How Does The Acas Medicaid Expansion Affect State Budgets
Under the ACA, the federal government paid 100 percent of the cost of Medicaid expansion coverage from 2014 to 2016. The federal share then dropped gradually to 93 percent in 2019 and will settle at 90 percent in 2020 and each year thereafter. By comparison, the federal government pays between 50 and 76 percent of the cost of other Medicaid enrollees, depending on the state.
Many states and independent analyses have found that the Medicaid expansion has not only helped more than 12 million low-income people gain health coverage but also produced net savings for state budgets. It has done so by allowing states to move people who previously received health services through targeted Medicaid programs financed at the states regular match rate, such as family-planning services and care for certain women with breast and cervical cancer, into the new expansion group, for which the federal government pays nearly all of the cost. And as more low-income uninsured residents have gained coverage, demand for entirely state-funded services that serve the uninsured has declined, such as funding for hospitals uncompensated care costs and for mental health services. States like Arkansas, Colorado, Michigan, and Virginia expect the expansion to produce net budgetary savings in the coming years even though states have had to pay a modest share of the expansion costs since 2017.
Understand Your Employers Health Coverage Costs
In the past, many employers offered health care with little or no premium required from the employee. Employees are now required to carry a bigger and bigger portion of the premium. It is important to not only know the employee portion of premium, but all other relevant costs like deductibles, coinsurance, and Maximum-Out-of-Pocket .
Medicaid Is Structured As A Federal
Subject to federal standards, states administer Medicaid programs and have flexibility to determine covered populations, covered services, health care delivery models, and methods for paying physicians and hospitals. States can also obtain Section 1115 waivers to test and implement approaches that differ from what is required by federal statute but that the Secretary of HHS determines advance program objectives. Because of this flexibility, there is significant variation across state Medicaid programs.
The Medicaid entitlement is based on two guarantees: first, all Americans who meet Medicaid eligibility requirements are guaranteed coverage, and second, states are guaranteed federal matching dollars without a cap for qualified services provided to eligible enrollees. The match rate for most Medicaid enrollees is determined by a formula in the law that provides a match of at least 50% and provides a higher federal match rate for poorer states .
Figure 2: The basic foundations of Medicaid are related to the entitlement and the federal-state partnership.
Also Check: Therapists In Lansing Mi That Accept Medicaid
Transitioning From Expanded Medicaid To Medigap
The more expensive way to cover the gaps in traditional Medicare is to buy a Medigap policy, which generally costs anywhere from a minimum of $25/month to more than $200/month to cover out-of-pocket costs for Parts A and B. Thats on top of premiums for Medicare Parts B and D .
The payoff is maintaining unlimited access to all healthcare providers who accept Medicare which almost all providers do. Heres more about choosing between Medigap and Medicare Advantage.
If I Lose My Job Or Find A New Job Will I Lose My Medicaid Coverage How About My Family Members
No. Unlike employer-sponsored plans, Medicaid is not tied to your job. Youll still have it even if you lose your job because of COVID-19 or for any other reason. If you find a job, your new financial situation will determine whether you qualify for Medicaid. Your eligibility is based on income, age, residency, citizenship, ability, pregnancy, family size and the role you play in your household.
You May Like: Will Medicaid Cover Gastric Bypass Surgery
Large Vs Small Employers
If you work at a small employer plan, your employer is permitted to require you to get Medicare when you turn 65. At that time, Medicare will become your primary health insurer. Your employer also has the option to cancel your workplace plan or retain it as a secondary payer of covered insurance claims. This distinction is important because it can affect the package of Medicare plans you may need, especially whether you need a Medigap supplement plan.
If you work at a large employer plan, your employer cannot treat you differently than younger employees. You and, if applicable, your spouse, must continue to be offered employer health insurance. These rules are very clear. If an employer with a large health plan tells you that you must get Medicare at age 65, it is breaking the law. The single exception is for people turning 65 who have end-stage renal disease they can be required to get Medicare.
