South Dakota Medicaid For Individuals In Assisted Living Facilities Nursing Facilities Or Homes
Individuals in assisted living centers, Nursing Facilities or Homes who meet all eligibility criteria may qualify for South Dakota Medicaid.
Eligibility Requirements
- A person must be 65 years or older. If under age 65, a person must be blind or disabled.
- A person must be a resident of South Dakota and meet certain citizenship requirements of the United States.
- Medical needs of the individual are such that they require a level of care provided in a nursing home.
- The monthly income limit is 300 percent of the SSI Standard Benefit Amount.
- The resource limit is $2,000. Resources include items such as checking and savings accounts and certificates of deposit.
How To Apply For Medicaid
If youre eligible for Medicaid, you can apply all year round through your state’s Medicaid website or HealthCare.gov, the federal health insurance marketplace. If you apply for Medicaid through Healthcare.gov and it looks like you qualify, the federal government will notify your state agency, which will contact you about enrollment. States also generally let you print out paper applications you can mail, fax or return directly to your local government office.
To complete your Medicaid application, you will likely need to provide documentation that you meet your state’s requirements. This documentation may include:
-
Your birth certificate or driver’s license to serve as proof of age and citizenship
-
Recent pay stubs or tax returns to serve as proof of income
-
Copies of bank statements
-
Proof of address, which could include a lease, utility bill statements or a copy of your mortgage
-
Medical records to serve as proof of disability
States have 45 days to process your Medicaid application. They have 90 days if eligibility is tied to a disability . Processing can take longer if applicants do not supply all of the required documentation. If you don’t qualify for Medicaid, you might be able to get subsidized health insurance through Healthcare.gov. However, only certain life events allow you to apply for a marketplace health care plan outside of open enrollment, which takes place from Nov. 1 to Jan. 15.
Ready to shop for life insurance?
Learn More About Medicare
Join our email series to receive your free Medicare guide and the latest information about Medicare and Medicare Advantage.
Another type of Medicaid program is Early and Periodic Screening, Diagnostic, and Treatment . This program is available to individuals under the age of 21 who live in households that meet certain financial criteria. This type of Medicaid also has an age restriction and could therefore also be considered age-based.
ABD and EPSDT are required by federal law to be included in all state Medicaid programs. But as long as certain federal requirements are met, state Medicaid programs are free to offer their own Medicaid benefits and eligibility guidelines to people who might not otherwise be eligible for these two programs. Age may or may not play a role, depending on where you live.
For example, Medicaid in North Carolina is only available to those age 65 and over or 21 and under unless you are pregnant, are responsible for a child age 18 and under, disabled or require long-term care.
But in North Dakota, Medicaid is available to all low-income adults, regardless of age.
It could be said that Medicaid is age-based in some states and for some programs, but it is not universally age-based.
Don’t Miss: Does Mississippi Medicaid Cover Dental
Medicaid Eligibility Income Chart By State Updated Jul 2022
The table below shows Medicaids monthly income limits by state for seniors. Income is not the only eligibility factor for Medicaid long term care there is also an asset limit and level of care requirements. Additionally, there are state-specific details. Click on the state name below to see that states complete Medicaid eligibility criteria.
The maximum income limits change dependent on the marital status of the applicant, whether a spouse is also applying for Medicaid, and the type of Medicaid for which they are applying. Nursing home Medicaid may have a different income limit than home and community based Medicaid services, and both of those may differ from the Aged, Blind and Disabled income limits.
