Member Advisory Council And Connected Advisors
UnitedHealthcare Care Managers for Member’s Unique Needs
Every UnitedHealthcare MyCare Ohio member receives a personal representative. These Care Managers are licensed professionals providing education and coordination of UnitedHealthcare Connected® for MyCare Ohio benefits, tailored for each member’s unique needs.
to watch a video on how these Care Managers are helping current members.
We recently mailed you a letter that included some information on benefit changes. Some of the information did not pertain to members that only have their Medicaid covered benefits through our plan. Please disregard that letter. The letter also had an incorrect number for the Ohio Medicaid Hotline. The correct number for the Hotline is 1-800-324-8680. We are sorry for any confusion this may have caused you. Please view the Member Clarification Letter for additional information.
Use the documents below to learn more about each important health topic.
-
PDF 180.50KB – Last Updated: 11/12/2020
UnitedHealthcare Member Advisory Council and “Connected Advisors”
UnitedHealthcare Member Advisory Council and “Connected Advisors” is an advisory council to ensure that UnitedHealthcare actively engages consumers, families, advocacy groups, and other key stakeholders as partners in the program design and delivery system.
Who is involved?
They will advise and guide the UnitedHealthcare Community Plan of Ohio on:
How is it organized?
What will they do?
-
PDF 26.62KB – Last Updated: 11/12/2020
To Qualify For The Medicare Premium Assistance Program Applicants Must:
- Be eligible for Medicare
- Have or get a social security number and
- Meet certain financial requirements
When applying for MPAP, proof of income, resources, age or disability, citizenship and other health insurance is required. No face-to-face interview with the local county department of job and family services is necessary. Applicants can ask an authorized representative to apply on their behalf.
About The Dayton Ohio Medicaid Office
The Dayton Ohio Medicaid Office, located in Dayton, OH, administers the Medicaid program and the Children’s Health Insurance Program , in Dayton. Medicaid and CHIP are federally-funded health insurance programs for low-income individuals, families, and children. Medicaid also provides health insurance to high-risk populations, including people with disabilities and low-income elder care residents.
You may contact the Medicaid Office for questions about:
- Dayton Medicaid benefits
- Applying for Medicaid in Dayton
- Dayton healthcare and prescription drug plans
- Doctors and dentists that accept Medicaid in Dayton, OH
- Making an appointment
Also Check: Can You Get Medicaid At 62
How To Choose Caresource
Medicaid health care coverage is available for eligible Ohioans with low income, pregnant women, infants and children, older adults and individuals with disabilities.
| Choose CareSource |
|---|
| When you apply for Ohio Medicaid, you can choose CareSource as your managed care plan. Whether you apply online, by mail, over the phone or at your local Department of Job and Family Services , tell them you want to choose CareSource. |