Employees with access to large employer-sponsored plans do not have to get Medicare, but they may do so if they wish. Historically, employee plans were so comprehensive and affordable that it seldom made sense for someone to get Medicare. However, rising health care expenses have led many employers to reduce the percentage of the coverage they pay, with many adopting high-deductible plans.
Anyone considering this decision should contact their employer plan. They should ask two primary questions:
Do Beneficiaries Have Adequate Access To Health Care
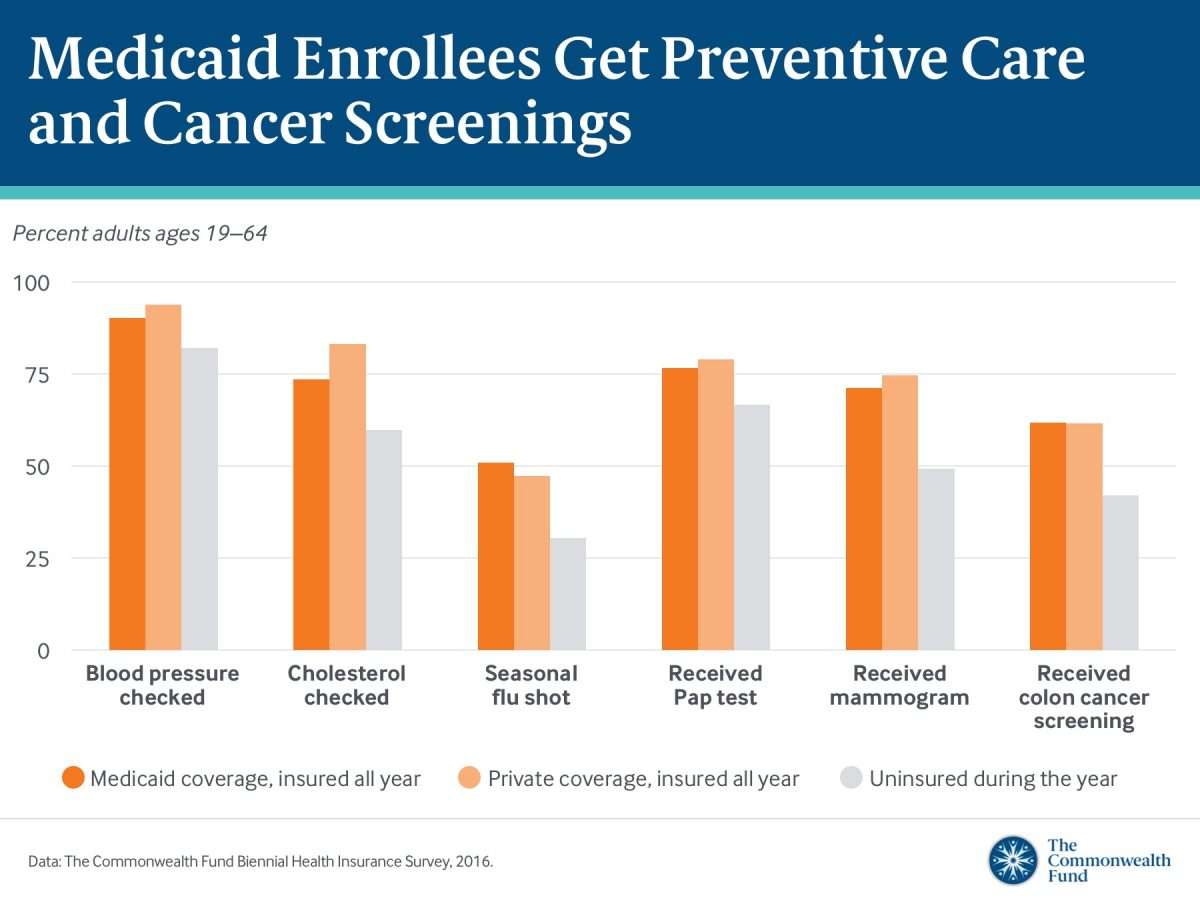
Numerous studies show that Medicaid helps make millions of Americans healthier by improving access to preventive and primary care and by protecting against serious diseases.
