Does Kentucky Help With My Medicare Premiums
Many Medicare beneficiaries who struggle to afford the cost of Medicare coverage are eligible for help through a Medicare Savings Program .
- Qualified Medicare Beneficiary pays for Part A and B cost sharing, Part B premiums, and Part A premiums . The income limit is $1,063 a month if single or $1,437 a month if married.
- Specified Low-Income Medicare Beneficiary pays for Part B premiums. The income limit is from QMB levels up to $1,276 a month if single or $1,724 a month if married.
- Qualified Individuals pays for Part B premiums. The income limit is from SLMB levels up to $1,436 a month if single or $1,940 a month if married.
- Qualified Disabled Working Individuals pays the Part A premiums owed by certain disabled beneficiaries who have returned to work. The income limit is 200 percent of the federal poverty level or $2,126 a month if living alone and $2,873 a month if living with one other person.
MSP asset limits: Kentucky uses federal asset limits for QMB, SLMB and QI: $7,860 if single and $11,800 if married. The QDWI asset limit is $4,000 if single and $6,000 if living with others.
Kentucky Medicaid Expansion Update
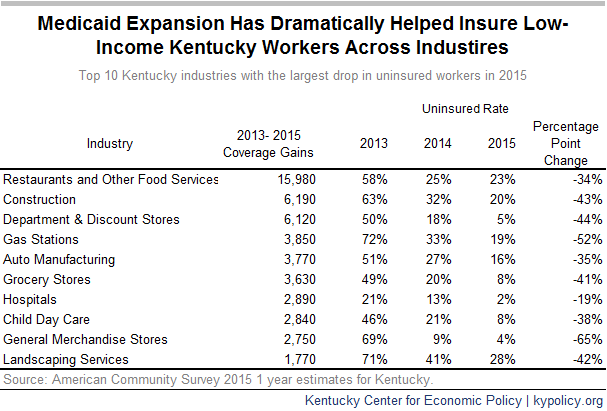
Kentucky has been one of the most successful states in reducing its uninsured rate through the Affordable Care Act .
Medicaid expansion in Kentucky was effective as of Jan. 1, 2014.
Kentuckys Medicaid work requirement was initially slated to take effect in July 2018.
However, Gov. Andy Beshear rescinded Kentuckys Medicaid work requirement.
Data collected by the Kentucky Cabinet for Health and Family Services shows that the new Medicaid beneficiaries are taking advantage of preventive screenings, with the following increases from 2013 to 2014:
- 30 percent increase in breast cancer screenings
- 3 percent increase in cervical cancer screenings
- 16 percent increase in colorectal cancer screening
- 37 percent increase in adult dental visits
According to the Center for Medicaid, as of July 2019, 450,700 Kentucky residents gained eligibility and gained health insurance coverage under the ACAs Medicaid expansion.
Kentucky Long Term Care
Kentucky is an income cap state, meaning that in order to be eligible for Medicaid long term care benefits there is a hard income limit. Non income cap states allow applicants to spend down money for their care, whereas income cap states require the amount to be no higher than their limit at time of application.
Also Check: Pregnancy Medicaid Ga Phone Number
Medicaid If You Have A Disability And Need A High Level Of Care
If you have a disability, but don’t qualify for SSI, 1619, or income-based Medicaid, you might still qualify for Medicaid benefits. This situation is most common for people who are elderly or have a disability and need the level of care that a nursing home or other institution offers. In this case, you may qualify for a Medicaid Waiver program, which would let you get the services you need to be able to live in your own home. Learn more about Medicaid Waiver programs.
Work Requirements Would Double The Number Of Adults Who Churn Off Medicaid In Kentucky
According to federal data, there were about 325,000 nondisabled adults ages 18 to 64 enrolled in Kentuckys Medicaid program in 201617.8 We estimate that prior to the implementation of work requirements, about 108,000 enrollees would be expected to leave Medicaid over a 24-month period . Of those, about 80,000 would either become uninsured and remain so or experience a gap in coverage .