| Switch to CareSource |
|---|
| If you were assigned to another managed care plan and want to switch to CareSource, call the Ohio Medicaid hotline, complete a change request within 90 days and tell them you want to switch to CareSource. If you have been on your plan more than 90 days, you can switch to CareSource during your next open enrollment period. |
Medicaid Managed Care Procurement Award
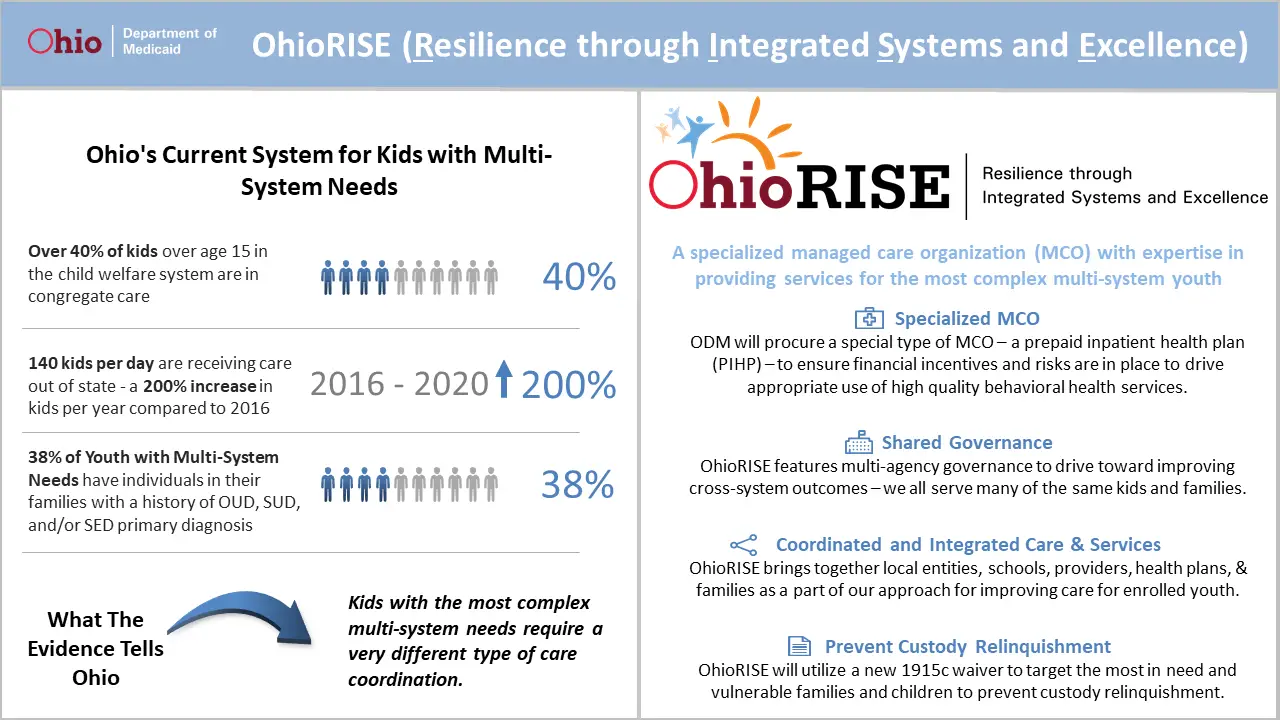
On April 9, 2021, ODM announced the selection of six managed care plans to lead the departments evolution of managed care services for its more than 3 million members and thousands of medical providers. Additional information about the announcement can be found in the press release and supplemental briefing document.
The selection reflects the results of intensive stakeholder engagement efforts to define opportunities to strengthen the structure of Ohios $20 billion managed care program. It addresses Governor Mike DeWines direction at the beginning of his term to re-evaluate Ohios managed care system with the goal of making the system more focused on individuals.
The seven MCOs selected for the next generation managed care program are:
- AmeriHealth Caritas Ohio, Inc.
- Anthem Blue Cross and Blue Shield
- Buckeye Community Health Plan
- Humana Health Plan of Ohio, Inc.
- Molina Healthcare of Ohio, Inc.
- UnitedHealthcare Community Plan of Ohio, Inc.
You May Like: How Can I Apply For Medicaid In Florida
I Would Like To Select My Plan
To make a next generation plan selection, Ohio Medicaid members can use the Ohio Medicaid Consumer Hotline Portal by clicking on the Select a Plan Online option below or by contacting the Ohio Medicaid Consumer Hotline at 324-8680.
Other Ways to Change your Health Plan
If you are unable to change health plans online at this time, there are several other options available to you.
Visiting The Medicaid Office
If you do not want to call the Medicaid office number and speak to a representative, you can go to the office. This is a helpful option if you would benefit from speaking to a program official in person. However, keep in mind that your Medicaid office may require you to schedule an appointment before you can meet with a representative. If this is true for your facility, call the office to schedule your meeting time.
You May Like: Dental Care That Accepts Medicaid
Previous Procurement Phases: Request For Applications And Requests For Information
We begin by first considering feedback and suggestions from individuals and providers when making decisions about how to evolve the Medicaid managed care program in Ohio. The feedback received through our first Request for Information informed development of RFI #2, outlining our vision for the next generation of Ohio’s Medicaid managed care program. The second RFI sought input from providers, associations, advocacy groups, data and information technology vendors, and managed care organizations. The response period for both RFI #1 and RFI #2 closed on Tuesday, March 3, 2020.
