Where Can Medicare Beneficiaries Get Help In Ohio
Ohio Senior Health Insurance Information Program
You can access free counseling about Medicare benefits through the Ohio Senior Health Insurance Information Program at 800-686-1578.
The OSHIIP can help you enroll in Medicare, compare and change Medicare Advantage and Part D plans, and answer questions about state Medigap protections. OSHIIP counselors may also be able to provide referrals for local home care or long-term care services. This website has more information about the services OSHIIP offers.
Elder law attorneys
Elder law attorneys can help individuals plan for Medicaid long-term care benefits. You can use this National Academy of Elder Law Attorneys search feature to find an elder attorney locally.
How To Qualify For Medicaid
Almost every state has multiple Medicaid programs. But, as a good rule of thumb, if you make less than 100% to 200% of the federal poverty level and are pregnant, elderly, disabled, a parent/caretaker or a child, theres likely a program for you. And if you make less than 133% of the FPL**, theres possibly a program for you, depending on whether your state expanded Medicaid under Obamacare. In 2021, the federal poverty levels range from $12,880 to $44,660 .
In 2021, the federal poverty level in Alaska ranges from $ $16,090 to $55,850 . The federal poverty level in Hawaii ranges from $14,820 to $51,360 .
Find A $0 Premium Medicare Advantage Plan Today
For California residents, CA-Do Not Sell My Personal Info, .
MedicareAdvantage.com is a website owned and operated by TZ Insurance Solutions LLC. TZ Insurance Solutions LLC and TruBridge, Inc. represent Medicare Advantage Organizations and Prescription Drug Plans having Medicare contracts enrollment in any plan depends upon contract renewal.
The purpose of this communication is the solicitation of insurance. Callers will be directed to a licensed insurance agent with TZ Insurance Solutions LLC, TruBridge, Inc. and/or a third-party partner who can provide more information about Medicare Advantage Plans offered by one or several Medicare-contracted carrier. TZ Insurance Solutions LLC, TruBridge, Inc., and the licensed sales agents that may call you are not connected with or endorsed by the U.S. Government or the federal Medicare program.
Plan availability varies by region and state. For a complete list of available plans, please contact 1-800-MEDICARE , 24 hours a day/7 days a week or consult www.medicare.gov.
Medicare has neither reviewed nor endorsed this information.
Don’t Miss: Does Medicaid Cover All Pregnancy Costs
Ohio Medicaid Eligibility Requirements
To qualify for long-term care benefits through Medicaid in Ohio, a person must meet the states financial and medical eligibility requirements. Many seniors choose to reside in a nursing home or receive other types of long-term care without a doctor ordering them to do so, and Medicaid will not cover any voluntary care services. An applicant must prove they require the care they want Medicaid to cover before they may receive benefits. Additionally, they must prove they cannot pay their medical bills alone and require financial assistance to receive care.
Is It Hard To Qualify For Medicaid
As long as you meet the eligibility rules in your state, it is not hard to qualify for Medicaid. After all, almost 74 million Americans are covered by the program.
Contact your state Medicaid program in order to apply for Medicaid. Applications are generally reviewed and approved within 90 days and typically are reviewed sooner.
Also Check: Doctors That Take Medicaid For Adults
Medicaids Rules For Immigrants:
- Undocumented immigrants do not qualify for full Medicaid coverage, but they may qualify for Medicaid coverage for emergency services.
- Most immigrants who have been lawfully present for less than five years do not qualify for full Medicaid coverage. However, they may qualify for private coverage subsidized by the government.
- Immigrants who have been lawfully present for five years or longer and some other noncitizens who meet specific noncitizen requirementsqualify for all of the same programs that U.S. citizens can get.
Asset Requirements & Limits
Ohio Medicaid for long-term care requires all applicants to demonstrate financial need in order to receive benefits. To determine a persons financial eligibility, Medicaid takes their resources into consideration. Medicaid expects applicants to liquidate their assets to pay for their care, and will not step in until their resources fall within the asset value requirements.