Notably, the ACAs expansion of Medicaid to low-income adults prevents thousands of premature deaths each year, a landmark study found. It saved the lives of at least 19,200 adults aged 55 to 64 over the four-year period from 2014 to 2017. Conversely, 15,600 older adults died prematurely because of some states decisions not to expand Medicaid. The lifesaving impacts of Medicaid expansion are large: an estimated 39 to 64 percent reduction in annual mortality rates for older adults gaining coverage.
This new research is consistent with earlier studies finding that the ACAs Medicaid expansion improves the health and financial well-being of those who newly gain coverage. One recent study, for example, found that expansion states had a lower mortality rate for near-elderly adults than non-expansion states. Another study, comparing low-income adults in Arkansas and Kentucky with similar adults in Texas , found the expansion has increased utilization of primary care and screenings and treatment for chronic conditions like diabetes. It has also resulted in fewer skipped medications due to cost, lower out-of-pocket medical spending, and improved overall health. Moreover, the benefits of the Medicaid expansion grew in its second year of implementation, the study found.
Recommended Reading: Does Medicaid Pay For Partial Dentures
How To Switch To Your Spouse’s Health Insurance Policy
If you and your spouse are both eligible for employee health benefits, you may want to explore each company’s health insurance options to see which is best for you and your wallet.
If you want to switch to a spouses policy, or your spouse wants to enroll in yours, its usually a simple task to accomplish. However, its important to get the timing right and to know when youre eligible for special enrollment periods .
Im Single And Just Lost My Job Is Medicaid For Me
Maybe. Medicaid eligibility is based on where you live, how much money you make each year and the number of people in your household.
Its worth applying even if you dont think you qualify. Whether you have children, are pregnant or have a disability are all taken into consideration. You can check to see whats offered in your state through the Aetna Better Health website.
Do I qualify for Medicaid?
Those who earn less than a certain amount can qualify for Medicaid.
Depending on the state where you live, you can be covered if your income is below these ranges:
$16,970-$25,520 for a household of one
$22,929-$34,480 for a household of two
$28,887-$43,440 for a household of three
$34,846-$52,400 for a household of four
Recommended Reading: Medicaid Customer Service Number Va
Q If I Dont Qualify For Medicaid Is There Any Other Help For Me Or My Children
A. Yes. Many organizations in Delaware are dedicated to the principle that health care should never be beyond the reach of those who need it. If you need health care, but do not have insurance coverage, the people at the Delaware HelpLine have a wealth of information about organizations that provide health care at reduced rates for uninsured individuals. Call the Delaware HelpLine toll-free at 1-800-464-HELP from Monday Friday from 8:00 a.m. to 5:00 p.m. The Delaware Helpline service is also available in Spanish. Additional information about the support provided by the Delaware Helpline can also be found by visiting www.delawarehelpline.org.
For example, you may qualify to receive discounted medical services through the Community Healthcare Access Program . CHAP helps connect uninsured individuals with affordable health care from primary care doctors, medical specialists, and other health providers including prescription programs, laboratory and radiology services. To find out more about this program, visit the website for the Community Healthcare Access Program, or call 1-800-996-9969 for eligibility guidelines.
You can read about CHAP and other healthcare resources for uninsured individuals in the Delaware Healthcare Resource Guide. This guide is also available in Spanish: Guía de Recursos de Salud.
