Section : Who Is Eligible To Apply For Medicaid In Missouri
Eligibility for the MO HealthNet program is based on several factors including income and resource criteria. Disabled, blind, and elderly individuals who meet the income and resource requirements may qualify as well as pregnant women and children. Indeed, children make up the majority of Medicaid recipients in the state of Missouri at this time.
Low-income women who are pregnant or who have recently given birth may qualify for Medicaid. Parents, guardians, and caregivers in low-income families may also be eligible. The goal of the program is to make sure that low-income individuals are able to find good health, treat illness, avoid premature death, and correct, rehabilitate, or limit a disability.
To qualify for the MO HealthNet program, applicants must be U.S. citizens, permanent residents, legal, aliens or nationals and a resident of Missouri who is in need of health care and insurance assistance. Your financial situation must be considered âlow-incomeâ or âvery low-incomeâ according to certain federal and state guidelines. And you must also be disabled , blind, elderly , pregnant, or be a parent or relative caregiver of dependent children who are under the age of 19 years.
Virginia Medicaid Phone Number
Heres how to contact the Virginia Medicaid Agency:
For Medicaid Applicant & Member Services
Cover Virginia also operates a statewide customer service call center for Medicaid and the FAMIS Programs:
The call center provides:
- Explanation of coverage and benefits
- Assistance in resolving application issues
- Assistance in submitting state-sponsored health insurance applications and
- renewals Records address, household, and income changes
- Enrolls individuals in their choice of managed care organization or assists
- them in changing their MCO
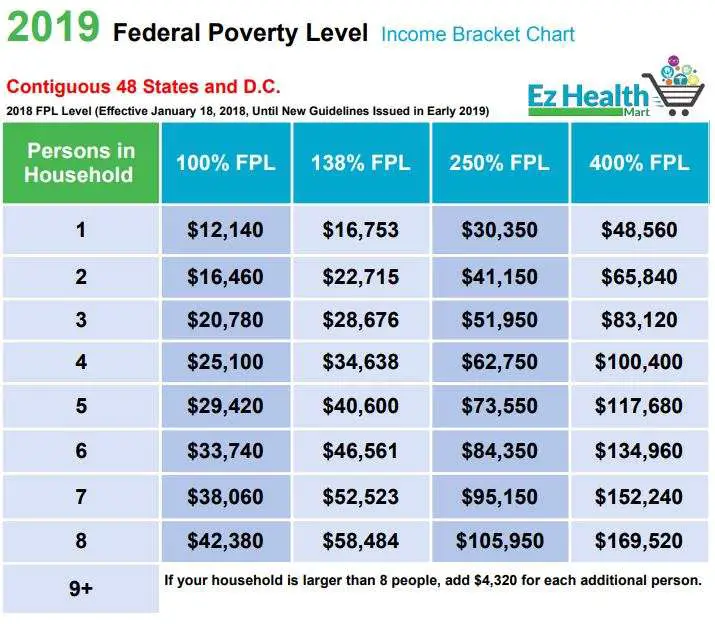
How Is The Federal Poverty Level Used In Health Care
The federal poverty level is used to determine eligibility for Medicaid and CHIP to determine eligibility for ACA premium tax credits and cost-sharing reductions and eligibility for Medicare Savings Programs .
Medicaid and CHIP:
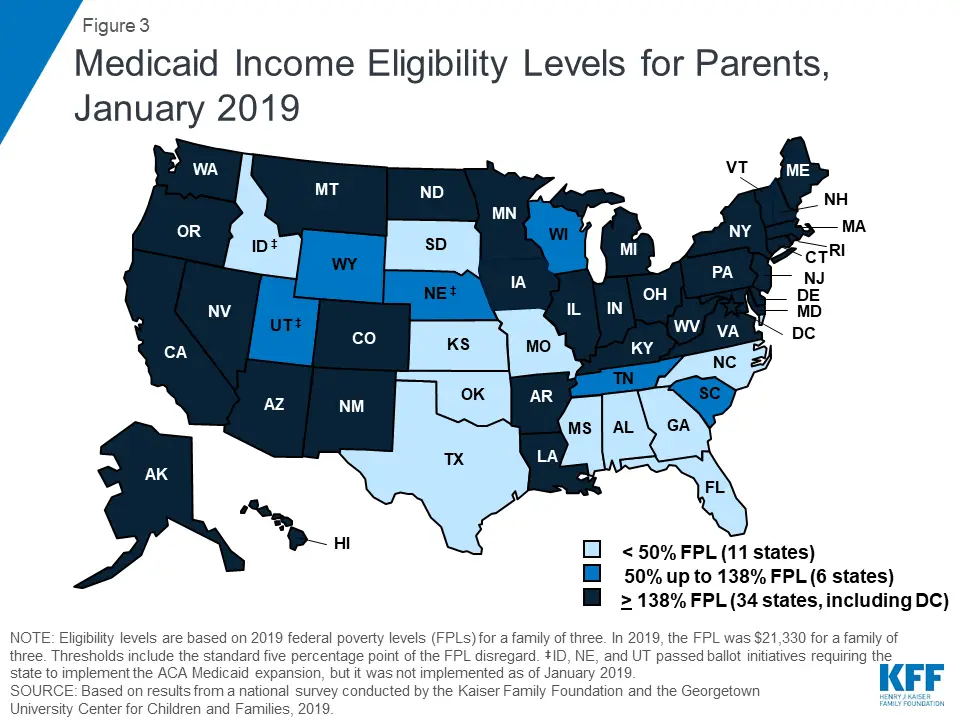
- In states that have expanded Medicaid, Americans under the age of 65 will qualify for Medicaid if they earn up to 138% of the federal poverty level.
