People Who Have Both Medicare & Medicaid
People who have both Medicare and full Medicaid coverage are dually eligible. Medicare pays first when youre a dual eligible and you get Medicare-covered services. Medicaid pays last, after Medicare and any other health insurance you have.
You can still pick how you want to get your Medicare coverage: Original Medicare or Medicare Advantage . Check your Medicare coverage options.
If you choose to join a Medicare Advantage Plan, there are special plans for dual eligibles that make it easier for you to get the services you need, include Medicare coverage , and may also cost less, like:
- Special Needs Plans
- Medicare-Medicaid Plans
- Program of All-Inclusive Care for the Elderly plans can help certain people get care outside of a nursing home
How Much Will Medicaid Cost Me
It depends. Every state is different. You will probably not have to pay a monthly premium for Medicaid, but most people do have some out-of-pocket costs.2 Emergency services, family-planning services, pregnancy-related services and preventive care for children are all fully covered with no additional cost to you.
Which Medicaid Plan Is Best In Texas
There is no best Medicaid program. There is only the program that is best for you. Again, this is something best determined by a consultation with someone from Health and Human Services. Medicaid and CHIP cover half of all children in Texas. If yours is a low-income family, or you are an individual that meets other Medicaid qualifications, there is a very good chance that one of the programs is right for you.
You May Like: Can A Person Have Medicaid And Private Insurance
Income Requirements For Virginia Medicaid
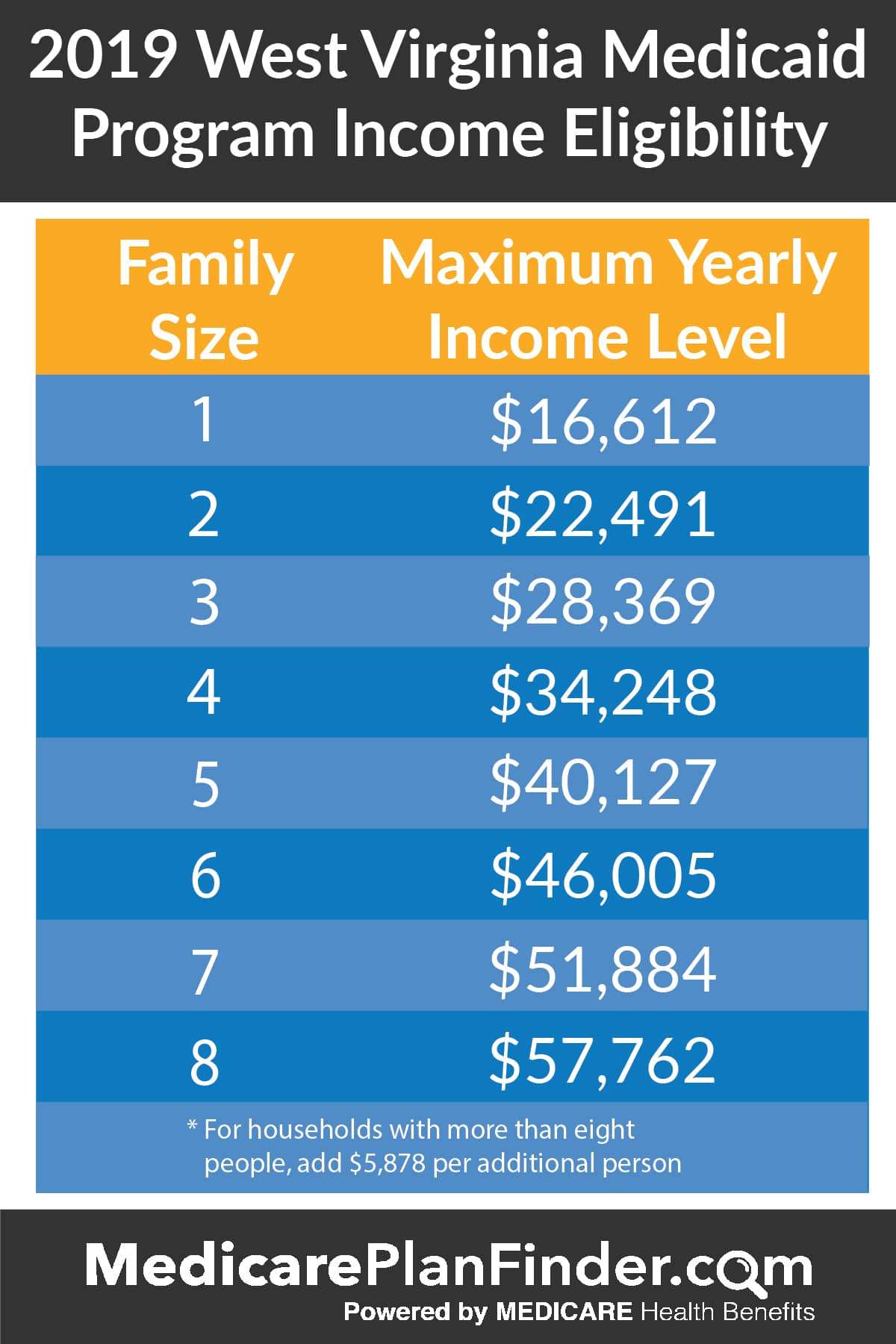
If you would like to be able to qualify for one of the Medicaid programs in Virginia, you will have to fall into the income bracket for the program you think you should be in. Pregnant women who might be in the FAMIS Plus program or Medicaid can make no more than 143% of the FPL as determined by the MAGI . For the childrens FAMIS program, MOMS, or Plan First, you cant earn more than 200% of the FPL. Children who are not yet 19 have to be in households that earn less than 143% of the FPL.
You can click here to find out more about the income limits for each household size.
How To Qualify For Medicaid