Under 18:
Over 65:
I Got Laid Off But They Offered Me Cobra It Is Way Too Expensive Can I Qualify For Medicaid
Maybe. For many people, COBRA, the insurance you can buy into when you lose your job, is too expensive. And even if you decide to enroll in COBRA, it doesnt mean you cant apply for Medicaid. You can apply for and enroll in Medicaid any time. If you qualify for Medicaid, you can drop your COBRA coverage even after you enrolled in it.
Recommended Reading: Assisted Living In New Jersey That Accepts Medicaid
What If I Am On Medicare Still Working And Have An Employer Health Insurance Plan
If you decide to leave your job, or lose your job, you have options available to you, you may be eligible for COBRA, which is a federal law that allows eligible individuals to keep their existing employer-sponsored health insurance coverage after experiencing a qualified event, like reduced employment hours, loss of dependent child status, divorce, or death of a covered employee. For more information, see Triage Cancer’s Quick Guide to COBRA.
COBRA might be a good option to pay for medical costs that Medicare does not cover. However, you should do some math to figure out which plan is the best for you. Use this Medicare Plan Comparison Worksheet to weigh your options.
The Majority Of The Public Holds Favorable Views Of Medicaid

Public opinion polling suggests that Medicaid has broad support. Seven in ten Americans say they have ever had a connection with Medicaid including three in ten who were ever covered themselves. Even across political parties, majorities have a favorable opinion of Medicaid and say that the program is working well . In addition, polling shows that few Americans want decreases in federal Medicaid funding. In addition to broad-based support, Medicaid has very strong support among those who are disproportionately served by Medicaid including children with special health care needs, seniors, and people with disabilities.
Figure 10: Large Shares Across Parties Say They Have a Favorable Opinion of Medicaid
Read Also: Walk In Clinic Takes Medicaid
Special Enrollment Periods For Complex Situations
Some Special Enrollment Periods, like those due to misrepresentation or plan display error, gaining or maintaining status as a member of a federally recognized tribe or an Alaska Native Claim Settlement Act Corporation shareholder, or other very rare situations, dont limit your ability to choose a new plan during a Special Enrollment Period. Learn about Special Enrollment Periods for complex issues.
When Do I Have To Decide
Medicares annual open enrollment period is right around the corner. From Oct. 15 through Dec. 7, all those with Original Medicare, Medicare Advantage or Part D prescription drug coverage can switch plans. There is an additional opportunity for individuals enrolled in Medicare Advantage or prescription drug plans to switch to a 5-star rated Medicare Advantage plan or return to Original Medicare between Dec. 8 and Nov. 30.
Also, if you are approaching or already age 65 and still working, most employers offer a life event to transfer from your employer coverage at any time throughout the year if you enroll in Medicare Part B. This means you may be able to look at your Medicare options at any time.
Don’t Miss: How Quickly Can You Get Medicaid
What Changes Can I Make During Open Enrollment
Annual open enrollment is held in the fall. To make any of the changes below we must receive the required forms no later than the last day of open enrollment. The change will become effective January 1 of the next year.
- Change your medical or dental plans.
- Enroll or remove dependents.
The PEBB Program must receive the appropriate PEBB Continuation Coverage Election/Change or PEBB Continuation Coverage Election/Change form within the timelines. You may also make some changes using PEBB My Account.
For Redetermination Or Open Enrollment Questions
Need Help?
Blue Cross and Blue Shield of Illinois, a Division of Health Care Service Corporation, a Mutual Legal Reserve Company, an Independent Licensee of the Blue Cross and Blue Shield Association
PDF File is in portable document format . To view this file, you may need to install a PDF reader program. Most PDF readers are a free download. One option is Adobe® Reader® which has a built-in reader. Other Adobe accessibility tools and information can be downloaded at
External link You are leaving this website/app . This new site may be offered by a vendor or an independent third party. The site may also contain non-Medicare related information. In addition, some sites may require you to agree to their terms of use and privacy policy.