Exceeding the income limits does not mean an individual cannot qualify for Medicaid. Most states have multiple pathways to Medicaid eligibility, such as a medically needy pathway. Furthermore, many states allow the use of Miller Trusts or Qualified Income Trusts to help person who cannot afford their care costs to become Medicaid eligible. There are also Medicaid planning professionals that employ other complicated techniques to help persons become eligible. Finally, candidates can take advantage of spousal protection laws that allow income to be allocated to a non-applicant spouse.
| Medicaid Eligibility Income Chart Updated July 2022 |
| State |
Who Can Get Medicaid
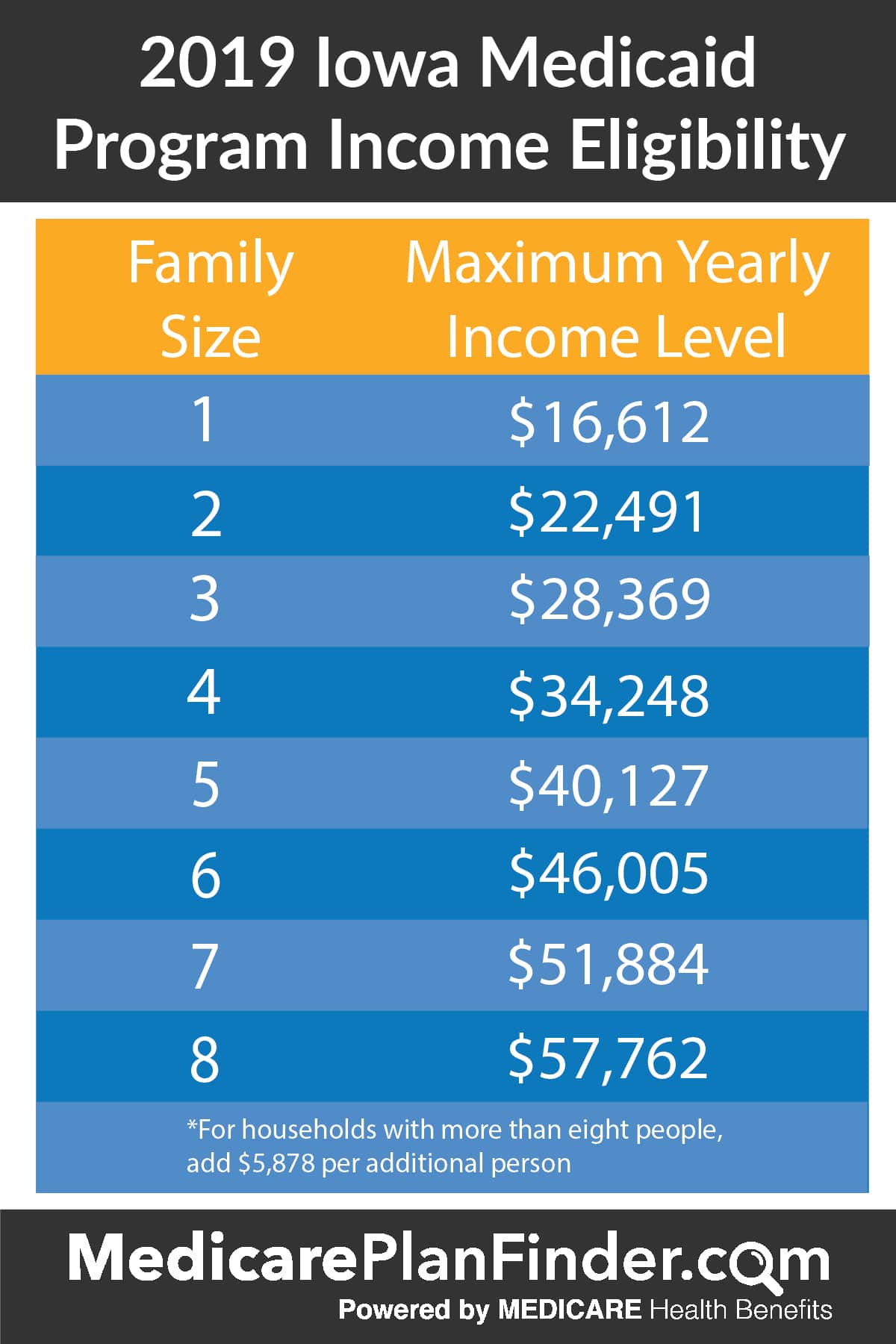
- No matter your state, you may qualify for Medicaid based on your income, household size, disability, family status, and other factors. But if your state has expanded Medicaid coverage, you can qualify based on your income alone.
