Does It Work Well
Medicaid’s share-of-cost works especially well for people with high healthcare expenses that recur every month.
For example, if youre on a medication that costs $3,000 every month, and your share-of-cost is $1,900, youll meet your share-of-cost every month when you refill your prescription.
Time your refills to the first day of every month, and youll be covered with full Medicaid benefits all month every month.
What Does The Medically Needy Program Cover
Households participating in the Medically Needy program must submit copies of medical expenses to the state agency that administers Medicaid and the Medically Needy program. Some examples of expenses that Medically Needy households may submit to meet the monthly share of cost expenses include:
- Medical bills paid or incurred during the current month.
- Health insurance premiums .
- Doctor-prescribed medical goods and services .
- Costs of transportation to receive medical care.
Beneficiaries can submit proof of these expenses in the form of received bills, receipts for paid bills or canceled checks for paid bills. Beneficiaries can submit proof of medical expenses to the approved state agency. Proof of medical expenses should include the following information:
- Amount of expense
Can An Uninsured Woman Enroll In A Public Health Insurance Plan Upon Becoming Pregnant
Yes, women who meet the eligibility criteria for Medicaid or Childrens Health Insurance Program can enroll in one of these public programs at any point during pregnancy:
Full-Scope Medicaid
A pregnant woman is eligible for full-scope Medicaid coverage at any point during pregnancy if eligible under state requirements. Eligibility factors include household size, income, residency in the state of application, and immigration status. An uninsured woman who is already pregnant at the time of application is not eligible for enrollment in expansion Medicaid.
Pregnancy-Related Medicaid
If household income exceeds the income limits for full-scope Medicaid coverage, but is at or below the states income cutoff for pregnancy-related Medicaid, a woman is entitled to Medicaid under the coverage category for pregnancy-related services and conditions that might complicate the pregnancy. The income limits for pregnancy-related Medicaid vary, but states cannot drop eligibility for this coverage below a legal floor that ranges from an income of 133% to 185% of FPL , depending on the state. States are permitted to set a higher income cutoff.
Childrens Health Insurance Program
You May Like: Medicaid And Other Health Insurance
How Does The Medically Needy Pathway To Medicaid Eligibility Work
In states where the Medically Needy pathway exists for applicants above the Medicaid income limit, a certain amount of money must be spent down on medical bills before Medically Needy Medicaid will pay for the same services as Medicaid. The Medically Needy Income Limits are the amount one has left over after paying medical bills. Put another way, MNIL is ones income minus monthly healthcare costs.
The MNIL may be called by a different name, depending on the state. Share of cost, for example, is the term used in California. It is the dollar amount of medical bills that must be paid before Medicaid will pay the rest of ones medical expenses that month. Share of cost is therefore like the deductible on a health insurance policy. The higher an individuals income, the higher their share of cost will be.
Did You Know?
Example
Here is an example of when the Medically Needy pathway would apply to someone otherwise over the Medicaid income limit: Jack makes $4,000 per month in income and spends $3,500 on medical bills. This leaves him with $500 in monthly income after healthcare expenses. If he lives in a state that has a Medical Needy Income Limit above $500 , then he would qualify for Medicaid coverage of care services via Medically Needy Medicaid.
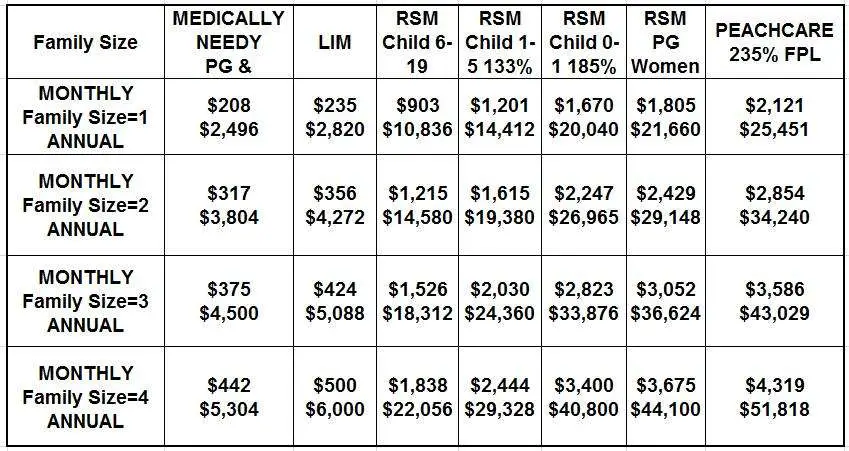
For a full list of states Medically Needy Income Limits, see below.