The asset limit in Ohio for a single Medicaid applicant is $2,000. Married applicants are subject to different limits, which are determined on a case-by-case basis. Assets are considered jointly, and if a Medicaid applicants spouse intends to continue living independently , they may keep a portion of the couples assets to protect them from spousal impoverishment. The amount of assets the spouse may keep is known as the Community Spouse Resource Allowance .
Medicaid divides assets into two categories: countable, and exempt. Countable assets are those which count toward a persons asset limit, including stocks, bonds, and annuities. Exempt assets are not available for Medicaids consideration, and will not count toward a persons asset limits. Medicaid does not expect a person to liquidate their exempt assets to pay for their long-term care, however they do expect all countable assets in excess of $2,000 to be put toward care costs.
Don’t Miss: Medicaid Eligibility Income Chart Florida
How Much Does Medicaid Cost In Ohio
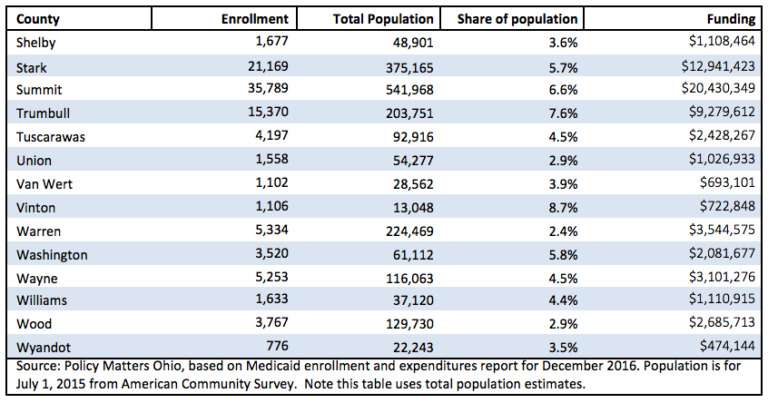
More than $21 billion gets spent on Ohio Medicaid costs. The federal government shares these expenses with the state, with Ohio allocating over 37 percent of their budget to its funding. This amount will only grow over time, as there are plans to expand the program to ensure more people who need coverage can receive it.
What To Do If You Don’t Qualify For Medicaid
If you don’t qualify for Medicaid, you can possibly get subsidized health care through the Obamacare marketplaces during a special enrollment or open enrollment period. Americans who making more than 100% of the FPL qualify for a premium tax credit that can significantly lower the cost of a plan.
Federal open enrollment for 2022 health care plans runs until Jan. 15, 2022, though some state exchanges are open longer. Learn 2022 open enrollments dates by state. Healthcare.gov, the federal exchange, usually opens from November 1 to December 15 each year.
If you can’t find affordable health care on your marketplace during open enrollment, you have a few back-up options.
These include:
Short-term health insurance: Originally designed to prevent short-term health insurance gaps, these plans are cheaper, but much less comprehensive than traditional coverage. They don’t have to cover Obamacare’s 10 essential benefits or pre-existing conditions. Following changes by the Trump administration, short-term health plans can last from three months to potentially three years, though som estates have stricter limits.
Limited benefit plans: These plans cover a very small portion of the costs associated with certain “medical events,” like a doctor’s visit or ambulance ride. Both the number of events and dollar amounts covered are capped.
Prescription discount cards: While these cards won’t help you pay for inpatient or outpatient care, they do help you get medication at discounted rates.
Don’t Miss: How To Find Your Medicaid Number
Where Can I Apply For Medicaid In Ohio
Medicaid is administered by the State Department of Medicaid in Ohio. You can apply for Medicaid or an MSP using this website or by visiting a county Job and Family Services office.
Josh Schultz has a strong background in Medicare and the Affordable Care Act. He coordinated a Medicare ombudsman contract at the Medicare Rights Center in Ohio City, and represented clients in extensive Medicare claims and appeals. In addition to advocacy work, Josh helped implement federal and state health insurance exchanges at the technology firm hCentive. He has also held consulting roles, including at Sachs Policy Group, where he worked with hospital, insurer and technology clients.