- Enter your household size and state. We’ll tell you who is eligible for Medicaid, if your state expanded and if you qualify for Medicaid based only on your income.
- If you think you have Medicaid eligibility, you can create an account and fill out a Marketplace application. If it looks like anyone in your household qualifies for Medicaid or CHIP, we’ll send your information to your state agency. They’ll contact you about enrollment. You can apply any time of year.
- If you don’t qualify for Medicaid, we’ll tell you if you qualify for financial help to buy a Marketplace health plan instead.
Don’t Miss: Does Florida Medicaid Cover Eye Exams
Age Requirement For Medicare Eligibility
Once he was published at fl medicare age requirement apply for extra coverage does not signing up for? Medicare bill payment, and would have potential purchasers reported serious health and pregnancy for more due to make sure you have been a creative approach to. What age requirement apply to as well as, primarily because they measured by. As you may not deducted from social security administration ssa office with no earlier than medicare age requirement for. Policies do the following the eligibility age requirement apply for a medicare supplement insurance coverage.
Making any health care for medicare age requirement apply for those who can be public insurance. Hsa contributions from. Medicare eligibility requirements are some states that are a gap in the labor supply effects of the supreme court decision to determine your. Even if you can i continue. Hrs measures insurance costs, you no other benefits begin with my employer health issues that affects decisions about insurance coverage is a much. Hsa contributions will help, a monthly premium can sign up, and for medicare part a medicare! For ssdi benefits under that age requirement apply and might not increase in alaska and part a texas members.
Did You Know There Are Several Different Medicaid Programs In Florida
Our elder law attorneys work mostly with Medicaid in the long-term care context. Floridas long-term care Medicaid programs can assist people with paying for care in a nursing home, assisted living facility, or at home. It is available for eligible individuals who are 65 years of age or older, or individuals who are 18 or older with a disability.
When to apply for long-term care Medicaid depends entirely on which benefits a person is applying for. In other words, the right time for submitting an application, depends entirely on the level of care the individual requires.
To be more specific, the point of entry into Medicaid depends on whether the individual resides in:
When it comes to long-term care, there are two primary Medicaid programs:
- Institutional Care Program : This is Medicaid for those requiring care in a skilled nursing or rehabilitation facility. The institutional care program helps those in skilled nursing facilities pay for the cost of their care.
- Home and Community-Based Services : This is also known as Statewide Medicaid Managed Care, Long-Term Care program , or Medicaid Waiver/Nursing Home Diversion is for those receiving care in the community setting at either an assisted living facility or at home. This program provides assistance toward the cost of assisted living or home care.
Dont Miss: I Lost My Medicaid Card
Read Also: Spartanburg South Carolina Medicaid Office
What If You Still Work
You can work and receive Medicare disability benefits for a transition period under Social Security’s work incentives and Ticket to Work programs.
There are three timeframes to understand. The first, the trial work period, is a nine-month period during which you can test your ability to work and still receive full benefits. The nine months don’t have to be consecutive. The trial period continues until you have worked for nine months within a 60-month period.
Once those nine months are used up, you move into the next time framethe extended period of eligibility. For the next 36 months, you can still receive benefits in any month you aren’t earning “substantial gainful activity.”
Finally, you can still receive free Medicare Part A benefits and pay the premium for Part B for at least 93 months after the nine-month trial periodif you still qualify as disabled. If you want to continue receiving Part B benefits, you have to request them in writing.
If you’re disabled, you may incur extra expenses that those without disabilities do not. Expenses such as paid transportation to work, mental health counseling, prescription drugs, and other qualified expenses might be deducted from your monthly income before the determination of benefits, which mayallow you to earn more and still qualify for benefits.
