Medicare visit with your doctor aims to establish the state of your health when you enter the program and provide a plan of future care. The doctor will:
- record your vital information
- review your personal and family health history
- check risk factors that could indicate future serious illnesses
- recommend tests and screenings that could catch medical issues early and provide a checklist of preventive services to help you stay healthy
- offer you the option of discussing end-of-life issues, including information on how to prepare an advance directive naming someone to make medical decisions on your behalf if you became too ill to make them yourself
- provide counseling and referrals as appropriate
Annual visit: During an annual wellness visit, the doctor measures your height, weight, body mass and blood pressure, and may listen to your heart through your clothes. The rest is a discussion of your own and your familys medical history, any physical or mental impairments, and risk factors for diseases such as diabetes and depression.
Both services are free of charge if the following conditions are met:
Also Check: Does Medicare Pay For Breast Reconstruction
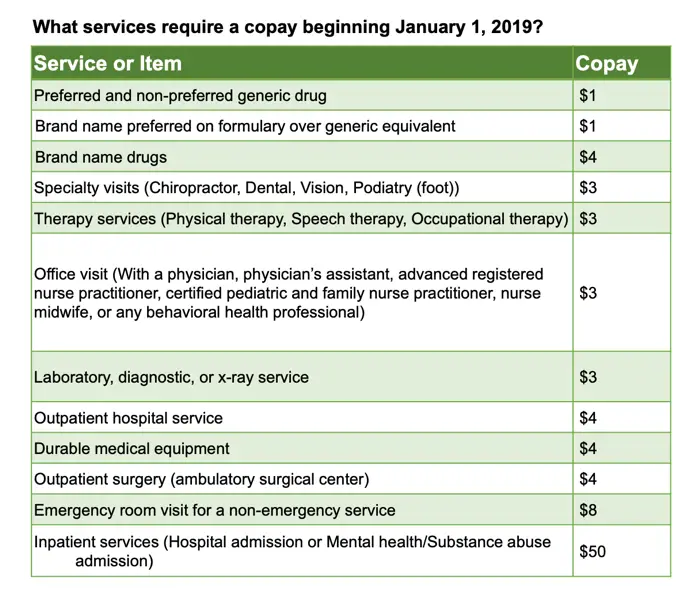
What Services May Require A Medicaid Copay
There are a variety of services that might require a copay, including the following.
- In patient services, where you are officially admitted to the hospital
- Outpatient services, like tests, consultations, clinic appointments, etc.
- If you have to go the emergency room for non-emergency care
- Prescription drugs
Don’t Miss: How Do I Find My Medicaid Number Online
How Does An Office Visit Copay Work
- Post comments:
Office visit copays work differently depending on the type of plan you have. An office visit copay works differently for a Medicare PPO plan than a Medicare HMO plan. And the Medicare Supplement Plan N copay is also different then the previous two plans.
Medicare Supplement Plan N Plan N has a copay of $20 per visit. Plan N also has an annual outpatient deductible of $198 which first needs to be paid before the copays commence. Once the copays start, you are responsible for the $20 copay for each Dr visit, lab, x-ray, outpatient surgery, physical therapy, etc. The Plan N hospital benefit is 100% coverage.
HMO Typically when you receive services from your HMO primary care physician or a specialist, whatever services or procedures and costs you receive during the visit, all are included in your Plan co-pay. For example you schedule a visit because your knee hurts from your day of hiking. The doctor who sees you discusses your knee issue, examines your knee, has you walk down the hall for an X-Ray, then gives you a cortisone shot. If your HMO plan has a $30 copay, that is all you would pay for this days visit.
Some PPOs offer plans with unlimited office visit co-pays, other plans have a limited number of co-pays per year, such as three or five, after they are used you simple pay the cost of the visit. And others offer no office visit co-pays.
Have questions or would like more details, please contact me anytime.
John Conner
How Do You Enroll In Medicare
You can enroll in original Medicare directly through the Social Securitys website during your initial enrollment period. This period includes the 3 months before, the month of, and the 3 months after your 65th birthday.
If you miss your initial enrollment period or want to change or enroll in a different Medicare plan, here are the additional enrollment periods:
- General and Medicare Advantage enrollment: from January 1 to March 31
- Open enrollment: from October 15 to December 7
- Special enrollment: a number of months depending on your circumstances
The initial enrollment period is the time in which you can enroll into Medicare parts A and B. Once youre enrolled in original Medicare, though, you may decide that you would rather enroll into a Medicare Advantage plan.
Before you choose an Advantage plan, youll want to shop around to compare the different plans available in your area. Comparing benefits, health perks, and plan costs including copay amounts can help you choose the best Medicare Advantage plan for you.
