Additional Cares Act Funding
On March 27, 2020, former President Donald Trump signed the CARES Acta $2 trillion coronavirus emergency relief packageinto law. A sizable chunk of those funds$100 billionwas earmarked for healthcare providers and suppliers, including those that are Medicare and Medicaid enrolled for expenses related to COVID-19.
Below are some examples of what the additional funding covers:
- A 20% increase in Medicare payments to hospitals for COVID-19 patients.
- A scheduled payment reduction was eliminated for hospitals treating Medicare patients from May 1, 2020, through Dec. 31, 2020.
- An increase in Medicaid funds for states.
How To Apply For Medicaid In In Ohio
Multiple methods exist for applying for Ohio Medicaid. Many people have taken to the online version which is fast to use and initiates a quick response. A pop-up window comes on the screen when attempting to start a new application. It allows users to either sign in with an existing account or create an account if it is their first time. Provide a first and last name, date of birth, and social security number to sign up and start the process.
Those who do not wish to use the online version may instead visit their local office to fill out a paper form. It can get submitted directly to a worker who can assess the information and approve or deny the claim. It is also possible to apply by telephone by calling the Ohio Medicaid Consumer Hotline at 324-8680.
Also Check: Can I Get Medicaid For Pregnancy If I Have Insurance
Why Are Letters Going Out Now
Two reasons. First, we want to give everyone impacted by this cut as much notice as possible in order to make plans for such a change and begin the process of seeing if individuals may be eligible for other services. We know from speaking with some individuals and their families already that explaining these complex reductions can take time.
Second, because of federally required timelines and approval processes, we must start the public notice step of rulemaking, CMS notification and their approval process. This could be lengthy. We believe it to be responsible to explain to enrollees what that public notice means, provide advice on applying for other available programs, and how to contact us if they have questions.
You May Like: Do I Have To Pay For Medicaid
Recommended Reading: If You Have Medicaid Do You Need Medicare Part B
Does Medicaid Pay Secondary To Medicare Advantage Plans
Medicaid is always the secondary payer when it comes to health insurance, says Watts.
Medicaid never pays first for services covered by Medicare. Instead, it pays for whatever isnt covered by Medicare. Medicaid may also cover some drugs and additional services that the Medicare Advantage plan doesnt cover fully or at all.
Medicaid is a great benefit for consumers who are eligible, says Watts. However, if you dont meet the criteria, he recommends looking into other avenues of help that may be available. For instance, if you dont qualify for Medicaid, you may qualify for a Low Income Subsidy . LIS helps cover prescription card costs, and pays for a portion of your drugs as well, says Watts.
Some states like New York may have pharmacy assistance programs, as well as additional help from private drug companies.
How To Apply For Medicaid
If youâre eligible for Medicaid, you can apply all year round through your states Medicaid website or HealthCare.gov, the federal health insurance marketplace. If you apply for Medicaid through Healthcare.gov and it looks like you qualify, the federal government will notify your state agency, which will contact you about enrollment. States also generally let you print out paper applications you can mail, fax or return directly to your local government office.
To complete your Medicaid application, you will likely need to provide documentation that you meet your states requirements. This documentation may include:
-
Your birth certificate or drivers license to serve as proof of age and citizenship
-
Recent pay stubs or tax returns to serve as proof of income
-
Copies of bank statements
-
Proof of address, which could include a lease, utility bill statements or a copy of your mortgage
-
Medical records to serve as proof of disability
States have 45 days to process your Medicaid application. They have 90 days if eligibility is tied to a disability . Processing can take longer if applicants do not supply all of the required documentation. If you dont qualify for Medicaid, you might be able to get subsidized health insurance through Healthcare.gov. However, only certain life events allow you to apply for a marketplace health care plan outside of open enrollment, which takes place from Nov. 1 to Jan. 15.
Free in your inbox each Friday.
Sign up now
Also Check: Therapists Rochester Ny Accept Medicaid
The Difference Between Medicare And Medicaid And How People Can Get The Best Care
Medicare and Medicaid are two of the most important health insurance programs in the United States. They provide coverage for people over the age of 65, people with disabilities, and low-income families. Medicare is a government program, while Medicaid is a program run by the states.