Also Check: Dentist In Newport News Va That Accept Medicaid
Social Security Work Incentives
Dont let concerns about SSI benefits stop you from encouraging your child to find an employment setting that is right for them. Parents of youth with disabilities are very aware of the importance of healthcare for their children. Many have heard that SSI recipients will lose their Medicaid coverage if they earn any money. As a result, some families discourage their young adults from joining the workforce. This is not true. Be aware that the Social Security Administration has Work Incentive programs that allow young adults with disabilities to continue to receive Medicaid coverage while they explore careers or attend postsecondary education or job training.
Make an informed choice. If your son or daughter receives SSI, contact a Work Incentives Planning and Assistance Project in your state to see how they can continue to receive health coverage through Medicaid while they work. WIPA projects are community-based organizations that receive grants from SSA to provide all Social Security and Supplemental Security Income disability beneficiaries with free work incentives planning and assistance.
WIPA services are available in every state, the District of Columbia, and the U.S. Territories of American Samoa, Guam, the Northern Mariana Islands, Puerto Rico, and the Virgin Islands. Call 1-866-968-7842 or 1-866-833-2967 for locations WIPA organizations or see the online SSA service provider directory.
Q How Much Income Can I Receive And Still Be Eligible For Medicaid
A. Income is money that you get from working, or money that someone gives you, or checks that you receive, such as a Social Security check, unemployment benefits, child support, retirement benefits, or sick pay. Whether your income level qualifies you or your family for Medicaid depends on the size of your family and the Medicaid program for which you are applying.
Income limits are set each year by the federal government to define the Federal Poverty Level for different family sizes. In general, if your household income is at or below the current 100% Federal Poverty Level for your household size, your family is likely to be eligible for Medicaid. Children from age 1 to under age 6 can qualify for Medicaid benefits when household income is at or below 133% of the Federal Poverty Level. Pregnant women and infants under age 1 qualify for Medicaid with family income at or below the 200% Federal Poverty Level, and pregnant women count as 2 family members.
See our tables of income limits for applying for DMMA programs to find out where your family income is, in relation to these income benchmarks.
Medical assistance programs other than Medicaid have different income level requirements. For example, uninsured children under age 19 who live in families with incomes at or below the 200% Federal Poverty Level are eligible for low cost health insurance under the Delaware Healthy Children Program.
Recommended Reading: Rehabs In Michigan That Accept Medicaid
Switching To A Spouses Policy During Open Enrollment
If you want to switch to a spouses health insurance policy during the annual open enrollment period, changing your coverage is easy. You simply need to cancel your current coverage and enroll in your spouses policy. If youre making the change to cut back on group health insurance costs, timing the change during open enrollment means you start saving right away.
Most organizations run their coverage with the calendar year. Open enrollment generally begins in November for coverage beginning January 1. Be sure to check that you and your spouses plans follow the same plan year with the same start date for changes made during open enrollment to avoid a gap in coverage.
If youre switching from group health insurance to a qualified small employer health reimbursement arrangement or an individual coverage HRA , your spouse must be enrolled in an individual or family policy before they can participate in the HRA on a tax-free basis.
Changing Your Health Insurance: Reasons Why You Might Want To

People choose to change their health insurance plans for all kinds of reasons. A few of the most common include:
- Changes in your plans network If your preferred doctors or specialists stop accepting your insurance, you could pay significantly more. Other health insurance options may help lower your overall medical bills.
- You need more or less coverage If, for example, you visit the doctor frequently and copays are eating into your budget, a different plan may help you keep medical expenses under control. On the other hand, if youre paying for top-tier coverage but dont often use it, a more modest plan could be a better fit.
- Moving to a new area, changes to your employment or your family These events are often good times to review your entire financial situation. Referred to as qualifying life events, theyre also times when youll be able to change your health insurance coverage.
No matter why you want to switch or make changes to your health insurance plans, there are two windows of opportunity when you can: Open Enrollment Period and a Special Enrollment Period.
Recommended Reading: How Do I Add Someone To My Medicaid