- In states that havent expanded Medicaid, the eligibility guidelines are stricter, with much lower income limits for parents and coverage generally not available at all to non-disabled childless adults, regardless of how low their income is. This creates a coverage gap that exists in a dozen states as of 2021.
- For people who are disabled or 65+, Medicaid eligibility also depends on assets .
- CHIP eligibility is also based on the federal poverty level, but the specific thresholds vary from one state to another.
- For Medicaid and CHIP eligibility determinations, the current years federal poverty level numbers are used .
Premium tax credits:
Cost-sharing reductions:
| If more than 8 in household / family, add $4,480 per additional person. | If more than 8 in household / family, add $5,600 per additional person. | If more than 8 in household / family, add $5,150 per additional person. |
Don’t Miss: Blue Cross Complete Medicaid Providers
South Dakota Medicaid For Individuals In Assisted Living Facilities Nursing Facilities Or Homes
Individuals in assisted living centers, Nursing Facilities or Homes who meet all eligibility criteria may qualify for South Dakota Medicaid.
Eligibility Requirements
- A person must be 65 years or older. If under age 65, a person must be blind or disabled.
- A person must be a resident of South Dakota and meet certain citizenship requirements of the United States.
- Medical needs of the individual are such that they require a level of care provided in a nursing home.
- The monthly income limit is 300 percent of the SSI Standard Benefit Amount.
- The resource limit is $2,000. Resources include items such as checking and savings accounts and certificates of deposit.
What Does Medicaid Cover In Florida
The amount and type of services that will be covered by Medicaid will depend on things like how old the beneficiary is, which program the beneficiary is actually enrolled in, and even the type of services that will be necessary medically. These services might include community behavioral health, prescription medications, visual, dental, transportation, hospice, nursing home, home health care, family planning, hospital, doctor visits, and more.
Read Also: Dentist In Meridian Ms That Accept Medicaid
How Medicaid Eligibility Is Determined
Income eligibility is determined by your modified adjusted gross income , which is your taxable income, plus certain deductions. Those deductions include non-taxable Social Security benefits, individual retirement contributions and tax-exempt interest. For most people, MAGI is identical or very close to your adjusted taxable income, which you can find on your tax return. Specific income requirements in dollars rise alongside the size of your household.
Our guide focuses on each stateâs major programs for adults. Most are only available to state residents, U.S. citizens, permanent residents or legal immigrants .
Looking for insurance for a child? Check out our guide to the Children’s Health Insurance Program .
How Federal Poverty Levels Are Used To Determine Eligibility For Reduced
- Income above 400% FPL: If your income is above 400% FPL, you may now qualify for premium tax credits that lower your monthly premium for a 2021 Marketplace health insurance plan.
- Income between 100% and 400% FPL: If your income is in this range, in all states you qualify for premium tax credits that lower your monthly premium for a Marketplace health insurance plan.
- Income below 138% FPL: If your income is below 138% FPL and your state has expanded Medicaid coverage, you qualify for Medicaid based only on your income.
- Income below 100% FPL: If your income falls below 100% FPL, you probably wont qualify for savings on a Marketplace health insurance plan or for income-based Medicaid.
“Income” above refers to “modified adjusted gross income” . For most people, it’s the same or very similar to “adjusted gross income” . MAGI isn’t a number on your tax return.
Read Also: Is My Medicaid Still Active
Who Is Eligible For Medicaid 272 Medically Needy
2.7.2 Medically Needy Program The Medically Needy program is for individuals who would be eligible for Florida Medicaid except for income or assets that exceed the limit for eligibility. If the households income is greater than the income limit, the exceeding amount is determined as the share of cost.
Whats The Income Level Requirement To Qualify For Medicaid
The income level to be eligible for Medicaid will be determined by two factors. First, the state you live in. While the federal Medicaid program sets minimum standards, each state has the authority to increase the income eligibility level in order to provide coverage for more people.
Income eligibility for federal Medicaid standards is based on the Federal Poverty Level or a percentage of the FPL. The table below shows income levels based on FPL and family size.
| Family Size | |
|---|---|
| $73,460 | $91,825 |
So, for example, if your state sets eligibility at 200% of the FPL, you just look at 200% and find your family size to see what your maximum income can be for eligibility. In order to determine the income eligibility levels for your state, you can visit your states Medicaid website. You can also contact the Medicaid office within your county. When you apply for Medicaid, you apply through the county office.
The second factor taken into consideration is the size of your household. The more people there are in your household the higher your income can be. For Medicaid, a household is determined by those that are claimed as dependents when filing your taxes. It includes you, your spouse, and any dependents, which may include children, elderly parents, or other elderly or disabled relatives.
Also Check: How To Recertify For Medicaid
South Dakota Medicaid For Certain Newborns
South Dakota children born to women eligible for South Dakota Medicaid are also eligible for South Dakota Medicaid.
Eligibility Requirements
- The child must be born to a woman eligible for and receiving South Dakota Medicaid on the date of the childs birth.
- There is no resource or income limit.
- Coverage continues from the month of birth until the end of the month in which the child turns one year of age as long as the child continues to live in South Dakota.
Who Qualifies For Medicaid
In all but 13 states, adults who make below a certain income may qualify for Medicaid. In all states, Medicaid is available to people who make a low income and also meet other criteria such as being at least 65 years old, disabled, pregnant or other qualifications.
Each state runs its own Medicaid programs with its own set of qualifying criteria.
Recommended Reading: How Can I Check The Status Of My Medicaid Application
What Is The Income Limit For Missouri Medicaid
Individuals who qualify for the federal Supplemental Security Income program who are disabled according to the SSI guidelines are eligible for Missouri Medicaid as long as their income doesnât exceed certain levels. For disabled individuals, income should not exceed 85% of the Federal Poverty Level . For blind individuals, income should not exceed 100% of FPL. Some disabled individuals may also qualify to receive MO HealthNet financial assistance to pay for Medicare premiums, deductibles, and copayments.
The elderly can sometimes spend down their incomes or medical expenses in order to meet the Medicaid income requirements in Missouri. âSpending downâ is a term that refers to the amount of medical expenses that a person must pay monthly in order to become eligible for Medicaid coverage. An individual or couple may need to spend down their income so that their net income is equal to or lower than the income eligibility requirement for the Missouri Medicaid program.
âSpending downâ to meet income eligibility requirements may include either of the following:
â Monthly submission of medical expenses to a caseworker
â Monthly payments of the spend down amount to the MO HealthNet Division
MO HealthNet may also provide assistance to some seniors to pay their Medicare premiums, deductibles, and copayments.
Medicaid And Medicare Dual Eligibility
If you qualify for both Medicare and Medicaid, you are considered dual eligible. In this case, you may qualify for a certain type of Medicare Advantage plan called a Dual Eligible Special Needs Plan . D-SNPs are designed to meet the specific needs of people who have Medicaid and Medicare.
You can compare plans online to find out if D-SNPs are available where you live, or you can call to speak with a licensed insurance agent for information about eligibility and enrollment.
Also Check: Do Newborns Automatically Get Medicaid
District Of Columbia Medicaid
Eligibility overview: Washington, D.C., has one of the most generous Medicaid programs in the U.S., covering adults with household incomes up to 215% of the FPL as part of its expansion program. It also has programs for pregnant, parent/caretaker, elderly, disabled and child residents.
Income requirements: The expansion covers adults without dependents who make up to $2,082 a month when applying on their own. Elderly, blind or disabled D.C. residents are eligible if they make up to 100% of the FPL, or $1,073.33 per month for one individual, and have resources below $4,000 for one person. D.C. also covers pregnant women with incomes up to 319% of the FPL, or $4,703.40 monthly for a two-person household, and parents/caretakers with incomes up to 216% of the FPL.
How to apply for Washington, D.C. Medicaid: You can apply online at DC Health Link or by visiting your closest Income Maintenance Administration Service Center.
Other notable programs: Long-term care and nursing home care services Spend Down, a Medicaid program for people who exceed income limits, but have high medical bills Emergency Medicaid for people who canât qualify for standard Medicaid due to citizenship/immigration status.