Almost every state has multiple Medicaid programs. But, as a good rule of thumb, if you make less than 100% to 200% of the federal poverty level and are pregnant, elderly, disabled, a parent/caretaker or a child, theres likely a program for you. And if you make less than 133% of the FPL**, theres possibly a program for you, depending on whether your state expanded Medicaid under Obamacare. In 2021, the federal poverty levels range from $12,880 to $44,660 .
In 2021, the federal poverty level in Alaska ranges from $ $16,090 to $55,850 . The federal poverty level in Hawaii ranges from $14,820 to $51,360 .
Recommended Reading: Medicaid Services Department Frankfort Ky
What Is The Highest Income To Qualify For Medicaid
Washington D.C. has the highest allowable income to qualify for Medicaid, at 215% of the FPL for individuals and 221% for a family of three.
That means an individual in Washington D.C. can make up to $27,692 per year and still be eligible for Medicaid. Washington D.C.s high cost of living factors into its higher income limit for Medicaid. No other state uses more than the standard 138% limit for individuals.
A family of three can make up to $48,531.60 and still qualify for Medicaid in Washington D.C. Connecticut is the only other state to use a limit higher than 138%.
There Are Some Tools You Can Use To Avoid Spending Down All Of Your Assets And Potentially Impoverishing A Spouse While Still Meeting The Qualifications For Medicaid
The bill for long-term care adds up fast. The annual median cost for a private room in a nursing home was $105,850 in 2020, according to Genworth. The government could pick up these costs if you qualify for Medicaid, but thats easier said than done. Medicaid is a welfare program, says Neel Shah, estate-planning attorney and a certified financial planner at Shah & Associates in Monroe Township, N.J. There are strict income and wealth limits to qualify.
Medicaid should not be confused with Medicare, the national health insurance program for people age 65 and over that largely doesnt cover long-term care.
If you can pay for your own care, youll have more options as not all facilities accept Medicaid. Still, even couples with ample savings risk impoverishing the other spouse to pay for a long stay in a nursing home. If thats what you fear, you may be surprised to learn that you can preserve some assets for a spouse and qualify for Medicaid using tools designed for that purpose.