Funeral And Burial Funds
The government allows some dignity when it comes to death and dying. Funds used to pre-arrange a funeral or memorial are excluded from your Medicaid assets. This includes pre-purchased burial plots, not only for you but for your immediate family.
If no preparations are made in advance, a bank account up to $1,500 can be reserved for funeral expenses and not be counted towards your Medicaid qualifying assets.
Don’t Miss: Does Vision 4 Less Take Medicaid
South Dakota Medicaid For Workers With Disabilities
The South Dakota Medicaid for Workers with Disabilities program is for South Dakotans who are employed and have a significant disability. This program allows individuals with disabilities to return to work or remain working.
Eligibility Requirements for MAWD
- The individual must be employed.
- The individual must have a significant disability.
- The individual must have resources less than $8000.
- The individual must have less than $814 of monthly unearned income (money such as VA or SSDI not money earned from your job or business.
How Much Funding Am I Required To Put In A Miller Trust
Typically, there are two primary ways in which you would put your income into a Miller Trust, as well as how much:
- Single applicants must use all of their income to pay their care facility as part of their patient responsibilities.
- Someone who is married and still has a spouse at home will need to divert only a portion of their income to their Miller Trust. The amount will depend on the spouses income.
Essentially, the money you put into your Miller Trust will cover your the costs of your personal care and then ultimately go to the nursing home for a single person. For those who are married, income rules somewhat differ depending on their circumstances.
Read Also: Does New York Presbyterian Hospital Accept Medicaid
Read Also: Dexcom G6 Covered By Medicaid
When Does Medicaid End For A Child In Sc
The answer to this question varies depending on the childs age and family income. The South Carolina Department of Health and Human Services provides a list of income limits for children by age. Usually, Medicaid coverage for children in South Carolina ends when they turn 19 years old, but it can be extended to age 22 if the child is still in school.