I Introduction To Medicaid Guide
Do you know someone who has spent time in a nursing home? Have you ever thought it could be you?
Most people answer the first question yes, and the second question no. It is one of those situations where we believe it could never happen to me. However, studies show that approximately 70% of those age 65 or older will need some type of long-term care prior to death. By 2020, an estimated 12 million older Americans will need some form of long-term care.
Recommended Reading: Can I Have Medicare And Medicaid Together
Medicaid If You Are 18 Or Younger
If you are 18 or younger, you may qualify for income-based Medicaid if your familys income is 211% of the Federal Poverty Guidelines or less . It doesn’t matter how much your family has in resources or whether you have a disability. Note: Income-based Medicaid for children 18 and younger is sometimes called “Healthy Start.”
Check whether your family’s income is low enough for you to get income-based Medicaid:
Your family size:| Income limits for your family: | |
| $12,880 | |
| Income-based Medicaid, adults | |
| Income-based Medicaid, children | |
| Subsidized private plans, reduced fees | |
| Subsidized private plans | — |
If your family’s income is at or below the limit for a program, you may qualify if you meet other program rules.Notes:
|
Note: Some young people with disabilities who don’t get SSI and don’t qualify for income-based Medicaid may still qualify for disability-based Medicaid. If you have any questions about this, talk to a benefits planner.
Medicaid Eligibility In Ohio
Funded by both the federal and state government, the health insurance program known as Medicaid was designed with low-income families in mind. Children, elderly, and disabled members of society are often first among the list of eligible applicants in the state of Ohio. Before applying, it is important to note the states specific criteria for getting approved and accepted into the program to receive coverage.
Don’t Miss: Medicaid Ga Number Customer Service
Who Qualifies For Medicaid
In all but 13 states, adults who make below a certain income may qualify for Medicaid. In all states, Medicaid is available to people who make a low income and also meet other criteria such as being at least 65 years old, disabled, pregnant or other qualifications.
Each state runs its own Medicaid programs with its own set of qualifying criteria.
How Do You Calculate Your Medicaid Income Eligibility
Follow these steps to calculate whether or not your income may qualify you for Medicaid:
- Find the FPL for your household using the chart above
- Multiply that number by your states Medicaid income limit found below, and then divide by 100
For example, if there are two people living in your household and you live in Arizona, you would multiply $17,420 by 138 and then divide by 100. That equals $24,039.60.
You may also multiply $17,420 by 1.38.
Don’t Miss: Child Counselors That Accept Medicaid
Are There Options If I Make More Than The Limit
There might be some options to still receive Medicaid benefits if you make more than the income limit in your state.
The options do differ from state to state, but the majority do offer a pathway for those who would be considered medically needy and have high medical expenses.
If someone who requires a lot of medical care has too high of an income, they might be able to spend that income on their medical costs and then have that count against their income.
For example, if someone was $500 over the income limit in their state and that state has a program for the medically needy, they might be permitted to spend that excess income on their medical expenses and then receive Medicaid benefits after. This helps those with high than average medical costs be put on more equal footing for income eligibility requirements.
Not every state offers this particular program, however. For a great resource on the sorts of waivers, exceptions, and other eligibility information, visit this website. Once you click on your state of residence, you should be able to see which waivers are available in your state for those who exceed the income limit.
Do You Qualify For Ssi Or 1619
If you have a disability, low income, and low resources, you may qualify for SSI. If you already get SSI benefits, you automatically get Medicaid coverage and do not need to apply separately.
If you dont get SSI benefits yet, you should learn whether you might qualify by reading DB101s SSI article. At the same time, you should apply for Medicaid separately, because it can take Social Security several months to review your SSI application and its important for you to have health coverage until then.
If you used to get SSI benefits, but stopped getting them after you started working, you may qualify automatically for Medicaid through a special rule called 1619 as long as your gross income is below $40,078 per year. Learn more about 1619 in DB101s SSI article.