This feedback informed the program design reflected in Ohio Medicaids next generation program structure and procurement processes.
Mental Health And Substance Abuse Services
Get help with personal problems that may affect your mental or physical health. These may include stress, depression, anxiety or drugs and alcohol abuse. Our services also include:
- Therapy
- Counseling
- Medications
For some of these services prior approval is required. Please contact Member Services to learn more.
With our plan there are no copayments for covered services.
Members get:
- Care from highly skilled and compassionate doctors.
- Treatments at respected hospitals and clinics.
- Home medical equipment and supplies to help them be their best.
Read Also: How To Apply For Pregnancy Medicaid Ga
Unitedhealthcare Connected Benefit Disclaimer
This is not a complete list. The benefit information is a brief summary, not a complete description of benefits. For more information contact the plan or read the Member Handbook. Limitations, copays and restrictions may apply. For more information, call UnitedHealthcare Connected® Member Services or read the UnitedHealthcare Connected® Member Handbook. Benefits, List of Covered Drugs, pharmacy and provider networks and/or copayments may change from time to time throughout the year and on January 1 of each year.
You can get this document for free in other formats, such as large print, braille, or audio. Call , TTY 711, 8 a.m. – 8 p.m., local time, Monday – Friday . The call is free.
You can call Member Services and ask us to make a note in our system that you would like materials in Spanish, large print, braille, or audio now and in the future.
Language Line is available for all in-network providers.
Puede obtener este documento de forma gratuita en otros formatos, como letra de imprenta grande, braille o audio. Llame al , TTY 711, de 08:00 a. m. a 08:00 p. m., hora local, de lunes a viernes correo de voz disponible las 24 horas del día,/los 7 días de la semana). La llamada es gratuita.
Puede llamar a Servicios para Miembros y pedirnos que registremos en nuestro sistema que le gustaría recibir documentos en español, en letra de imprenta grande, braille o audio, ahora y en el futuro.
Los servicios Language Line están disponibles para todos los proveedores dentro de la red.
How Do I Contact Medicaid
Many people wonder, Is there a Medicaid office near me? However, once you locate a facility in your city or county, you may need to know how to contact that office. The representatives at your program will serve as your points of contact as you apply for and enroll in this insurance network. Therefore, no matter how long you have received Medicare benefits, you must know how to contact program officials.
Recommended Reading: Buckeye Health Plan Medicaid Ohio
Video Result For Ohio State Medicaid Phone Number
CINCINNATI MLS | setting up your profile
Sun West Loves Our Military
hotohio.gov
state
state
bestwww.rcmguide.com
phone
greatwww.ohiohelps.org
phonestate
trendwww.medicaid.gov
statestatestate
CINCINNATI MLS | setting up your profile
Sun West Loves Our Military
Sun West’s Website Is Easy to Use
NEW GRANTS Expire Soon Plus 55Billion Grant House Vs…
Unitedhealthcare Senior Care Options Plan
UnitedHealthcare SCO is a Coordinated Care plan with a Medicare contract and a contract with the Commonwealth of Massachusetts Medicaid program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is a voluntary program that is available to anyone 65 and older who qualifies for MassHealth Standard and Original Medicare. If you have MassHealth Standard, but you do not qualify for Original Medicare, you may still be eligible to enroll in our MassHealth Senior Care Option plan and receive all of your MassHealth benefits through our SCO program.
Don’t Miss: What Age To Apply For Medicaid
See What Unitedhealthcare Has To Offer
Its your health. Its your choice.
Everyone deserves affordable health care, including you.
Working adults, people with disabilities, pregnant women, and children who qualify for Medicaid should check out UnitedHealthcare Community Plan.
We have the Medicaid benefits and extras that can make a real difference in your life. All at no cost to you.
Find a doctor you trust in our network
- Dental coverage
- Transportation to and from doctor appointments
- 24/7 NurseLine to answer your health questions
- No copays
Sometimes, you might need a little extra help. Get extras not covered by Medicaid.