How Does Medicaid Work
The Medicaid program does not provide health care services for everyone. Your application will be reviewed for all Medicaid programs. If you are found eligible for Medicaid, you will get:
- A letter in the mail from Medicaid telling you about your coverage
- A Medicaid ID card
- A Healthy Louisiana plan ID card, if you enroll in a plan.
Each time you go to your health care provider or pharmacy, take your Medicaid ID and Healthy LA plan ID cards with you. Show them at all medical visits before you receive any service. The health care provider or pharmacy will tell you if they accept your Medicaid benefits. You should also ask your health care provider or pharmacy if the service or prescription is covered by Medicaid before receiving the service or filling a prescription.
Medicaid does not pay money to you instead, it sends payments directly to your health care provider or pharmacy.
Don’t Miss: General Doctor That Accepts Medicaid
What Is The Cost
None. Medicaid law prohibits states from charging deductibles, copayments, or similar charges for services related to pregnancy or conditions that might complicate pregnancy, regardless of the Medicaid enrollment category. HHS presumes pregnancy related services includes all services otherwise covered under the state plan, unless the state has justified classification of a specific service as not pregnancy-related in its state plan. States may, however, impose monthly premiums on pregnant women with incomes above 150% of FPL and charge for non-preferred drugs.
Most states that cover pregnant women in their CHIP program do not have cost-sharing or any other fees associated with participation in the program.
How Do I Report An Address Change
Call Medicaid Customer Service toll free at 1-888-342-6207 or go online by visiting the Medicaid Self-Service Portal to update your address.
If you do not have an online account, you can create an account at any time. Creating an online account allows you to check the status of your application, report any household changes, report an address change, request a replacement Medicaid ID card, and renew your Medicaid benefits.
Don’t Miss: High Risk Ob Gyn That Accepts Medicaid
What Does Medically Needy Mean In Terms Of Medicaid Eligibility
The term medically needy refers to individuals who:
- Are in one of Medicaid’s traditional eligibility categoriesblind, aged, pregnant, disabled, a child, or the parent of a minor child.
- Have income is too high for regular Medicaid eligibility
- Have medical expenses significant enough that when subtracted from the person’s income, it brings the after-medical-expense income down to a level that the state deems eligible for Medicaid under its medically needy program.
- Have limited assets .
Learn How To Apply For Medicaid With Our Help
As an independent and private company, we are proud to help our users learn about the benefit application process.
- Get Free Information with Our Guide
- Take our optional survey to receive, based on your answers, related offers from our partners!
- Keep Updated with Curated Content
Please Read:
- Data We Will Collect: Contact information and answers to our optional survey.
- What You Will Get: Free guide, and if you answer the optional survey, marketing offers from us and our partners.
- Use, Disclosure, Sale: If you complete the optional survey, we will send your answers to our marketing partners.
- Who We Will Share Your Data With: Our .
Recommended Reading: How To Qualify For Medicaid
What If I Think A Decision You Make Is Unfair Incorrect Or Made Too Late
You have the right to appeal the Medicaid decision. There are several ways to request an appeal. You can write the reason you disagree with the decision on the back of the decision letter and then mail or fax it to Medicaid as directed on the letter. You can also fax the decision letter to the Division of Administrative Law at 225-219-9823 or mail it to the Division of Administrative Law, Department of Health Section, P. O. Box 4189, Baton Rouge, LA 70821-4183. You can request an appeal by phone by calling Medicaid Customer Service at 1-888-342-6207 or the Division of Administrative Law at 225-342-5800.
Who Is Eligible For Medicaid In Florida
The following people may qualify for Florida Medicaid if they meet certain financialrequirements:
- Infants and children under the age of 21
- Recipients of Supplemental Security Income
- Seniors who are aged 65 or older
- People who are blind or expected to be disabled for at least a year
- People who need nursing home care or home and community-based care
- Medicare Beneficiaries whose income is low
- Aliens and refugees under a special assistance program
- Individuals who are medically needy
Recommended Reading: Affordable Care Act And Medicaid
Your Local Health Department Can Help You Find Affordable Prenatal Care
Your local health department can connect you to the services that can keep you in prenatal care while youre pregnant.