What Are The Eligibility Requirements For Medicaid In Missouri
The MO HealthNet program covers individuals who meet certain income and resource criteria including:
â Low-income families
â The elderly
â Blind/visually impaired individuals
â Disabled individuals
â Pregnant women
â Newborns and infants
â Uninsured women under the age of 65
The income criteria for eligibility is determined by poverty guidelines set forth by the federal government. Resource criteria typically apply only to the elderly, disabled, and blind individuals. For these applicants, resources such as savings and countable assets can impact eligibility for the program.
Blind and disabled individuals can qualify for Medicaid due to a âphysical or mental impairment, disease, or lossâ that prevents them from working at a job within their skill level for 1 year or longer. Anyone who qualifies for assistance through the federal Supplemental Security Income program is automatically considered eligible for the MO HealthNet program on the basis of disability.
You May Like: Does Walmart Vision Center Accept Medicaid For Contacts
Virginia Medicaid Income Limit
The Virginia Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the Virginia Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 143 percent of FPL
- Any child age 1-5 with a family income up to 143 percent of FPL
- Children ages 6- 18 with family income up to 143 percent of FPL
- CHIP for children with family income up to 200 percent of FPL
- Pregnant women with family income up to 143 percent of FPL
- Parents of minor children with family income up to 49 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 81% of the FPL
- Adults without dependents under Medicaid expansion with income up to 133% of the FPL
California Governor Proposes Tax Cuts Expanded Health Care
Gov. Gavin Newsom wants to make California the first state to cover all low-income state residents under its Medicaid plan regardless of their immigration status
Family forcibly separated at the border speaks out
SACRAMENTO, Calif. — With state revenues at an all-time high, California Gov. Gavin Newsom on Monday proposed a budget that would cut taxes while also promising to pay the health care expenses of all of the state’s low-income adults who are living in the country illegally.
It will cost state taxpayers about $2.2 billion per year to cover the cost of health care for the state’s low-income immigrants. Meanwhile, Newsom’s tax cuts would reduce revenue by more than $6.5 billion.
But the numbers still balance because California has a projected $45.7 billion surplus, driven by incredible growth in tax collections during the pandemic. California taxes the wealthy more than people with lower incomes to the point that, in 2019, the top 1% of earners paid nearly 45% of all the state’s income tax collections.
That top 1% has only gotten richer during the pandemic. While California has the highest unemployment rate in the country, it is on pace to collect at least $25 billion in capital gains taxes in 2021, the most ever. A capital gain is income that comes from selling an asset, like a stock, and is how most wealthy people make their money.
Don’t Miss: How To Get Both Medicare And Medicaid
Lawfully Residing Targeted Low
States have the option to provide CHIP and Medicaid coverage to children and pregnant women who are lawfully residing in the United States and are otherwise eligible for coverage, including those within their first five years of having certain legal status. If states do not adopt this option, federal law requires a 5-year waiting period before many legal immigrants are permitted to enroll in Medicaid and CHIP. Learn more about providing health coverage to lawfully residing children and pregnant women at 2107 of the Social Security Act, and in SHO# 10-006 . A list of states providing Medicaid and CHIP coverage to lawfully residing children and/or pregnant women.
South Dakota Medicaid For Youth Formerly In Foster Care
The Former Foster Care Medical Program provides extended medical coverage for youth age 18 to 26 that are leaving State foster care after their 18th birthday. Referrals for this program are normally generated by the Division of Child Protection Services staff. You may also call 877.999.5612 for further information.
Eligibility Requirements
- The youth must have been in foster care under the responsibility of the State of South Dakota on his/her 18th birthday.
- The youth must be a resident of South Dakota.
- There is no resource or income limit.
- Eligibility continues from the month the youth is no longer under the responsibility of the State until the end of the month in which the youth attains age 26 if s/he meets all other eligibility requirements.
Also Check: Medicaid Provider Enrollment Phone Number
Is It Hard To Qualify For Medicaid
As long as you meet the eligibility rules in your state, it is not hard to qualify for Medicaid. After all, almost 74 million Americans are covered by the program.
Contact your state Medicaid program in order to apply for Medicaid. Applications are generally reviewed and approved within 90 days and typically are reviewed sooner.
Which Medicaid Plan Is Best In Florida
Each Medicaid plan in Florida comes with the same core benefits which are listed here. You can also compare the performance data for the various plans in your area by using what is known as the Medicaid Health Plan Report Card. You will also have to consider things like the types of services that might be needed along with how many doctor visits that will be necessary, the plan that is accepted by your doctors, the types of doctors you will need, and what extra benefits will meet your needs.
Recommended Reading: Medicaid Assisted Living Austin Texas