- Earn rewards for keeping you and your baby healthy
- Earn gift cards for getting preventive services
- Doctor Chat chat with a doctor wherever you are
- Wellhop for Mom & Baby
We also offer resources to help you make the most of your plan, including:
- Member Services
Helping you live a healthier life. We are here for you, OHIO. Remember to choose UnitedHealthcare Community Plan.
To learn more about UnitedHealthcare Senior Care Options, visit UHCCommunityPlan dot com forward slash OH.
Looking for the federal governments Medicaid website? Look here at Medicaid.gov.
Submit Your Application Online
The quickest and easiest way to apply for health care benefits is online at www.benefits.ohio.gov. There you will answer a series of questions and your answers will direct you to the correct application for health care.
- If your income is within the new legal limit implemented by Medicaid Expansion , you will be directed to the citizens self-service portal.
- If your income is above 205% of the Federal Poverty Level, you will be directed to the Federally Facilitated Health Insurance Marketplace to shop for health care.
After you submit your application online, you may be asked to send verification documents to Allen County Job and Family Services. The best way to return documents is to fax them to 227-2448.
Visit www.healthcare.gov or www.benefits.ohio.gov to learn more or call the Medicaid Consumer Hotline at 1-800-324-8680. Representatives are available to answer questions related to eligibility for Medicaid due to the Affordable Care Act and Medicaid Expansion and answer questions about where to apply.
You May Like: Is Horizon Nj Health Medicaid
Wellhop For Mom & Baby
Connect with other expectant moms. Get support and information during your pregnancy and after you deliver. This program is part of your health plan and there is no extra cost to you.
Heres how it works:
- Join video conversations every other week with women who have similar due dates and a group leader.
- Chat and share experiences with moms from your group on the Wellhop app or website.
- Visit the Wellhop library. Youll find articles, videos and more.
-
PDF 4.58MB – Last Updated: 04/20/2021
Apply For Medicaid Only
In some cases, you may want to apply to receive Medicaid without applying for cash or foodassistance. By visiting www.benefits.ohio.gov or calling 1-844-640-OHIO , you can apply forMedicaid only, without applying for cash or food assistance at the same time.To apply through the site, click Check your eligibility and follow the prompts.
Recommended Reading: How To Apply For Medicaid In Houston
Health Care With Heart
There is a reason more Ohioans choose CareSource for their Medicaid plan than all other plans combined. Its because CareSource is more than just quality health care. We care about you and your familys health and wellbeing. CareSource members get access to a large provider network, reward programs like Kids First and Babies First®, free rides to health care appointments, pharmacies and more. Plus, we never charge a copay for any medical or behavioral health service!
Choose CareSource for your Ohio Medicaid health care plan and join over 1.2 million members who trust us with their health and well-being.
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
Recommended Reading: How To Add New Baby To Medicaid
How To Contact Medicaid Offices Near You
You can contact Medicaid if you have any questions regarding this program. No matter where you live, you can easily contact your local Medicaid office with any questions you may have. Since this program and its application process may seem complex, an office representative can easily assist you.
Depending on where you are located, there are many different ways you can find a helpful Medicaid contact. You can choose a method that is most comfortable for you. Furthermore, remember that when you are learning how to contact Medicaid, procedures may vary by location. Even though Medicaid is a federal program, it is jointly funded on a state level. As a result, the steps you may need to follow to make contact can vary by facility.
Contracting With The Ohiorise Plan

Providers interested in contracting with Aetna to provide behavioral health services to children and youth enrolled in the OhioRISE program are encouraged to contact Aetna Better Health of Ohio. Providers can contact Aetna via the Provider Relations contact information listed below.
| OhioRISE Provider Relations Contact Information |
|---|
| MCO |
|
Aetna Better Health of Ohio, Inc |
Don’t Miss: Medicaid Brooklyn Ny Phone Number
Hamilton County Medicaid Resource Guide For Consumers
The quickest and easiest way to apply or renew health care benefits is to call 1-844-640-OHIO Monday Friday between 8 a.m. and 4 p.m.