If youre at a low income and eligible, Presumptive Eligibility for Pregnant Women will be your first step toward prenatal coverage. PEPW is temporary coverage that can keep you healthy early in your pregnancy before Medicaid kicks in.
In Florida, the Department of Children and Families determines Medicaid eligibility for prenatal care. After PEPW, Medicaid will cover you for the rest of your pregnancy.
Healthy Start offers services to pregnant women, infants and children up to age three. Services include: provider referral, ongoing care coordination, and childbirth, breastfeeding and parenting support.
Who Is Eligible For Medicaid

The general guidelines for eligibility for Medicaid are set by the Federal government however, each state sets up their own specific requirements for eligibility and these can differ from state to state.
All States are required to include certain individuals or groups of people in their Medicaid plan.
The state eligibility groups are:
- Categorically needy
- Medically needy
- Special groups
In the categorically needy group, this will cover pregnant women whose income level is at or below 133% of the Federal Poverty level.
In the medically needy group, this will cover a pregnant woman who makes too much money to qualify in the categorically needy group. This means that women, who may have been denied Medicaid before, may be able to qualify now.
You May Like: Where Can I Apply For Medicaid In Florida
For Which Types Of Long Term Care Does Medically Needy Medicaid Apply
The three types of Medicaid which will pay for long term care to help seniors and those with chronic illnesses are Nursing Home Medicaid, Home and Community Based Services Waivers, and Aged, Blind and Disabled Medicaid. These benefits will pay for a high level of care in an institution or in ones home, depending on needs.
Whether the Medically Needy pathway to eligibility depends on the state and that states specific rules around the different types of Medicaid. Unfortunately, one cannot generalize at the national level.
Nursing Home MedicaidThe income limit in most states for an individual to qualify for Nursing Home Medicaid coverage is $2,523 per month in 2022. Someone who needs a Nursing Facility Level of Care but who has income higher than the limit would qualify for Medically Needy Medicaid if they spend a disproportionate amount of money on healthcare. See the chart below. For more on Nursing Home Medicaid, .
Home and Community Based Services WaiversFor HCBS Medicaid waivers that pay for care in ones own home or assisted living community, the income limits are often the same as Nursing Home Medicaid: $2,523 in most states in 2022 . Someone who earns above their states income limit but has high monthly medical costs could potentially qualify for Medically Needy Medicaid to pay for the same services as waivers. See the chart below. For more on HCBS waivers, .
How Do I Apply For Medicaid
You can apply for Medicaid at any time.
Even if you applied by mail, in-person, or over the phone, you can create an online account to check the status of your application, report household and address changes, request a new Medicaid ID card, and renew your Medicaid coverage.
You May Like: Does Doctors Care Accept Medicaid
Can A Pregnant Woman Receive Medicaid Or Chip Services Prior To An Eligibility Decision
Maybe. States may elect, but are not required, to provide some categories of Medicaid enrollees, including pregnant women, with presumptive eligibility. This allows pregnant women to receive immediate, same-day Medicaid services, typically at the clinic or hospital where they submit an application for Medicaid presumptive eligibility. Currently, 30 states provide presumptive eligibility to pregnant women.
You May Like: Does Nc Medicaid Cover Chiropractic
Maternity Coverage Is Still Way Too Complicated
Bethany married her college sweetheart a year and a half ago. But because her husband has had a few different jobs since graduating, most of which were contract positions with lackluster benefits, Bethany opted to stay on her moms insurance. Young adults can remain on their parents insurance until theyre 26, regardless of marital status.
It seemed ideal: Her parents have had some health issues in recent years, which meant they always hit their deductible. They had no idea about the dependent exemptions until it was too late, Bethany says.
In hindsight, it would be more affordable if Bethany was unmarried and therefore had a lower household income so she could claim Medicaid benefits, or if she taken out her own policy through a marketplace. While there are some federal laws that protect maternity rights, Bethany falls into a loophole.