Contents
Read Also: Medicaid Requirements For Gastric Sleeve
What Medicaid Covers For Medicare Enrollees
Medicare has four basic forms of coverage:
- Part A: Pays for hospitalization costs
- Part B: Pays for physician services, lab and x-ray services, durable medical equipment, and outpatient and other services
- Part C: Medicare Advantage Plan offered by private companies approved by Medicare
- Part D: Assists with the cost of prescription drugs
Medicare enrollees who have limited income and resources may get help paying for their premiums and out-of-pocket medical expenses from Medicaid . Medicaid also covers additional services beyond those provided under Medicare, including nursing facility care beyond the 100-day limit or skilled nursing facility care that Medicare covers, prescription drugs, eyeglasses, and hearing aids. Services covered by both programs are first paid by Medicare with Medicaid filling in the difference up to the state’s payment limit.
Read Also: How Do I Pay My Medicaid Spend Down
Q How Do I Join A Managed Care Organization
A. After being notified that you are eligible for Medicaid , you will receive in the mail a packet of information about the different MCO plan options for receiving your Medicaid benefits. You may choose any plan described in this mailing. You probably want to choose a Managed Care Organization to which your doctor belongs. If you need help making this decision, call the Health Benefit Manager at the phone number in the mailing.
When Does Medicaid End For A Child In Virginia
There are many situations when people may need Medicaid to help with medical costs. Perhaps the most common situation involves children who are eligible for Medicaid if they have a household income below the federal poverty level. A child will no longer be eligible for Medicaid in Virginia if they exceed these limits. The Virginia Medicaid program will continue coverage until the child turns 19 years old.
You May Like: Do Newborns Automatically Get Medicaid
Recommended Reading: Does Medicaid Cover Medical Alert Systems
How To Apply For Medicaid In Texas
You can apply online for benefits. You will need to be prepared to answer questions about the following for each family member:
- Social Security number and birth date
- Citizenship or immigration status
- Money from jobs and other sources
- The value of cars and other property
- Costs you pay for bills
You can also call 211 if you are in Texas. Alternatively, you can dial 1-877-541-7905 Monday to Friday, 8 a.m. to 6 p.m.
You can also visit a community partner in person. Printing and mailing a copy to HHS is also an option
Read Also: Dc Medicaid Customer Service Number
Find A $0 Premium Medicare Advantage Plan Today
For California residents, CA-Do Not Sell My Personal Info, .
MedicareAdvantage.com is a website owned and operated by TZ Insurance Solutions LLC. TZ Insurance Solutions LLC and TruBridge, Inc. represent Medicare Advantage Organizations and Prescription Drug Plans having Medicare contracts enrollment in any plan depends upon contract renewal.
The purpose of this communication is the solicitation of insurance. Callers will be directed to a licensed insurance agent with TZ Insurance Solutions LLC, TruBridge, Inc. and/or a third-party partner who can provide more information about Medicare Advantage Plans offered by one or several Medicare-contracted carrier. TZ Insurance Solutions LLC, TruBridge, Inc., and the licensed sales agents that may call you are not connected with or endorsed by the U.S. Government or the federal Medicare program.
Plan availability varies by region and state. For a complete list of available plans, please contact 1-800-MEDICARE , 24 hours a day/7 days a week or consult www.medicare.gov.
Medicare has neither reviewed nor endorsed this information.
Read Also: Does Nc Medicaid Cover Chiropractic
Medicaid Eligibility: Older Adults And Individuals With Disabilities
Medicaid is a joint federal-state program that finances the delivery of primary and acute medical services, as well as long-term services and supports , to a diverse low-income population. In general, individuals qualify for Medicaid coverage by meeting the requirements of a specific eligibility pathway. An eligibility pathway is the federal statutory reference that extends Medicaid coverage to certain groups of individuals.
Each eligibility pathway specifies the group of individuals covered by the pathway . It also specifies the financial requirements applicable to the group , including income and, sometimes, resources . In addition, an eligibility pathway often dictates the services that individuals are entitled to under Medicaid. Some eligibility groups are mandatory, meaning all states with a Medicaid program must cover them other eligibility groups are optional.
This report focuses on the ways in which adults aged 65 and older and individuals with disabilities qualify for Medicaid based on their age or disability status that is, the eligibility pathways where the categorical criteria are being aged, blind, or disabled . Individuals who qualify for Medicaid on the basis of being blind or disabled include adults under the age of 65 as well as children. Generally, ABD populations qualify for Medicaid through an eligibility pathway under one of two broad coverage groups described in this report: Supplemental Security Income -Related Pathways and Other ABD Pathways.