Redistributing your assets can help you meet Medicaids standards. Rather than keeping $100,000 in the bank, use that money to pay off your mortgage or pay for home renovations, says Shah. Alternatively, you could prepay a burial plot, replace a vehicle or upgrade household appliances. Your spouse will keep these purchases if you need long-term care, and with fewer assets to spend down, youll qualify for Medicaid sooner.
Read Also: Is Qsymia Covered By Medicaid
Apply For Medicaid Coverage Even If Your State Hasnt Expanded
Even if your state hasnt expanded Medicaid and it looks like your income is below the level to qualify for financial help with a Marketplace plan, you should fill out a Marketplace application.
Each state has coverage options that could work for you particularly if you have children, are pregnant, or have a disability. And when you provide more detailed income information you may fall into the range to save.
Donât Miss: How To Get Medicaid To Cover Tummy Tuck
Do You Qualify For Ssi Or 1619
If you have a disability, low income, and low resources, you may qualify for SSI. If you already get SSI benefits, you automatically get Medicaid coverage and do not need to apply separately.
If you dont get SSI benefits yet, you should learn whether you might qualify by reading DB101s SSI article. At the same time, you should apply for Medicaid separately, because it can take Social Security several months to review your SSI application and its important for you to have health coverage until then.
If you used to get SSI benefits, but stopped getting them after you started working, you may qualify automatically for Medicaid through a special rule called 1619 as long as your gross income is below $40,078 per year. Learn more about 1619 in DB101s SSI article.
If you do not get SSI benefits and do not qualify for 1619, income-based Medicaid might cover you.
Recommended Reading: Doctors In Denver That Take Medicaid
Don’t Miss: Who Qualifies For Medicaid In New Jersey
Q How Do I Join A Managed Care Organization
A. After being notified that you are eligible for Medicaid , you will receive in the mail a packet of information about the different MCO plan options for receiving your Medicaid benefits. You may choose any plan described in this mailing. You probably want to choose a Managed Care Organization to which your doctor belongs. If you need help making this decision, call the Health Benefit Manager at the phone number in the mailing.
Medicaid Eligibility Costs And Benefits
If youve fallen on hard times, applying for Medicaid may not be the first item on your to-do list but you might want to add it now.
Medicaid is the public health insurance program available to people with low incomes. It covers more than 72 million Americans, making it the single largest provider of health insurance in the U.S. If you have a medical condition or take expensive prescriptions, it can greatly help in your time of need.
Unlike Medicare, the federal health insurance program primarily for people ages 65 and older, Medicaid is run jointly by federal and state governments. So, although your state government determines many benefits, all state Medicaid programs must meet certain minimum federal standards. Heres what to know about Medicaid.
Recommended Reading: Pediatricians In Amarillo Tx That Accept Medicaid
Don’t Miss: Apply For Medicaid When Pregnant
Lawfully Residing Targeted Low
States have the option to provide CHIP and Medicaid coverage to children and pregnant women who are lawfully residing in the United States and are otherwise eligible for coverage, including those within their first five years of having certain legal status. If states do not adopt this option, federal law requires a 5-year waiting period before many legal immigrants are permitted to enroll in Medicaid and CHIP. Learn more about providing health coverage to lawfully residing children and pregnant women at 2107 of the Social Security Act, and in SHO# 10-006. A list of states providing Medicaid and CHIP coverage to lawfully residing children and/or pregnant women.
Q If I Dont Qualify For Medicaid Is There Any Other Help For Me Or My Children
A. Yes. Many organizations in Delaware are dedicated to the principle that health care should never be beyond the reach of those who need it. If you need health care, but do not have insurance coverage, the people at the Delaware HelpLine have a wealth of information about organizations that provide health care at reduced rates for uninsured individuals. Call the Delaware HelpLine toll-free at 1-800-464-HELP from Monday Friday from 8:00 a.m. to 5:00 p.m. The Delaware Helpline service is also available in Spanish. Additional information about the support provided by the Delaware Helpline can also be found by visiting www.delawarehelpline.org.