Also Check: How Much Do You Have To Earn To Get Medicaid
How Are Part D Copays Determined
Since Medicare Part D plans are sold by private insurance companies, they can choose how much to charge for a copayment. Medicare Part D copays can vary between plans, which is why it is important to compare plans before enrolling in prescription drug coverage.
Generally, Part D plans organize their covered prescription drugs into different tiers. The tiers determine how much a copay will cost for a specific drug. Each plan can determine how to organize its tiers, which means different plans can have a different tier structure. Here is an example of a Medicare Part D drug plan tier according to Medicare.gov:
- Tier 1lowest copayment: most generic drugs
- Tier 2medium copayment: preferred, brand-name drugs
- Tier 3higher copayment: non-preferred, brand-name drugs
- Specialty tierhighest copayment: very high-cost prescription drugs
It is important to note, once you enter the last two parts of the four coverage stages of Medicare Part D you will no longer pay your plans set copay amount. Instead, in the coverage gap or donut hole phase, you will be responsible for 25% of the cost of your medications. After you exit the donut hole phase and enter the catastrophic coverage phase, your prescription drug costs will dramatically decrease and youll only be responsible for around 5% of the cost of your medications.
When Does Medicare Not Cover Medical Visits
Medicare doesnt cover certain medical services that you may consider preventive or medically necessary. However, there are sometimes exceptions to this rule.
For questions about your Medicare coverage, contact Medicares customer service line at 800-633-4227, or visit the State health insurance assistance program website or call them at 800-677-1116.
If your doctor lets Medicare know that a treatment is medically necessary, it may be covered partially or fully. In some instances, you may incur additional, out-of-pocket medical costs. Always check before you assume that Medicare will or wont pay.
Other circumstances under which Medicare will not pay for a medical appointment include the following:
There may be other medical visits and services that Medicare wont cover. When in doubt, always check your policy or enrollment information.
Also Check: My Texas Benefits Pregnancy Medicaid
Copays With Medicare Advantage
When it comes to copays, Medicare Advantage is a whole other story. Medicare Advantage, or Part C, refers to a way of receiving your Medicare coverage through a private health insurance company. If you have a Medicare Advantage plan, many of the associated fees will be set by that insurance company, rather than Medicare. Although there are some regulations on these costs, there will be more variety.
This means that some Medicare Advantage plans will have copays, and others wont. The amount of the copay will vary, and some plans may use copays for one type of care while using a coinsurance for others it depends. If you have a Medicare Advantage plan, make sure that you know in advance what the copay is, so you can be prepared when you go see your healthcare provider.
Can I Be Refused Service If I Cant Pay My Medicaid Copay
If your income level falls below 100% FPL, the provider canât refuse you service even if youâre not able to pay your out-of-pocket expense. But you may be billed for your copay at a later date and youâll be held liable for what you owe.
If your income is above 100% FPL, then the provider might have the option to refuse you care if you arenât able to pay your copay, depending on your state. If you fall in this category and you have questions, it is best to contact your state Medicaid administration.
If you fall under one of the exempt groups, the medical services provider who accepts Medicaid can never refuse you service.
For all the details on Medicaidâs âcost-sharingâ rules, check out Medicaid.govâs Overview of Cost Sharing and Premium Requirements.
You May Like: Phone Number For California Medicaid
Medicaid Coverage In The State Of New York
There are insurance companies that provide services to Medicare recipients to manage the relationship between the state and the individuals. They make sure that you get all the benefits youâre entitled to and help you navigate the process.
In the state of New York, there are quite a few of these providers. With a little research, you will find the one that best suits your needs.
For detailed information, be sure to check out our page on best Medicaid plans in NY.
Ability To Pay Copays:

If you are unable to pay your copayment, you cannot be refused medical services. However, you still owe the copayment to your health care services provider. Your health care services provider may refuse medical services if you have past unpaid copayments. Your health care services provider must tell you that this is their policy and they must have the same policy for all of their patients.
Read Also: The Phone Number For Medicaid
A Solution To The Medicare Copay Problem
RE AssistRE AssistSolving the Medicare Co-pay DilemmaA Solution to the Medicare Copay ProblemRE Assistaverage 70-year-old$3200are four times more likely to abandon therapyRE AssistSolving the Medicare Co-pay DilemmaSponsored guest posts are bylined articles that are screened by Drug Channels to ensure a topical relevance to our exclusive audience. These posts do not necessarily reflect our opinions and should not be considered endorsements. To find out how you can publish a guest post on Drug Channels, please contact
Can Doctors Refuse Medicare
The short answer is yes. Thanks to the federal programs low reimbursement rates, stringent rules, and grueling paperwork process, many doctors are refusing to accept Medicares payment for services.
Medicare typically pays doctors only 80% of what private health insurance pays. While a gap always existed, many physicians feel that Medicare reimbursements havent kept pace with inflation in the past several years, especially the rising costs of running a medical practice. At the same time, the rules and regulations keep getting more onerous, as do penalties for not complying with them.
Most American physicians participate in Medicare and accept assignment for their services without additional charges. However, if your doctor is non-participating or has opted out of Medicare, here are five options.
Also Check: Who Qualifies For Qmb Medicaid
Who Is Exempt From Medicaid Copay
The detailed exemption from Medicaid copay may vary depending on the state, but in general the following groups are exempt from Medicaid copay.
- Children
- People who have reached their quarterly limit of Medicaid copay
- People who are terminally ill, including those in hospice
- Medicaid recipients who are living in an institution
- Alaska Natives and American Indians who have ever received a treatment from the Indian Health Service, tribal health programs, or under contract health services referral
- Women in the Breast and Cervical Cancer Treatment Medicaid Program are exempt from alternative out of pocket costs
One critical factor to keep in mind is that youâll most likely still have access to medical care even if you donât fall in the exempt group and canât pay your out-of-pocket expense, especially if youâre severely ill. But if you arenât exempt, you might be billed for the unpaid copay later on.
Medicaid Copay For Emergency Room Visits
Emergency services are exempt from Medicaid copay. But there are situations and reasons why you may visit the ER even when it is not an emergency. Or, you might not be sure if itâs an emergency and visit the ER to be on the safe side.
In such situations, your state has the right to charge a copay for non-emergency use of emergency room services.
If your income is below 150% of FPL, then your copy will be nominal. But if it is above 150$ FPL, then there is no limit on the copay, and could reach the max for the quarter, which is 5% of your quarterly household income .
Medicaid regulations make sure that the hospitals donât abuse the ability to charge copays. Before they can charge you a copay for using the ER, the hospital has to meet certain conditions.
- They have to conduct an adequate screening to determine that the situation is not actually an emergency.
- They have to inform you about the costs associated with the non emergency service.
- An alternative non-emergency medical provider is available and accessible with the necessary timeframe to provide treatment.
- The copayment of the alternative provider must be less than the use of the emergency room.
- They must provide you the directions and instructions to access the other provider.
- The hospital must also assist in the process of setting up a visit with an alternative provider.
Also Check: Who Is Eligible For Medicaid In Nebraska
You Will Not Be Charged A Copayment If:
- Younger than age 21
- Pregnant or your pregnancy ended up 90 days ago
- Living in a nursing home or an intermediate care facility for the mentally retarded
- Receiving emergency services in a hospital, clinic, office, or other facility
- Receiving family planning-related services
- In a managed care plan that does not charge copayments
Have Medicare And Medicaid
If you have Medicare, there is a prescription drug benefit program known as Medicare Part D that helps you pay for your prescriptions. Medicaid will only pay for certain prescriptions that Medicare Part D does not cover. Be sure to give both your Medicare Part D and your Medicaid cards to your pharmacist.Also, you will automatically qualify for “extra help” so you will not be charged a deductible or monthly premiums. However, you will have to pay copayments between $1 and $5 per prescription.
Recommended Reading: Does Medicaid Cover A Breast Reduction
Behavioral Health And Substance Use Disorder Services
If you are enrolled in a private health plan through MassHealth, call the health plans member-services department for the names of behavioral health and substance use disorder providers who participate in that health plan. If you are not enrolled in a health plan, you can go to any therapist who takes MassHealth. If you need help finding a behavioral health or substance use disorder provider, you can call the MassHealth Customer Service Center.
How To Apply For Medicaid
You can apply for Medicaid at any time you do not have to wait for an open enrollment period. If you think medical expenses may qualify you for Medicaid, you can apply to find out.
You can apply for Medicaid even if you already have health insurance, and you wont be penalized for switching plans outside of open enrollment. If you do already have insurance and are deemed eligible for Medicaid, make sure you discontinue your current health plan.
If you think you make too much money to qualify for Medicaid, but your income is close to the eligibility levels, there are three good reasons to apply anyway:
- You may still gain coverage if you have a lot of medical bills.
- If you have children, your application doubles as a CHIP application for them.
- Your states Medicaid office can help find other health insurance solutions for you.
You can apply for Medicaid in two ways: through the Affordable Care Act marketplace or through your states Medicaid office. Once you apply, you should receive more information on what to expect and how to use your Medicaid benefits.
Also Check: Does Nc Medicaid Cover Chiropractic