For years, federal laws have stipulated that employers need to cover maternity care for their employees and their spouses. But there are no laws that specifically state companies have to cover maternity care for adult children because, until the ACA passed in 2009, most employer-based health insurance plans cut off coverage when the children legally became adults or upon college graduation.
There are all these disparate puzzle pieces fitting together and not fitting together.Julie StichThe International Foundation of Employee Benefit Plans
You May Like: First Choice Medicaid Eye Doctors
Who Does Medically Needy Cover
Pregnant women if
- Family income is over 300% of the federal poverty limits for a household of the same size. This includes the unborn baby.
- Family resources are not more than $10,000. People under age 21 if family income is over the income limit for regular Medicaid.
People who are aged, blind or disabled who
- Would be eligible for SSI except that income or resources are over the limit, and
- Are age 65 or older, or
- Are legally blind as defined by Social Security, or
- Are disabled as defined by Social Security.
Adults who care for dependent children under age 18 or age 19 and still in school, if:
- They are the parent, aunt, uncle, grandparent or disabled stepparent of a dependent child, and
- Their income is over the income limit for Medicaid for families, or their resources are over the resource limit for Medicaid for families.
What Is Floridas Medically Needy Program And How Does It Work
With the implementation of the Affordable Care Act, many states have enacted laws expanding Medicaid coverage by offering insurance to more people than were previously eligible. However, not all states participate in Medicaid expansion. Florida remains one of several states that have opted out of expansion therefore, it is very difficult for adults to receive Medicaid coverage. Many adults in the state fall into a coverage gap, meaning the make too much to qualify for Medicaid, yet too little to reasonably afford Marketplace coverage without a tax subsidy. The Medically Needy program is designed in part to ease the burden this places on lower income Floridians. Here is how it works.
What is the Medically Needy Program?
For those who make too much to be eligible for traditional Medicaid in Florida, the Medically Needy program is based on family size and household income and sets forth the maximum amount you must spend on healthcare in a given month. The program basically allows the state to share in the cost of your care each month, but only once you meet a certain out-of-pocket amount. In fact, it acts a lot like a deductible in many ways. Consider the following example.
EXAMPLE
But its not really a deductible at all
Does the Medically Needy program take care of the nursing home bill?
Read Also: What Does Medicaid Cover In Illinois
Categories Of Individuals Eligible For Medically Needy Programs
States that choose to have medically needy programs may decide not to offer the medically needy option to all categories of Medicaid-eligible people. For example, a state might chose to offer the medically needy program to elderly but not disabled people. However, states that offer any medically needy programs must offer them to most children and pregnant women.
Effective Date Of Coverage

Once an individual is determined eligible for Medicaid, coverage is effective either on the date of application or the first day of the month of application. Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
Don’t Miss: Delta Dental Medicaid Phone Number
Whats The Eligibility Requirement For Long
An applicant is not eligible for Florida Long Term Care Medicaid unless he or she meets certain asset and income limitations.
To be approved for Long Term Care Medicaid in Florida, you must be:
- At least 65 years of age or disabled
- A United States citizen or a qualified alien
- A Florida resident
- Gross monthly income must not exceed $2,382/month and
- Countable assets for a single person must not exceed $2,000.Assets for a married couple allow the Community Spouse to have $130,380 in countable assets.
How Does The Medically Needy Program Work
Even if you’re blind, disabled, pregnant, elderly, a child, or the parent of a minor child, your income might be too high for Medicaid eligibility .
But if you have to spend so much of your income on medical costs that your leftover income is quite low, you could qualify for Medicaid if your state has a medically needy program . Once you’ve spent enough on medical expenses to qualify for Medicaid, your remaining medical expenses will be covered by Medicaid until you have to qualify again, typically monthly or quarterly.
States don’t have to apply their medically needy programs to all of their categories of Medicaid eligibility. For example, a state can allow elderly people, but not disabled people, to qualify for Medicaid via the medically needy programor vice versa. But if a state has a medically needy program, it must be available to pregnant women and children.
The opportunity to subtract the money you spend on medical care from your income in order to qualify for Medicaid may be particularly useful if you are elderly and reside in a nursing home. Also, children and adults with disabilities may need to pay high costs for prescription drugs, medical equipment, or other healthcare expenses.
Don’t Miss: Therapy Places That Accept Medicaid