Most Medicaid Enrollees Get Care Through Private Managed Care Plans

Over two-thirds of Medicaid beneficiaries are enrolled in private managed care plans that contract with states to provide comprehensive services, and others receive their care in the fee-for-service system . Managed care plans are responsible for ensuring access to Medicaid services through their networks of providers and are at financial risk for their costs. In the past, states limited managed care to children and families, but they are increasingly expanding managed care to individuals with complex needs. Close to half the states now cover long-term services and supports through risk-based managed care arrangements. Most states are engaged in a variety of delivery system and payment reforms to control costs and improve quality including implementation of patient-centered medical homes, better integration of physical and behavioral health care, and development of value-based purchasing approaches that tie Medicaid provider payments to health outcomes and other performance metrics. Community health centers are a key source of primary care, and safety-net hospitals, including public hospitals and academic medical centers, provide a lot of emergency and inpatient hospital care for Medicaid enrollees.
Figure 6: Over two-thirds of all Medicaid beneficiaries receive their care in comprehensive risk-based MCOs.
Don’t Miss: Pediatricians In Amarillo Tx That Accept Medicaid
I Have Ssdi Does That Qualify Me What Is The Difference Between Ssi And Ssdi
Social Security Disability Income is not the same as Supplemental Security Income . SSDI is based on an individuals earnings record. Whereas, Supplemental Security Income serves the needy and eligibility is based on having limited income and resources. It is possible for an individual to qualify for both SSDI and SSI benefits but you must apply for SSI with the Social Security Administration to retain Medicaid eligibility if there are budget cuts to these programs. Having SSDI will not maintain your eligibility.
Dont Miss: Does Medicaid Cover Long Term Care Facilities
What Is The Texas Health Information Counseling And Advocacy Program
If you are eligible for Medicare, the Texas’ Health Information, Counseling and Advocacy Program can help you enroll, find information and provide counseling about your options. This partnership between the Texas Health and Human Services system, Texas Legal Services Center and the Area Agencies on Aging trains and oversees certified benefits counselors across the state.
Don’t Miss: How To Qualify For Medicaid In Utah
Medicare And Medicaid Costs
Medicare is administered by the Centers for Medicare & Medicaid Services , a component of the Department of Health and Human Services. CMS works alongside the Department of Labor and the U.S. Treasury to enact insurance reform. The Social Security Administration determines eligibility and coverage levels.
Medicaid, on the other hand, is administered at the state level. Although all states participate in the program, they aren’t required to do so. The Affordable Care Act increased the cost to taxpayersparticularly those in the top tax bracketsby extending medical coverage to more Americans.
According to the most recent data available from the CMS, national healthcare expenditure grew 9.7% to $4.1 trillion in 2020. That’s $12,530 per person. This figure accounted for 19.7% of gross domestic product that year. If we look at each program individually, Medicare spending grew 3.5% to $829.5 billion in 2020, which is 20% of total NHE, while Medicaid spending grew 9.2% to $671.2 billion in 2020, which is 16% of total NHE.
Services That Medicare Does Not Provide
If Medicare does not cover a medical expense or service, a person may wish to take out a Medigap plan for supplemental coverage.
Private companies also offer Medigap plans. Depending on the individual plan, Medigap may cover:
- copayments
- deductibles
- care outside of the U.S.
If a person has a Medigap policy, Medicare will first pay their eligible portion. Afterward, Medigap will pay the rest.
To have a Medigap policy, a person must have both Medicare Parts A and B and pay a monthly premium.
Medigap policies do not cover prescription drugs, which a Part D plan covers.
An individual must be one of the following to be eligible for Medicare:
- age over 65 years
- age under 65 years and living with a disability
- any age with end stage renal disease or permanent kidney failure needing dialysis or transplant
They must also be:
- a U.S. citizen or permanent legal resident for 5 years continuously
- eligible for Social Security benefits with at least 10 years of contributing payment
Don’t Miss: Medicaid Office Panama City Fl
Medicaid Eligibility In Maryland
Medicaid is a nationwide program that provides free and/or affordable health care coverage for millions of citizens including children, expectant mothers, seniors, individuals with disabilities, and low-income families. Benefits include primary care, prescription, dental, eye care, hospitalizations, specialized care, and mental health services.