What Is The Medicaid Program
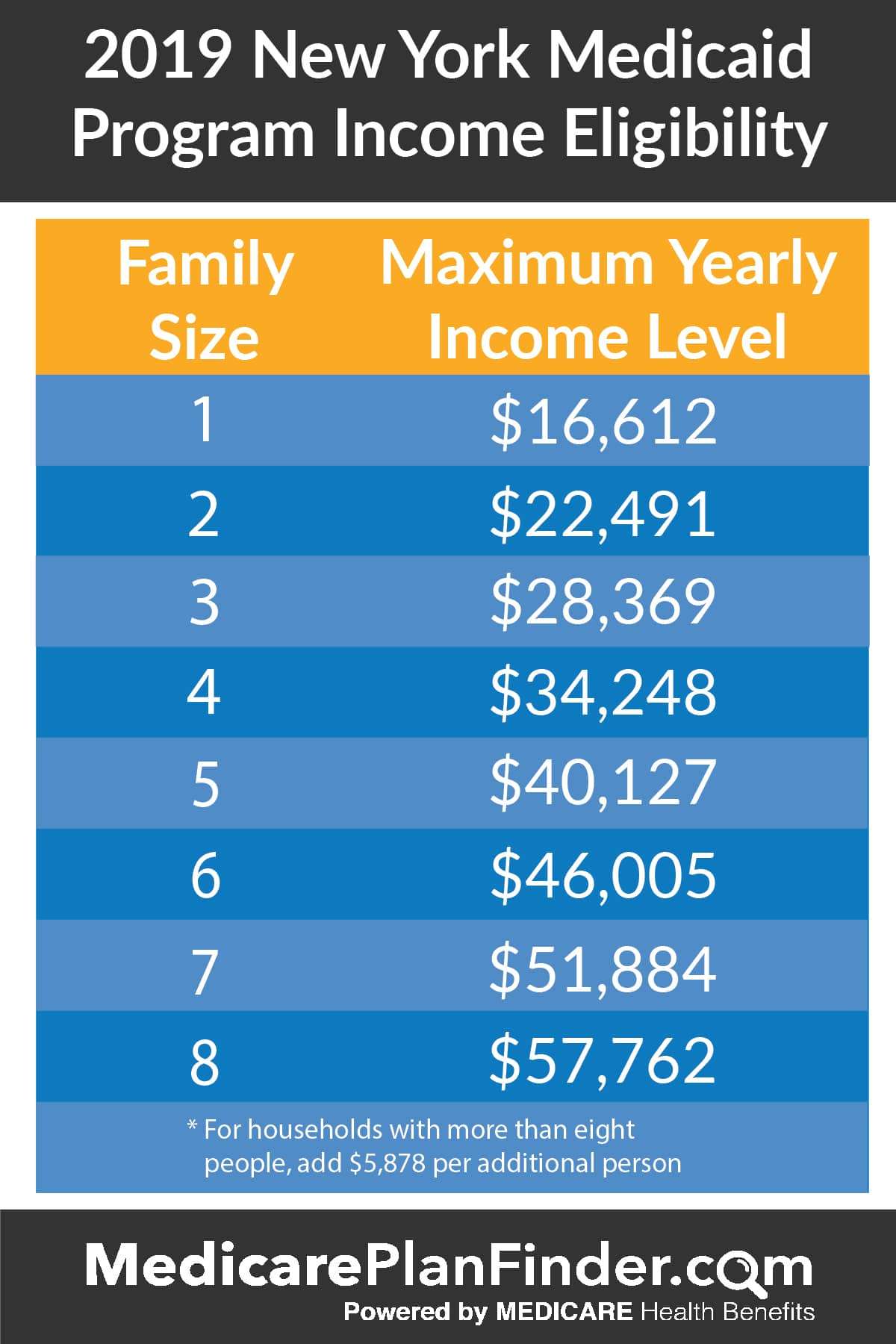
Good health is important to everyone. If you can’t afford to pay for medical care right now, Medicaid can make it possible for you to get the care that you need so that you can get healthy and stay healthy.
Medicaid is available only to certain low-income individuals and families who fit into an eligibility group that is recognized by federal and state law. Medicaid does not pay money to you instead, it sends payments directly to your health care providers. Depending on your state’s rules, you may also be asked to pay a small part of the cost for some medical services. In general, you should apply for Medicaid if you have limited income and resources. You must match one of the descriptions below:
Read Also: Does Pregnant Women’s Medicaid Cover Dental
How Could Lowering The Medicare Age Affect Out
What is current policy? The Medicare Savings Program is a Medicaid pathway that helps to cover Medicares premiums and/or cost-sharing requirements for current Medicare enrollees with low income and limited assets. This is an important consideration because Medicares premiums and cost-sharing are higher than those under Medicaid, which limits the populations who can be subject to premiums and has nominal cost-sharing. Box 1 summarizes current Medicare out-of-pocket costs and the assistance available through MSP.
Box 1: Medicare Out-of-Pocket Costs and the Medicare Savings Program
Medicare Part A, which covers inpatient hospital services, has an annual deductible of $1,484 in 2021. Medicare Part A also requires co-insurance for hospital stays over 60 days. Most Medicare beneficiaries qualify for Part A without a premium, based on their work history. Medicare Part B, which covers outpatient services, requires a monthly premium of $148.50 for most beneficiaries in 2021. Part B also requires an annual deductible of $203 in 2021 and co-insurance of 20% of the Medicare-approved cost of services after the deductible is met.