For example, you may qualify to receive discounted medical services through the Community Healthcare Access Program . CHAP helps connect uninsured individuals with affordable health care from primary care doctors, medical specialists, and other health providers including prescription programs, laboratory and radiology services. To find out more about this program, visit the website for the Community Healthcare Access Program, or call 1-800-996-9969 for eligibility guidelines.
You can read about CHAP and other healthcare resources for uninsured individuals in the Delaware Healthcare Resource Guide. This guide is also available in Spanish: Guía de Recursos de Salud.
Under 18:
Over 65:
Recommended Reading: Indiana Medicaid Provider Phone Number
Q Who Qualifies For Medicaid
A. Citizenship and Residency – To obtain full Medicaid benefits in Delaware, you must be a Delaware resident and either a U.S. citizen or a legally residing noncitizen. Full coverage for noncitizens which include DACA recipients is dependent on the availability of state funding. However, noncitizens can qualify for coverage for emergencies and labor & delivery services if income requirements are met.
Income Level – Qualifying for Medicaid is also based on need. Household income must be under certain limits as defined by the Federal Poverty Level and is based on family size. For Long Term Care programs, financial resources must also be under a certain amount. There are also specific programs for individuals who meet certain medical or disability tests, or who qualify due to age or pregnancy. To find out more about different Medicaid and other medical assistance programs, visit DMMA Programs & Services.
What Does Medicaid Cover In Virginia
Medicaid in Virginia has three levels of benefits.
Full coverage provides members with the complete range of benefits. This includes pharmacy, hospital, and doctor services for qualified individuals.
Time-limited coverage is for people who meet the spend-down or women who get 24 months of services regarding family planning once the Medicaid coverage they had expires at the end of their pregnancy.
Medicare-related coverage is where Medicaid will pay for Medicare premiums. This might also include payments for Medicare coinsurance and deductible.
Don’t Miss: How And Where To Apply For Medicaid
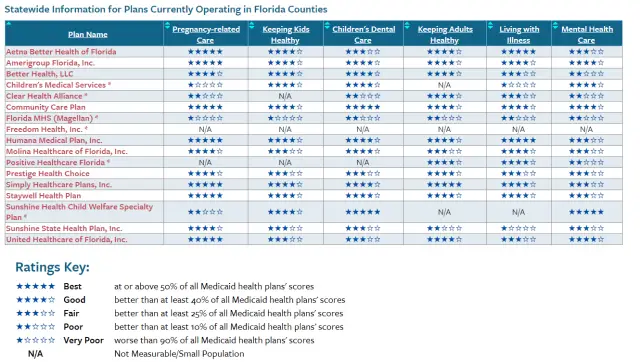
Florida Medicaid Program Eligibility
Medicaid is a program for medical assistance that gives low-income individuals and families access to health care that they wouldnt otherwise have. Medicaid also assists people with disabilities and the elderly with the costs of expenses like care in nursing facilities and other long-term medical bills.
The agency responsible for Medicaid in Florida is the Agency for Health Care Administration, also known as simply the Agency. The Agency has successfully completed implementing the SMMC program. Under this program, most of the recipients of Medicaid are enrolled into one of a variety of health plans. These health plans are accredited nationally and selected by a competitive procurement process.
Current Law: 16 Weeks Of Federal Additional Income Included In Eligibility
At present, vulnerable workers who become unemployed can receive $600 in additional federal income for 16 weeks. This federal unemployment compensation is included in income eligibility determinations for ACA marketplace eligibility but not for Medicaid and CHIP eligibility.
Eligibility for assistance of any kind is not substantially different between expansion and nonexpansion states when all the cash assistance available is received, the researchers stated.
READ MORE:Medicaid Expansion States May See Lower Uninsurance Amid COVID-19
However, workers in expansion states are seven times more likely to be eligible for Medicaid, the researchers found. This is a critical metric because Medicaid usually has limited additional out-of-pocket healthcare spending for beneficiaries, as opposed to health plans on the ACA federal or state health insurance marketplace. This would make healthcare more affordable for Medicaid-eligible workers in Medicaid expansion states.