If Kentucky were to implement work requirements, most of the 325,000 nondisabled adults enrolled in the program would have to demonstrate that they work at least 20 hours per week or engage in other activities, like looking for a job. Based on Arkansass experience, MEPS data, and estimates from Randy Haught and colleagues at Dobson, DaVanzo and Associates, about 108,000 people would likely lose Medicaid coverage as result of the work requirements over a 24-month period. Adding work requirements would thus increase the number of nondisabled adults churning off Medicaid in Kentucky from an estimated 108,000 adults to 216,000 a 100 percent increase.
Read Also: How Does A Person Get On Medicaid
Enrollment In Medicaid Is Dynamic
Insurance coverage in the United States is highly dynamic: people move in and out of employer coverage, individual coverage, Medicaid, and Medicare because of life changes as simple as a birthday, moving to a new city, getting a new job, or getting married. This phenomenon is often referred to as churn. Income eligibility rules in Medicaid supercharge this dynamic even a small change in income can make someone eligible or ineligible for benefits. If your income even temporarily ticks above the eligibility threshold for the Affordable Care Acts Medicaid expansion , you are no longer eligible for Medicaid.
Take seasonal farmworkers. They typically lack health insurance while they are working since they are unlikely to receive coverage from their employers. By working hard for several months at a time, they may lose Medicaid eligibility because their incomes rise above the threshold. When their seasonal work ends, their incomes may drop, making them again eligible for Medicaid.
Medicaid enrollees also face significant documentation requirements both at the time of enrollment and during reenrollment. Prior research by Benjamin Sommers has suggested that administrative barriers, particularly renewal, are likely a key reason adults become disenrolled from Medicaid.6
Recommendations For The Future Of Medicaid Expansion In Kentucky:
Download a PDF of this special report with references here.
Edited 9/16/2016 to reflect release of new data from the U.S. Census Bureau.
Recommended Reading: Where To Get Braces With Medicaid
Kentucky Has Accepted Federal Medicaid Expansion
- 1,597,263 Number of Kentuckians covered by Medicaid/CHIP as of November 2021
- 990,458 Increase in the number of Kentuckians covered by Medicaid/CHIP fall 2013 to October 2021
- 58% Reduction in the uninsured rate from 2010 to 2019
- 161% Increase in total Medicaid/CHIP enrollment in Kentucky since Medicaid expansion took effect
How Medicaid Eligibility Is Determined
Income eligibility is determined by your modified adjusted gross income , which is your taxable income, plus certain deductions. Those deductions include non-taxable Social Security benefits, individual retirement contributions and tax-exempt interest. For most people, MAGI is identical or very close to your adjusted taxable income, which you can find on your tax return. Specific income requirements in dollars rise alongside the size of your household.
Our guide focuses on each stateâs major programs for adults. Most are only available to state residents, U.S. citizens, permanent residents or legal immigrants .
Looking for insurance for a child? Check out our guide to the Children’s Health Insurance Program .
Read Also: South Carolina Medicaid Long Term Care
Dual Eligibile Medicare And Medicaid Plans In Kentucky
Did you know that you can get both Medicare and Medicaid benefits at the same time? You can qualify for Medicare if you are age 65 or older or if you have a qualifying disability such as End-Stage Renal Disease or Lou Gehrigs Disease.
If you arent sure whether or not you qualify for both Medicare and Medicaid, or to speak to a Medicare licensed agent about your options, either complete this form or call Medicare Plan Finder at 833-438-3676.
Medicaid Income Eligibility Chart State By State
The following is each of the states, listed alphabetically. Under your state of residence, you will find all of the relevant information regarding the Medicaid Income Eligibility Chart for each of three programs available: regular, in-home nursing care, and institutional nursing care.
Additionally, each of these programs will have additional information about the income limits for those who are single, married with both spouses applying, and married with only one spouse applying.
Don’t Miss: Who Gets Medicaid In Florida
How Does Medicaid Work In The State Of Kentucky
Kentucky Medicaid is a state and federal program authorized by Title XIX of the Social Security Act to provide health care for eligible low-income residents including children, families, pregnant women, the aged and the disabled. Eligibility is determined by a number of factors, including family size, income, and the federal poverty level.