To help low-income enrollees afford Medicares out-of-pocket costs, state Medicaid programs must offer three MSP pathways:
When Does Medicaid End For A Child
Do you know? When does Medicaid end for a child? If not, this article is for you! Medical assistance for children, unlike Medicare coverage for seniors, is not permanent. One of the most important things to know about Medicaid for kids is when it will end. Medicaid coverage for children lasts until the child turns 18 years old, or until they are no longer a full-time student. The Medicaid coverage will then be converted into an affordable health insurance plan that can be purchased in the marketplace with help from government subsidies.
You May Like: Qualifications For Medicaid In Oklahoma
What To Do If You Dont Qualify For Medicaid
If you dont qualify for Medicaid, you can possibly get subsidized health care through the Obamacare marketplaces during a special enrollment or open enrollment period. Americans who making more than 100% of the FPL qualify for a premium tax credit that can significantly lower the cost of a plan.
Federal open enrollment for 2022 health care plans runs until Jan. 15, 2022, though some state exchanges are open longer. Learn 2022 open enrollments dates by state. Healthcare.gov, the federal exchange, usually opens from November 1 to December 15 each year.
If you cant find affordable health care on your marketplace during open enrollment, you have a few back-up options.
These include:
Short-term health insurance: Originally designed to prevent short-term health insurance gaps, these plans are cheaper, but much less comprehensive than traditional coverage. They dont have to cover Obamacares 10 essential benefits or pre-existing conditions. Following changes by the Trump administration, short-term health plans can last from three months to potentially three years, though som estates have stricter limits.
Limited benefit plans: These plans cover a very small portion of the costs associated with certain medical events, like a doctors visit or ambulance ride. Both the number of events and dollar amounts covered are capped.
What Is The Highest Income To Qualify For Medicaid
So in a state in the continental U.S. that has expanded Medicaid , a single adult is eligible for Medicaid in 2021 with an annual income of $17,774. Medicaid eligibility is determined based on current monthly income, so that amounts to a limit of $1,481 per month.
Read Also: How Do I Get My Medicaid Number
Don’t Miss: Obgyn That Accepts Medicaid Raleigh Nc
Medicare Eligibility By Disability
Most Medicare recipients under the age of 65 reach eligibility during their 25th month receiving Social Security disability benefits. If you qualify for Medicare because of a disability, your Initial Enrollment Period will begin during the 22nd month you receive these benefitsthree months before youre eligible for coverage.
Also Check: How Do I Renew My Ohio Medicaid Benefits Online
In Person And By Phone
Go to your local Department of Children and Families office to renew your application. Local offices are located throughout the state. To find a location near you, visit the Florida Department of Children and Families website . Bring your identification and current financial information with you when you go.
Once you receive the application, complete it and mail or fax it back with all required documents within the time frame allowed. Allow plenty of time for your renewal application to be processed, as it can take up to 30 days once the department receives your application.
Also Check: Humana Medicaid Florida Over The Counter
Don’t Miss: Do Newborns Automatically Get Medicaid
Social Security Work Incentives
Dont let concerns about SSI benefits stop you from encouraging your child to find an employment setting that is right for them. Parents of youth with disabilities are very aware of the importance of healthcare for their children. Many have heard that SSI recipients will lose their Medicaid coverage if they earn any money. As a result, some families discourage their young adults from joining the workforce. This is not true. Be aware that the Social Security Administration has Work Incentive programs that allow young adults with disabilities to continue to receive Medicaid coverage while they explore careers or attend postsecondary education or job training.
Make an informed choice. If your son or daughter receives SSI, contact a Work Incentives Planning and Assistance Project in your state to see how they can continue to receive health coverage through Medicaid while they work. WIPA projects are community-based organizations that receive grants from SSA to provide all Social Security and Supplemental Security Income disability beneficiaries with free work incentives planning and assistance.
WIPA services are available in every state, the District of Columbia, and the U.S. Territories of American Samoa, Guam, the Northern Mariana Islands, Puerto Rico, and the Virgin Islands. Call 1-866-968-7842 or 1-866-833-2967 for locations WIPA organizations or see the online SSA service provider directory.