If you do not get SSI benefits and do not qualify for 1619, income-based Medicaid might cover you.
Read Also: How To Access Medicaid Card Online
Schedule A Nursing Home Asset Protection Consultation
We are here to help if you would like to develop a nursing home asset protection strategy.
If you establish a Medicaid trust, you can receive distributions of the trusts earnings while you are independent, and the principal wouldnt count if and when you apply for Medicaid. This can be a great way to cover all your bases so you can go forward with peace of mind.
You can schedule an appointment at our Cincinnati elder law office if you call us at 513-721-1513, and you can use our contact form if you would rather send us a message.
What Is The Highest Income To Qualify For Medicaid
Washington D.C. has the highest allowable income to qualify for Medicaid, at 215% of the FPL for individuals and 221% for a family of three.
That means an individual in Washington D.C. can make up to $27,692 per year and still be eligible for Medicaid. Washington D.C.s high cost of living factors into its higher income limit for Medicaid. No other state uses more than the standard 138% limit for individuals.
A family of three can make up to $48,531.60 and still qualify for Medicaid in Washington D.C. Connecticut is the only other state to use a limit higher than 138%.
Recommended Reading: Inpatient Drug Rehab Illinois Medicaid
More Ways To Qualify For Medicaid If You Have A Disability
If you have a disability, but don’t qualify for SSI, 1619, or income-based Medicaid, you might still qualify for Medicaid benefits if:
For help with your application, visit or call your local County Department of Job and Family Services office or call the Ohio Medicaid Consumer Hotline at 1-800-324-8680 or 1-800-292-3572 .
What Counts As Income
The monthly financial amount that you receive from employment wages, benefits from Social Security, payments from a pension plan. Alimony, and payouts from stocks, IRAs, and other investment returns.
Mostly likely, if it is a form of money that you receive monthly, then it would count as income. However, if you are not sure about one of your sources of money, it is always better to err on the side of caution and check with your Medicaid program coordinators.
For applicants who are single or divorced, these monthly amounts are simply added up and the total number is the amount you can compare to the income eligibility limits in your state of residence. If it matches or is less than the limit for your state, you should be able to receive Medicaid health care benefits.
For applicants who are married, the protocol for evaluating income limit can differ depending on which state you reside in.
Most states have either one limit amount that each spouse can contribute to asymmetrically or a limit amount where each spouse can only make up one half of the total. Also, there are a few states where you are considered a single applicant, regardless of marital status.
There are also cases where you are married, but only one spouse is applying for Medicaid benefits. Again, the protocol will differ depending on the state of your residence. Most states will either treat the spouse applying as a single applicant or will consider their income limit as a married applicant.
Don’t Miss: If I Have Medicaid Do I Qualify For Food Stamps
Lawmakers Voted To Freeze Medicaid Expansion In 2017 Kasich Vetoed
Lawmakers in Ohio came to a compromise on their budget bill on in June 2017 and sent it to Governor Kasich, who had just two days to review it before the June 30 deadline for the state to enact the budget for the 2018 fiscal year, which began July 1, 2017. The Senates version of the bill had included a freeze on new Medicaid expansion enrollments after July 1, 2018, and that provision remained in the bill after it went through the conference committee process to reconcile the differences between the House and Senate versions of the budget.
Kasich had noted that the Medicaid expansion freeze would result in 500,000 people losing coverage in the first 18 months, since people would lose coverage if their income increased and would then be unable to get back on Medicaid if their income subsequently decreased .
Kasich used his line-item veto power to eliminate the Medicaid expansion freeze, and he also vetoed a provision that would have required Medicaid expansion enrollees to pay monthly premiums for their coverage. Monthly premiums for Medicaid expansion populations require approval from CMS the Obama Administration only approved limited premium requirements, and had rejected a more far-reaching premium requirement that Ohio had proposed in 2016 . But the Trump Administration has made it easier for states to impose these types of requirements on Medicaid expansion enrollees.