In both Medicaid expansion and nonexpansion states, under the current law, a similar percentage of vulnerable workers are not eligible for any federal funding . The percentage is slightly lower in Medicaid expansion states.
Recommended Reading: North Carolina Medicaid Income Guidelines
How To Get Or Keep Medicaid While Working
I am bedridden and cannot work outside the home. However, when I am able I enjoy making jewelry and crafts in bed. I started selling them on Etsy. Then a friend told me that I would be considered self-employed and I could apply for Medicaid for Working Disabled. So I applied and it got approved! Now Medicaid pays 100% of all my doctors bills and prescriptions, but the best thing is it also provides me with a personal care attendant 20 hours per week in my home. Juniper
People arent aware of Medicaid programs for working adults while disabled. People think Medicaid is only for really poor people. One of the ADAPT protestors who was arrested in Colorado is a full-time attorney. She has Medicaid, which provides services so she can live at home, get assistance getting in and out of her wheelchair, take care of her kids, and work.Pansy
My sister had $300 per month in medicaid spend down expenses. She started tutoring a neighbors child, and we helped her apply for Medicaid for Working Adults with Disabilities. Now she tutors a one afternoon each week and she pays $20 per month for Medicaid. All her medical expenses and surgeries are covered. Sweet Pea
MEDICAID FOR WORKING PEOPLE WITH DISABILITIES
Good news about Medicaid and working while disabled. If you start working, you may be able to keep Medicaid, even if you would not normally qualify.
OPTION ONE: MEDICAID BUY INS
Most states have a program called Medicaid Buy In for Working Adults with Disabilities
GET HELP
Can I Get Medicaid For My Children
Yes, if your income is not too high. Medicaid and The Childrens Health Insurance Program provide low cost coverage to millions of families with children. Income requirements vary by state. In all but two states, children who live in four-person households with incomes up to $52,400 qualify for either Medicaid or CHIP. Eighteen states and DC will cover children in families of four who earn even up to $78,600, although sometimes families at the higher eligibility levels may need to pay more for the coverage.
If you have a baby while youre on Medicaid, your baby will automatically be enrolled in Medicaid for their first year.
You May Like: Is Obamacare And Medicaid The Same Thing
Can A College Student Receive Food Stamps
If you are otherwise eligible for SNAP benefits, you can get them for a short time while you are waiting for your Social Security number. Students: Most able-bodied students ages 18 through 49 who are enrolled in college or other institutions of higher education at least half time are not eligible for SNAP benefits.
Recommended Reading: Is Wisdom Teeth Removal Covered By Medicaid
Q How Long Will My Medicaid Benefits Remain Active
A. Medicaid is based on month to month eligibility. However, your benefits are redetermined on a yearly basis by DMMA to confirm whether you still remain eligible for the program you are receiving. Certain Medicaid programs require you to report changes in your situation within 10 days of the change. One example of a change that must be reported is new employment.
Recommended Reading: Does Medicaid Pay For Dental Work
What If Im Turned Down By Medicaid
- You may be able to buy a private health plan through the Marketplace instead for the 2018 plan year in the fall. You may qualify for savings based on your income through a premium tax credit and savings on out-of-pocket costs.
- If you dont qualify for either Marketplace or Medicaid savings, you still have options. Learn more here.
Illinoiss Requirements For Medicaid Qualification
The state of Illinois sets particular requirements for enrollees to qualify for the Medicaid program. First, certain income standards must get met if residents in the area hope to qualify. What was once given to children and pregnant women is now available for women and men as well, as long as they meet the criteria. Those who fall far above the poverty level cannot receive this state insurance. If you would like to find out if you should apply, use the Check If I Should Apply button on the Application for Benefits Eligibility website. It asks questions regarding your family size, age, gender, taxes, health coverage through work, medical needs, and more.
Dont Miss: How To Find Your Medicaid Number
You May Like: Different Types Of Medicaid In Nc