Also Check: How Do I Add Someone To My Medicaid
Medicaid Covers A Broad Range Of Health And Long
Medicaid covers a broad range of services to address the diverse needs of the populations it serves . In addition to covering the services required by federal Medicaid law, many states elect to cover optional services such as prescription drugs, physical therapy, eyeglasses, and dental care. Coverage for Medicaid expansion adults contains the ACAs ten essential health benefits which include preventive services and expanded mental health and substance use treatment services. Medicaid plays an important role in addressing the opioid epidemic and more broadly in connecting Medicaid beneficiaries to behavioral health services. Medicaid provides comprehensive benefits for children, known as Early Periodic Screening Diagnosis and Treatment services. EPSDT is especially important for children with disabilities because private insurance is often inadequate to meet their needs. Unlike commercial health insurance and Medicare, Medicaid also covers long-term care including both nursing home care and many home and community-based long-term services and supports. More than half of all Medicaid spending for long-term care is now for services provided in the home or community that enable seniors and people with disabilities to live independently rather than in institutions.
Figure 5: Medicaids benefits reflect the needs of the population it serves.
Don’t Miss: Chiropractors That Accept Medicaid In Louisiana
More Resources For Medicare Beneficiaries
When approaching the age to qualify for Medicare benefits, visit the official Social Security Administration Medicare website to determine your eligibility and calculate your premium. In the meantime, read more about when and how to apply for Medicare and visit medicare.gov to prepare for when that time comes.
Differences In Medicare Vs Medicaid

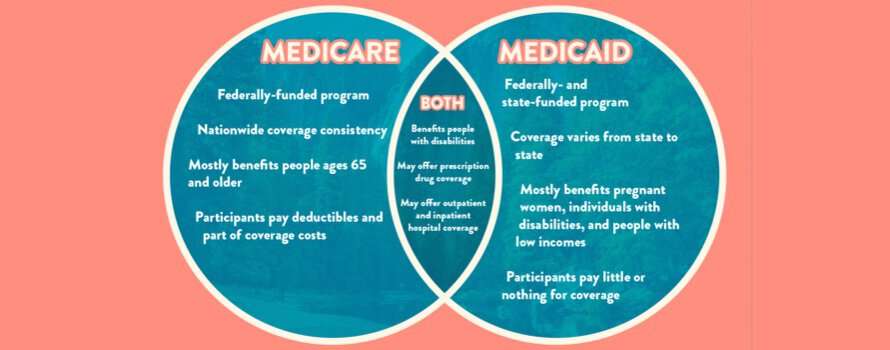
Medicare and Medicaid are both health insurance programs offered to U.S. citizens and permanent residents. However, there are two key differences between the two programs: coverage and the types of services that are eligible for reimbursement. Below you can see the Medicare vs. Medicaid chart which outlines all the differences in the policies.
| Medicare |
|---|
| Federal and state governments |
You May Like: If I Have Medicaid Do I Qualify For Food Stamps
Are You Eligible For Medicaid
Wondering if you could qualify for Medicaid? One of the main criteria used to determine eligibility is your level of income. If you dont have income over the federal poverty level and have limited assets, depending on your specific circumstances and the state in which you reside, you may qualify for some level of Medicaid coverage.
Keep in mind, however, that there are different categories of eligibilityâand each category has its own unique set of requirements. For example, the eligibility requirements for a pregnant woman may not be the same as that of a disabled person.
Recommended Reading: Kansas Nursing Homes That Accept Medicaid
If Your Income Is Low And Your State Hasnt Expanded Medicaid
If your state hasnt expanded Medicaid, your income is below the federal poverty level, and you dont qualify for Medicaid under your states current rules, you wont qualify for either health insurance savings program: Medicaid coverage or savings on a private health plan bought through the Marketplace.
- Find out why
-
- When the health care law was passed, it required states to provide Medicaid coverage for all adults 18 to 65 with incomes up to 133% of the federal poverty level, regardless of their age, family status, or health.
- The law also provides premium tax credits for people with incomes between 100% and 400% of the federal poverty level to buy private insurance plans in the Health Insurance Marketplace®.
- The U.S. Supreme Court later ruled that the Medicaid expansion is voluntary with states. As a result, some states havent expanded their Medicaid programs.
- Adults in those states with incomes below 100% of the federal poverty level, and who dont qualify for Medicaid based on disability, age, or other factors, fall into a gap.
- Their incomes are too high to qualify for Medicaid in their states.
- Their incomes are below the range the law set for savings on a Marketplace insurance plan.
-
States are continuing to make coverage decisions. They could expand Medicaid in the future.
You May Like: Mental Health Places That Accept Medicaid