What To Do If You Don’t Qualify For Medicaid
If you don’t qualify for Medicaid, you can possibly get subsidized health care through the Obamacare marketplaces during a special enrollment or open enrollment period. Americans who making more than 100% of the FPL qualify for a premium tax credit that can significantly lower the cost of a plan.
Federal open enrollment for 2022 health care plans runs until Jan. 15, 2022, though some state exchanges are open longer. Learn 2022 open enrollments dates by state. Healthcare.gov, the federal exchange, usually opens from November 1 to December 15 each year.
If you can’t find affordable health care on your marketplace during open enrollment, you have a few back-up options.
These include:
Short-term health insurance: Originally designed to prevent short-term health insurance gaps, these plans are cheaper, but much less comprehensive than traditional coverage. They don’t have to cover Obamacare’s 10 essential benefits or pre-existing conditions. Following changes by the Trump administration, short-term health plans can last from three months to potentially three years, though som estates have stricter limits.
Limited benefit plans: These plans cover a very small portion of the costs associated with certain “medical events,” like a doctor’s visit or ambulance ride. Both the number of events and dollar amounts covered are capped.
Don’t Miss: Does Medicaid Cover Ivf Treatment
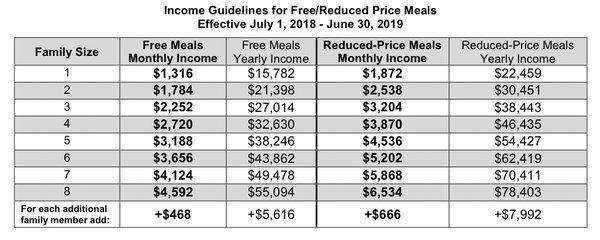
Is Your Income Low Enough For Income
These are the main income rules for income-based Medicaid:
- If your familys income is at or under 138% of the Federal Poverty Guidelines , you may qualify.
- If you are 18 or younger and your familys income is at or under 218% of FPG , you may qualify for Kentucky Children’s Health Insurance Program coverage.
- If you are pregnant and your familys income is at or under 195% of FPG , you may qualify. The unborn baby is counted as a family member.
Income-based Medicaid counts most types of earned and unearned income you have. However, some income is not counted, including Supplemental Security Income benefits and some contributions to retirement accounts. Learn more about what types of income affect income-based Medicaid eligibility.
Note: There are no limits to how much money or other resources you can have for income-based Medicaid.
Your family size:
|
If your income is low enough and you meet all other requirements, you should sign up for Medicaid.
You may see the income limit for income-based Medicaid listed as 133% of FPG in some places. However, when Medicaid counts your income, theyll knock 5% of FPG off your income if you make more than 133% of FPG. That’s why we say that you can make up to 138% of FPG, because it more accurately shows how much income you could have and still get Medicaid.
Work Requirements Would Increase The Number Of Adults In Kentucky Who Are Uninsured Or Experience A Coverage Gap By 118000
We used the MEPS data to simulate the coverage experience over a 24-month period of the adults who disenroll from Medicaid as a consequence of work requirements. We estimate that of the 108,000 adults who are expected to disenroll as a result of work requirements, 68,000 to 107,000 will experience a permanent coverage loss and 600 to 40,000 will experience a gap in coverage. The ranges reflect different assumptions about the degree to which people are able to regain Medicaid or gain private coverage .
We also use the MEPS data to estimate the effect of work requirements on people who disenroll from Medicaid for other reasons, such as income fluctuations. In Kentucky, of the 108,000 adults projected to disenroll for reasons other than work requirements, about 10,000 would be expected to regain Medicaid based on MEPS data. We include a scenario in which all members of this group regain Medicaid under work requirements and one in which none of this group would regain Medicaid.
Thus, as many as 118,000 people would either experience a permanent coverage loss or gap in coverage as a result of work requirements over a 24-month period. Depending on peoples ability to regain Medicaid or gain private coverage with work requirements in place, the number of adults who would remain uninsured at the end of the two-year period ranges from 77,500 to 117,400.
Don’t Miss: What Is Medicaid In Wisconsin
Do You Qualify For Ssi Or 1619
If you have a disability, low income, and low resources, you may qualify for SSI. If you already get SSI benefits, you automatically get Medicaid coverage and do not need to apply separately.
If you dont get SSI benefits yet, you should learn whether you might qualify by reading DB101s SSI article. At the same time, you should apply for Medicaid separately, because it can take Social Security months to review your SSI application and its important for you to have health coverage until then.
If you used to get SSI benefits, but stopped getting them after you started working, you may qualify automatically for Medicaid through a special rule called 1619 as long as your gross income is below $35,658 per year. Learn more about 1619 in DB101s SSI article.
If you do not get SSI benefits and do not qualify for 1619, income-based Medicaid might cover you.
Penalty Information In Kentucky For Medicaid
If a gift of any amount is given in Kentucky during a period of 5 years before applying to Medicaid, a penalty period will be initiated. This penalty period in Kentucky is called a look-back period and it can make an individual not eligible for Medicaid. Medicaid will not pay for care until the penalty period is over. The penalty is calculated by taking the total amount of any gifts given, and dividing it by $ 6,067, which creates a number of months before Medicaid kicks in.
The average cost of Nursing home care in Kentucky is $6,981, so penalties can become very costly for a family that has not planned appropriately for Medicaid.
Don’t Miss: How To Qualify For Medicaid
Who Is Eligible For Medicaid In Kentucky
Kentucky residents are eligible for Medicaid if they meet federal guidelines, including income and asset limits that are adjusted for the state. To be eligible for Kentucky Medicaid, you must live in the state and be a U.S. citizen, permanent resident or legal alien and lack the financial resources to pay for medically necessary care.
Beneficiaries must also be pregnant, over 65, blind, responsible for a child who is under 18 or have a disability or family member in the household with a disability. To qualify for Medicaid in Kentucky, adult applicants between the ages of 19 and 64 must earn less than 138% of the federal poverty level. The federal numbers are $12,800 a year for individual adults and $26,500 for a family of four in 2021, and the maximum qualifying incomes in Kentucky are $17,609 and $36,156, respectively.
Pregnant women must earn less than 200% of the federal poverty level or $25,520 a year for individuals and $52,400 for a family of four.
In Kentucky, children up to 12 months old are eligible for Medicaid or the Kentucky Childrens Health Insurance Program if their family earns less than 200% of the federal poverty level, or $52,400 annually for a family of four. For children ages 1 to 18, that figure is 147% of the federal poverty level or an estimated $38,517 a year for a family of four.
What Are The Medicaid Income Limits For 2022
Finding out if you are eligible for Medicaid can be quite a headache. Since Medicaid is jointly funded by federal and state governments, there are different eligibility criteria for each state! One of the biggest factors for Medicaid eligibility are the income limits.
If you are trying to learn more about whether your income is within the Medicaid income limit for your state of residence, then you are reading the right article!
I will be explaining which sources of monthly incoming money are considered income, how each state decides their income limit, and providing an easy-to-use list of each states income limits for the year 2022.
Read on to learn more about Medicaid income limits and determine if your income would be considered within the limit set by your state of residence!
Also Check: How Do I Get A Breast Pump Through Medicaid
What Are The Different Types Of Care Available
The Medicaid programs available in each state are: regular Medicaid, Medicaid for long-term nursing home care, and Medicaid for home-based nursing care.
Regular Medicaid is the health care benefits program available to all of a states residents, providing they meet the eligibility requirements. Some of the eligibility requirements include:
- Low-income
- Legal status on the United States
- Resident of the state of application
Those who meet these criteria are able to use their regular Medicaid benefits for their doctors visits, hospital care, laboratory testing, and transportation for medical purposes.
The income limit for regular medicaid will be a set amount, depending on state and marital status. Some states allow one lump sum for a married couple and others have an income limit per spouse.
Medicaid for long-term nursing home care is for those who are elderly and can no longer live independently, those with chronic illness, and people with disabilities. At the facility, the residents receive 24/7 supervision and medical care, as well as lodgings and meals.
All state residents who meet the eligibility criteria and require long-term nursing home care are entitled to and will receive the care. There are no waitlists or lotteries for this benefit and you cant be denied if you meet the eligibility requirements.