You may also apply online at www.benefits.ohio.gov. There, you will answer a series of questions and your answers will direct you to the correct application for health care.
- If your income is within the current legal limit, you will be directed to the current Medicaid eligibility process
- If your income is above 205% of the Federal Poverty level, you will be directed to the Federally Facilitated Health Insurance Marketplace to shop for health care.
Visit www.healthcare.gov or www.benefits.ohio.gov to learn more, or contact HCJFS at 9461000, option 3, and a second option 3. Representatives are available to answer questions related to eligibility for Medicaid due to the Affordable Care Act and Medicaid Expansion and answer questions about how and where to apply.
If you are unable to complete an application over the phone or online, applications are available to print from our website, www.hcjfs.org , or you can complete an application in person at our office.
Hamilton County Main Fax Number
946-1076 The fax number is the best way to:
- Send in your Medicaid application*
- Send in verification documents as requested by HCJFS to process your online application
Applications can also be submitted via US mail or by utilizing the kiosk services on the 1st floor of the agency office, 222 E. Central Parkway, Cincinnati, Ohio, 45202
Medicaid Expansion
How To Apply For Medicaid
How do I complete an online application?
The quickest and easiest way to apply for health care benefits is online at benefits.ohio.gov. There you will answer a series of questions and your answers will direct you to the correct application for health care.
If your income is within the new legal limit implemented by Medicaid Expansion , you will be directed to the citizens self-service portal. If your income is above 205 percent of the Federal Poverty Level, you will be directed to the Federally Facilitated Health Insurance Marketplace to shop for health care.
After you submit your application online, you may be asked to send verification documents to Richland County Job & Family Services. The best way to return documents is to fax them to 774-0051.
Visit healthcare.gov or benefits.ohio.gov to learn more or call the Medicaid Consumer Hotline at . Representatives are available to answer questions related to eligibility for Medicaid due to the Affordable Care Act and Medicaid Expansion and answer questions about where to apply.
How do I complete a phone application?
If you are unable to complete an online application, you can complete an application by contacting Ohio Benefits at .
Please note, if you are applying for waiver services an additional application and interview may be required. You can find additional information regarding the waiver application process here. Medicaid.ohio.gov
How do I complete a paper application?
Don’t Miss: Medicaid Ga Number Customer Service
Prior Authorization And Notification Resources
- Ohio Department of Medicaid Emergency Provider Agreement Changes
- The ODM Provider FAQs has specific information on Ohios changes:
- Prior authorization requirements resume for services rendered July 1, 2020 and later. Providers must submit prior authorization requests in accordance with UnitedHealthcare policies and procedures.
- Timely filing for claims extended to 365 calendar days from the date of service.
- Access to telehealth services is expanded.
- For the pharmacy benefit, there are changes to prescription guidance, refill limits and prior authorization requirements.
Monday-Friday, 8 a.m. 5 p.m.
Postal Mailing Address
9200 Worthington Road, 3rd FloorWesterville, OH 43082
Attn: Complaint and Appeals DepartmentP.O. Box 31364Salt Lake City, UT 84131Fax: 994-1082
Attn: Complaint and Appeals DepartmentP.O. Box 31364Salt Lake City, UT 84131Fax: 994-1082
UHC Connected For MyCare Ohio Appeals Mailing Address
Part C Appeals or Grievances:UnitedHealthcare Community PlanAttn: Complaint and Appeals DepartmentP.O. Box 31364Salt Lake City, UT 84131Fax: 994-1082
Attn: Complaint and Appeals DepartmentP.O. Box 31364Salt Lake City, UT 84131Fax: 994-1082
Attn: Part D Standard AppealsP.O. Box 6103
For Credentialing and Attestation updates, contact the National Credentialing Center at 1-877-842-3210.
Need to make a change to your provider or facility directory information?
Behavioral Health Providers
The Centers for Medicare & Medicaid Services established the Medicaid Managed Care Rule to:
